Summary
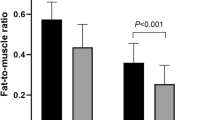
The study aimed to determine the relationships between the basal metabolic rate (BMR) and body composition of overweight and obese Chinese adults with type 2 diabetes mellitus (DM). This cross-sectional clinical study enrolled 193 Chinese adults with type 2 DM who were overweight (24 kg/m2=BMI≤28 kg/m2, n=99), or obese (BMI ≥28 kg/m2, n=94). Ninety-seven adults with normal BMIs, including 50 DM patients and 47 healthy adults, were recruited as a control group. BMR was measured by indirect calorimetry; predicted BMR was calculated according to the Schofield equation; and the relationships between BMR, body composition, and biochemical results were determined by the Pearson correlation. The results showed that obese DM patients had significantly higher BMRs than both overweight patients (P<0.05) and patients with normal BMI did (P<0.05). The measured BMR was significantly lower than the predicted BMR (P<0.05) in all groups. Obese and overweight DM patients had significantly greater weight, waist circumference, hip circumference, BMI, body surface area, body fat percentage, fat mass, and fat-free mass than patients with normal BMI. Except for waist circumference, these body composition measurements were significantly increased in obese DM patients when compared with those in overweight DM patients (P<0.05). Fat-free mass was closely correlated with BMR in both DM patients (r=0.874, P<0.01) and in healthy controls (r=0.902, P<0.01). It was concluded that overweight and obese Chinese adults with type 2 DM had increased BMRs compared with normal-weight controls, which may result from the difference in fat-free mass.
Similar content being viewed by others
References
Hou X, Lu J, Weng J, et al. Impact of waist circumference and body mass index on risk of cardiometabolic disorder and cardiovascular disease in Chinese adults: a national diabetes and metabolic disorders survey. PLoS One, 2013,8(3):e57319
Miyake R, Ohkawara K, Ishikawa-Takata K, et al. Obese Japanese adults with type 2 diabetes have higher basal metabolic rates than non-diabetic adults. J Nutr Sci Vitaminol (Tokyo), 2011,57(5):348–354
Fontvieille AM, Lillioja S, Ferraro RT, et al. Twenty-four-hour energy expenditure in Pima Indians with type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia, 1992,35(8):753–759
Bitz C, Toubro S, Larsen TM, et al. Increased 24-h energy expenditure in type 2 diabetes. Diabetes Care, 2004,27(10):2416–2421
Moller JB, Pedersen M, Tanaka H, et al. Body composition is the main determinant for the difference in type 2 diabetes pathophysiology between Japanese and Caucasians. Diabetes Care, 2014,37(3):796–804
Zhou BF. Predictive values of body mass index and waist circumference for risk factors of certain related diseases in Chinese adults—study on optimal cut-off points of body mass index and waist circumference in Chinese adults. Biomed Environ Sci, 2002,15(1):83–96
Schofield WN. Predicting basal metabolic rate, new standards and review of previous work. Hum Nutr Clin Nutr, 1985,39(Suppl 1):5–41
Ravussin E, Burnand B, Schutz Y, et al. Twenty-four-hour energy expenditure and resting metabolic rate in obese, moderately obese, and control subjects. Am J Clin Nutr, 1982,35(3):566–573
Huang KC, Kormas N, Steinbeck K, et al. Resting metabolic rate in severely obese diabetic and nondiabetic subjects. Obes Res, 2004,12(5):840–845
Franssila-Kallunki A, Groop L. Factors associated with basal metabolic rate in patients with type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia, 1992,35(10):962–966
Thaler JP, Guyenet SJ, Dorfman MD, et al. Hypothalamic inflammation: marker or mechanism of obesity pathogenesis?. Diabetes, 2013,62(8):2629–2634
Dulloo AG, Montani JP. Body composition, inflammation and thermogenesis in pathways to obesity and the metabolic syndrome: an overview. Obes Rev, 2012,13(Suppl 2):1–5
Constantinopoulos P, Michalaki M, Kottorou A, et al. Cortisol in tissue and systemic level as a contributing factor to the development of metabolic syndrome in severely obese patients. Eur J Endocrinol, 2015,172(1):69–78
Czernichow S, Kengne AP, Stamatakis E, et al. Body mass index, waist circumference and waist-hip ratio: which is the better discriminator of cardiovascular disease mortality risk?: evidence from an individual-participant meta-analysis of 82 864 participants from nine cohort studies. Obes Rev, 2011,12(9):680–687
Shah NR, Braverman ER. Measuring adiposity in patients: the utility of body mass index (BMI), percent body fat, and leptin. PLoS One, 2012,7(4):e33308
James WP, Ferro-Luzzi A, Waterlow JC. Definition of chronic energy deficiency in adults. Report of a working party of the International Dietary Energy Consultative Group. Eur J Clin Nutr, 1988,42(12):969–981
Wulan SN, Westerterp KR, Plasqui G. Ethnic differences in body composition and the associated metabolic profile: a comparative study between Asians and Caucasians. Maturitas, 2010,65(4):315–319
Seo DY, Lee S, Figueroa A, et al. Yoga training improves metabolic parameters in obese boys. Korean J Physiol Pharmacol, 2012,16(3):175–180
Aragao FR, Abrantes CG, Gabriel RE, et al. Effects of a 12-month multi-component exercise program on the body composition of postmenopausal women. Climacteric, 2014,17(2):155–163
Author information
Authors and Affiliations
Corresponding author
Additional information
This project was supported by the National Natural Science Foundation of China (No. 81370942).
Rights and permissions
About this article
Cite this article
Sun, Mx., Zhao, S., Mao, H. et al. Increased BMR in overweight and obese patients with type 2 diabetes may result from an increased fat-free mass. J. Huazhong Univ. Sci. Technol. [Med. Sci.] 36, 59–63 (2016). https://doi.org/10.1007/s11596-016-1542-6
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-016-1542-6