Abstract
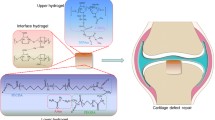
A layered gelatin-chitosan hydrogel with graded composition was prepared via photocrosslinking to simulate the polysaccharide/collagen composition of the natural tissue and mimic the multi-layered gradient structure of the cartilage-bone interface tissue. Firstly, gelatin and carboxymethyl chitosan were reacted with glycidyl methacrylate (GMA) to obtain methacrylated gelatin (Gtn-GMA) and carboxymethyl chitosan (CS-GMA). Then, the mixed solutions of Gtn-GMA in different methacrylation degrees with CS-GMA were prepared to form the superficial, transitional and deep layers of the hydrogel, respectively under the irradiation of ultraviolet light, while polyhedral oligomeric silsesquioxane was introduced in the deep layer to improve the mechanical properties. Results suggested that the pore sizes of the superficial, transitional and deep layers of the layered hydrogel were 115 ± 30, 94 ± 34, 51 ± 12 μm, respectively and their porosities were all higher than 80 %. The compressive strengths of them were 165 ± 54, 565 ± 50 and 993 ± 108 kPa, respectively and the strain of the gradient hydrogel decreased along the thickness direction, similar to the natural tissue. The in vitro cytotoxicity results showed that the hydrogel had good cytocompatibility and the in vivo repair results of osteochondral defect demonstrated remarkable recovery by using the gradient gelatin-chitosan hydrogel, especially when the hydrogel loading transforming growth factor-β1. Therefore, it was suggested that the prepared layered gelatin-chitosan hydrogel in this study could be potentially used to promote cartilage-bone interface tissue repair.
Similar content being viewed by others
1 Introduction
Osteochondral defects containing damages of both cartilage and subchondral bone are common in symtomatic knees as an increasing health threat. Tissue engineering combining of cells, scaffolds and growth factors has been considered as a promising strategy to repair osteochondral defects [1–3]. However, the functional repair of articular cartilage remains a big challenge because of the gradient changes in composition and properties of the cartilage-bone interface-tissue [3–5]. The cartilage has a limited self-repair capacity after injury, because of its inherent avascular and alymphatic nature [3, 6, 7]. Recently, there are many investigations on the improvement of the osteochondral defect repair by providing a layered osteochondral scaffold to induce the simultaneous regeneration of articular cartilage and the subchondral bone [1, 4, 8, 9].
Hydrogels have gained much attention as the cartilage tissue engineering scaffolds because the hydrated polymer networks of the hydrogel can retain great quantity of water, benefit the exchange of nutrients and metabolite wastes, and bear mechanical loading for enhanced matrix production and organization [10–12]. Among them, poly(ethylene glycol) (PEG) hydrogel was most prevalent class of synthetic materials for cartilage tissue engineering. PEG hydrogels are relatively inert and biocompatible, and could support chondrocytes and mesenchymal stem cells growth, but it was limited to support specific cartilage matrix production identical to the natural tissue [13]. Natural hydrogels based on proteins and polysaccharides are also helpful for cartilage regeneration. Collagen was an abundant protein within native articular cartilage, but collagen hydrogels were very soft and easily contracted during culture [14]. Gelatin (Gtn) is a denatured collagen, it exhibits well cell adhesion properties with cell binding motifs, that makes it an attractive material for cartilage tissue engineering [15]. Carboxymethyl chitosan (CS) is a derivative of chitosan which has been widely used in biomedical applications. A double-network complex hydrogel prepared by CS and oxidized gellan gum could maintain its original shape and enhance the cell viabilities of encapsulated chondrocytes [12].
It was reported that the spatially-varying matrix composition and mechanical properties by preparation a three-layer hydrogel with different compositions in the top layer (PEG/chondroitin sulfate/metalloproteinase-sensitive peptides), the middle layer (PEG/chondroitin sulfate) and the bottom layer (PEG/hyaluronic acid) could direct bone marrow-derived stem cells (BMSCs) differentiate into multiple, spatially distinct cell phenotypes within the multi-layered scaffold and stimulate regeneration of the complex tissues [9]. The Gtn-CS hydrogel with well pro-chondrogenic properties, could be a promising scaffold for cartilage regeneration and will be the focus of this study.
