Abstract
Background
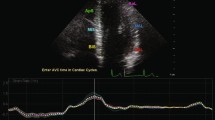
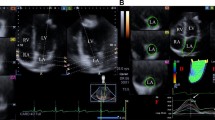
Speckle tracking echocardiography (STE) allows for the study of myocardial strain (ε), a marker of early and subclinical ventricular systolic dysfunction. Cardiac disease may be present in patients with acromegaly; however, STE has never been used to evaluate these patients.
Objective
To evaluate left ventricular (LV) global longitudinal strain in patients with active acromegaly with normal LV systolic function.
Design
Cross-sectional clinical study.
Methods
Patients with active acromegaly with no detectable heart disease and a control group were matched for age, gender, arterial hypertension and diabetes mellitus underwent STE. Global LV longitudinal ε (GLS), left ventricular mass index (LVMi), left ventricular ejection fraction (LVEF) and relative wall thickness (RWT) were obtained via two-dimensional (2D) echocardiography using STE.
Results
Thirty-seven patients with active acromegaly (mean age 45.6 ± 13.8; 48.6% were males) and 48 controls were included. The mean GLS was not significantly different between the acromegaly group and the control group (in %, −20.1 ± 3.1 vs. −19.4 ± 2.2, p = 0.256). Mean LVMi was increased in the acromegaly group (in g/m2, 101.6 ± 27.1 vs. 73.2 ± 18.6, p < 0.01). There was a negative correlation between LVMi and GLS (r = −0.39, p = 0.01).
Conclusions
Acromegaly patients, despite presenting with a higher LVMi when analyzed by 2D echocardiography, did not present with impairment in the strain when compared to a control group; this finding indicates a low chance of evolution to systolic dysfunction and agrees with recent studies that show a lower frequency of cardiac disease in these patients.




Similar content being viewed by others
References
Colao A, Ferone D, Marzullo P, Lombardi G (2004) Systemic complications of acromegaly: epidemiology, pathogenesis, and management. Endocr Rev 25:102–152
Holdaway IM, Rajasoorya RC, Gamble GD (2004) Factors influencing mortality in acromegaly. J Clin Endocrinol Metab 89:667–674
Dekkers OM, Biermasz NR, Pereira AM, Romijn JA, Vandenbroucke JP (2008) Mortality in acromegaly: a metaanalysis. J Clin Endocrinol Metab 93:61–67
McCabe J, Ayuk J, Sherlock M (2016) Treatment factors that influence mortality in acromegaly. Neuroendocrinology 103:66–74
Hurchard H (1895) Anatomie pathologique lesions et troubles cardiovasculares de l’acromegalie. J Prat 9:249–251
Lie JTG, S J (1980) Pathology of heart in acromegaly: anatomic findings in 27 autopsied patients. Am Heart J 100:41–52
Colao A, Marzullo P, Di Somma C, Lombardi G Growth hormone and the heart. Clin Endocrinol 54, 137–154 (2001)
Colao A SL, Cuocolo A, Spiezia S, Pivonello R, di Smma C, Bonaduce D, Salvatore M, Lombardi G (2002) Cardiovascular consequences of early-onset growth hormone excess. J Clin Endocrinol Metab 87:3097–3104
Matta MP, Caron P (2003) Acromegalic cardiomyopathy : a review of the literature. Pituitary 6:203–207
Mosca S, Paolillo S, Colao A, Bossone E, Cittadini A, Iudice FL, Parente A, Conte S, Rengo G, Leosco D, Trimarco B, Filardi PP (2013) Cardiovascular involvement in patients affected by acromegaly: an appraisal. Int J Cardiol 167:1712–1718
Colao A, Cuocolo A, Marzullo P, Nicolai E, Ferone D, Della Morte AM, Petretta M, Salvatore M, Lombardi G (1999) Impact of patient’s age and disease duration on cardiac performance in acromegaly: a radionuclide angiography study. J Clin Endocrinol Metab 84:1518–1523
Colao A, Cuocolo A, Marzullo P, Nicolai E, Ferone D, Della Morte AM, Pivonello R, Salvatore M, Lombardi G (2001) Is the acromegalic cardiomyopathy reversible? Effect of 5-Year normalization of growth hormone and insulin-like growth factor I levels on cardiac performance. J Clin Endocrinol Metab 86:1551–1557
Bihan H, Espinosa C, Valdes-Socin H, Salenave S, Young J, Levasseur S, Assayag P, Beckers A, Chanson P (2004) Long-term outcome of patients with acromegaly and congestive heart failure. J Clin Endocrinol Metab 89:5308–5313
