Abstract
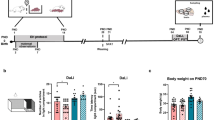
Males are more likely to develop autism as a neurodevelopmental disorder than females, but the mechanisms underlying male susceptibility are not fully understood. In this paper, we used a well-characterized propionic acid (PPA) rodent model of autism to study sex differences in stress hormones, antioxidants’ status, and the neuroimmune response that may contribute to the preponderance of autism in males. Sprague Dawley rats of both sexes were divided into a saline-treated group as controls and PPA-treated groups, receiving 250 mg/kg of PPA per day for three days. Animals’ social behavior was examined using the three-chamber social test. Hormones (ACTH, corticosterone, melatonin, and oxytocin), oxidative stress biomarkers (glutathione, glutathione-S-transferase, and ascorbic acid), and cytokines (IL-6, IL-1α, IL-10, and IFNγ) were measured in the brain tissue of all the animals. The results showed a sex dimorphic social response to PPA treatment, where males were more susceptible to the PPA treatment and exhibited a significant reduction in social behavior with no effects observed in females. Also, sex differences were observed in the levels of hormones, antioxidants, and cytokines. Female rats showed significantly higher corticosterone and lower oxytocin, antioxidants, and cytokine levels than males. The PPA treatment later modulated these baseline differences. Our study indicates that the behavioral manifestation of autism in PPA-treated males and not females could be linked to neural biochemical differences between the sexes at baseline, which might play a protective role in females. Our results can contribute to early intervention strategies and treatments used to control autism, an increasingly prevalent disorder.





Similar content being viewed by others
Change history
09 April 2022
A Correction to this paper has been published: https://doi.org/10.1007/s11011-022-00982-x
References
Al-Suwailem E, Abdi S, El-Ansary A (2018) Sex differences in the glutamate signaling pathway in juvenile rats. J Neurosci Res 96(3):459–466
Atkinson HC, Waddell BJ (1997) Circadian variation in basal plasma corticosterone and adrenocorticotropin in the rat: sexual dimorphism and changes across the estrous cycle. Endocrinology 138(9):3842–3848
Beck RD Jr, Wasserfall C, Ha GK, Cushman JD, Huang Z, Atkinson MA, Petitto JM (2005) Changes in hippocampal IL-15, related cytokines, and neurogenesis in IL-2 deficient mice. Brain Res 1041(2):223–230
Besedovsky HO, del Rey AZ (2000) The cytokine-HPA axis feedback circuit. Z Rheumatol 59(2):II26–II30
Besedovsky HO, del Rey A (1996) Immune-neuro-endocrine interactions: facts and hypotheses. Endocr Rev 17(1):64–102
Beutler E (1963) Improved method for the determination of blood glutathione. J Lab Clin Med 61:882–888
Borrás C, Gambini J, Gómez-Cabrera MC, Sastre J, Pallardó FV, Mann GE, Viña J (2005) 17β-oestradiol up-regulates longevity-related, antioxidant enzyme expression via the ERK1 and ERK2 [MAPK]/NFκB cascade. Aging Cell 4(3):113–118
Bülbül M, Babygirija R, Cerjak D, Yoshimoto S, Ludwig K, Takahashi T (2011) Hypothalamic oxytocin attenuates CRF expression via GABAA receptors in rats. Brain Res 1387:39–45
Carey MP, Deterd CH, De Koning J, Helmerhorst F, De Kloet ER (1995) The influence of ovarian steroids on hypothalamic-pituitary-adrenal regulation in the female rat. J Endocrinol 144(2):311–321
Choi J, Lee S, Won J, Jin Y, Hong Y, Hur T-Y, Kim J.H., Lee S.R., Hong Y. (2018) Pathophysiological and neurobehavioral characteristics of a propionic acidmediated autism-like rat model. PLoS One 13(2): e0192925. https://doi.org/10.1371/journal. pone.0192925
