Abstract
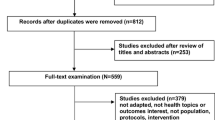
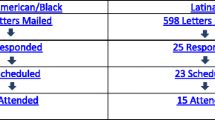
Mammography and fecal occult blood testing (FOBT) improve the detection, management, and prognosis of breast and colorectal cancer, respectively, but are underperformed in the recent immigrant and refugee population. We aimed to identify barriers to screening and potential solutions in this population. A mixed-methods study involving a retrospective chart review and focus group interviews was conducted, with data analyzed using univariate logistic regression and thematic analysis, respectively. Mammography completion was associated with greater time in Canada (p = 0.01) and region of origin (p = 0.04), while FOBT completion was associated with region of origin (p = 0.03). Barriers included time constraints, language and cultural differences, and poor interprofessional communication. This study of recent immigrants and refugees identifies barriers to screening and supports potential solutions including culturally-congruent peer workers, targeted screening workshops, and visual screening aids. Further work is needed to address the unique healthcare needs of this diverse and growing population.

Similar content being viewed by others
References
Bromfield G, Dale D, De P, Newman K, Rahal R, et al.: Canadian cancer statistics 2015. 2015. http://www.cancer.ca/~/media/cancer.ca/CW/cancer%20information/cancer%20101/Canadian%20cancer%20statistics/Canadian-Cancer-Statistics-2015-EN.pdf?la=en. Accessed Aug 28 2017
Berry DA, Plevritis SK, Fryback DG, Clarke L, Zelen M, Mandelblatt JS, Yakovlev AY, Habbema JDF, Feuer EJ. Effect of screening and adjuvant therapy on mortality from breast cancer. N Engl J Med. 2005;353:1784–92.
Kalager M, Langmark F, Adami H. Effect of screening mammography on breast-cancer mortality in Norway. N Engl J Med. 2010;363:1203–10.
Richards M, Westcombe A, Love S, Littlejohns P, Ramirez A. Influence of delay on survival in patients with breast cancer: a systematic review. Lancet. 1999;353:1119–26.
Jorgensen O, Kronborg O, Fenger C. A randomized study of screening for colorectal cancer using faecal occult blood testing: results after 13 years and seven biennial screening rounds. Gut. 2002;50(29):3229–32.
Kronborg O, Jorgensen OD, Fenger C, Rasmussen M. Randomized study of biennial screening with faecal occult blood test: results after nine screening rounds. Scand J Gastroenterol. 2004;39:846–51.
Humphrey LL, Helfand M, Chan BK, Woolf SH. Breast cancer screening: a summary of the evidence for the U.S. preventive services task force. Ann Intern Med. 2002;137(5 Part 1):347–60.
Behl M, Dawe D, Kennecke H, Kerba M, Kumar E, et al.: The 2016 cancer system performance report. 2016. https://www.longwoods.com/articles/images/the-2016-cancer-system-performance-report-en.pdf. Accessed Aug 28 2017
Cancer Care Ontario. Breast cancer screening. 2017. https://www.cancercare.on.ca/pcs/screening/breastscreening/. Accessed Aug 28 2017
Cancer Care Ontario. Fecal occult blood test. 2016. https://www.cancercare.on.ca/pcs/screening/coloscreening/fobt/. Accessed Aug 28 2017
Decker K, Singh H. Reducing inequities in colorectal cancer screening in North America. J Carcinog. 2014;13(12).
Yuan Y, Li M, Yang J, Winget M. Using administrative data to estimate time to breast cancer diagnosis and percent of screen-detected breast cancers—a validation study in Alberta, Canada. Eur J Cancer Care. 2015;24:367–75.
Lofters A, Vahabi M, Glazier RH. The validity of self-reported cancer screening history and the role of social disadvantage in Ontario, Canada. BMC Public Health 2015;15(28).
Vahabi M, Lofters A, Kumar M, Glazier RH. Breast cancer screening disparities among urban immigrants: a population-based study in Ontario, Canada. BMC Public Health 2015;15(679).
Gupta S, Sussman DA, Doubeni CA, Anderson DS, Day L, Deshpande AR, et al.: Challenges and possible solutions to colorectal cancer screening for the underserved. JNCI 2014;106(4).
United Nations Statistics Division. Standard country or area codes for statistical use (M49). 2017. https://unstats.un.org/unsd/methodology/m49/. Accessed Aug 28 2017
Scheffer J. Dealing with missing data. Res Lett Inf Math Sci. 2002;3:153–60.
Krueger RA, Casey MA, Donner J, Kirsch S, Maack JN: Social analysis selected tools and techniques. Washington, DC; 2001. http://siteresources.worldbank.org/INTCDD/Resources/SAtools.pdf.