Although hydrogels have their favorable properties as the tissue engineering scaffold, one of the limitations is their insufficient mechanical properties [16]. The combination of the hydrogel with hydroxyapatite (HA) can effectively improve the mechanical properties [4]. For example, the HA-reinforced poly(vinyl achohol) (HA/PVA) hydrogel exhibited superior physical and mechanical properties than the pure PVA hydrogel did [4], and it also showed osteoconductivity as an articular cartilage implant [17]. As hybrid organic–inorganic molecules, polyhedral oligomeric silsesquioxanes (POSS) form well-dispersed nanocomposites with precisely size-controlled hard blocks within the soft organic matrix [18]. Previous reports have demonstrated that incorporation of POSS into polymers could improve the mechanical stability [19, 20]. For example, the shear modulus of the PEG-POSS hybrid hydrogels spanned a range from 0.3 to 4.0 MPa, higher than the most hydrogels reported [20]. In this study, octavinyl POSS (OV-POSS) was introduced in the deep layer of the Gtn-CS hydrogel to obtain higher mechanical strength.
In order to enhance the cell performance, one or more growth factors can be loaded in a tissue engineering scaffold [21, 22]. For example, transforming growth factor β1 (TGF-β1) was covalently tethered in the poly(ethylene glycol) hydrogel [23]. After the incorporation of chondrocytes, the immobilized TGF-β1 demnostrated more extracellular matrix production than the soluble TGF-β1 did. In our previous study, a graded Gtn-CS hydrogel/poly(lactide-co-glycolide) (PLGA) scaffold was ever prepared for the osteochondral defect repair, in which the Gtn-CS hydrogel containing TGF-β1 was used for chondrogenesis, while the PLGA scaffold loading bone morphogenetic protein-2 (BMP-2) for osteogenesis [24]. The results showed that regenerated hyaline-like cartilage surface and subchondral bone integrated with the native tissues by using this scaffold.
In this study, a layered Gtn-CS hydrogel with graded compositions and mechanical properties was prepared via photocrosslinking to induce the osteochondral regeneration by a three-layered structure with different compositions in the top, middle and bottom layers. It was hypothesized that the different physical and chemical properties dictating by the composition could be propitious to cartilage and bone repair in the cartilage-bone defect. TGF-β1 was also encapsulated into the layered Gtn-CS hydrogel to enhance chondrogenesis. The properties of the hydrogel including morphology, swelling ratio and mechanical properties were studied, and in vitro cytotoxicity and in vivo implantation were performed to evaluate the biocompatibility and the in vivo repair ability.
2 Materials and methods
2.1 Materials
Gelatin (Gtn, Porcine Type A, 200 Bloom), poly(ethylene glycol) dimethacrylate (PEGDMA, M n = 875 Da), 2-hydroxy-1-[4-(hydroxyeth-oxyphenyl]-2-methyl-1-propanone (Irgacure 2959), 3-(4,5-dimethythiazol-2-yl)-2,5 dipheyl tetrazolium bromide (MTT), fluorescein isothiocyanate-dextran (FD70S, M w = 70 kDa) were purchased from Sigma. Carboxymethyl chitosan (CS, M w = 9 kDa, ≥95 % degree of deacetylation, 82 % degree of carboxymethylation) was purchased from Shanghai Demo Pharmaceutical Technology Co., Ltd. Glycidyl methacrylate (GMA) was purchased from Shanghai TCI Chemical Industry Co., Ltd. OV-POSS was purchased from Hybrid Plastics. Transforming growth factor-β1 (TGF-β1) was purchased from Shenzhen Dakota Biotech Company Limited. Fetal bovine serum (FBS) was purchased from Gibco (USA), and α-MEM was supplied by Hyclone, USA. Other chemicals were all supplied by Kermel Reagent Company, Tianjin, China.
