Abstract
The invasion- and apoptosis-associated thromboxane synthase gene encoding an enzyme of the arachidonic acid pathway has been implicated in glioma progression. Furegrelate, a specific inhibitor of thromboxane synthase, blocks cell motility, induces apoptosis and increases sensitivity to drug induced apoptosis in human glioma cells in vitro. The impact of furegrelate on the sensitivity of human glioma cells to γ-irradiation was analyzed using colony formation assay in vitro and an orthotopic mouse model in vivo. Pre-treatment of glioma cells with furegrelate increases radiation sensitivity of cultured glioma cells. Treatment of experimental gliomas with suboptimal doses of radiation and furegrelate results in a significant decrease in tumor volumes compared to untreated controls. Thus, the specific thromboxane synthase inhibitor furegrelate increases death response induced by γ-radiation in glioma cells in vitro and sensitizes experimental gliomas to radiation treatment in vivo.
Similar content being viewed by others
Introduction
Prostanoids synthesis appears to be important in pathogenesis and progression of cancer because arachidonic acid metabolites affect several important cellular behaviors such as mitogenesis, cellular adhesion, invasion, and apoptosis [1]. In many cancers the levels of prostanoid synthesis exceed those of normal tissues. In human glioma cells cyclooxygenase (COX) and thromboxane synthase (TXSA) are strongly overexpressed and expression levels of these enzymes of the arachidonic acid pathway correlate with the grade of malignancy [2, 3]. Thromboxane A2 (TXA-2), one of the downstream metabolites of COX, is synthetisized from prostaglandin H2 endoperoxide (PGH2) by TXSA. One of the physiological functions of TXA-2 is to promote vasoconstriction and platelet aggregation. Now an important role of TXSA as a tumor promoting factor emerges. Experimental overexpression of TXSA promotes tumor growth in vivo [4], and it appears that high levels of TXSA enhance angiogenesis and increase the invasive potential of neoplastic cells [2, 3, 5–7]. In human gliomas TXSA renders tumor cells resistant to apoptosis and we have demonstrated that specific inhibitors of TXSA block motility and sensitize migration arrested glioma cells to apoptotic cell death [7]. The role of TXSA as an invasion- and apoptosis-associated gene is further substantiated by our findings that the gene encoding for TXSA is a target gene for both the tumor suppressor gene p53 and the proto-oncogenic factor ets-1 [8]. p53 and ets-1 co-regulate TXSA in an antagonistic fashion with ets-1 being a potent transcriptional activator and p53 inhibiting ets-1 dependent transcription. This implicates that the loss of p53’s negative control over ets-1 dependent transcription may lead to the acquisition of an invasive and apoptosis resistant phenotype in tumor cells. Therefore, TXSA emerges as a regulatory element at intersecting pathways of tumor promoting and tumor suppressing signaling cascades. Targeted inhibition of the TXSA activity may therefore increase the susceptibility of glioma cells to conventional chemo- and radiation therapy.
We have previously shown that furegrelate, a pharmacological inhibitor of TXSA which impedes the metabolic conversion of cyclic endoperoxide into TXA-2, induces apoptosis in glioma cell lines in vitro [2, 3, 5–7]. In this study, we examined the effects of furegrelate on the radio response in glioma cells. Our results demonstrate that treatment with the specific TXSA inhibitor furegrelate sensitizes glioma cell lines to γ-radiation in vitro and in vivo, as shown in an experimental glioma mouse model.
Material and methods
Cell culture
Human glioma cell lines were propagated in minimal essential medium (MEM, Biochem, Berlin, Germany) with 10% fetal calf serum (FCS) and were passaged using trypsinization at regular intervals depending on growth characteristics. Normal human astrocytes were cultured as described in [9]. The specific TXSA inhibitor furegrelate (Sodium 5-(3′-pyridinylmethyl) benzofuran-2-carboxylate) (Sigma # F-3764, Deisenhofer, Germany) was prepared according to manufacturer’s instructions for use in tissue culture. The concentration range for functional assays was based on our previous studies using human glioma cell lines [2, 3, 7, 10].