Christensen DL, Baio J, Van Naarden Braun K, Bilder D, Charles J, Constantino JN, Daniels J, Durkin MS, Fitzgerald RT, Kurzius-Spencer M, Lee L-C, Pettygrove S, Robinson C, Schulz E, Wells C, Wingate MS, Zahorodny W, Yeargin-Allsopp M, Centers for Disease Control and Prevention (CDC) (2016) Prevalence and characteristics of autism spectrum disorder among children aged 8 years—autism and developmental disabilities monitoring network, 11 sites, United States, 2012. MMWR Surveill Summ 65(3):1–23. https://doi.org/10.15585/mmwr.ss6503a1
Chrousos GP (2000) The role of stress and the hypothalamic–pituitary–adrenal axis in the pathogenesis of the metabolic syndrome: neuro-endocrine and target tissue-related causes. Int J Obes 24(2):S50–S55
Critchlow V, Liebelt RA, Bar-Sela M, Mountcastle W, Lipscomb HS (1963) Sex difference in resting pituitary-adrenal function in the rat. American Journal of Physiology-Legacy Content 205(5):807–815
Debono M, Ghobadi C, Rostami-Hodjegan A, Huatan H, Campbell MJ, Newell-Price J, Darzy K, Merke DP, Arlt W, Ross RJ (2009) Modified-release hydrocortisone to provide circadian cortisol profiles. The Journal of Clinical Endocrinology & Metabolism 94(5):1548–1554
Dong H, Xu J, Li W, Gan J, Lin W, Ke J, Jiang J, du L, Chen Y, Zhong X, Zhang D, Yeung SCJ, Li X, Zhang H (2017) Reciprocal androgen receptor/interleukin-6 crosstalk drives oesophageal carcinoma progression and contributes to patient prognosis. J Pathol 241(4):448–462. https://doi.org/10.1002/path.4839
Dumais KM, Veenema AH (2016) Vasopressin and oxytocin receptor systems in the brain: sex differences and sex-specific regulation of social behavior. Front Neuroendocrinol 40:1–23
El-Ansary AK, Al-Daihan SK, El-Gezzery AR. (2011) On the protective effect of omega-3 against propionic acid-induced neurotoxicity in rat pups. Lipids Health Dis. 10: 142. https://doi.org/10.1186/1476- 511X-10-142 PMID: 21854591
El-Ansary AK, Ben Bacha AB, Kotb M. (2012) Etiology of autistic features: the persisting neurotoxic effects of propionic acid. J Neuroinflammation. 9: 74. https://doi.org/10.1186/1742-2094-9-74 PMID: 22531301
El-Ansary AK, Shaker GH (2013) Rizk MZ role of gut–brain axis in the aetiology of neurodevelopmental disorders with reference to autism. J Clin Toxicol S6:005
Fransen F, van Beek AA, Borghuis T, Meijer B, Hugenholtz F, van der Gaast-de Jongh C, de Vos P (2017). The impact of gut microbiota on gender-specific differences in immunity. Front immunol 8(JUN), 754. https://doi.org/10.3389/fimmu.2017.00754
Fujita Y, Fujita A, Ishima T, Hirai A, Suzuki S, Suganuma H, Hashimoto K (2020). Dietary intake of glucoraphanin during pregnancy and lactation prevents the behavioral abnormalities in the offspring after maternal immune activation. Neuropsychopharmacol Rep npr2.12112. https://doi.org/10.1002/npr2.12112
Gallucci WT, Baum A, Laue L, Rabin DS, Chrousos GP, Gold PW, Kling MA (1993) Sex differences in sensitivity of the hypothalamic-pituitary-adrenal axis. Health Psychol 12(5):420–425
Gawryluk JW, Wang J-F, Andreazza AC, Shao L, Young LT (2011) Decreased levels of glutathione, the major brain antioxidant, in post-mortem prefrontal cortex from patients with psychiatric disorders. Int J Neuropsychopharmacol 14(1):123–130
Ghasemi A, Zahediasl S (2012) Normality tests for statistical analysis: a guide for non-statisticians. International Journal of Endocrinology and Metabolism 10(2):486–489. https://doi.org/10.5812/ijem.3505