Mann DL, Zipes DP, Libby P, Bonow RO (2015) Braunwald’s heart disease: a textbook of cardiovascular medicine. 4th edn. Elservier, Amsterdam
Geyer H, Caracciolo G, Abe H, Wilansky S, Carerj S, Gentile F, Nesser HJ, Khandheria B, Narula J, Sengupta PP (2010) Assessment of myocardial mechanics using speckle tracking echocardiography: fundamentals and clinical applications. J Am Soc Echocardiogr 23:351–369, quiz 453–355
de Almeida AL, Gjesdal O, Mewton N, Choi EY, Teixido-Tura G, Yoneyama K, Lima JA (2013) Speckle-Tracking pela Ecocardiografia Bidimensional – Aplicações Clínicas. Revista Brasileira Ecocardiogr imagem cardiovasc 26:38–49
Katznelson L, Laws ER Jr, Melmed S, Molitch ME, Murad MH, Utz A, Wass JA, Endocrine S (2014) Acromegaly: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 99:3933–3951
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL, Jones DW, Materson BJ, Oparil S, Wright JT, Roccella EJ, National Heart, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure, National High Blood Pressure Education Program Coordinating Committee (2003) The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. Jama. 289:2560–2572
American Diabetes Association (2010) Diagnosis and classification of diabetes mellitus. Diabetes Care 33(Suppl 1):S62–69
Lang, RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, Picard MH, Roman MJ, Seward J, Shanewise JS, Solomon SD, Spencer KT, Sutton MS, Stewart WJ, Chamber Quantification Writing Group, American Society of Echocardiography’ Guidelines and Standards Commiitee, European Association of Echocardiography (2005) Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr. 18:1440–1463
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, Flachskampf FA, Foster E, Goldstein SA, Kuznetsova T, Lancellotti P, Muraru D, Picard MH, Rietzschel ER, Rudski L, Spencer KT, Tsang W, Voigt JU (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr 28:1–39.e14
Yingchoncharoen T, Agarwal S, Popovic ZB, Marwick TH (2013) Normal ranges of left ventricular strain: a meta-analysis. J Am Soc Echocardiogr 26:185–191
Marwick TH, Leano RL, Brown J, Sun JP, Hoffmann R, Lysyansky P, Becker M, Thomas JD (2009) Myocardial strain measurement with 2-dimensional speckle-tracking echocardiography: definition of normal range. JACC Cardiovasc Imaging 2:80–84
Dalen H, Thorstensen A, Aase SA, Ingul CB, Torp H, Vatten LJ, Stoylen A (2010) Segmental and global longitudinal strain and strain rate based on echocardiography of 1266 healthy individuals: the HUNT study in Norway. Eur J Echocardiogr 11:176–183
Cheng S, Larson MG, McCabe EL, Osypiuk E, Lehman BT, Stanchev P, Aragam J, Benjamin EJ, Solomon SD, Vasan RS (2013) Age- and sex-based reference limits and clinical correlates of myocardial strain and synchrony: the Framingham Heart Study. Circ Cardiovasc Imaging 6:692–699
dos Santos Silva CM, Gottlieb I, Volschan I, Kasuki L, Warszawski L, Balarini Lima GA, Xavier SS, Pedrosa RC, Neto LV, Gadelha MR (2015) Low frequency of cardiomyopathy using cardiac magnetic resonance imaging in an acromegaly contemporary cohort. J Clin Endocrinol Metab 100:4447–4455
Marwick TH, Venn AJ (2015) The strain of detecting early target organ damage in hypertension. J Am Coll Cardiol 65:2688–2690
Mignot A, Donal E, Zaroui A, Reant P, Salem A, Hamon C, Monzy S, Roudaut R, Habib G, Lafitte S (2010) Global longitudinal strain as a major predictor of cardiac events in patients with depressed left ventricular function: a multicenter study. J Am Soc Echocardiogr 23:1019–1024
Ersboll M, Valeur N, Andersen MJ, Mogensen UM, Vinther M, Svendsen JH, Moller JE, Kisslo J, Velazquez EJ, Hassager C, Sogaard P, Kober L (2013) Early echocardiographic deformation analysis for the prediction of sudden cardiac death and life-threatening arrhythmias after myocardial infarction. JACC Cardiovasc Imaging 6:851–860