Colony formation and irradiation
Human glioma cell lines and human astrocytes were seeded in 10 cm culture dishes and were maintained till sub-confluence. The cultures were pre-treated with the TXSA inhibitor furegrelate at doses and treatment schedules indicated in the figures and the cultures were irradiated according to the schedules indicated. Following radiation treatment cells were trypsinized, washed in PBS and counted. A single cell suspension was plated in MEM containing 10% FCS into six well plates at a density of 5 × 105 cells per well. The cultures were maintained for two weeks, and then the cells were fixed in 1% glutaraldehyde and stained using crystal violet. The number of colonies was counted and the surviving fraction was calculated as the percentage of colonies of the non-irradiated control. Values indicated represent the mean of triplicate wells, error bars indicate standard deviation.
Cell migration
Cell migration was quantified using a monolayer migration assay, which measures the dispersion of cell populations on surfaces [9]. Ten-well HTC-treated slides (Dynex Technologies, Denkendorf, Germany) were coated with AES (3-aminopropyltriethoxysilane) (Sigma #A-3648) to optimize protein and cell adhesion. Slides were passively coated with human laminin (100 μg/ml) and a cell sedimentation manifold (CSM) was placed over the slides containing 50 μl of culture media. Cells were seeded in a volume of 1 μl MEM (2,000 cells) and slides were incubated for 48 h at 37°C. The CSM was removed and the circular area occupied by attached cells in each well was measured using an image analysis system. The cell populations were measured as the radius in μm of the circular area covered by migrating cells. Serial images were captured for up to 48 h. Quantitative migration scores were calculated as the increase in radius beyond the initial radius. Values indicated represent the mean of triplicate wells, error bars indicate standard deviation.
Assessment of cell death
A photometric enzyme-immunoassay was used for quantitative in vitro determination of cytoplasmic histone-associated-DNA fragments (Boehringer, Mannheim, Germany) [11]. In this assay the intracellular enrichment of mono- and oligo-nucleosomes, which occurs after induction of endogenous endonucleases, is due to the fact that in apoptosis DNA degradation occurs several hours before plasma membrane breakdown. In contrast, necrotic cell death results in early release of fragmented DNA into the culture supernatant [7]. 20,000 cells were seeded into 96-well plates and cells were allowed to adhere for 4 h before treatment. Cultures were rinsed and compounds were added at concentrations indicated in the figures. Furegrelate doses higher than 0.75 mg/ml were found toxic in cell culture conditions of previous studies and were not used in this study [2, 3, 7, 10]. After incubation (4–48 h) cultures were centrifuged at 200× g and culture supernatants were collected. Cells were lysed and 20 μl of lysate or 20 μl of corresponding supernatant were used in a Cell Death Detection ELISAPlus (Boehringer, Mannheim, Germany) according to manufacturer’s instructions. A specific enrichment factor of mono- and oligo-nucleosomes released into the cytoplasm was calculated by absorbance of treated sample divided by absorbance of the corresponding untreated control. Data reported represent the mean of triplicate wells per experimental determination.
RT-PCR
Total RNA was isolated from monolayer cultures of U87 and quantified by absorbance measurement at 260/280 nm. RT synthesis of cDNA was done using a First Strand Synthesis Kit (Stratagene, La Jolla, CA, USA). Primers for TXSA (CAA GCA GGT GTT GGT TCA GAA and TAA ATG AGC CAG GAG AAG GTC), and the thromboxane receptor (GGC TGT CCT TCC TGC TGA AC and GCT GAG GCG AGG CTG GAG AC) were designed as described in [2]. The amplification of cDNA (1 μl of RT product, 1 μl of each primer, 0.1 μl of Taq polymerase (Perkin Elmer), and 1 μl of nucleotides in 2 μl of 10 × buffer) was allowed to run for 40 cycles. Aliquots of 9 μl were collected and run on a 2% agarose gel, stained with ethidium bromide and photographed under UV illumination. Specific amplification was confirmed by sequencing of PCR products.
Thromboxane B2 ELISA
Thromboxane B2 (TXB-2), a stable but biologically inactive metabolite of TXA-2, was analyzed in cell culture supernatants by incubating monolayer cultures to 70% sub-confluence in serum free culture conditions. Cultures were rinsed with PBS and fresh media was added, the cultures were irradiated as indicated in the figures and cultures were maintained for 12 h. Supernatants were collected, centrifuged and stored at −80°C and cells were trypsinized and counted. TXB-2 was detected by an enzyme immunoassay using peroxidase labeled TXB-2 conjugates according to manufacturer’s instructions (Biotrak, code RPN 220, Amersham International plc). TXB-2 levels were reported as ng/106 cells from triplicate experiments per data point.