Gomaa AM, Galal HM, Abou-Elgait AT (2017) Neuroprotective effects of melatonin administration against chronic immobilization stress in rats. International journal of physiology, pathophysiology and pharmacology 9(2):16–27
Greenfield LJ Jr (2013) Molecular mechanisms of antiseizure drug activity at GABAA receptors. Seizure 22(8):589–600
Hastings WJ, Chang A-M, Ebstein RP, Shalev I (2018) Neuroendocrine stress response is moderated by sex and sex hormone receptor polymorphisms. Horm Behav 106:74–80
Heberling C, Dhurjati P, Sasser M (2013) Hypothesis for a systems connectivity model of autism spectrum disorder pathogenesis: links to gut bacteria, oxidative stress, and intestinal permeability. Med Hypotheses 80(3):264–270. https://doi.org/10.1016/j.mehy.2012.11.044
Hoang YD, Nakamura BN, Luderer U (2009) Follicle-stimulating hormone and estradiol interact to stimulate glutathione synthesis in rat ovarian follicles and granulosa cells. Biol Reprod 81(4):636–646
Hoffman GE, Moore N, Fiskum G, Murphy AZ (2003) Ovarian steroid modulation of seizure severity and hippocampal cell death after kainic acid treatment. Exp Neurol 182(1):124–134
Hudson SP, Jacobson-Pick S, Anisman H (2014) Sex differences in behavior and pro-inflammatory cytokine mRNA expression following stressor exposure and re-exposure. Neuroscience 277:239–249
Jagota SK, Dani HM (1982). A new colorimetric technique for the estimation of vitamin C using Folin phenol reagent. Anal Biochem, 127(1), 178–182. https://doi.org/10.1016/0003-2697(82)90162-2
James SJ, Cutler P, Melnyk S, Jernigan S, Janak L, Gaylor DW, Neubrander JA (2004) Metabolic biomarkers of increased oxidative stress and impaired methylation capacity in children with autism. Am J Clin Nutr 80(6):1611–1617
Jiang Y, Platt ML (2018) Oxytocin and vasopressin increase male-directed threats and vocalizations in female macaques. Sci Rep 8(1):1–14
Johnson EO, Kamilaris TC, Carter CS, Calogero AE, Gold PW, Chrousos GP (1996) The biobehavioral consequences of psychogenic stress in a small, social primate (Callithrix jacchus jacchus). Biol Psychiatry 40(5):317–337
Kitay JI (1961) Sex differences in adrenal cortical secretion in the rat. Endocrinology 68(5):818–824
Klein SL, Flanagan KL (2016, October 1) Sex differences in immune responses. Nat Rev Immunol 16:626–638. https://doi.org/10.1038/nri.2016.90
Kwekel JC, Desai VG, Moland CL, Vijay V, Fuscoe JC (2013) Sex differences in kidney gene expression during the life cycle of F344 rats. Biol Sex Differ 4(1):1–13
Lakens D (2013) Calculating and reporting effect sizes to facilitate cumulative science: a practical primer for t-tests and ANOVAs. Front Psychol 4:863
Lang RE, Heil JWE, Ganten D, Hermann K, Unger T, Rascher W (1983) Oxytocin unlike vasopressin is a stress hormone in the rat. Neuroendocrinology 37(4):314–316
Lo S-C, Scearce-Levie K, Sheng M (2015) Characterization of social behaviors in caspase-3 deficient mice OPEN. Nat Publ Group 6. https://doi.org/10.1038/srep18335
Love TM (2018) The impact of oxytocin on stress: the role of sex. Curr Opin Behav Sci 23:136–142
MacFabe DF, Cain NF, Boon F, Ossenkopp KP, Cain DP (2011). Effects of the enteric bacterial metabolic product propionic acid on object-directed behavior, social behavior, cognition, and neuroinflammation in adolescent rats: relevance to autism spectrum disorder. Behav Brain Res 217(1), 47-54MacFabe, D. F., Cain, N. E., Boon, F., Ossenk. https://doi.org/10.1016/j.bbr.2010.10.005
