Abstract
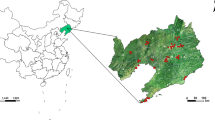
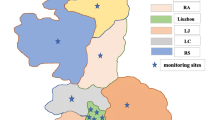
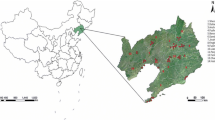
Evidence links exposure to maternal sulfur dioxide (SO2) and the risk of limb defects have been inconsistent. To investigate associations between SO2 exposure during preconception and the first trimester and risks of polydactyly and syndactyly. The study population was acquired from the Maternal and Child Health Certificate Registry of Liaoning Province between 2010 to 2015, and consisted of 2605 polydactyly, 595 syndactyly cases, and 7950 controls. Ambient air pollutants levels were retrieved from air quality monitoring stations. We used multivariable logistic regression model to assess the adjusted odds ratios (ORs) and 95% confidence intervals (CIs). We found that exposure to increased SO2 concentrations was associated with polydactyly during both the 3 months preconception (ORQ4 vs. Q1 = 3.76; 95% CI 2.61, 5.42; per 10 μg/m3 increment: OR = 1.07; 95% CI 1.04, 1.10) and the first trimester (ORQ4 vs. Q1 = 2.03; 95% CI 1.41, 2.92; per 10 μg/m3 increment: OR = 1.07; 95% CI 1.03, 1.11). However, we only observed increased risk for syndactyly in the analysis of high vs. low quartiles (three months preconception: ORQ4 vs. Q1 = 3.72; 95% CI 2.05, 6.75; first trimester: ORQ4 vs. Q1 = 1.98; 95% CI 1.11, 3.51). Most results of analyses based on single-month exposure window generally showed similar positive associations. Additionally, these findings were broadly consistent across subgroups and sensitivity analyses. Maternal SO2 exposure increase the risk of polydactyly and syndactyly.




Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Abbreviations
- ASD:
-
Absolute standardized difference
- CIs:
-
Confidence intervals
- ICD-10-CM:
-
International Classification of Diseases, Tenth Revision, Clinical Modification
- NO2 :
-
Nitrogen dioxide
- ORs:
-
Odds ratios
- PM10 :
-
Particulate matter with aerodynamic diameters ≤ 10 μm
- PSM:
-
Propensity score matching
- SD:
-
Standard deviation
- SO2 :
-
Sulfur dioxide
References
Austin PC (2009) Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med 28:3083–3107. https://doi.org/10.1002/sim.3697
Bell ML, Belanger K (2012) Review of research on residential mobility during pregnancy: consequences for assessment of prenatal environmental exposures. J Expo Sci Environ Epidemiol 22:429–438. https://doi.org/10.1038/jes.2012.42
Chang HH, Reich BJ, Miranda ML (2012) Time-to-event analysis of fine particle air pollution and preterm birth: results from North Carolina, 2001-2005. Am J Epidemiol 175:91–98. https://doi.org/10.1093/aje/kwr403
Chen EK, Zmirou-Navier D, Padilla C, Deguen S (2014) Effects of air pollution on the risk of congenital anomalies: a systematic review and meta-analysis. Int J Environ Res Public Health 11:7642–7668. https://doi.org/10.3390/ijerph110807642
Choi G, Stingone JA, Desrosiers TA, Olshan AF, Nembhard WN, Shaw GM, Pruitt S, Romitti PA, Yazdy MM, Browne ML, Langlois PH, Botto L, Luben TJ (2019) Maternal exposure to outdoor air pollution and congenital limb deficiencies in the National Birth Defects Prevention Study. Environ Res 179:108716. https://doi.org/10.1016/j.envres.2019.108716
Coker E, Ghosh J, Jerrett M, Gomez-Rubio V, Beckerman B, Cockburn M, Liverani S, Su J, Li A, Kile ML, Ritz B, Molitor J (2015) Modeling spatial effects of PM(2.5) on term low birth weight in Los Angeles County. Environ Res 142:354–364. https://doi.org/10.1016/j.envres.2015.06.044
Dolk H, Armstrong B, Lachowycz K, Vrijheid M, Rankin J, Abramsky L, Boyd PA, Wellesley D (2010) Ambient air pollution and risk of congenital anomalies in England, 1991-1999. Occup Environ Med 67:223–227. https://doi.org/10.1136/oem.2009.045997
