Abstract
Purpose
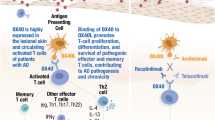
The class IV semaphorin Sema4A is critical for efficient TH1 differentiation and Sema4a −/− mice exhibit impaired TH1 immune responses. However, the role of Sema4A in TH2 cell-mediated allergic diseases has not been fully studied. The aim of this study was to clarify the regulatory role possessed by Sema4A in mouse models of allergic diseases, particularly allergic asthma.
Methods
Sema4a −/− mice on a BALB/c background were examined for the development of allergic diseases. To induce experimental asthma, mice were sensitized with ovalbumin (OVA) followed by intranasal challenges with OVA. After challenge, airway hyperreactivity (AHR) and airway inflammation were evaluated. The role of Sema4A in asthma was examined using Sema4a −/− mice and Sema4A-Fc fusion proteins. The direct effects of Sema4A-Fc on antigen-specific effector CD4+ T cells were also examined.
Results
A fraction of Sema4a −/− BALB/c mice spontaneously developed skin lesions that resembled atopic dermatitis (AD) in humans. Furthermore, AHR, airway inflammation, and TH2-type immune responses were enhanced in Sema4a −/− mice compared to wild type (WT) mice when immunized and challenged with OVA. In vivo systemic administration of Sema4A-Fc during the challenge period ameliorated AHR and lung inflammation and reduced the production of TH2-type cytokines in WT mice. The inhibitory effects of Sema4A on airway inflammation were also observed in mice deficient in Tim-2, a Sema4A receptor. Finally, we showed that Sema4A-Fc directly inhibited IL-4-producing OVA-specific CD4+ T cells.
Conclusion
These results demonstrate that Sema4A plays an inhibitory role in TH2-type allergic diseases, such as allergic asthma.






Similar content being viewed by others
References
Zheng T, Yu J, Oh MH, Zhu Z. The atopic march: progression from atopic dermatitis to allergic rhinitis and asthma. Allergy Asthma Immunol Res. 2011;3:67–73.
Von Mutius E. Gene-environment interactions in asthma. J Allergy Clin Immunol. 2009;123:3–11.
Zhang J, Paré PD, Sandford AJ. Recent advances in asthma genetics. Respir Res. 2008;9:4.
Cohn L, Elias JA, Chupp GL. Asthma: mechanisms of disease persistence and progression. Annu Rev Immunol. 2004;22:789–815.
Hamid Q, Tulic M. Immunobiology of asthma. Annu Rev Physiol. 2009;71:489–507.
Leung DY, Bieber T. Atopic dermatitis. Lancet. 2003;361:151–60.
Broide DH. Allergic rhinitis: pathophysiology. Allergy Asthma Proc. 2010;31:370–4.
Bardana Jr EJ. 10 Occupational asthma. J Allergy Clin Immunol. 2008;121(2Suppl):S408–11.
Wegmann M. Th2 cells as targets for therapeutic intervention in allergic bronchial asthma. Expert Rev Mol Diagn. 2009;9:85–100.
Holgate ST. Pathogenesis of asthma. Clin Exp Allergy. 2008;38:872–97.
Barrett NA, Austen KF. Innate cells and T helper 2 cell immunity in airway inflammation. Immunity. 2009;31:425–37.
Kim HY, DeKruyff RH, Umetsu DT. The many paths to asthma: phenotype shaped by innate and adaptive immunity. Nat Immunol. 2010;11:577–84.
Lloyd CM, Hessel EM. Functions of T cells in asthma: more than just T(H)2 cells. Nat Rev Immunol. 2010;10:838–48.
Paul WE, Zhu J. How are T(H)2-type immune responses initiated and amplified? Nat Rev Immunol. 2010;10:225–35.
Lemanske Jr RF, Busse WW. Asthma: clinical expression and molecular mechanisms. J Allergy Clin Immunol. 2010;125(2 suppl 2):S95–S102.
Robinson DS. The role of the T cell in asthma. J Allergy Clin Immunol. 2010;126:1081–91.
Kikutani H, Kumanogoh A. Semaphorins in interactions between T cells and antigen-presenting cells. Nat Rev Immunol. 2003;3:159–67.
Mizui M, Kumanogoh A, Kikutani H. Immune Semaphorins: novel features of neural guidance molecules. J Clin Immunol. 2009;29:1–11.
Suzuki K, Kumanogoh A, Kikutani H. Semaphorins and their receptors in immune cell interactions. Nat Immunol. 2008;9:17–23.
Kumanogoh A, Marukawa S, Suzuki K, Takegahara N, Watanabe C, Ch’ng E, Ishida I, Fujimura H, Sakoda S, Yoshida K, Kikutani H. ClassIV semaphorin Sema4A enhances T-cell activation and interacts with Tim-2. Nature. 2002;419:629–33.
Kumanogoh A, Shikina T, Suzuki K, Uematsu S, Yukawa K, Kashiwamura S, Tsutsui H, Yamamoto M, Takamatsu H, Ko-Mitamura EP, Takegahara N, Marukawa S, Ishida I, Morishita H, Prasad DV, Tamura M, Mizui M, Toyofuku T, Akira S, Takeda K, Okabe M, Kikutani H. Nonredundant roles of Sema4A in the immune system: defective T cell priming and Th1/Th2 regulation in Sema4A-deficient mice. Immunity. 2005;22:305–16.
Glaab T, Taube C, Braun A, Mitzner W. Invasive and noninvasive methods for studying pulmonary function in mice. Respir Res. 2007;8:63.
Pichavant M, Goya S, Hamelmann E, Gelgfand EW, Umetsu DT. Animal models of airway sensitization. Curr Protoc Immunol. 2007;15:18.