Maenner MJ, Shaw KA, Baio J, et al. (2016) Prevalence of Autism Spectrum Disorder Among Children Aged 8 Years — Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States. MMWR Surveill Summ 2020, 69 (No. SS-4): 1–12. https://www.cdc.gov/mmwr/volumes/69/ss/ss6904a1.htm
McCarthy MM (1995) Estrogen modulation of oxytocin and its relation to behavior. Adv Exp Med Biol 395:235–245
McHenry J, Carrier N, Hull E, Kabbaj M (2014) Sex differences in anxiety and depression: role of testosterone. Front Neuroendocrinol 35(1):42–57
Nankova BB, Agarwal R, Macfabe DF, La Gamma EF. (2014) Enteric bacterial metabolites propionic and butyric acid modulate gene expression, including CREB-dependent catecholaminergic neurotransmission, in PC12 cells—possible relevance to autism spectrum disorders. PLoS One. 9: e103740. https://doi.org/10.1371/journal.pone.0103740 PMID: 25170769
Navarro F, Liu Y, Rhoads JM. (2016) Can probiotics benefit children with autism spectrum disorders? World J Gastroenterol. 22:10093–10102. https://doi.org/10.3748/wjg.v22.i46.10093 PMID: 28028357
Neumann ID (2008) Brain oxytocin: a key regulator of emotional and social behaviours in both females and males. J Neuroendocrinol 20(6):858–865
Neumann ID, Krömer SA, Toschi N, Ebner K (2000) Brain oxytocin inhibits the (re) activity of the hypothalamo–pituitary–adrenal axis in male rats: involvement of hypothalamic and limbic brain regions. Regul Pept 96(1–2):31–38
Paudel R, Raj K, Gupta YK, Singh S (2020) Oxiracetam and Zinc Ameliorates Autism-Like Symptoms in Propionic Acid Model of Rats. Neurotoxicity Research 37. https://doi.org/10.1007/s12640-020-00169-1
Pyter LM, Kelly SD, Harrell CS, Neigh GN (2013) Sex differences in the effects of adolescent stress on adult brain inflammatory markers in rats. Brain Behav Immun 30:88–94
Pacharra M, Schäper M, Kleinbeck S, Blaszkewicz M, Golka K, Thriel C (2016) Neurobehavioral effects of exposure to propionic acid revisited—does psychosocial stress interfere with distractive effects in volunteers? NeuroToxicology. 55:102–111. https://doi.org/10.1016/j.neuro.2016.05.019
Rea K, Dinan TG, Cryan JF (2016) The microbiome: a key regulator of stress and neuroinflammation. Neurobiology of stress 4:23–33. https://doi.org/10.1016/j.ynstr.2016.03.001
Rein B, Ma K, Yan ZA (2020) Standardized social preference protocol for measuring social deficits in mouse models of autism. Nat Protoc 15(10):3464–3477. https://doi.org/10.1038/s41596-020-0382-9
Rose S, Melnyk S, Pavliv O, Bai S, Nick TG, Frye RE, James SJ (2012) Evidence of oxidative damage and inflammation associated with low glutathione redox status in the autism brain. Transl Psychiatry 2(7):e134. https://doi.org/10.1038/tp.2012.61
Ruiz-Larrea MB, Leal AM, Martin C, Martinez R, Lacort M (1997) Antioxidant action of estrogens in rat hepatocytes. Rev Esp Fisiol 53(2):225–229
Sanchez MM, Mccormack K, Grand AP, Fulks R, Graff A, Maestripieri D (2010) Effects of sex and early maternal abuse on adrenocorticotropin hormone and cortisol responses to the corticotropin-releasing hormone challenge during the first 3 years of life in group-living rhesus monkeys. Dev Psychopathol 22(1):45–53
Schwartzer JJ, Careaga M, Onore CE, Rushakoff JA, Berman RF, Ashwood P (2013) Maternal immune activation and strain specific interactions in the development of autism-like behaviors in mice. Transl Psychiatry 3(3):e240. https://doi.org/10.1038/tp.2013.16
Shams S, Foley KA, Kavaliers M, MacFabe DF, Ossenkopp K-P (2019) Systemic treatment with the enteric bacterial metabolic product propionic acid results in reduction of social behavior in juvenile rats: contribution to a rodent model of autism spectrum disorder. Dev Psychobiol 61(5):688–699. https://doi.org/10.1002/dev.21825