Debus M. Methodological review: a handbook for excellence in focus group research. Washington, DC: Academy for Educational Development; 1989.
Gubrium J, Holstein J, Marvasti A, McKinney K. The SAGE handbook of interview research: the complexity of the craft. Los Angeles: Sage; 2012. 1–613.
Boyatzis B. Transforming qualitative information: thematic analysis and code development. Los Angeles: Sage; 1998.
Vaismoradi M, Turunen H, Bondas T. Content analysis and thematic analysis: Implications for conducting a qualitative descriptive study. Nurs Health Sci. 2013;15(3):398–405.
Attride-Stirling J. Thematic networks: an analytic tool for qualitative research. Qualitative research. Los Angeles: Sage; 2001.
Ward E, Jemal A, Cokkinides V, Singh GK, Cardinez C, Ghafoor A, et al. Cancer disparities by race/ethnicity and socioeconomic status. CA Cancer J Clin. 2004;54(2):78–93.
Goel MS, Wee CC, McCarthy EP, Davis RB, Ngo-Metzger Q, Phillips RS. Racial and ethnic disparities in cancer screening: the importance of foreign birth as a barrier to care. J Gen Intern Med. 2003;18(12):1028–35.
Center MM, Jemal A, Smith RA, Ward E. Worldwide variations in colorectal cancer. CA Cancer J Clin. 2009;59(6):366–78.
Youlden DR, Cramb SM, Dunn NAM, Muller JM, Pyke CM, Baade PD. The descriptive epidemiology of female breast cancer: an international comparison of screening, incidence, survival and mortality. Cancer Epidemiol. 2012;36(3):237–48.
Robles SC, Galanis E. Breast cancer in Latin America and the Caribbean. Rev Panam Salud Pública. 2002;11(3):178–85.
Perry N, Broeders M, de Wolf C, Tornberg S, Holland R, von Karsa L. European guidelines for quality assurance in breast cancer screening and diagnosis. Fourth edition–summary document. Ann Oncol. 2007;19(4):614–22.
Zavoral M, Suchanek S, Zavada F, Dusek L, Muzik J, Seifert B, et al.: Colorectal cancer screening in Europe. World J Gastroenterol. 2009;15(47):5907–15.
Sung JJY, Ng SC, Chan FKL, Chiu HM, Kim HS, Matsuda T, et al. An UPDATED Asia Pacific consensus recommendations on colorectal cancer screening. Gut. 2015;64(1):121–32.
Tan SM, Evans AJ, Lam TP, Cheung KL. How relevant is breast cancer screening in the Asia/Pacific region? Breast. 2007;16(2):113–9.
Richards M, Love S, Littlejohns P, Ramirez A. Influence of delay on survival in patients with breast cancer: a systematic review. Lancet. 1999;353:1119–26.
Ioannou GN, Chapko MK, Dominitz JA. Predictors of colorectal cancer screening participation in the United States. Am J Gastroenterol. 2003;98(9):2082–91.
Beydoun HA, Beydoun MA. Predictors of colorectal cancer screening behaviors among average-risk older adults in the United States. Cancer Causes Control. 2008;19(4):339–59.
Maxwell AE, Bastani R, Warda US. Demographic predictors of cancer screening among Filipino and Korean immigrants in the United States. Am J Prev Med. 2000;18(1):62–8.
Samuel PS, Pringle JP, James NW, Fielding SJ, Fairfield KM. Breast, cervical, and colorectal cancer screening rates amongst female Cambodian, Somali, and Vietnamese immigrants in the USA. Int J Equity Health. 2009;8(1):30.
Brown WM, Consedine NS, Magai C. Time spent in the united states and breast cancer screening behaviors among ethnically diverse immigrant women: evidence for acculturation? J Immigr Minor Health. 2006;8(4):347–58.
De Alba I, Hubbell FA, McMullin JM, Sweningson JM, Saitz R: Impact of U.S. citizenship status on cancer screening among immigrant women. J Gen Intern Med. 2005;20(3):290–6.
Miller BA, Chu KC, Hankey BF, Ries LAG: Cancer incidence and mortality patterns among specific Asian and Pacific Islander populations in the U.S. Cancer Causes Control. 2008;19(3):227–56.
Kem R, Chu KC. Cambodian cancer incidence rates in California and Washington, 1998–2002. Cancer. 2007;110(6):1370–5.
Ross JA, Xie Y, Kiffmeyer WR, Bushhouse S, Robison LL. Cancer in the Minnesota Hmong population. Cancer. 2003;97(12):3076–9.
Rodriguez MA, Ward LM, Pérez-Stable EJ. Breast and cervical cancer screening: impact of Health insurance status, ethnicity, and Nativity of Latinas. Ann Fam Med. 2005;3(3):235–41.
