Abstract
Introduction
Impaired kidney function is common in kidney-transplanted patients and complications of chronic kidney disease (CKD), such as mineral and bone disorders (MBD) are also prevalent in this population. Similarly to other stages of CKD, increasing evidence supports the association between MBD and cardiovascular risk after kidney transplantation as well. Still, little is known about the prevalence, clinical correlates of MBD and its management in transplanted patients. In this study, we aimed to examine the characteristics of MBD and its associations with clinical parameters in a large prevalent cohort of patients after kidney transplantation.
Methods
Nine hundred and ninety stable patients followed at a single kidney transplant outpatient clinic were included in the study. Detailed medical history, demographic data and routine laboratory results, including Ca, P and intact PTH were collected. Estimated GFR was calculated using the abbreviated MDRD formula, patients were stratified into three groups based on eGFR. Target levels for Ca, P and iPTH were based on CKD stages according to the NKF-K/DOQI guidelines. Standard statistical procedures, binomial and multinomial regressions were used in the analysis.
Results
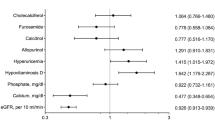
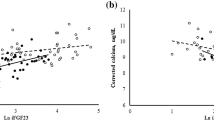
The mean age was 51 years, 57% were males and 21% were diabetic, with 72 months (median) post-transplantation. Most of the patients were in CKD stage 3. Serum phosphorus showed strong negative correlation with graft function in CKD stages 4–5 (r = −0.633, P < 0.001). Hyperphosphatemia was independently associated with the time spent on dialysis before transplantation, serum iPTH and CKD stages 4–5. iPTH showed negative correlation with eGFR in CKD stages 3–5 (rho = −0.289, P < 0.001) and weak positive correlation with time spent on dialysis prior to transplant (rho = 0.114, P < 0.001). Both hyperparathyroidism (42%) and relative hypoparathyroidism (15%) were frequent. The prescription of P-binders (6%) and vitamin D analogs (33%) was sporadic.
Conclusion
Disturbances of bone and mineral metabolism after transplantation are prevalent and are strongly correlated with the kidney function, similarly to non-transplanted CKD patients. MBD in this population is not adequately managed.
Similar content being viewed by others
References
Oniscu GC, Brown H, Forsythe JL (2005) Impact of cadaveric renal transplantation on survival in patients listed for transplantation. J Am Soc Nephrol 16:1859–1865
Karthikeyan V, Karpinski J, Nair RC et al (2004) The burden of chronic kidney disease in renal transplant recipients. Am J Transplant 4:262–269
Molnar MZ, Novak M, Ambrus C et al (2005) Anemia in kidney transplanted patients. Clin Transpl 19:825–833
Vanrenterghem Y (2009) Anemia after kidney transplantation. Transplantation 87:1265–1267
Helal I, Abderrahim E, Ben Hamida F et al (2009) The first year renal function as a predictor of long-term graft survival after kidney transplantation. Transplant Proc 41:648–650
Alonso A, Oliver J (2004) Causes of death and mortality risk factors. Nephrol Dial Transplant 19(Suppl 3):iii8–10
Sprague SM, Belozeroff V, Danese MD et al (2008) Abnormal bone and mineral metabolism in kidney transplant patients—a review. Am J Nephrol 28:246–253
Sadideen H, Covic A, Goldsmith D (2008) Mineral and bone disorder after renal transplantation: a review. Int Urol Nephrol 40:171–184
Bravo J, Esteban RJ, Medina A et al (2007) Successful kidney transplantation reduces hyperplastic parathyroid gland. Transplant Proc 39:125–131
Evenepoel P, Meijers BK, de Jonge H et al (2008) Recovery of hyperphosphatoninism and renal phosphorus wasting one year after successful renal transplantation. Clin J Am Soc Nephrol 3:1829–1836
Messa P, Sindici C, Cannella G et al (1998) Persistent secondary hyperparathyroidism after renal transplantation. Kidney Int 54:1704–1713
Torres A, Rodriguez AP, Concepcion MT et al (1998) Parathyroid function in long-term renal transplant patients: importance of pre-transplant PTH concentrations. Nephrol Dial Transplant 13(Suppl 3):94–97
Velasquez-Forero F, Mondragon A, Herrero B et al (1996) Adynamic bone lesion in renal transplant recipients with normal renal function. Nephrol Dial Transplant 11(Suppl 3):58–64
Monier-Faugere MC, Mawad H, Qi Q et al (2000) High prevalence of low bone turnover and occurrence of osteomalacia after kidney transplantation. J Am Soc Nephrol 11:1093–1099