Shultz SR, MacFabe DF, Ossenkopp KP, Scratch S, Whelan J, Taylor R, Cain DP (2008) Intracerebroventricular injection of propionic acid, an enteric bacterial metabolic end-product, impairs social behavior in the rat: implications for an animal model of autism. Neuropharmacology 54(6):901–911. https://doi.org/10.1016/j.neuropharm.2008.01.013
Sinha S, Kaler LJ, Proctor TM, Teuscher C, Vandenbark AA, Offner H (2008) IL-13-mediated gender difference in susceptibility to autoimmune encephalomyelitis. J Immunol 180(4):2679–2685. https://doi.org/10.4049/jimmunol.180.4.2679
Snyder MJ, Maddison DR (1997) Molecular phylogeny of glutathione-S-transferases. DNA Cell Biol 16(11):1373–1384
Toufexis DJ, Wilson ME (2012) Dihydrotestosterone differentially modulates the cortisol response of the hypothalamic–pituitary–adrenal axis in male and female rhesus macaques, and restores circadian secretion of cortisol in females. Brain Res 1429:43–51
Uvnäs-Moberg K (1997) Oxytocin linked antistress effects--the relaxation and growth response. Acta Physiol Scand Suppl 640:38–42
Velíšková J, DeSantis KA (2013) Sex and hormonal influences on seizures and epilepsy. Horm Behav 63(2):267–277
Villa A, Rizzi N, Vegeto E, Ciana P, Maggi A (2015) Estrogen accelerates the resolution of inflammation in macrophagic cells. Sci Rep 5:15224
Wang L, Ahn YJ, Asmis R (2020) Sexual dimorphism in glutathione metabolism and glutathione-dependent responses. Redox Biol 31:101410
Windle RJ, Shanks N, Lightman SL, Ingram CD (1997) Central oxytocin administration reduces stress-induced corticosterone release and anxiety behavior in rats. Endocrinology 138(7):2829–2834
Yilmaz B, Kutlu S, Mogulkoç R, Canpolat S, Sandal S, Tarakçi B, Kelestimur H (2000) Melatonin inhibits testosterone secretion by acting at hypothalamo-pituitary-gonadal axis in the rat. Neuro Endocrinol Lett; 21(4):301–306. PMID: 11455362
Acknowledgments
This research project was supported by the Deanship of Scientific Research, Princess Nourah Bint Abdulrahman University, Grant number RGP-1441-0027. The authors thank the Deanship of Scientific Research and RSSU at King Saud University for the technical support.
Availability of data and materials
The datasets generated analyses during the current study are available from the corresponding author on reasonable request.
Funding
This research project was supported by the Deanship of Scientific Research, Princess Nourah Bint Abdulrahman University.
Author information
Authors and Affiliations
Contributions
Conceptualization: AE.
Formal analysis: SA.
Funding acquisition: KA.
Investigation: SA, NMA, SAA.
Methodology: RSB, SMA, SA.
Supervision: AE, KA.
Writing – original draft: AE.
Writing – review & editing: TSA, SA.
Corresponding author
Ethics declarations
Ethical approval
Ethical approval from the Institutional Review Board were obtained.
Consent of participants
NA
Consent for publication
All authors read the manuscript and agree to publish.
Competing interests
The authors declare no potential conflicts of interest with respect to the authorship and/or publication of this article.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Abuaish, S., Al-Otaibi, N.M., Aabed, K. et al. The role of sex-differentiated variations in stress hormones, antioxidants, and neuroimmune responses in relation to social interaction impairment in a rodent model of autism. Metab Brain Dis 36, 1369–1379 (2021). https://doi.org/10.1007/s11011-021-00732-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-021-00732-5