Transfection and luciferase reporter assay
For transient transfection, 2.0 × 105 cells were plated into six-well tissue culture plates (Nunc, Roskilde, Denmark) and transiently transfected using the Effectin transfection reagent (Quiagen, Hilden, Germany) according to the manufacturer’s instructions. 0.5 μg per well of the (−306) TXSA-Luc reporter plasmids containing a luciferase gene under the control of the thromboxane synthase promoter was used [8]. About 24 h after transfection, cells were γ-irradiated or mock treated and lysed at time points indicated in the figures. Cell lysates were cleared by centrifugation at 13,000 rpm for 5 min at 4°C and transferred to new tubes. The protein concentration was determined in the cell lysates and equalized with the lysis buffer. The luciferase activity was measured using a luciferase assay system (Promega, Madison, USA).
Orthotopic glioma model and radiation treatment
The human glioblastoma derived cell line U87 was grown in MEM containing 10% FCS. For intracranial implantation in nude NMRI mice cells were harvested from monolayer cultures. Cells were washed and resuspended at a concentration of 2 × 104 cells/μl. All procedures were performed in accordance with regulations of the Animal Care and Use Committee of the University Hospital of Schleswig-Holstein under permit No. 30/o/03. Prior to the implantation animals were anaesthetized by peritoneal injection of ketamine/xylazine solution (1.2 ml ketamine 5% and 0.8 ml xylazine 2% in 8 ml of saline) at 0.01 ml/g of body weight. For the procedure the cranium was fixed in a stereotactic frame (TSE Systems, Bad Homburg, Germany). About 3 μl of cell suspension were injected into the internal capsule of the right-brain hemisphere of ketamine-anesthetized mice using the following stereotactic coordinates in reference to the bregma: 1 mm (anteroposterior axis), 3 mm (lateromedial axis), 2.5 mm (vertical axis). Following implantation 1 mg/ml novaminsulfone was added to the drinking water for 3 days to relieve early post-operative pain. At day 5 post-implantation 0.5–8 mg/kg/day furegrelate were administered intracranially using mini osmotic pumps (Model 1002, Alzet, Durect corporation, Cupertino, CA, USA) and intratumoral catheters (brain infusion kit 3, Alzet) for 14 days. On day seven post-implantation whole brain radiation treatment of 1, 2 or 3 Gy was given using a Mevatron (Siemens, Erlangen, Germany) following a peritoneal injection of ketamine/xylazine solution as described above. Radiation treatment was repeated on day 8, 9, 10, and 11. Three weeks post-implantation tumor bearing brains were explanted following a lethal intraperitoneal injection of 0.7 ml ketamine/xylazine solution and the brain specimens were fixed in formalin. Coronal sections of the mouse brains were paraffin embedded and histological sections of 10 μm were processed for H&E staining. The tumor area was calculated from the largest cross sectional diameters measured by microscopical determination in consecutive histological sections and using a Cell A image analysis software. Tumor volumes were further calculated assuming the tumor to be spherical by using the formula for the volume of a sphere, V = 4/3 πr 3 = 4/3 π (√(A/π))3 where A is a tumor square area. Statistical analyses were performed by one way ANOVA test using GraphPrism software. Error bars shown in the figures represent standard deviation.
