Abstract
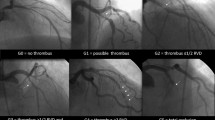
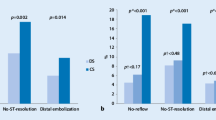
Background Mounting interest has emerged on the role of distal embolization as a major explanation of poor myocardial perfusion among patients with ST-segment elevation myocardial infarction (STEMI) undergoing primary angioplasty. The aim of the current study was to evaluate the relationship between vessel size, distal embolization, myocardial perfusion and clinical outcome in patients with STEMI treated by primary angioplasty. Methods Our population is represented by 1969 patients with STEMI undergoing primary stenting from 1997 to 2002. All clinical, angiographic, and follow-up data were prospectively collected. Results Vessel size was linearly associated with gender, diabetes, anterior infarction location, shorter time-delay, the rate of stenting and glycoprotein IIb-IIIa inhibitors. Small vessel size was associated with poor perfusion, despite lower rates of distal embolization. These data were confirmed after correction for confounding factors. The higher risk profile and poor myocardial perfusion contribute to explain the worse outcome observed in patients with smaller vessel size. Conclusions This study shows that in patients undergoing primary angioplasty for STEMI, small vessel size is associated with poor myocardial perfusion, despite less distal embolization, that contributes to explain the worse outcome observed among patients with small infarct related arteries.


Similar content being viewed by others
References
Grines CL, Browne KF, Marco J, Rothbaum D, Stone GW, O’Keefe J, Overlie P, Donohue B, Chelliah N, Timmis GC (1993) A comparison of immediate angioplasty with thrombolytic therapy for acute myocardial infarction. The Primary Angioplasty in Myocardial Infarction Study Group. N Engl J Med 328:673–679
Zijlstra F, Hoorntje JC, de Boer MJ, Reiffers S, Miedema K, Ottervanger JP, van’t Hof AW, Suryapranata H (1999) Long-term benefit of primary angioplasty as compared with thrombolytic therapy for acute myocardial infarction. N Engl J Med 341:1413–1419
Keeley EC, Boura JA, Grines CL (2003) Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review of 23 randomised trials. Lancet 361:13–20
De Luca G, van’t Hof AW, Ottervanger JP, Hoorntje JC, Gosselink AT, Dambrink JH, Zijlstra F, de Boer MJ, Suryapranata H (2005) Unsuccessful reperfusion in patients with ST-segment elevation myocardial infarction treated by primary angioplasty. Am Heart J 150:557–562
De Luca G, van’t Hof AW, de Boer MJ, Hoorntje JC, Gosselink AT, Dambrink JH, Ottervanger JP, Zijlstra F, Suryapranata H (2004) Impaired myocardial perfusion is a major explanation of the poor outcome observed in patients undergoing primary angioplasty for ST-segment-elevation myocardial infarction and signs of heart failure. Circulation 109:958–961
Kotani J, Mintz GS, Pregowski J, Kalinczuk L, Pichard AD, Satler LF, Suddath WO, Waksman R, Weissman NJ (2003) Volumetric intravascular ultrasound evidence that distal embolization during acute infarct intervention contributes to inadequate myocardial perfusion grade. Am J Cardiol 92(6):728–732
De Luca G, Suryapranata H, Stone GW, Antoniucci D, Tcheng JE, Neumann FJ, Van de Werf F, Antman EM, Topol EJ (2005) Abciximab as adjunctive therapy to reperfusion in acute ST-segment elevation myocardial infarction: a meta-analysis of randomized trials. JAMA 293:1759–1765
van’t Hof AW, Liem A, Suryapranata H, Hoorntje JC, de Boer MJ, Zijlstra F, on the behalf of the Zwolle Myocardial Infarction Study Group (1998) Angiographic assessment of myocardial reperfusion in patients treated with primary angioplasty for acute myocardial infarction. Myocardial blush grade. Circulation 97:2302–2306
Henriques JP, Zijlstra F, Ottervanger JP, de Boer MJ, van’t Hof AW, Hoorntje JC, Suryapranata H (2002) Incidence and clinical significance of distal embolization during primary angioplasty for acute myocardial infarction. Eur Heart J 23:1112–1117