Ezzati M, Kammen DM (2002) The health impacts of exposure to indoor air pollution from solid fuels in developing countries: knowledge, gaps, and data needs. Environ Health Perspect 110:1057–1068. https://doi.org/10.1289/ehp.021101057
Gong TT, Wu QJ, Chen YL, Jiang CZ, Li J, Li LL, Liu CX, Li D, Zhou C, Huang YH (2016) Evaluating the time trends in prevalence of exomphalos in 14 cities of Liaoning province, 2006 to 2015. Sci Rep 6:32901. https://doi.org/10.1038/srep32901
Ha S, Hu H, Roussos-Ross D, Haidong K, Roth J, Xu X (2014) The effects of air pollution on adverse birth outcomes. Environ Res 134:198–204. https://doi.org/10.1016/j.envres.2014.08.002
Huang CC, Wen HJ, Chen PC, Chiang TL, Lin SJ, Guo YL (2015) Prenatal air pollutant exposure and occurrence of atopic dermatitis. Br J Dermatol 173:981–988. https://doi.org/10.1111/bjd.14039
Huang YH, Wu QJ, Chen YL, Jiang CZ, Gong TT, Li J, Li LL, Zhou C (2018) Trends in the prevalence of congenital hydrocephalus in 14 cities in Liaoning province, China from 2006 to 2015 in a population-based birth defect registry from the Liaoning Women and Children's Health Hospital. Oncotarget 9:14472–14480. https://doi.org/10.18632/oncotarget.24239
Jalaludin B, Mannes T, Morgan G, Lincoln D, Sheppeard V, Corbett S (2007) Impact of ambient air pollution on gestational age is modified by season in Sydney, Australia. Environ Health 6:16. https://doi.org/10.1186/1476-069X-6-16
Jin L, Qiu J, Zhang Y, Qiu W, He X, Wang Y, Sun Q, Li M, Zhao N, Cui H, Liu S, Tang Z, Chen Y, Yue L, Da Z, Xu X, Huang H, Liu Q, Bell ML, Zhang Y (2015) Ambient air pollution and congenital heart defects in Lanzhou, China. Environ Res Lett 10. https://doi.org/10.1088/1748-9326/10/7/074005
Kampa M, Castanas E (2008) Human health effects of air pollution. Environ Pollut 151:362–367. https://doi.org/10.1016/j.envpol.2007.06.012
Kannan S, Misra DP, Dvonch JT, Krishnakumar A (2006) Exposures to airborne particulate matter and adverse perinatal outcomes: a biologically plausible mechanistic framework for exploring potential effect modification by nutrition. Environ Health Perspect 114:1636–1642. https://doi.org/10.1289/ehp.9081
Langlois PH, Hoyt AT, Lupo PJ, Lawson CC, Waters MA, Desrosiers TA, Shaw GM, Romitti PA, Lammer EJ (2012) Maternal occupational exposure to polycyclic aromatic hydrocarbons and risk of neural tube defect-affected pregnancies. Birth Defects Res A Clin Mol Teratol. 94:693–700. https://doi.org/10.1002/bdra.23045
Liang Z, Wu L, Fan L, Zhao Q (2014) Ambient air pollution and birth defects in Haikou city, Hainan province. BMC Pediatr 14:283. https://doi.org/10.1186/s12887-014-0283-6
Lin YT, Lee YL, Jung CR, Jaakkola JJ, Hwang BF (2014) Air pollution and limb defects: a matched-pairs case-control study in Taiwan. Environ Res 132:273–280. https://doi.org/10.1016/j.envres.2014.04.028
Lupo PJ, Langlois PH, Reefhuis J, Lawson CC, Symanski E, Desrosiers TA, Khodr ZG, Agopian AJ, Waters MA, Duwe KN, Finnell RH, Mitchell LE, Moore CA, Romitti PA, Shaw GM (2012) Maternal occupational exposure to polycyclic aromatic hydrocarbons: effects on gastroschisis among offspring in the National Birth Defects Prevention Study. Environ Health Perspect 120:910–915. https://doi.org/10.1289/ehp.1104305
Lv Y, Wang H, Wei S, Zhang L, Zhao Q (2017) The Correlation between indoor and outdoor particulate matter of different building types in Daqing, China. Procedia Eng 205:360–367
Malik S (2014) Polydactyly: phenotypes, genetics and classification. Clin Genet 85:203–212. https://doi.org/10.1111/cge.12276
Ministry of Health of China (2020) Report on Women and Children’s Health Development in China. Ministry of Health of China Publishing Maternal and Child health Monitoring Web. http://www.mchscn.org/Article_Show.asp?ArticleID=712/ (accessed 18 March 2020)
