Abstract
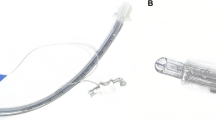
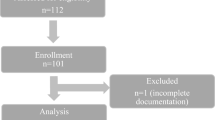
Placing an esophageal temperature probe (ETP) in the optimal esophageal site is important in various anesthetic and critical care settings to accurately monitor the core temperature of a pediatric patient. However, no reported study has provided a formula to calculate the optimal insertion depth of ETP placement in children based on direct measurement of the optimal depth. The aim of this study was to develop a simple and reliable method to determine the optimal depth of ETP placement in children via their mouth. Using preoperative chest computed tomography scans, intraoperative chest X-rays, and the actual depth of ETP insertion, we measured the optimal depth of ETP placement retrospectively in 181 children aged 3–13 years who underwent minimally invasive repairs of the pectus excavatum and removal of a pectus bar. A linear regression analysis was performed to assess the correlation of the optimal depth of ETP placement with the children’s age, weight, and height. The optimal depth of ETP placement had a greater correlation with height than with age or weight, and the best-fit equation was ‘0.180 × height + 6.749 (cm) (R2 = 0.920).’ We obtained three simplified formulae, which showed no statistically significant difference in predicting the optimal depth of ETP placement: height/6 + 8 (cm), height/5 + 4 (cm), and height/5 + 5 (cm). The optimal depth of ETP via children’s mouths has a close correlation with height and can be calculated with a simple formula ‘height/5 + 5 (cm)’.



Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- ETP:
-
Esophageal temperature probe
References
Sessler DI. Temperature monitoring and perioperative thermoregulation. Anesthesiology. 2008;109:318–38.
Sarti A, Recanati D, Furlan S. Thermal regulation and intraoperative hypothermia. Minerva Anestesiol. 2005;71:379–83.
Ohlson KB, Mohell N, Cannon B, Lindahl SG, Nedergaard J. Thermogenesis in brown adipocytes is inhibited by volatile anesthetic agents. A factor contributing to hypothermia in infants? Anesthesiology. 1994;81:176–83.
Xiong Y, Sun Y, Ji B, Liu J, Wang G, Zheng Z. Systematic review and meta-analysis of benefits and risks between normothermia and hypothermia during cardiopulmonary bypass in pediatric cardiac surgery. Paediatr Anaesth. 2015;25:135–42.
Shankaran S, Laptook AR, Ehrenkranz RA, et al. Whole-body hypothermia for neonates with hypoxic-ischemic encephalopathy. N Engl J Med. 2005;353:1574–84.
Gluckman PD, Wyatt JS, Azzopardi D, et al. Selective head cooling with mild systemic hypothermia after neonatal encephalopathy: multicentre randomised trial. Lancet. 2005;365:663–70.
Perkin RM, Anas N. Pulmonary artery catheters. Pediatr Crit Care Med. 2011;12:S12–20.
Snoek AP, Saffer E. Agreement between lower esophageal and nasopharyngeal temperatures in children ventilated with an endotracheal tube with leak. Paediatr Anaesth. 2016;26:213–20.
Robinson J, Charlton J, Seal R, Spady D, Joffres MR. Oesophageal, rectal, axillary, tympanic and pulmonary artery temperatures during cardiac surgery. Can J Anaesth. 1998;45:317–23.
Robinson JL, Seal RF, Spady DW, Joffres MR. Comparison of esophageal, rectal, axillary, bladder, tympanic, and pulmonary artery temperatures in children. J Pediatr. 1998;133:553–6.
Kaufman RD. Relationship between esophageal temperature gradient and heart and lung sounds heard by esophageal stethoscope. Anesth Analg. 1987;66:1046–8.
Bloch EC, Ginsberg B, Binner RA Jr. The esophageal temperature gradient in anesthetized children. J Clin Monit. 1993;9:73–7.
Brengelmann GL, Johnson JM, Hong PA. Electrocardiographic verification of esophageal temperature probe position. J Appl Physiol Respir Environ Exerc Physiol. 1979;47:638–42.
Sato D, Teramoto K, Kitajima H, et al. Measuring luminal esophageal temperature during pulmonary vein isolation of atrial fibrillation. World J Cardiol. 2012;4:188–94.
Whitby JD, Dunkin LJ. Oesophageal temperature differences in children. Br J Anaesth. 1970;42:1013–5.
Mekjavic IB, Rempel ME. Determination of esophageal probe insertion length based on standing and sitting height. J Appl Physiol. 1985;1990(69):376–9.
Sanchez-Quintana D, Cabrera JA, Climent V, Farre J, Mendonca MC, Ho SY. Anatomic relations between the esophagus and left atrium and relevance for ablation of atrial fibrillation. Circulation. 2005;112:1400–5.
Lemola K, Sneider M, Desjardins B, et al. Computed tomographic analysis of the anatomy of the left atrium and the esophagus: implications for left atrial catheter ablation. Circulation. 2004;110:3655–60.
Makic MB, Lovett K, Azam MF. Placement of an esophageal temperature probe by nurses. AACN Adv Crit Care. 2012;23:24–31.
Strobel CT, Byrne WJ, Ament ME, Euler AR. Correlation of esophageal lengths in children with height: application to the Tuttle test without prior esophageal manometry. J Pediatr. 1979;94:81–4.
Acknowledgements
The authors would like to thank Joon-Yong Jung, a radiologist, Department of Radiology, Seoul St. Mary’s Hospital for X-ray and CT scan analyses, and Su Jung Park, a biostatistician, Department of Biostatistics, College of Medicine, The Catholic University of Korea for help with the statistical analysis.
Funding
This study was funded entirely by the Department of Anesthesiology and Pain Medicine at Seoul St. Mary’s Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
We declare that there were no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hong, S.H., Lee, J., Jung, JY. et al. Simple calculation of the optimal insertion depth of esophageal temperature probes in children. J Clin Monit Comput 34, 353–359 (2020). https://doi.org/10.1007/s10877-019-00327-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-019-00327-7