Abstract
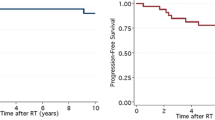
The goal of the study is to examine the practice pattern and survival outcome of adult and pediatric patients with intracranial germinoma. Patients from the National Cancer Database (NCDB) brain tumor registry between the years 2004–2014 with intracranial germinoma were extracted for analysis. Patients who had distant metastasis, received no treatments, or only surgery/chemotherapy alone were excluded. An age cutoff of > 21 years old was used to define the pediatric population. Patients were stratified by the treatments radiation therapy alone (RT) and chemotherapy followed by radiation therapy (C + RT). 445 patients with intracranial germinoma meeting our inclusion criteria were identified. Of the adult patients, 65.7% received RT and 34.3% received C + RT, compared to the pediatric patients, where 31.8% received RT and 68.2% received C + RT. Those patients who received C + RT had a lower radiation dose compared to the RT group (p < 0.001). The 5 and 10 year overall survival (OS) for the entire cohort was 92.6 and 87.9%, respectively. Univariate analysis demonstrated improved OS with younger age, private insurance, C + RT treatment, and pediatric patients. Only age and insurance type remained significant on multivariate analysis. The 5 year OS was 92.6% (RT) versus 97.2% (C + RT) (p = 0.307) and 83.4% (RT) versus 95.4% (C + RT) (p = 0.122) in the pediatric and adult patients, respectively. There is a higher use of C + RT with an accompanied reduction in RT dose in the treatment of intracranial germinoma. There is no difference in survival between the treatment approaches of RT or C + RT in the NCDB patient cohort.


Similar content being viewed by others
References
Villano JL et al (2008) Malignant pineal germ-cell tumors: an analysis of cases from three tumor registries. Neuro-Oncol 10(2):121–130
Echevarria ME, Fangusaro J, Goldman S (2008) Pediatric central nervous system germ cell tumors: a review. Oncologist 13(6):690–699
Bamberg M et al (1999) radiation therapy for intracranial germinoma: results of the german cooperative prospective trials MAKEI 83/86/89. J Clin Oncol 17(8):2585–2585
Rogers S, Mosleh-Shirazi M, Saran F (2005) Radiotherapy of localised intracranial germinoma: time to sever historical ties? Lancet Oncol 6(7):509–519
Balmaceda C et al (1996) Chemotherapy without irradiation–a novel approach for newly diagnosed CNS germ cell tumors: results of an international cooperative trial. The First International Central Nervous System Germ Cell Tumor Study. J Clin Oncol 14(11):2908–2915
da Silva NS et al (2010) Primary chemotherapy for intracranial germ cell tumors: results of the third international CNS germ cell tumor study. Pediatr Blood Cancer 54(3):377–383
Laughton SJ et al (2008) Endocrine outcomes for children with embryonal brain tumors after risk-adapted craniospinal and conformal primary-site irradiation and high-dose chemotherapy with stem-cell rescue on the SJMB-96 Trial. J Clin Oncol 26(7):1112–1118
Ellenberg L et al (2009) Neurocognitive status in long-term survivors of childhood CNS malignancies: a report from the Childhood Cancer Survivor Study. Neuropsychology 23(6):705–717
Kretschmar C, Kleinberg L, Greenberg M, Burger P, Holmes E, Wharam M (2007) Pre-radiation chemotherapy with response-based radiation therapy in children with central nervous system germ cell tumors: a report from the Children’s Oncology Group. Pediatr Blood Cancer 48(3):285–291
Calaminus G et al (2013) SIOP CNS GCT 96: final report of outcome of a prospective, multinational nonrandomized trial for children and adults with intracranial germinoma, comparing craniospinal irradiation alone with chemotherapy followed by focal primary site irradiation for patients with localized disease. Neuro-Oncology 15(6):788–796
Leonard M, Dhall G, Ute B (2016) ACNS1123: Phase 2 Trial of Response-Based Radiation Therapy for Patients with Localized Central Nervous System Germ Cell Tumors. https://www.childrensoncologygroup.org/index.php/acns1123. Accessed 15 Dec 2016.
Ogawa K et al (2004) Long-term results of radiotherapy for intracranial germinoma: a multi-institutional retrospective review of 126 patients. Int J Radiat Oncol 58(3):705–713
Yang JC, Terezakis SA, Dunkel IJ, Gilheeney SW, Wolden SL (2016) intensity-modulated radiation therapy with dose painting: a brain-sparing technique for intracranial germ cell tumors: DP-IMRT for intracranial GCT. Pediatr Blood Cancer 63(4):646–651
Takizawa D et al (2017) A comparative study of dose distribution of PBT, 3D-CRT and IMRT for pediatric brain tumors. Radiat Oncol 12(1):40
Beltran C, Naik M, Merchant TE (2010) Dosimetric effect of setup motion and target volume margin reduction in pediatric ependymoma. Radiother Oncol 96(2):216–222
Kahalley LS et al (2016) Comparing intelligence quotient change after treatment with proton versus photon radiation therapy for pediatric brain tumors. J Clin Oncol 34(10):1043–1049
Park Y, Yu E-S, Ha B, Park H-J, Kim J-H, Kim J-Y (2017) Neurocognitive and psychological functioning of children with an intracranial germ cell tumor. Cancer Res Treat. https://doi.org/10.1111/10.4143/crt.2016.204
O’Neil S et al (2011) Neurocognitive outcomes in pediatric and adolescent patients with central nervous system germinoma treated with a strategy of chemotherapy followed by reduced-dose and volume irradiation. Pediatr Blood Cancer 57(4):669–673
Eom K-Y et al (2008) Upfront chemotherapy and involved-field radiotherapy results in more relapses than extended radiotherapy for intracranial germinomas: modification in radiotherapy volume might be needed. Int J Radiat Oncol 71(3):667–671
Austin MT et al (2016) Health disparities and impact on outcomes in children with primary central nervous system solid tumors. J Neurosurg Pediatr 18(5):585–593
Bona K, Blonquist TM, Neuberg DS, Silverman LB, Wolfe J (2016) Impact of socioeconomic status on timing of relapse and overall survival for children treated on Dana-Farber Cancer Institute ALL Consortium Protocols (2000–2010): socioeconomic status and early relapse in ALL. Pediatr Blood Cancer 63(6):1012–1018
Chao C, Chiu V, Xu L, Cooper RM (2015) Survival Differences by race/ethnicity and neighborhood socioeconomic status in adolescents and young adults diagnosed with non-hodgkin lymphoma. J Adolesc Young Adult Oncol 4(2):76–83
Lee JM, Wang X, Ojha RP, Johnson KJ (2017) The effect of health insurance on childhood cancer survival in the United States: insurance and childhood cancer survival. Cancer. https://doi.org/10.1002/cncr.30925
Rosenberg AR, Kroon L, Chen L, Li CI, Jones B (2015) Insurance status and risk of cancer mortality among adolescents and young adults: AYA insurance status. Cancer 121(8):1279–1286
Koroukian SM, Bakaki PM, Raghavan D (2012) Survival disparities by medicaid status: an analysis of 8 cancers. Cancer 118(17):4271–4279
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Wang, W.G., Ye, H. & Chinnaiyan, P. Practice patterns and survival outcomes of intracranial germinoma: an analysis of the National Cancer Database. J Neurooncol 137, 77–82 (2018). https://doi.org/10.1007/s11060-017-2696-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-017-2696-1