Papadakis M, Manios A, Trompoukis C (2019) Surgical treatment of polydactyly and syndactyly during the 4th century AD. Acta Chir Belg 119:64–65. https://doi.org/10.1080/00015458.2018.1534392
Rac MWF, McKinney J, Gandhi M (2019) Polydactyly. Am J Obstet Gynecol 221:B13–B15. https://doi.org/10.1016/j.ajog.2019.09.023
Ritz B (2010) Air pollution and congenital anomalies. Occup Environ Med 67:221–222. https://doi.org/10.1136/oem.2009.051201
Ritz B, Yu F, Fruin S, Chapa G, Shaw GM, Harris JA (2002) Ambient air pollution and risk of birth defects in Southern California. Am J Epidemiol 155:17–25. https://doi.org/10.1093/aje/155.1.17
Ritz B, Wilhelm M, Hoggatt KJ, Ghosh JK (2007) Ambient air pollution and preterm birth in the environment and pregnancy outcomes study at the University of California, Los Angeles. Am J Epidemiol 166:1045–1052. https://doi.org/10.1093/aje/kwm181
Schembari A, Nieuwenhuijsen MJ, Salvador J, de Nazelle A, Cirach M, Dadvand P, Beelen R, Hoek G, Basagana X, Vrijheid M (2014) Traffic-related air pollution and congenital anomalies in Barcelona. Environ Health Perspect 122:317–323. https://doi.org/10.1289/ehp.1306802
Shi Y, Zhang B, Kong F, Li X (2018) Prenatal limb defects: epidemiologic characteristics and an epidemiologic analysis of risk factors. Medicine (Baltimore) 97:e11471. https://doi.org/10.1097/MD.0000000000011471
Shi J, Lv ZT, Lei Y, Kang H (2019) Maternal occupational exposure to chemicals in the textile factory during pregnancy is associated with a higher risk of polydactyly in the offspring. J Matern Fetal Neonatal Med 33:1–7. https://doi.org/10.1080/14767058.2019.1593358
Slama R, Darrow L, Parker J, Woodruff TJ, Strickland M, Nieuwenhuijsen M, Glinianaia S, Hoggatt KJ, Kannan S, Hurley F, Kalinka J, Sram R, Brauer M, Wilhelm M, Heinrich J, Ritz B (2008) Meeting report: atmospheric pollution and human reproduction. Environ Health Perspect 116:791–798. https://doi.org/10.1289/ehp.11074
Stingone JA, Luben TJ, Daniels JL, Fuentes M, Richardson DB, Aylsworth AS, Herring AH, Anderka M, Botto L, Correa A, Gilboa SM, Langlois PH, Mosley B, Shaw GM, Siffel C, Olshan AF (2014) Maternal exposure to criteria air pollutants and congenital heart defects in offspring: results from the national birth defects prevention study. Environ Health Perspect 122:863–872. https://doi.org/10.1289/ehp.1307289
Tang Z, Zhang H, Bai H, Chen Y, Zhao N, Zhou M, Cui H, Lerro C, Lin X, Lv L, Zhang C, Zhang H, Xu R, Zhu D, Dang Y, Han X, Xu X, Lin R, Yao T, Su J, Ma B, Liu X, Wang Y, Wang W, Liu S, Luo J, Huang H, Liang J, Jiang M, Qiu W, Bell ML, Qiu J, Liu Q, Zhang Y (2018) Residential mobility during pregnancy in Urban Gansu, China. Health Place 53:258–263. https://doi.org/10.1016/j.healthplace.2018.08.021
Vinikoor-Imler LC, Davis JA, Meyer RE, Luben TJ (2013) Early prenatal exposure to air pollution and its associations with birth defects in a state-wide birth cohort from North Carolina. Birth Defects Res A Clin Mol Teratol 97:696–701. https://doi.org/10.1002/bdra.23159
Vinikoor-Imler LC, Stewart TG, Luben TJ, Davis JA, Langlois PH (2015) An exploratory analysis of the relationship between ambient ozone and particulate matter concentrations during early pregnancy and selected birth defects in Texas. Environ Pollut 202:1–6. https://doi.org/10.1016/j.envpol.2015.03.001
Vrijheid M, Martinez D, Manzanares S, Dadvand P, Schembari A, Rankin J, Nieuwenhuijsen M (2011) Ambient air pollution and risk of congenital anomalies: a systematic review and meta-analysis. Environ Health Perspect 119:598–606. https://doi.org/10.1289/ehp.1002946
Wang L, Xiang X, Mi B, Song H, Dong M, Zhang S, Bi Y, Zhao Y, Li Q, Zhang Q, Zhang L, Yan H, Wang D, Dang S (2019) Association between early prenatal exposure to ambient air pollution and birth defects: evidence from newborns in Xi'an, China. J Public Health (Oxf) 41:494–501. https://doi.org/10.1093/pubmed/fdy137