2.2 Synthesis of Gtn-GMA and CS-GMA
Gtn was methacrylated following a protocol adopted from Pierce et al. [25]. Briefly, 2.5 g of Gtn was dissolved in 25 mL of carbonate/bicarbonate buffer (0.05 M, pH = 9.6) at 50 °C until complete dissolution. Then, a certain amount of GMA was added into the Gtn solution, and the reaction was allowed to keep stir at 50 °C for 3 h under nitrogen. The product was precipitated in ethanol at room temperature. The methacrylated gelatin (Gtn-GMA) was dissolved in water, dialyzed in a large amount of distilled water for 3 days and then lyophilized for 48 h. 1H nuclear magnetic resonance (1H NMR) spectra of Gtn before and after GMA modification were recorded on a Varian spectrometer (Bruker AVANCE III 400 MHz, Switzerland) in D2O (Fig. 1) to confirm the methacrylation of Gtn. By introducing different amounts of GMA in 10, 20 or 30 mL, three methacrylation degrees of Gtn-GMA were prepared and designated as G1, G2 and G3, respectively. The methacrylation degree of gelatin methacrylation was measured by quantitatively detecting the amount of amino groups in the gelatin before and after the reaction using ninhydrin method [26].
CS was methacrylated following a protocol adopted from Poon et al. [27]. Briefly, CS (1 g) was dissolved in 100 mL distilled water, then 5 mL triethylamine, 15 mL GMA and 5 g tetrabutyl ammonium bromide were added in sequence and stirred for 3 days at ambient temperature. After 1 h of heating at 60 °C, the solution was precipitated in ethanol. The precipitated product was collected by centrifugation and then dissolved in water and dialyzed in water for 2 days in order to completely remove any excess reactants. The solution was then lyophilized for 2 days to get the methacrylated carboxymethyl chitosan (CS-GMA). 1H NMR spectra of CS and CS-GMA were recorded in D2O to verify the methacrylation degree of methacrylate groups in the CS-GMA, as shown in Fig. 1.
2.3 Preparation of the layered Gtn-CS hydrogel
A layered Gtn-CS hydrogel with biomimetic multi-layer for cartilage repair was prepared in this study. A schematic representation of the layered hydrogel preparation is shown in Fig. 2. The three layers of the layered hydrogel, i.e., superficial, transitional and deep layers that mimicked the superficial, transitional and deep zones of cartilage, were prepared and designated as S, T and D samples, respectively. The composition in the three layers was controlled as CS-GMA/G1 (the total amount of CS-GMA and G1 was 18 % w/v) and PEGDMA (8 %, w/v) in the superficial layer, CS-GMA/G2 (the total amount of CS-GMA and G1 was 10 % w/v) and PEGDMA (20 %, w/v) in the transitional layer and CS-GMA/G3 (the total amount of CS-GMA and G1 was 15 % w/v), PEGDMA (30 %, w/v) and OV-POSS (10 %, w/v) in the deep layer. The mass ratio of CS-GMA and Gel-GMA were controlled as 1:8 (wt/wt) and the amount of photoinitiator Igracure 2959 in each polymer solution was 2 % (w/w) relative to the total amount of Gtn-GMA and CS-GMA. The solutions (50 μL) from deep layer to superficial layer were rapidly transferred into cylindrical molds (5 mm internal diameter) and exposed for 30 min under UV light (365 nm) (Spectrollinker, XL-1000 UV Crosslinker, USA). Then the prepared hydrogel was immersed into distilled water to remove the unreacted substances.
Schematic representation of preparation of the layered Gtn-CS hydrogel with graded compositions via photocrosslinking. a Gtn-GMA, CS-GMA and PEGDMA in superficial (S) and transitional layers (T); b Gtn-GMA, CS-GMA and OV-POSS in the deep layer (D); c graded compositions of the layered Gtn-CS hydrogel. G1, G2 and G3 are referred to the methacrylated gelatin (Gtn-GMA) with 22, 39 and 43 % of methacrylation degrees, respectively. The methacrylated carboxymethyl chitosan (CS-GMA) has a methacrylation degree of 12 %
To evaluate the effect of the TGF-β1 on the cartilage-bone defect repair, the layered hydrogel (designated as O group) and the layered hydrogel loaded with TGF-β1 (T group) were tested in this experiment. The T sample was prepared according to the following method. TGF-β1 in 10 μg was dissolved in 150 μL PBS solution (containing 150 μg BSA). Then, TGF-β1 solution with different volumes was added into the polymer solutions, making the loading TGF-β1 amount in the superficial and transitional layers of the layered hydrogel was 200 and 64 ng, respectively and the deep layer was free of the growth factor. Under UV condition, the gradient-loaded TGF-β1 hydrogel was prepared with the size of 5 mm in diameter and 6 mm in height. From the surface to the bottom, the layered hydrogel was divided into three layers, and the thickness of each layer was about 2 mm.