Nembrini C, Marsland BJ, Kopf M. IL-17-producing T cells in lung immunity and inflammation. J Allergy Clin Immunol. 2009;123:986–94.
McKinley L, Alcorn JF, Peterson A, Dupont RB, Kapadia S, Logar A, Henry A, Irvin CG, Piganelli JD, Ray A, Kolls JK. TH17 cells mediate steroid-resistant airway inflammation and airway hyperresponsiveness in mice. J Immunol. 2008;181:4089–97.
Fujiwara M, Hirose K, Kagami S, Takatori H, Wakashin H, Tamachi T, Watanabe N, Saito Y, Iwamoto I, Nakajima H. T-bet inhibits both TH2 cell-mediated eosinophil recruitment and TH17 cell-mediated neutrophil recruitment into the airways. J Allergy Clin Immunol. 2007;119:662–70.
Smith EP, Shanks K, Lipsky MM, DeTolla LJ, Keegan AD, Chapoval SP. Expression of neuroimmune semaphorins 4A and 4D and their receptors in the lung is enhanced by allergen and vascular endothelial growth factor. BMC Immunol. 2011;12:30.
Freeman GJ, Casasnovas JM, Umetsu DT, Dekruyff RH. TIM genes: a family of cell surface phosphatidylserine receptors that regulate innate and adaptive immunity. Immunol Rev. 2010;235:172–89.
Rennert PD, Ichimura T, Sizing ID, Bailly V, Li Z, Rennard R, McCoon P, Plablo L, Miklasz S, Tarilonte L, Bonventre JV. T cell, Ig domain, mucin domain-2 gene-deficient mice reveal a novel mechanism for the regulation of Th2 immune responses and airway inflammation. J Immunol. 2006;117:4311–21.
Lambrecht BN, Hammad H. The role of dendritic and epithelial cells as master regulators of allergic airway inflammation. Lancet. 2010;376:835–43.
Wisniewski JA, Borish L. Novel cytokines and cytokine-producing T cells in allergic disorders. Allergy Asthma Proc. 2011;32:83–94.
Neill DR, Wong SH, Bellosi A, Flynn RJ, Daly M, Langford TK, Bucks C, Kane CM, Fallon PG, Pannell R, Jolin HE, McKenzie AN. Nuocytes represent a new innate effector leukocyte that mediates type-2 immunity. Nature. 2010;464:1367–70.
Barlow JL, Bellosi A, Hardman CS, Drynan LF, Wong SH, Cruickshank JP, McKenzie AN. Innate IL-13-producing nuocytes arise during allergic lung inflammation and contribute to airways hyperreactivity. J Allergy Clin Immunol. 2012;129:191–8.
Yoshimoto T, Yoshimoto T, Yasuda K, Mizuguchi J, Nakanishi K. IL-27 suppresses Th2 cell development and Th2 cytokines production from polarized Th2 cells: a novel therapeutic way for Th2-mediated allergic inflammation. J Immunol. 2007;179:4415–23.
Pouliot P, Camateros P, Radzioch D, Lambrecht BN, Olivier M. Protein tyrosine phosphatases regulate asthma development in a murine asthma model. J Immunol. 2009;182:1334–40.
Matsunaga Y, Inoue H, Fukuyama S, Yoshida H, Moriwaki A, Matsumoto T, Matsumoto K, Asai Y, Kubo M, Yoshimura A, Nakanishi Y. Effects of Janus kinase inhibitor, pyridone 6, on airway responses in a murine model of asthma. Biochem Biophys Res Commun. 2011;404:261–7.
Walter DM, Wong CP, Dekruyff RH, Berry GJ, Levy S, Umetsu DT. Il-18 gene-transfer by adenovirus prevents the development of and reverses established allergen-induced airway hyperreactivity. J Immunol. 2001;166:6392–8.
Park JW, Min HJ, Sohn JH, Kim JY, Hong JH, Sigrist KS, Glimcher LH, Hwang ES. Restoration of T-box-containing protein expressed in T cells protects against allergen-induced asthma. J Allergy Clin Immunol. 2009;123:479–85.
Finotto S, De Sanctis GT, Lehr HA, Herz U, Buerke M, Schipp M, Bartsch B, Atreya R, Schmitt E, Galle PR, Renz H, Neurath MF. Treatment of allergic airway inflammation and hyperresponsiveness by antisense-induced local blockade of GATA-3 expression. J Exp Med. 2001;193:1247–60.
Nakatsuji Y, Okuno T, Moriya M, Sugimoto T, Kinoshita M, Takamatsu H, Nojima S, Kimura T, Kang S, Ito D, Nakagawa Y, Toyofuku T, Takata K, Nakano M, Kubo M, Suzuki S, Matsui-Hasumi A, Uto-Konomi A, Ogata A, Mochizuki H, Sakoda S, Kumanogoh A. Evaluation of Sema4A Implicates Th Cell Skewing and the Efficacy of IFN-β Therapy in Multiple Sclerosis. J Immunol. 2012;188:4858–65.
Acknowledgments
We thank Ms. K. Kubota for excellent secretarial assistance. We also thank T. Sugimoto, T. Shiozaki, T. Yazawa, M. Ishiguro and M. Morihana for technical support.
Conflict of interest
The authors declare that they have no conflict of interest.
All sources of funding
This research was supported by a Grant-in-Aid for Scientific Research (S) from the Ministry of Education, Culture, Sports, Science and Technology of Japan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Morihana, T., Goya, S., Mizui, M. et al. An Inhibitory Role for Sema4A in Antigen-Specific Allergic Asthma. J Clin Immunol 33, 200–209 (2013). https://doi.org/10.1007/s10875-012-9798-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-012-9798-5