De Luca G, van’t Hof AW, Ottervanger JP, Hoorntje JC, Gosselink AT, Dambrink JH, de Boer MJ, Suryapranata H (2005) Ageing, impaired myocardial perfusion, and mortality in patients with ST-segment elevation myocardial infarction treated by primary angioplasty. Eur Heart J 26:662–666
Brodie BR, Stuckey TD, Hansen C, Kissling G, Muncy D (2000) Influence of vessel size on early and late outcomes after primary angioplasty for acute myocardial infarction. J Invasive Cardiol 12:13–19
De Luca G, Suryapranata H, Zijlstra F, van’t Hof AW, Hoorntje JC, Gosselink AT, Dambrink JH, de Boer MJ, ZWOLLE Myocardial Infarction Study Group (2003) Symptom-onset-to-balloon time and mortality in patients with acute myocardial infarction treated by primary angioplasty. J Am Coll Cardiol 42:991–997
Roberts CS, Roberts WC (1980) Cross-sectional area of the proximal portions of the three major epicardial coronary arteries in 98 necropsy patients with different coronary events: relationship to heart weight, age and sex. Circulation 62:953–959
Sheifer S, Canos M, Weinfurt K, Arora U, Mandelsohn F, Gersh B, Weissman N (2000) Sex difference in coronary artery size assessed by intravascular ultrasound. Am Heart J 139(4):649–653
Dodge JTJ, Brown G, Bolson E, Dodge H (1992) Lumen diameter of normal human coronary arteries. Influence of age, sex, anatomic variation, and left ventricular hypertrophy or dilation. Circulation 86:232–246
Vijayalakshmi K, Kunadian B, Whittaker VJ, Williams D, Wright RA, Sutton AG, Hall JA, de Belder MA (2007) The impact of chronically diseased coronary arteries and stenting on the corrected TIMI frame count in elective coronary angiography and percutaneous coronary intervention procedures. Catheter Cardiovasc Interv 70:691–700
Langille B, O’Donnell F (1986) Reductions in arterial diameter produced by chronic decrease in blood flow are endothelium dependent. Science 231:405–407
White C, Wright C, Doty D, Hiratza L, Eastham C, Harrison D, Marcus M (1984) Does visual interpretation of the coronary arteriogram predict the physiologic importance of a coronary stenosis. N Engl J Med 310:819–824
Yokoyama I, Momomura S, Ohtake T et al (1997) Reduced myocardial flow reserve in non-insulin-dependent diabetes mellitus. J Am Coll Cardiol 30:1472–1477
Camici PG, Crea F (2007) Coronary microvascular dysfunction. N Engl J Med 356:830–840
Kotani J, Nanto S, Mintz GS, Kitakaze M, Ohara T, Morozumi T, Nagata S, Hori M (2002) Plaque gruel of atheromatous coronary lesion may contribute to the no-reflow phenomenon in patients with acute coronary syndrome. Circulation 106:1672–1677
Rezkalla SH, Kloner RA (2002) No-reflow phenomenon. Circulation 105:656–662
Kloner RA, Ganote CE, Jennings RB (1974) The “no reflow” phenomenon after temporary coronary occlusion in the dog. J Clin Invest 54:1496–1508
Michaels AD, Gibson CM, Barron HV (2000) Microvascular dysfunction in acute myocardial infarction: focus on the roles of platelet and inflammatory mediators in the no-reflow phenomenon. Am J Cardiol 85:50B–60B
Komatsu H, Koo A, Ghadishah E, Zeng H, Kuhlenkamp JF, Inoue M, Guth PH, Kaplowitz N (1992) Neutrophil accumulation in ischemic reperfused rat liver: evidence for a role for superoxide free radicals. Am J Physiol 262:G669–G676
Neumann FJ, Zohlnhöfer D, Fakhoury L, Ott I, Gawaz M, Schömig A (1999) Effect of glycoprotein IIb/IIIa receptor blockade on platelet–leukocyte interaction and surface expression of the leukocyte integrin Mac-1 in acute myocardial infarction. J Am Coll Cardiol 34:1420–1426
Neumann FJ, Blasini R, Schmitt C, Alt E, Dirschinger J, Gawaz M, Kastrati A, Schomig A (1998) Effect of glycoprotein IIb/IIIa receptor blockade on recovery of coronary flow and left ventricular function after the placement of coronary-artery stents in acute myocardial infarction. Circulation 98:2695–2701
Napodano M, Pasquetto G, Sacca S, Cernetti C, Scarabeo V, Pascotto P, Reimers B (2003) Intracoronary thrombectomy improves myocardial reperfusion in patients undergoing direct angioplasty for acute myocardial infarction. J Am Coll Cardiol 42:1395–1402