Results
Inhibition of TXSA and radiation sensitivity in vitro
We have previously demonstrated that the specific TXSA inhibitor furegrelate leads to caspase activation and DNA fragmentation 48 h after treatment and subsequent cell death in glioma cells. Furthermore, inhibition of TXSA by furegrelate increased the susceptibility to drug induced apoptosis by camptothecin and BCNU [7]. To analyze the effect of furegrelate on γ-radiation induced cell death the human glioblastoma derived cell line G-44 was treated with increasing concentrations of furegrelate 12 h prior to γ-irradiation and the surviving fraction of cells was determined in a clonogenic survival assay. A dose dependent decrease in the surviving fraction of G-44 cells was observed between 0.1 and 0.5 mg/ml furegrelate (Fig. 1), a dose range that has previously been demonstrated to result in migration arrest and apoptosis in various glioma cell lines in vitro [2, 7]. About 36 h pre-treatment of G-44 glioma cells with 0.5 mg/ml/12 h furegrelate prior to γ-irradiation resulted in a significant decrease in the surviving fraction of cells and an increase in radiation sensitivity at low irradiation doses. A single dose of furegrelate applied 4 h before irradiation resulted in a moderately decreased surviving fraction at high γ-irradiation doses only. Treatment at the time of radiation or following radiation showed no effect on radiation induced cell death (Fig. 2). In G-44 glioma cells a 6 Gy single dose radiation resulted in a decrease in the surviving fraction to approximately 35% of the non-irradiated control. Fractionation of the radiation dose led to a significant increase in the surviving fraction. A radiation dose of 2 × 3 Gy given with a one or three hour treatment interval resulted in an increase in the surviving fraction of up to 240 and 460%, respectively (Fig. 3a). About 36 h pre-treatment with 0.5 mg/ml/12 h furegrelate prior to γ-irradiation resulted in a loss of the recovery of the surviving fraction of G-44 glioma cells treated with a fractionated radiation dose (Fig. 3a). G-44 cells irradiated with a single dose of 6 Gy and trypsinized 12 h after radiation treatment showed a significant decrease in the surviving fraction compared to G-44 glioma cells trypsinized and replated immediately after irradiation (Fig. 3b).
Furegrelate’s inhibition of clonogenic survival in G-44 glioma cells is increased by a fractionated radiation. (a) Fractionation of the radiation dose and clonogenic survival of G-44 glioma cells pre-treated with the TXSA inhibitor furegrelate. Fractionation of the radiation dose led to a significant loss of efficiency against clonogenic growth. Prolonged treatment intervals resulted in further diminution of cytotoxicity, i.e., increased clonogenic survival. No recovery of the surviving fraction of cell populations treated with a fractionated radiation dose was observed following pre-treatment with furegrelate. (b) Furegrelate pre-treated G-44 cells irradiated with a single dose of 6 Gy and plated into clonogenic survival assays immediately showed a significantly increased survival (left) compared to cell populations trypsinized and plated 12 h after radiation treatment (right)
We have previously shown that, the invasion-associated gene TXSA is under the negative control of the tumor suppressor gene p53 and that the TXSA promoter is transactivated by the proto-oncogenic factor ets-1 [8]. To investigate whether TXSA may be up-regulated by radiation the p53 negative glioma cell line G-130 was irradiated with a single dose of 6 Gy and the levels of TXB-2 were measured 24 h after treatment. In G-130 glioma cells, which are deficient for p53 [12], γ-irradiation led to a significant increase in TXB-2 levels (Fig. 4a). Irradiation of G-130 cells transiently transfected with the luciferase reporter controlled by the TXSA promoter demonstrated that γ-irradiation led to induction of the TXSA promoter within 2 h following treatment (Fig. 4b).
Increased formation of TXB-2 and activation of the TXSA promoter induced by radiation in the p53 negative glioma cell line G-130. (a) TXB-2 formation in γ-irradiated p53 negative G-130 glioma cells 24 h after treatment. In G-130 cells γ-irradiation led to a significant increase in TXB-2 levels. (b) Activation of the TXSA promoter in G-130 cells by γ-irradiation. Activity of the TXSA promoter was assessed by a reporter assay in G-130 cells transiently transfected with a luciferase reporter gene under the control of the TXSA promoter [8]. Luciferase activity was measured in transfected cells which were γ-irradiated or mock treated and lysed at the indicated time points. Values represent the mean of triplicate wells, error bars indicate standard deviation
Irradiation of a panel of glioma cell lines and a strain of normal human astrocytes showed that in three of five glioma cell lines furegrelate treatment resulted in a strong increase in radiation sensitivity and in a moderate increase in radiation sensitivity in two other cell lines (Fig. 5). In normal astrocytes no decrease in the surviving fraction was observed in furegrelate treated cell populations. For human fibroblasts, which generally showed a higher resistance to radiation than astrocytes, also no radiation sensitizing effect of furegrelate was found (data not shown). Because U87 glioma cells showed a mid range radiation sensitizing effect of furegrelate in vitro this cell line was selected for further in vivo studies in NMRI mice. RT-PCR demonstrated that both TXSA and the thromboxane receptor are expressed in U87 cells in monolayer cell cultures (Fig. 6a). A monolayer migration assay showed that, a single dose furegrelate treatment resulted in a dose dependent inhibition of U87 cell migration (Fig. 6b) and that furegrelate resulted in histone-complexed-DNA fragmentation in an apoptosis assay 48 h after treatment (Fig. 6c).