2.4 Scanning electron microscopy
The morphology of freeze-dried hydrogels in different layers as well as the interfaces between the layers was viewed under a scanning electron microscope (SEM, Hitachi S-4800, Japan) after coated with gold. Pore sizes of each layer hydrogel were measured from SEM micrographs using photoshop software, all results were obtained from at least 50 measurements each layers.
2.5 Porosity and swelling ratio
The porosity of the layered Gtn-CS hydrogel was determined by a modified liquid replacement according to our previous study [28]. To measure the equilibrium swelling ratios of each layer hydrogel, the freeze-dried hydrogels were weighed (m d), then submerged in PBS (pH 7.4) at 37 °C until the weight reach equilibrium (m w). Swelling ratio of the each hydrogel was defined as 100 % × (m w − m d)/m d.
2.6 Mechanical tests
The compressive test of three layers of the Gtn-CS hydrogel was performed by using a tensile testing machine (Testmetric, M350-20KN, UK) at a crosshead speed of 1 mm/min at room temperature. The sample in each layer was prepared as cylindrical blocks with a size of 8 mm in diameter and 4 mm in height. The compressive stress and strain responses were monitored. The slope of the linear region was defined as the compressive modulus of the hydrogel, and the stress at 10 % strain was referred to as the compression strength. Five samples in each group were tested to obtain average values and standard deviations.
An optimized digital image correlation technique was applied and the depth-dependent normal strain in the layered Gtn-CS hydrogel under compression was measured [29]. The loading rate of mechanical loading system is 1 mm/min and the load capacity is 100 N. The captured sequential images were analyzed using the image processing software to generate the displacement and the strain. The essence of this technique is to automatically measure displacements by tracking the changes in position in digitized images of the object’s surface. The commercial iron oxide nanoparticles as the fiducial marker, that were scattered on the layered hydrogel sample, were observed and the relative position of these nanoparticles gave rise to a random pattern of the sample surface. Then, the strain of the different position in the layered hydrogel could be calculated in comparison with the cartilage of a pig.
2.7 In vitro release study
FD70S was used as the model substance to study the release behavior. Briefly, 0.5 mL FD70S solution (5 mg/mL) was added to 1.5 mL polymer solution of each layer to prepare the FD70S-loaded multi-layered hydrogel. Three layers of the Gtn-CS hydrogel (S, T and D samples) were immersed into phosphate buffered saline (PBS, pH 7.4), respectively for 10 min to remove unloaded FD70S and determine the encapsulation efficiency. For in vitro release study, the S, T and D samples were immersed in 4 mL PBS solution and incubated in a water shaker at 37 °C. At predetermined times, 1 mL PBS was removed for analysis, and 1 mL fresh PBS was added. The released FD70S in the solution was assayed by measuring the fluorescence intensity (485 nm of the excitation wavelength, 528 nm of the emission wavelength) using the enzymelinked immunosorbent assay (Synergy HT, US Biotech). The cumulative release of released FD70S was calculated according to the previous report [30, 31].
2.8 In vitro cytotoxicity
The in vitro cytotoxicity of the layered hydrogels was examined according to the reported method [32]. Each layer of the multi-layered hydrogel was incubated in α-MEM medium (25 mg/mL) maintained at 37 °C in 5 % CO2 for 24 h to get the hydrogel extracts. The L929 mouse fibroblast cells were placed in a 96-well plate at a seeding density of 4,000 cells per well. The culture medium was supplemented with 10 % FBS and 200 μL extract solution was added into per well. After another 24, 48, 72 h of incubation, MTT assay was performed to determine the in vitro cytotoxicity. The α-MEM medium and 10 % dimethylsulfoxide were negative control and the positive control, respectively. All reported values were the means of five replicates. The relative growth rate (RGR) of L929 mouse fibroblast cells was calculated as 100 % × A s/A c, where, A s and A c were referred to the absorptions of the extracted fluid of the hydrogel sample and the negative control sample, respectively.