Almeida AL, Silva VA, Souza Filho AT, Rios VG, Lopes JR, Afonseca SO, Cunha DD, Mendes MO, Miranda DL, Júnior S (2015) Disfunção Ventricular Subclínica Detectada por Speckle Tracking Dois Anos após Uso de Antraciclina. Arq Bras Cardiologia 104:274–283
Jurcut R, Galoiu S, Florian A, Vladaia A, Ionita OR, Amzulescu MS, Baciu I, Popescu BA, Coculescu M, Ginghina C (2014) Quantifying subtle changes in cardiovascular mechanics in acromegaly: a Doppler myocardial imaging study. J Endocrinol Invest 37:1081–1090
Mercuro G, Zoncu S, Colonna P, Cherchi P, Marlotti S, Pigliaru F, Petrini L, Iliceto S (2000) Cardiac dysfunction in acromegaly- evidence by pulsed wave tissue Doppler imaging. Eur J Endocrinol 143:363–369
Galderisi M, Vitale G, Bianco A, Pivonello R, Lombardi G, Divitiis O, Colao A (2006) Pulsed tissue Doppler identifies subclinical myocardial biventricular dysfunction in active acromegaly. Clin Endocrinol 64:390–397
Bogazzi F, Di Bello V, Palagi C, Donne MG, Di Cori A, Gavioli S, Talini E, Cosci C, Sardella C, Brogioni S, Mariani M, Martino E (2005) Improvement of intrinsic myocardial contractility and cardiac fibrosis degree in acromegalic patients treated with somatostatin analogues: a prospective study. Clin Endocrinol 62:590–596
Edvardsen T, Gerber BL, Garot J, Bluemke DA, Lima JA, Smiseth OA (2002) Quantitative assessment of intrinsic regional myocardial deformation by Doppler strain rate echocardiography in humans: validation against three-dimensional tagged magnetic resonance imaging. Circulation 106:50–56
Amundsen BH, Helle-Valle T, Edvardsen T, Torp H, Crosby J, Lyseggen E, Støylen A, Ihlen H, Lima JA, Smiseth OA, Slørdahl SA (2006) Noninvasive myocardial strain measurement by speckle tracking echocardiography: validation against sonomicrometry and tagged magnetic resonance imaging. J Am Coll Cardiol 47:789–793
Sacca L, Cittadini A, Fazio S (1994) Growth hormone and the heart. Endocr Rev 15:555–573
Terzolo M, Avonto L, Matrella C, Pozzi R, Luceri S, Borretta G, Pecchio F, Ugliengo G, Magro GP, Reimondo G (1995) Doppler echocardiographic patterns in patients with acromegaly. J Endocrinol Invest 18:613–620
Colao A, Baldelli R, Marzullo P, Ferretti E, Ferone D, Gargiulo P, Petretta M, Tamburrano G, Lombardi G, Liuzzi A (2000) Systemic hypertension and impaired glucose tolerance are independently correlated to the severity of the acromegalic cardiomyopathy. J Clin Endocrinol Metab 85:193–199
Pereira AM, van Thiel SW, Lindner JR, Roelfsema F, van der Wall EE, Morreau H, Smit JW, Romijn JA, Bax JJ (2004) Increased prevalence of regurgitant valvular heart disease in acromegaly. J Clin Endocrinol Metab 89:71–75
Casini AF, Araújo PB, Fontes R, Xavier SS, Gadelha MR (2006) Alteracoes Morfologicas e Funcionais Cardiacas e Análise dos Fatores Determinantes de Hipertrofia Ventricular Esquerda em 40 Pacientes com Acromegalia. Arq Bras Endocrinol Metab 50:82–90
Colao A, Grasso LF (2011) Aortic root ectasia in patients with acromegaly: an emerging complication. Clin Endocrinol 75:420–421
Akdeniz B, Gedik A, Turan O, Ozpelit E, Ikiz AO, Itil O, Badak O, Baris N, Çömlekçi A (2012) Evaluation of left ventricular diastolic function according to new criteria and determinants in acromegaly. Int Heart J 53:299–305
López-Velasco R, Escobar-Morreale HF, Vega B, Villa E, Sancho JM, Moya-Mur JL, García-Robles R (1997) Cardiac involvement in acromegaly: specific myocardiopathy or consequence of systemic hypertension? J Clin Endocrinol Metab 82:1047–1053
Nascimento GC, de Oliveira MT, Carvalho VC, Lopes MH, Sá AM, Souza MT, Ferreira AS, Ferreira PA, Faria MD (2013) Acromegalic cardiomyopathy in an extensively admixed population: is there a role for GH/IGF-I axis? Clin Endocrinol 78:94–101
Sacca L, Fazio S, Longobardi S, Cittadini A (1999) Cardiac effects of growth hormone in physiology and in heart failure. Endocrine J 46(Suppl):S5–S10