The effects of furegrelate on the migratory and apoptotic potential of U87 glioma cells. (a) mRNA expression of TXSA and the thromboxane receptor (TP) in U87 glioma cells by RT-PCR. (b) Dose dependent inhibition of cell motility of U87 glioma cells in a monolayer migration assay treated with increasing concentrations of the TXSA inhibitor furegrelate. (c) Induction of apoptosis in U87 glioma cells treated with the TXSA inhibitor furegrelate. Furegrelate treatment resulted in a dose dependent histone-complexed-DNA fragmentation 48 h after treatment
Furegrelate treatment and radiation of experimental U87 gliomas
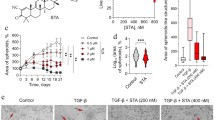
Intracranial implantation of 6 × 104 U87 glioma cells in NMRI mice results in establishment of solid tumors 5 days following implantation and growth of a lethal tumor mass approximately 4 weeks after inoculation [13, 14]. Furegrelate was administered using mini osmotic pumps (Model 1002, Alzet, Durect Corporation, Cupertino, CA, USA) and intratumoral catheters (brain infusion kit 3, Alzet) that were placed stereotactically through the bur hole used for the implantation of tumor cells. Whole brain irradiation of U87 tumor bearing mice was started 7 days after implantation. The animals were sacrificed on day 21 and the tumor volumes were determined by measurements of H&E stained serial coronal sections of mouse brains. As expected, radiation of U87 tumors led to a dose dependent decrease in tumor volumes (Fig. 7a). Intratumoral furegrelate treatment of U87 tumor bearing mice led to a reduction of intracranial tumor volumes, which at a concentration of 8 mg/kg/day, was significantly decreased in comparison to the untreated control (Fig. 7b). We next assessed the efficacy of a combined treatment with furegrelate and radiation on U87 tumors. To be able to distinguish the combined effects of radiation and furegrelate from those elicited by each of the treatments alone, suboptimal doses of radiation and furegrelate, 5 × 1 Gy and 2 mg/kg/day, respectively, were selected for a combined treatment of U87 tumors (Fig. 7c). Neither the suboptimal radiation dose of 5 × 1 Gy nor the suboptimal furegrelate dose of 2 mg/kg/day alone resulted in a significant reduction of tumor volumes, whereas a combined treatment led to a significant decrease in tumor volume compared to the untreated control.
Furegrelate sensitizes experimental U87 glioma to radiation. (a) Radiation of U87 tumors in an intracranial mouse model. Radiation treatment resulted in a dose dependent decrease in tumor volumes. (b) Effect of intratumoral furegrelate treatment on intracranial U87 tumor volumes. (c) Suboptimal treatment schedules of radiation dose and oral furegrelate were selected for co-treatment of intracranial U87 tumors in a mouse model. The combination of a suboptimal radiation dose of 5 × 1 Gy and a suboptimal dose of 2 mg/kg/day furegrelate resulted in a significant decrease in tumor volumes compared to the untreated control
Discussion
Cyclooxygenase-2 (COX-2), an enzyme induced by inflammatory cytokines, mitogens, oncogenes, growth factors and hypoxia among others, converts arachidonic acid to prostaglandins. COX-2 overexpression in several neoplastic tissues has been well documented. For this enzyme the link to carcinogenesis, tumor progression and metastatic tumor spread has been firmly established. Overexpression of COX-2 in human tumors is associated with a poor prognosis and a poor response to radiation therapy [15–18].
Pharmacological inhibitors of COX-2 have shown to enhance the radiation response of tumors of several histotypes in vitro and in vivo without serious side effects on normal tissues [19, 20]. Generally, COX-2 inhibitors increased radiation sensitivity at concentrations higher than necessary for inhibition of prostaglandin synthesis and also required prolonged exposure. Furthermore, in some cellular systems the sensitizing effect did not correlate with COX-2 expression [21, 22]. This suggests that COX independent effects of those drugs including inhibition of kinases, transcription factors, inhibition of sublethal cell damage repair, and changes in cell cycle distribution may add to COX-2 specific effects in the modulation of radiosensitivity in tumor cells [23–25].
