Abstract
Objectives
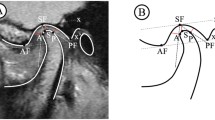
The aim of this study is to investigate the effect of internal derangements and degenerative bone changes on the minimum thickness of the roof of the glenoid fossa (RGF).
Methods
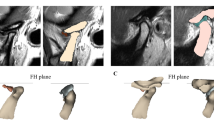
MRI and cone beam CT records of temporomandibular joints (TMJ) of 68 patients were evaluated retrospectively in this study. The joints were divided into three groups according to TMJ disc status which had been diagnosed in MRI: normal disc status, anterior disc displacement with reduction, and anterior disc displacement without reduction. Cone beam CT was used to evaluate the degenerative bone changes of TMJ and to measure the minimum thickness of RGF. The joints were categorized as “with osteoarthritis (OA)” or “without OA”. The findings of OA were determined as erosion, osteophyte, flattening, sclerosis, and pseudocyst.
Results
No significant relationship was found between gender and the thickness of RGF (p > 0.05). RGF was found significantly higher in “with OA” group compared to “without OA” group (p < 0.001). No significant difference was found between disc displacement groups for minimum thickness of RGF (p > 0.005). No significant difference was found between condyles without erosion and condyles with erosion for the minimum thickness of RGF (p = 0.272). In the present study, osteophyte, sclerosis, flattening, and pseudocyst were found to be associated with the minimum thickness of RGF.
Conclusions
Osteophyte, flattening, pseudocyst, and sclerosis have an influence on RGF thickness. The minimum thickness of RGF is not significantly correlated with internal derangements. Erosion is not significantly correlated with RGF thickness. RGF thickness may be unaffected by the early stages of OA.



Similar content being viewed by others
References
Honda K, Kawashima S, Kashima M, Sawada K, Shinoda K, Sugisaki M. Relationship between sex, age, and the minimum thickness of the roof of the glenoid fossa in normal temporomandibular joints. Clin Anat. 2005;18:23–6.
Gil C, Santos K, Dutra M, Kodaira S, Oliveira J. MRI analysis of the relationship between bone changes in the temporomandibular joint and articular disc position in symptomatic patients. Dentomaxillofac Radiol. 2012;41:367–72.
Tomas X, Pomes J, Berenguer J, Quinto L, Nicolau C, Mercader JM, et al. MR imaging of temporomandibular joint dysfunction: a pictorial review. Radiographics. 2006;26:765–81.
Alkhader M, Kuribayashi A, Ohbayashi N, Nakamura S, Kurabayashi T. Usefulness of cone beam computed tomography in temporomandibular joints with soft tissue pathology. Dentomaxillofac Radiol. 2010;39:343–8.
Tsiklakis K, Syriopoulos K, Stamatakis H. Radiographic examination of the temporomandibular joint using cone beam computed tomography. Dentomaxillofac Radiol. 2004;33:196–201.
Matsumoto K, Honda K, Sawada K, Tomita T, Araki M, Kakehashi Y. The thickness of the roof of the glenoid fossa in the temporomandibular joint: relationship to the MRI findings. Dentomaxillofac Radiol. 2006;35:357–64.
Ejima K, Schulze D, Stippig A, Matsumoto K, Rottke D, Honda K. Relationship between the thickness of the roof of glenoid fossa, condyle morphology and remaining teeth in asymptomatic European patients based on cone beam CT data sets. Dentomaxillofac Radiol. 2013;42:90929410.
Kijima N, Honda K, Kuroki Y, Sakabe J, Ejima K, Nakajima I. Relationship between patient characteristics, mandibular head morphology and thickness of the roof of the glenoid fossa in symptomatic temporomandibular joints. Dentomaxillofac Radiol. 2007;36:277–81.
Tsuruta A, Yamada K, Hanada K, Hosogai A, Tanaka R, Koyama J, et al. Thickness of the roof of the glenoid fossa and condylar bone change: a CT study. Dentomaxillofac Radiol. 2003;32:217–21.
Ahmad M, Hollender L, Anderson Q, Kartha K, Ohrbach R, Truelove EL, et al. Research diagnostic criteria for temporomandibular disorders (RDC/TMD): development of image analysis criteria and examiner reliability for image analysis. Oral Surg Oral Med Oral Pathol Oral Radiol. 2009;107:844–60.
Shaefer JR, Riley CJ, Caruso P, Keith D. Analysis of criteria for MRI diagnosis of TMJ disc displacement and arthralgia. Int J Dent 2012;96:312–25.
Honda K, Arai Y, Kashima M, Takano Y, Sawada K, Ejima K, et al. Evaluation of the usefulness of the limited cone-beam CT (3DX) in the assessment of the thickness of the roof of the glenoid fossa of the temporomandibular joint. Dentomaxillofac Radiol. 2004;33:391–5.
Barron RP, Kainulainen VT, Gusenbauer AW, Hollenberg R, Sàndor GK. Management of traumatic dislocation of the mandibular condyle into the middle cranial fossa. J Can Dent Assoc. 2002;68:676–8.
İlgüy D, İlgüy M, Fişekçioğlu E, Dölekoğlu S, Ersan N. Articular eminence inclination, height, and condyle morphology on cone beam computed tomography. Sci World J. 2014;2014:2.
Emshoff R, Brandlmaier I, Gerhard S, Strobl H, Bertram S, Rudisch A. Magnetic resonance imaging predictors of temporomandibular joint pain. J Am Dent Assoc. 2003;134:705–14.
Roh H-S, Kim W, Kim Y-K, Lee J-Y. Relationships between disk displacement, joint effusion, and degenerative changes of the TMJ in TMD patients based on MRI findings. J Craniomaxillofac Surg. 2012;40:283–6.
Honda K, Natsumi Y, Urade M. Correlation between MRI evidence of degenerative condylar surface changes, induction of articular disc displacement and pathological joint sounds in the temporomandibular joint. Gerodontology. 2008;25:251–7.
Wiberg B, Wänman A. Signs of osteoarthrosis of the temporomandibular joints in young patients: a clinical and radiographic study. Oral Surg Oral Med Oral Pathol Oral Radiol. 1998;86:158–64.
Alexiou K, Stamatakis H, Tsiklakis K. Evaluation of the severity of temporomandibular joint osteoarthritic changes related to age using cone beam computed tomography. Dentomaxillofac Radiol. 2009;38:141–7.
Dworkin SF, Huggins KH, LeResche L, et al. Epidemiology of signs and symptoms in temporomandibular disorders: clinical signs in cases and controls. J Am Dent Assoc. 1990;120(3):273–81.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Soydan, D., Doğan, S., Canger, E.M. et al. Effect of internal derangements and degenerative bone changes on the minimum thickness of the roof of the glenoid fossa in temporomandibular joint. Oral Radiol 36, 25–31 (2020). https://doi.org/10.1007/s11282-019-00373-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-019-00373-6