Sacca L, Napoli R, Cittadini A (2003) Growth hormone, acromegaly, and heart failure: an intricate triangulation. Clin Endocrinol 59:660–671
Fazio S, Cittadini A, Cuocolo A, Merola B, Sabatini D, Colao A, Biondi B, Lombardi G, Saccà L (1994) Impaired cardiac performance is a distinct feature of uncomplicated acromegaly. J Clin Endocrinol Metab 79:441–446
Fazio S, Cittadini A, Biondi B, Palmieri EA, Riccio G, Bonè F, Oliviero U, Saccà L (2000) Cardiovascular effects of short-term growth hormone hypersecretion. J Clin Endocrinol Metab 85:179–182
Omerovic E, Bollano E, Mobini R, Kujacic V, Madhu B, Soussi B, Fu M, Hjalmarson A, Waagstein F, Isgaard J (2000) Growth hormone improves bioenergetics and decreases catecholamines in postinfarct rat hearts. Endocrinology 141:4592–4599
Fazio S, Sabatini D, Capaldo B, Vigorito C, Giordano A, Guida R, Pardo F, Biondi B, Saccà L (1996) A preliminary study of growth hormone in the treatment of dilated cardiomyopathy. N Engl J Med 334:809–814
Imanishi R, Ashizawa N, Ohtsuru A, Seto S, Akiyama-Uchida Y, Kawano H, Kuroda H, Nakashima M, Saenko VA, Yamashita S, Yano K (2004) GH suppresses TGF-beta-mediated fibrosis and retains cardiac diastolic function. Mol Cell. Endocrinol 218:137–146
Bogazzi F, Lombardi M, Strata E, Aquaro G, Di Bello V, Cosci C, Sardella C, Talini E, Martino E (2008) High prevalence of cardiac hypertophy without detectable signs of fibrosis in patients with untreated active acromegaly: an in vivo study using magnetic resonance imaging. Clin Endocrinol 68:361–368
Perdrix L, Mansencal N, Cocheteux B, Chatellier G, Bissery A, Diebold B, Mousseaux E, Abergel E (2011) How to calculate left ventricular mass in routine practice? An echocardiographic versus cardiac magnetic resonance study. Arch Cardiovasc Dis 104:343–351.
Bottini PB, Carr AA, Prisant LM, Flickinger FW, Allison JD, Gottdiener JS (1995) Magnetic resonance imaging compared to echocardiography to assess left ventricular mass in the hypertensive patient. Am J Hypertens 8:221–228
Armstrong AC, Gidding S, Gjesdal O, Wu C, Bluemke DA, Lima JA (2012) LV mass assessed by echocardiography and CMR, cardiovascular outcomes, and medical practice. JACC Cardiovasc Imaging 5:837–848
Arosio M, Reimondo G, Malchiodi E, Berchialla P, Borraccino A, De Marinis L, Pivonello R, Grottoli S, Losa M, Cannavo S, Minuto F, Montini M, Bondanelli M, De Menis E, Martini C, Angeletti G, Velardo A, Peri A, Faustini-Fustini M, Tita P, Pigliaru F, Borretta G, Scaroni C, Bazzoni N, Bianchi A, Appetecchia M, Cavagnini F, Lombardi G, Ghigo E, Beck-Peccoz P, Colao A, Terzolo M, Italian Study Group of Acromegaly (2012) Predictors of morbidity and mortality in acromegaly: an Italian survey. Eur J Endocrinol 167:189–198
Varadhan L, Reulen RC, Brown M, Clayton RN (2016) The role of cumulative growth hormone exposure in determining mortality and morbidity in acromegaly: a single centre study. Pituitary 19:251–261
Funding
The research has not received funding from any organization or company and was sponsored by the authors themselves.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
MRG has received unrestricted research grants and lecture fees from Novartis, Ipsen and Pfizer, has participated on advisory boards of Novartis and Ionis, and is a principal investigator in clinical trials by Novartis and Ipsen. The other authors have no conflicts of interest.
Ethical approval
All procedures performed were in accordance with the ethical standards of the HUCFF/UFRJ ethical committee and with the 1964 Helsinki declaration and its later amendments. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Volschan, I.C.M., Kasuki, L., Silva, C.M.S. et al. Two-dimensional speckle tracking echocardiography demonstrates no effect of active acromegaly on left ventricular strain. Pituitary 20, 349–357 (2017). https://doi.org/10.1007/s11102-017-0795-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-017-0795-9