Overexpression of TXSA, a downstream enzyme converting the COX product PGH2 to TXA-2, also seems to be associated with the progression and poor prognosis of many human tumors including thyroid, prostate, bladder, breast, colon cancer, and gliomas [2, 3, 26–30]. Differential mRNA expression analysis performed on human glioma cells proved TXSA to be highly overexpressed in migratory glioma cells [5]. Further evaluation of human glioma cells in vitro demonstrated that several pharmacological inhibitors of this enzyme block cell migration and lead to caspase activation and subsequent apoptosis in migration arrested glioma cell populations [2, 7]. Interestingly, pre-treatment of glioma cells with the specific TXSA inhibitor furegrelate resulted in increased sensitivity to apoptosis induced by camptothecin, etoposide or BCNU [7]. This evidence has implicated TXSA as an anti-apoptotic and survival factor in human glioma cells.
The notorious resistance to radiation comprises one of the challenges of glioma treatment [31]. An increase in radiation dose in order to increase the efficacy of radiotherapy is a futile approach as it is inevitably associated with severe damage to normal brain tissue. Instead, a combination of radiation sensitizing agents and low-dose radiation might be a promising strategy.
In this study we have shown that the specific TXSA inhibitor furegrelate decreases clonogenic survival of γ-irradiated glioma cells in vitro and sensitizes experimental gliomas to radiation treatment in vivo. No increase in radiation induced cell death was observed in normal human astrocytes (Fig. 5) or normal human fibroblasts (data not shown) adding to our previous observation that specific TXSA inhibitors do not result in migration arrest or apoptosis in astrocytes and fibroblasts [7]. The enhancing effect of furegrelate on radiation efficacy suggests that this synergistic treatment may provide means of increasing the therapeutic effects of radiation without the need for increased radiation doses. Our finding that furegrelate exerts radiosensitizing effects on glioma cells holds important implications concerning furegrelate’s potential therapeutic value and warrants further investigation of its potential value as an adjuvant therapeutic agent for glioma treatment.
Similar to data reported for COX-2 inhibitors, prolonged exposure of glioma cells prior to irradiation was required to achieve a significant effect. The most striking effect of the inhibitor was observed in glioma cells irradiated with a fractionated dose suggesting that furegrelate treatment interferes with the repair of radiation induced cell damage. In line with these findings a decreased clonogenic survival of furegrelate treated and irradiated cells plated for clonogenic survival assays 12 h after radiation versus immediate plating was observed. Whether furegrelate, in addition to its known inhibiting effects on TXSA, directly affects expression of DNA repair genes and thereby sensitizes glioma cells to apoptosis is unknown.
Further implicating TXSA as a survival factor we found that irradiation of glioma cells transfected with a reporter construct driven by a human TXSA promoter significantly increased the promoter activity 2 h after irradiation. A significant increase in TXB-2, a stable but inactive downstream conversion of TXA-2, in irradiated cells confirmed that γ-radiation induces endogenous thromboxane synthesis.
These experiments were performed on a p53 negative glioma cell line in order to eliminate the potential influence of radiation inducible p53. This is important, because we have shown that the gene encoding for TXSA is a target gene for both the tumor suppressor p53 and the proto-oncogenic factor ets-1 [8]. p53 and ets-1 co-regulate TXSA in an antagonistic and inter-related fashion, with ets-1 being a potent transcriptional activator of TXSA and p53 inhibiting ets-1 dependent transcription. Ets-1 and p53 associate physically in vitro and in vivo and their interaction rather than direct binding of p53 to the TXSA promoter is required for transcriptional repression of TXSA by wild type p53 [8].
An important implication of these findings may be that increased activity of TXSA in tumor cells promotes the invasive phenotype and resistance to cellular damage i.e., through radiation or agents inducing apoptosis. Such increased TXSA activity may be caused by loss of p53-mediated negative control which occurs in mutant p53 proteins or through abnormal expression of ets-1 [8]. Ets-1 is frequently found overexpressed in different types of human cancers including gliomas [32, 33]. Generally, an increased expression of ets-1 correlates with the grade of tumor invasiveness and malignancy, an association that prompts to consider ets-1 as one of the candidate targets for cancer therapy [34]. As a downstream target of the intersecting signaling cascades promoting (ets-1) or suppressing (p53) tumor progression, targeted inhibition of TXSA activity may therefore provide an effective strategy for modulation of the glioma cells’ response to conventional chemo- and radiotherapy.