Wennborg H, Magnusson LL, Bonde JP, Olsen J (2005) Congenital malformations related to maternal exposure to specific agents in biomedical research laboratories. J Occup Environ Med 47:11–19. https://doi.org/10.1097/01.jom.0000150237.67801.93
Xiong L, Xu Z, Wang H, Liu Z, Xie D, Wang A, Kong F (2019) The association between ambient air pollution and birth defects in four cities in Hunan province, China, from 2014 to 2016. Medicine (Baltimore) 98:e14253. https://doi.org/10.1097/MD.0000000000014253
Xu L, Li X, Dai L, Yuan X, Liang J, Zhou G, Li Q, He C, Miao L, Wang Y, Zhu J (2011) Assessing the trend of gastroschisis prevalence in China from 1996 to 2007 using two analytical methods. Birth Defects Res A Clin Mol Teratol. 91:177–184. https://doi.org/10.1002/bdra.20753
Yao C, Chen Y, Zhu X, Liu Y, Zhang J, Hou L, Xu Y, Zhang C, Cao J (2016) Air pollution and the risk of birth defects in Anqing City, China. J Occup Environ Med 58:e124–e127. https://doi.org/10.1097/JOM.0000000000000676
Zhang B, Liang S, Zhao J, Qian Z, Bassig BA, Yang R, Zhang Y, Hu K, Xu S, Zheng T, Yang S (2016) Maternal exposure to air pollutant PM2.5 and PM10 during pregnancy and risk of congenital heart defects. J Expo Sci Environ Epidemiol 26:422–427. https://doi.org/10.1038/jes.2016.1
Zhang TN, Gong TT, Chen YL, Wu QJ, Zhang Y, Jiang CZ, Li J, Li LL, Zhou C, Huang YH (2017) Time trends in the prevalence and epidemiological characteristics of neural tube defects in Liaoning Province, China, 2006-2015: A population-based study. Oncotarget 8:17092–17104. https://doi.org/10.18632/oncotarget.15060
Zhang JY, Wu QJ, Huang YH, Li J, Liu S, Chen YL, Li LL, Jiang CZ, Chen ZJ (2020) Association between maternal exposure to ambient PM10 and neural tube defects: A case-control study in Liaoning Province, China. Int J Hyg Environ Health 225:113453. https://doi.org/10.1016/j.ijheh.2020.113453
Zhao Q, Liang Z, Tao S, Zhu J, Du Y (2011) Effects of air pollution on neonatal prematurity in Guangzhou of China: a time-series study. Environ Health 10:2. https://doi.org/10.1186/1476-069X-10-2
Funding
This work was supported by the National Key R&D Program of China (no. 2017YFC0907403 to Yu-Hong Zhao), Liaoning Providence science and technology project (2015225025 to Yan-Hong Huang), the Shenyang science and technology project (F15-139-9-09 to Yan-Hong Huang), the LiaoNing Revitalization Talents Program (No. XL-YC1907102 to Qi-Jun Wu), and 345 Talent Project to Qi-Jun Wu.
Author information
Authors and Affiliations
Contributions
Study conceptualization and design: Q-JW, Y-HZ and Y-HH; Data collection: JL, SL, Y-LC, and L-LL; Data cleaning and discrepancy checks: Q-JW; Analytic strategy: J-YZ and Y-HH; Analysis and interpretation of data: Y-TJ, T-TG, C-ZJ, and Z-JC; Manuscript preparation: Y-TJ, T-TG, and Y-HZ. All authors read and approved the final manuscript. Y-TJ and T-TG contributed equally to this work.
Corresponding authors
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Ethics approval and consent to participate
The research was approved by the institutional review board of Liaoning Women and Children's Health Hospital.
Consent for publication
The manuscript is reviewed and approved by all authors.
Additional information
Responsible Editor: Lotfi Aleya
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 1723 kb).
Rights and permissions
About this article
Cite this article
Jiang, YT., Gong, TT., Zhang, JY. et al. Maternal exposure to ambient SO2 and risk of polydactyly and syndactyly: a population-based case-control study in Liaoning Province, China. Environ Sci Pollut Res 28, 11289–11301 (2021). https://doi.org/10.1007/s11356-020-11351-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-020-11351-5