Abstract
Introduction
Most existing measures of oral health focus solely on negative oral health, illness, and deficiencies and ignore positive oral health. In an attempt to commence exploration of this challenging field, an innovative instrument was developed, the “Positive Oral Health and Well-Being” (POHW) index. This study aimed to validate this instrument and to explore an initial model of the pathway between oral health attributes and positive oral health.
Methods
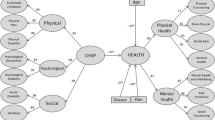
A cross-sectional, multicenter study (Israel, USA, and Germany), was conducted. Our conceptual model suggests that positive oral health attributes, which integrate with positive unawareness or positive awareness on the one hand and with positive perception on the other hand, may result via appropriate oral health behavior on positive oral health. The 17-item self-administered index was built on a theoretical concept by four experts from Israel and Germany. Reliability, factor, and correlation analyses were performed. For external correlations and to measure construct validity of the instrument, we utilized the oral health impact profile-14, self-perceived oral impairment, life satisfaction, self-perceived well-being, sociodemographic and behavioral data, and oral health status indices.
Results
Four hundred and seventy participants took part in our three-center study. The combined data set reliability analyses detected two items which were not contributing to the index reliability. Thus, we tested a 15-item construct, and a Cronbach’s α value of 0.933 was revealed. Primary factor analysis of the whole sample indicated three subconstructs which could explain 60 % of variance. Correlation analyses demonstrated that the POHW and OHIP-14 were strongly and negatively associated. The POHW correlated strongly and positively with general well-being, moderately with life satisfaction, and weakly with the perceived importance of regular dental checkups. It correlated moderately and negatively with perceived oral impairment, and marginally and negatively with dental caries experience (DMFT) and periodontal health status (CPI) scores. When DMFT and CPI clinical measurements were categorized, a higher score of POHW was revealed for better oral health.
Discussion
Our study introduced a new instrument with good reliability and sound correlations with external measures. This instrument is the first to allow measurability of positive instead of impaired oral health. We utilized subjective–psychological and functional–social measures. The current results indicate that by further exploring our conceptual model, POHW may be of importance for identifying patients with good and poor oral health, and building an effective and inexpensive strategy for prevention, by being able to evaluate the effect of interventions in a standardized way.

Similar content being viewed by others
References
Seligman, M. E. P. (2008). Applied psychology: An international review. International Association of Applied Psychology, 57, 3–18.
Antonovsky, A. (1979). Health, stress and coping. San Francisco, CA: Jossey-Bass.
Eriksson, M., & Lindstöm, B. (2005). Validity of Antonovsky’s sense of coherence scale: A systematic review. Journal of Epidemiology and Community Health, 59, 460–466.
Cohen, S., & Pressman, S. D. (2006). Positive affect and health. Current Directions in Psychological Science, 15, 122–125.
Seligman, M. E. P., & Csikszentmihalyi, M. (2000). Positive psychology. An introduction. American Psychologist, 55(1), 5–14.
Sheldon, K. M., & King, L. (2001). Why positive psychology is necessary. American Psychologists, 56(3), 2016–2017.
Fredrickson, B. L., & Joiner, T. (2002). Positive emotions trigger upward spirals toward emotional well-being. Journal of Personality and Social Psychology, 65(1), 45–55.
Barbara, L. (2004). Fredrickson: The broaden-and-build theory of positive emotions. Philosophical Transactions of the Royal Society of London. Series B, Biological sciences, 359(1449), 1367–1378.
Petersen, P. E., Bourgeois, D., Ogawa, H., Estupinan-Day, S., & Ndiyae, C. (2005). The global burden of oral disease and risks to oral health. Bulletin of the World Health Organization, 83, 661–669.
Sgan-Cohen, H. D., & Mann, J. (2007). Health, oral health and poverty. Journal of the American Dental Association, 138, 1437–1442.
Locker, D. (2008). Research on oral health and the quality of life: A critical overview. Community Dental Health, 25, 130–131.
Locker, D., & Gibson, B. (2006). The concept of positive health: A review and commentary on its application in oral health research. Community Dentistry and Oral Epidemiology, 34, 161–173.
Sischo, L., & Broder, H. L. (2011). Oral health-related quality of life: What, why, how, and future implications. Journal of Dental Research, 90, 124–1270.
McGrath, C., & Bedi, R. (2002). Population based norming of the UK oral health related quality of life measure (OHQoL-UK). British Dental Journal, 193, 521–524.
Slade, G. D. (1997). Derivation and validation of a short-form oral health impact profile. Community Dentistry and Oral Epidemiology, 25, 284–290.
Allen, P. F. (2003). Assessment of oral health related quality of life. Health and Quality of Life Outcomes, 1, 40.
Locker, D. (1988). Measuring oral health: A conceptual framework. Community Dental Health, 5, 3–18.
Baker, S. R., Gibson, B., & Locker, D. (2008). Is the oral health impact profile measuring up? Investigating the scale’s construct validity using structural equation modelling. Community Dentistry and Oral Epidemiology, 36, 532–541.
Rosenstock, I. M. (1974). Historical origins of the health belief model. Health Education Monograph, 2, 328.
Becker, M. H. (1974). The health belief model and personal health behavior. Health Education Monographs, 2, 324–508.
Rosenstock, I. M., Strecher, V. J., & Becker, M. H. (1988). Social learning theory and the Health Belief Model. Health Education Quarterly, 15(2), 175–183.
Paul-Dauphin, A., Guillemin, F., Virion, J. M., & Briancon, S. (1999). Bias and precision in visual analogue scales: A randomized controlled trial. American Journal of Epidemiology, 150, 1117–1127.
Bussing, A., Fischer, J., Haller, A., Heusser, P., Ostermann, T., & Matthiessen, P. F. (2009). Validation of the brief multidimensional life satisfaction scale in patients with chronic diseases. European Journal of Medical Research, 14, 171–177.
World Health Organization. (2004). Quality of life (WHOQOL)—BREF. Geneva.
World Health Organization. (1997). Oral health survey basic methods, 4 edn. Geneva.
Ostermann, T., Bussing, A., Beer, A. M., & Matthiessen, P. F. (2005). The Herdecke Questionnaire on Quality of Life (HLQ): Validation of factorial structure and development of a short form within a naturopathy treated in-patient collective. Health and Quality of Life Outcomes, 3, 40.
Fabrigar, L. R., Wegener, D. T., MacCallum, R. C., & Strahan, E. J. (1999). Evaluating the use of exploratory factor analysis in psychological research. Journal of Psychological Methods, 4, 272–299.
Cronbach, L. J. (1951). Coefficient α and the internal structure of tests. Psychometrika, 16, 297–334.
Cohen, L. K., & Jago, J. D. (1976). Toward the formulation of sociodental indicators. International Journal of Health Services, 6, 681–698.
Acknowledgments
We are grateful to Dr. Georg Gassman for his input during the development of the POHW items.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zini, A., Büssing, A., Chay, C. et al. Validation of an innovative instrument of Positive Oral Health and Well-Being (POHW). Qual Life Res 25, 847–858 (2016). https://doi.org/10.1007/s11136-015-1142-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-015-1142-0