References
Bennett A (1986) The production of prostanoids in human cancers, and their implications for tumor progression. Prog Lipid Res 25:539–542. doi:10.1016/0163-7827(86)90109-8
Giese A, Hagel C, Kim EL et al (1999) Thromboxane synthase regulates the migratory phenotype of human glioma cells. Neuro-oncol 1:3–13. doi:10.1215/15228517-1-1-3
Kürzel F, Hagel C, Zapf S et al (2002) Cyclooxygenase inhibitors and thromboxane synthase inhibitors differentially regulate migration arrest, proliferation, and apoptosis in human glioma cells. Acta Neurochir (Wien) 144:71–87. doi:10.1007/s701-002-8276-9
Pradono P, Tazawa R, Maemondo M et al (2002) Gene transfer of thromboxane A(2) synthase and prostaglandin I(2) synthase antithetically altered tumor angiogenesis and tumor growth. Cancer Res 62:63–66
McDonough W, Tran N, Giese A et al (1998) Altered gene expression in human astrocytoma cells selected for migration. I. Thromboxane synthase. J Neuropathol Exp Neurol 55:449–455. doi:10.1097/00005072-199805000-00008
Rodrigues S, Nguyen QD, Faivre S et al (2001) Activation of cellular invasion by trefoil peptides and src is mediated by cyclooxygenase- and thromboxane A2 receptor-dependent signaling pathways. FASEB J 15:1517–1528. doi:10.1096/fj.00-0802com
Yoshizato K, Zapf S, Westphal M et al (2002) Thromboxane synthase inhibitors induces apoptosis in migration arrested glioma cells. Neurosurgery 50:343–354. doi:10.1097/00006123-200202000-00021
Kim EL, Meissner H, Warneke G et al (2003) Regulation of thromboxane synthase by tumor suppressor p53 and ets-1. Oncogene 22:7716–7727. doi:10.1038/sj.onc.1207155
Giese A, Rief MD, Loo MA et al (1994) Determinants of human astrocytoma migration. Cancer Res 54:3897–3904
Jantke J, Kim E, Kürzel F et al (2004) Inhibition of the arachidonic acid metabolism blocks endothelial cell migration and induces apoptosis. Acta Neurochir (Wien) 146:483–494. doi:10.1007/s00701-004-0238-z
Aragane Y, Kulms D, Metze D et al (1998) Ultraviolet light induces apoptosis via direct activation of CD95 (Fas/APO-1) independently of its ligand CD95L. J Cell Biol 140:171–182. doi:10.1083/jcb.140.1.171
Kim EL, Yoshizato K, Meissner H et al (2005) Comparative assessment of status and function of p53 in human glioma cells. Anticancer Res 25:213–224
Brockmann MA, Westphal M, Lamszus K (2003) Improved method for the intracerebral engraftment of tumour cells and intratumoural treatment using a guide screw system in mice. Acta Neurochir (Wien) 145:777–781. doi:10.1007/s00701-003-0091-5
Brockmann MA, Ulmer S, Leppert J et al (2006) Analysis of mouse brain using a clinical 1.5 Tesla scanner and a standard small loop surface coil. Brain Res 1068:138–142. doi:10.1016/j.brainres.2005.10.098
Gaffney DK, Holden J, Davis M et al (2001) Elevated cyclooxygenase-2 expression correlates with diminished survival in carcinoma of the cervix treated with radiotherapy. Int J Radiat Oncol Biol Phys 49:1213–1217. doi:10.1016/S0360-3016(00)01583-2
Liao Z, Komaki R, Mason KA et al (2003) Role of cyclooxygenase-2 inhibitors in combination with radiation therapy in lung cancer. Clin Lung Cancer 4:356–365
Terakado N, Shintani S, Yano J et al (2004) Overexpression of cyclooxygenase-2 is associated with radioresistance in oral squamous cell carcinoma. Oral Oncol 40:383–389. doi:10.1016/j.oraloncology.2003.09.005
Nix P, Lind M, Greenman J et al (2004) Expression of Cox-2 protein in radioresistant laryngeal cancer. Ann Oncol 15:797–801. doi:10.1093/annonc/mdh185