Antoniucci D, Valenti R, Migliorini A, Parodi G, Memisha G, Santoro GM, Sciagra R (2004) Comparison of rheolytic thrombectomy before direct infarct artery stenting versus direct stenting alone in patients undergoing percutaneous coronary intervention for acute myocardial infarction. Am J Cardiol 93:1033–1035
Lefèvre T, Garcia E, Reimers B, Lang I, di Mario C, Colombo A, Neumann FJ, Chavarri MV, Brunel P, Grube E, Thomas M, Glatt B, Ludwig J, X AMINE ST Investigators (2005) X-sizer for thrombectomy in acute myocardial infarction improves ST-segment resolution: results of the X-sizer in AMI for neglible embolization and optimal ST resolution (X AMINE ST) trial. J Am Coll Cardiol 46:246–252
Burzotta F, Trani C, Romagnoli E, Mazzari MA, Rebuzzi AG, De Vita M, Garramone B, Giannico F, Niccoli G, Biondi-Zoccai GG, Schiavoni G, Mongiardo R, Crea F (2005) Manual thrombus-aspiration improves myocardial reperfusion: the randomized evaluation of the effect of mechanical reduction of distal embolization by thrombus-aspiration in primary and rescue angioplasty (REMEDIA) trial. J Am Coll Cardiol 46:371–376
Noel B, Morice MC, Lefevre T (2005) Thromboaspiration in acute ST-elevation MI improves myocardial reperfusion. Circulation 112(Suppl II):519
Ikari Y, Kawano S, Sakurada M (2005) Thrombus aspiration prior to coronary intervention improves myocardial microcirculation in patients with ST Elevation Acute Myocardial Infarction, the VAMPIRE Study. Circulation 112(Suppl II):659
De Luca G, Suryapranata H, Stone GW, Antoniucci D, Neumann FJ, Chiariello M (2007) Adjunctive mechanical devices to prevent distal embolization in patients undergoing mechanical revascularization for acute myocardial infarction: a meta-analysis of randomized trials. Am Heart J 153:343–353
Ito H, Taniyama Y, Iwakura K, Nishikawa N, Masuyama T, Kuzuya T, Hori M, Higashino Y, Fujii K, Minamino T (1999) Intravenous nicorandil can preserve microvascular integrity and myocardial viability in patients with reperfused anterior wall myocardial infarction. J Am Coll Cardiol 33:654–660
Marzilli M, Orsini E, Marraccini P, Testa R (2000) Beneficial effects of intracoronary adenosine as an adjunct to primary angioplasty in acute myocardial infarction. Circulation 101:2154–2159
Umeda H, Iwase M, Izawa H, Katoh T, Gochi T, Toyama J, Yokoya M, Matsushita T, Ishiki R, Inagaki H, Murohara T, Yokota M (2007) Is it possible to predict which patients need distal protection during primary angioplasty? Int J Cardiol [Epub ahead of print]
Limbruno U, De Carlo M, Pistolesi S, Micheli A, Petronio AS, Camacci T, Fontanini G, Balbarini A, Mariani M, De Caterina R (2005) Distal embolization during primary angioplasty: histopathologic features and predictability. Am Heart J 150:102–108
Stone GW, Webb J, Cox DA, Brodie BR, Qureshi M, Kalynych A, Turco M, Schultheiss HP, Dulas D, Rutherford BD, Antoniucci D, Krucoff MW, Gibbons RJ, Jones D, Lansky AJ, Mehran R (2005) Enhanced myocardial efficacy and recovery by aspiration of liberated debris (EMERALD) investigators. Distal microcirculatory protection during percutaneous coronary intervention in acute ST-segment elevation myocardial infarction: a randomized controlled trial. JAMA 293:1063–1072
Selvanayagam JB, Cheng AS, Jerosch-Herold M, Rahimi K, Porto I, van Gaal W, Channon KM, Neubauer S, Banning AP (2007) Effect of distal embolization on myocardial perfusion reserve after percutaneous coronary intervention: a quantitative magnetic resonance perfusion study. Circulation 116:1458–1464
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
De Luca, G., Suryapranata, H., de Boer, MJ. et al. Impact of vessel size on distal embolization, myocardial perfusion and clinical outcome in patients undergoing primary angioplasty for ST-segment elevation myocardial infarction. J Thromb Thrombolysis 27, 198–203 (2009). https://doi.org/10.1007/s11239-007-0179-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-007-0179-5