Wee CC, McCarthy EP, Phillips RS. Factors associated with colon cancer screening: the role of patient factors and physician counseling. Prev Med. 2005;41(1):23–9.
Tu S-P, Taylor V, Yasui Y, Chun A, Yip M-P, Acorda E, et al. Promoting culturally appropriate colorectal cancer screening through a health educator. Cancer. 2006;107(5):959–66.
Percac-Lima S, Grant RW, Green AR, Ashburner JM, Gamba G, Oo S, et al. A culturally tailored navigator program for colorectal cancer screening in a community health center: a randomized, controlled trial. J Gen Intern Med. 2009;24(2):211–7.
Larkey LK, Gonzalez J. Storytelling for promoting colorectal cancer prevention and early detection among Latinos. Patient Educ Couns. 2007;67(3):272–8.
Jandorf L, Gutierrez Y, Lopez J, Christie J, Itzkowitz SH: Use of a patient navigator to increase colorectal cancer screening in an urban neighborhood health clinic. J Urban Health. 2005;82(2):216–24.
Kwok C, Endrawes G, Lee CF. Cultural beliefs and attitudes about breast cancer and screening practices among Arabic Women in Australia. Cancer Nurs. 2016;39(5):367–74.
Azaiza F, Cohen M. Health beliefs and rates of breast cancer screening among Arab women. J Women’s Health. 2006;15(5):520–30.
Elnekave E, Gross R. The healthcare experiences of Arab Israeli women in a reformed healthcare system. Health Policy. 2004;69(1):101–16.
Consedine NS, Magai C, Krivoshekova YS, Ryzewicz L, Neugut AI. Fear, anxiety, worry, and breast cancer screening behavior: a critical review. Cancer Epidemiol Biomarkers Prev. 2004;13(4):501–10.
Janz NK, Wren PA, Schottenfeld D, Guire KE. Colorectal cancer screening attitudes and behavior: a population-based study. Prev Med. 2003;37(6 Pt 1):627–34.
Lasser KE, Ayanian JZ, Fletcher RH, Good M-JD. Barriers to colorectal cancer screening in community health centers: a qualitative study. BMC Fam Pract. 2008;9(1):15.
Walsh JME, Kaplan CP, Nguyen B, Gildengorin G, McPhee SJ, Pérez-Stable EJ: Barriers to colorectal cancer screening in Latino and Vietnamese Americans. Compared with non-Latino white Americans. J Gen Intern Med. 2004;19(2):156–66.
Kiran T, Wilton AS, Moineddin R, Paszat L, Glazier RH. Effect of payment incentives on cancer screening in Ontario primary care. Ann Fam Med. 2014;12(4):317–23.
Brownstein JN, Cheal N, Ackermann S, Bassford T, Campos-Outcalt D. Breast and cervical cancer screening in minority populations: a model for using lay health educators. J Cancer Educ. 1992;7(4):321–6.
Acknowledgements
The authors would like to thank My Dang, Dr. Heather Sampson, and Christopher Meaney for their invaluable help in the conduct and analysis of this study. There are no relevant external funding sources to report and the authors declare they have no relevant conflicts of interest to report. Dr. Aisha Lofters is supported as a Clinician Scientist by the Department of Family and Community Medicine at the University of Toronto and at St. Michael’s Hospital, and by the Canadian Institutes of Health Research as a New Investigator.
Author information
Authors and Affiliations
Contributions
All authors have made substantive intellectual contribution to the development of this article and have reviewed and agree with the content of the article.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Appendix: Standardized focus group question sets used in both sessions
Appendix: Standardized focus group question sets used in both sessions
-
1.
Views on the current screening climate at Access Alliance
-
With regards to colorectal cancer screening by FOBT and breast cancer screening by mammography, how do you think Access Alliance is meeting its goals?
-
-
2.
Barriers to screening at Access Alliance
-
What do you think are some barriers to screening at Access Alliance (please discuss barriers faced by clients, barriers faced by providers, and system-level barriers)?
-
What do you think are some factors that might encourage screening?
-
-
3.
Potential solutions and tools
-
Do you have any suggestions for a health promotion resource or tool that can improve the rates of cancer screening at Access Alliance?
-
Would you suggest that this tool be aimed at clients, providers, or at the organization level?
-
In the past, have there been other resources or tools that have been used at Access Alliance to improve cancer screening rates? Do you think they were effective?
-
Rights and permissions
About this article
Cite this article
Wang, A.M.Q., Yung, E.M., Nitti, N. et al. Breast and Colorectal Cancer Screening Barriers Among Immigrants and Refugees: A Mixed-Methods Study at Three Community Health Centres in Toronto, Canada. J Immigrant Minority Health 21, 473–482 (2019). https://doi.org/10.1007/s10903-018-0779-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10903-018-0779-5