Milas L (2003) Cyclooxygenase-2 (COX-2) enzyme inhibitors and radiotherapy: preclinical basis. Am J Clin Oncol 26:66–69
Petersen C, Baumann M, Petersen S (2003) New targets for the modulation of radiation response-selective inhibition of the enzyme cyclooxygenase 2. Curr Med Chem Anticancer Agents 3:354–359. doi:10.2174/1568011033482314
Liu W, Chen Y, Wang W et al (2003) Combination of radiation and Celebrex (celecoxib) reduce mammary and lung tumor growth. Am J Clin Oncol 26:103–109. doi:10.1097/00000421-200306000-00015
Williams CS, Watson AJ, Sheng H et al (2000) Celecoxib prevents tumor growth in vivo without toxicity to normal gut: lack of correlation between in vitro and in vivo models. Cancer Res 60:6045–6051
Raju U, Nakata E, Yang P et al (2002) In vitro enhancement of tumor cell radiosensitivity by a selective inhibitor of cyclooxygenase-2 enzyme: mechanistic considerations. Int J Radiat Oncol Biol Phys 54:886–894. doi:10.1016/S0360-3016(02)03023-7
Nakata E, Mason KA, Hunter N et al (2004) Potentiation of tumor response to radiation or chemoradiation by selective cyclooxygenase-2 enzyme inhibitors. Int J Radiat Oncol Biol Phys 58:369–375. doi:10.1016/j.ijrobp.2003.09.061
Tegeder I, Pfeilschifter J, Geisslinger G (2001) Cyclooxygenase-independent actions of cyclooxygenase inhibitors. FASEB J 15:2057–2072. doi:10.1096/fj.01-0390rev
Nie D, Che M, Zacharek A et al (2004) Differential expression of thromboxane synthase in prostate carcinoma: role in tumor cell motility. Am J Pathol 164:429–439
Moussa O, Yordy JS, Abol-Enein H et al (2005) Prognostic and functional significance of thromboxane synthase gene overexpression in invasive bladder cancer. Cancer Res 65:11581–11587. doi:10.1158/0008-5472.CAN-05-1622
Watkins G, Douglas-Jones A, Mansel RE et al (2005) Expression of thromboxane synthase, TBXAS1 and the thromboxane A2 receptor, TBXA2R, in human breast cancer. Int Semin Surg Oncol 2:23. doi:10.1186/1477-7800-2-23
Dassesse T, de Leval X, de Leval L et al (2006) Activation of the thromboxane A2 pathway in human prostate cancer correlates with tumor Gleason score and pathologic stage. Eur Urol 50:1021–1031. doi:10.1016/j.eururo.2006.01.036
Sakai H, Suzuki T, Takahashi Y et al (2006) Upregulation of thromboxane synthase in human colorectal carcinoma and the cancer cell proliferation by thromboxane A2. FEBS Lett 580:3368–3374. doi:10.1016/j.febslet.2006.05.007
Reardon DA, Rich JN, Friedman HS et al (2006) Recent advances in the treatment of malignant astrocytoma. J Clin Oncol 24:1253–1265. doi:10.1200/JCO.2005.04.5302
Dittmer J (2003) The biology of the Ets1 proto-oncogene. Mol Cancer 2:29. doi:10.1186/1476-4598-2-29
Gilliland DG et al (2001) The diverse roles of the ets family of transcription factor in cancer. Clin Cancer Res 7:451–453
Oikawa T (2004) ETS transcription factors: possible targets for cancer therapy. Cancer Sci 95:626–633. doi:10.1111/j.1349-7006.2004.tb03320.x
Acknowledgments
This work was supported by a grant of the Deutsche Krebshilfe #10-2166 Gi2. It contains parts of a doctoral thesis presented to the Medical Faculty of the University Hospital Schleswig-Holstein by Anne Katrin Schauff.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Schauff, A.K., Kim, E.L., Leppert, J. et al. Inhibition of invasion-associated thromboxane synthase sensitizes experimental gliomas to γ-radiation. J Neurooncol 91, 241–249 (2009). https://doi.org/10.1007/s11060-008-9708-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-008-9708-0