Sanchez CP, Salusky IB, Kuizon BD et al (1998) Bone disease in children and adolescents undergoing successful renal transplantation. Kidney Int 53:1358–1364
Ojo AO, Hanson JA, Wolfe RA et al (2000) Long-term survival in renal transplant recipients with graft function. Kidney Int 57:307–313
Connolly GM, Cunningham R, McNamee PT et al (2009) Elevated serum phosphate predicts mortality in renal transplant recipients. Transplantation 87:1040–1044
Suwelack B, Gerhardt U, Witta J et al (2001) Effect of parathyroid hormone levels on carotid intima-media thickness after renal transplantation. Am J Hypertens 14:1012–1018
Suwelack B, Gerhardt U, Witta J et al (2001) Structural vessel wall properties in kidney transplant recipients depend on hyperparathyroidism. Transplant Proc 33:2310–2312
Levey A, Greene T, Kusek J et al (2000) A simplified equation to predict glomerular filtration rate from serum creatinine {Abstract}. J Am Soc Nephrol 11:155A
Levey A, Greene T, Kusek J et al (2003) National kidney foundation/KDOQI clinical practice guidelines. Guideline 16 in bone metabolism and disease in chronic kidney disease. Am J Kidney Dis 42:S1–S201
Block GA, Klassen PS, Lazarus JM et al (2004) Mineral metabolism, mortality, and morbidity in maintenance hemodialysis. J Am Soc Nephrol 15:2208–2218
Kestenbaum B, Sampson JN, Rudser KD et al (2005) Serum phosphate levels and mortality risk among people with chronic kidney disease. J Am Soc Nephrol 16:520–528
Ganesh SK, Stack AG, Levin NW et al (2001) Association of elevated serum PO(4), Ca × PO(4) product, and parathyroid hormone with cardiac mortality risk in chronic hemodialysis patients. J Am Soc Nephrol 12:2131–2138
Ketteler M, Biggar PH (2009) Dietary and pharmacological control of calcium and phosphate metabolism in predialysis stages of chronic kidney disease. Blood Purif 27:345–349
Lehmann G, Ott U, Stein G et al (2007) Renal osteodystrophy after successful renal transplantation: a histomorphometric analysis in 57 patients. Transplant Proc 39:3153–3158
Danese MD, Kim J, Doan QV et al (2006) PTH and the risks for hip, vertebral, and pelvic fractures among patients on dialysis. Am J Kidney Dis 47:149–156
Coco M, Rush H (2000) Increased incidence of hip fractures in dialysis patients with low serum parathyroid hormone. Am J Kidney Dis 36:1115–1121
Spasovski GB (2007) Bone health and vascular calcification relationships in chronic kidney disease. Int Urol Nephrol 39:1209–1216
Isakova T, Gutierrez OM, Chang Y et al (2009) Phosphorus binders and survival on hemodialysis. J Am Soc Nephrol 20:388–396
Neves KR, Graciolli FG, dos Reis LM et al (2007) Vascular calcification: contribution of parathyroid hormone in renal failure. Kidney Int 71:1262–1270
Smith DH, Johnson ES, Thorp ML et al (2009) Hyperparathyroidism in chronic kidney disease: a retrospective cohort study of costs and outcomes. J Bone Miner Metab 27:287–294
Cantor T, Yang Z, Caraiani N et al (2006) Lack of comparability of intact parathyroid hormone measurements among commercial assays for end-stage renal disease patients: implication for treatment decisions. Clin Chem 52:1771–1776
Lomonte C, Antonelli M, Vernaglione L et al (2005) Are low plasma levels of 25-(OH)vitamin D a major risk factor for hyperparathyroidism independent of calcitriol in renal transplant patients? J Nephrol 18:96–101
Acknowledgments
The authors thank the patients and the staff in the Department of Transplantation and Surgery, Semmelweis University, Budapest, Hungary for helping this survey. This study was supported by grant from the National Research Fund (OTKA) (TS-049785, F-68841), Ministry of Health (ETT 172/2006), the Hungarian Kidney Foundation and the Foundation for Prevention in Medicine. This paper was supported by the János Bolyai Research Scholarship of the Hungarian Academy of Sciences (Miklos Zsolt Molnar). Miklos Zsolt Molnar was recipient of the Hungarian Eötvös Scholarship.
Author information
Authors and Affiliations
Corresponding author
Additional information
Csaba Ambrus and Miklos Zsolt Molnar contributed equally to this work.
Rights and permissions
About this article
Cite this article
Ambrus, C., Molnar, M.Z., Czira, M.E. et al. Calcium, phosphate and parathyroid metabolism in kidney transplanted patients. Int Urol Nephrol 41, 1029–1038 (2009). https://doi.org/10.1007/s11255-009-9631-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-009-9631-0