2.9 In vivo animal surgery and histological analysis
New Zealand white rabbits of 2–2.5 kg were used for in vivo experiments, and the procedures were approved by the Tianjin Experimental Animal Management Ordinance, China. General anesthesia was induced via an intravenous injection of Xylazine Sailaqin Zhusheye (0.4 mL/kg). Bilateral patellar groove osteochondral defects of 5 mm in diameter and 6 mm in depth were created in the patellar groove of the adult rabbits using a stainless steel drill according to the previous report [33]. Then, the different samples (O and T samples) were implanted into the rabbit osteochondral defects (two rabbits for per sample). Subsequently, patella was repositioned, and trochlea, muscle, and skin were closed with sutures. All the rabbits were housed in separate cages and allowed to move freely after surgery. The repaired osteochondral tissues were assessed by macroscopical and histological analysis at 1 and 2 months after the operation. For histological analysis, the harvested samples were fixed in 10 % neutral buffered formalin for 48 h, decalcified in mixed acid solution for 7 days, and embedded in paraffin. Then the sections were stained with hematoxylin and eosin (H&E) before the observation.
2.10 Statistical analysis
The data were presented as mean ± standard deviation with no less than triplicates for each group. Statistical analyses were performed using a Student t test, and difference with P < 0.05 was considered statistically significant.
3 Results
3.1 Methacrylation of Gtn and CS
In order to obtain the chemically crosslinkable Gtn-CS hydrogel, GMA and CS were methacrylated with GMA through the reaction between epoxy groups of GMA and NH2 groups of Gtn or CS [25, 27]. In the presence of the basic catalyst, transesterification also possibly occurred between epoxy groups of GMA and hydroxyl groups of CS [27]. The 1H NMR spectra of Gtn and CS before and after methacrylation are shown in Fig. 1. Analysis of 1H NMR confirmed the methacrylation of Gtn and CS, and the methacrylation degree of Gtn-GMA and CS-GMA was also evaluated. The peaks at about 5.6 and 6.0 ppm in Fig. 1 suggested that GMA was successfully methacrylated on Gtn and CS. The methacrylation degrees of G1, G2, G3 of Gtn-GMA were 22, 39 and 43 %, respectively, and the methacrylation degree of CS-GMA was 12 %.
3.2 Graded compositions and morphology of the layered Gtn and CS hydrogel
Hydrogel is useful in cartilage tissue engineering as it presents suitable three-dimensional (3D) microenvironments for tissue formation and defect repair. In this study, a biomimetic layered Gtn-CS hydrogel with graded compositions was designed and prepared. The compositions of superficial, transitional and deep layers in the hydrogel are illustrated in Fig. 2. The superficial layer contained a low methacrylation degree (22 %) of Gtn-GMA and CS-GMA, the transitional layer included a middle methacrylation degree (39 %) of Gtn-GMA and CS-GMA, and the deep layer composition consisted of a high methacrylation degree (43 %) of Gtn-GMA, CS-GMA and OV-POSS. The thickness of each layer is about 2 mm. Because of the solutions of the deep layer, the transitional layer and the superficial layer were added into cylindrical mold one by one, and the whole hydrogel was prepared under the same condition of exposure to UV light, it can be assumed that the hydrogel possesses interconnectivity.
Figure 3 displays the SEM images of the different layers of the multi-layered hydrogel as well as the interface morphology between the layers. The Gtn-CS hydrogel showed porous structure and interconnectivity. The pore sizes of the superficial layer, transitional layer and deep layer were 115 ± 30, 94 ± 34 and 51 ± 12 μm, respectively. And, it could also be seen that there were some POSS aggregated particles on the wall of the deep layer. The porosities of the superficial, transitional and deep layers were 82 ± 2, 86 ± 5 and 82 ± 3 %, respectively. It is assumed that the porosity value above 80 % is suitable to cartilage or bone tissue regeneration.
3.3 Swelling ratio
The swelling ratio of a hydrogel is an important factor affecting its properties. The swelling ratios of the layered Gtn-CS hydrogel in different layers were related with the compositions. As shown in Fig. 4, the swelling ratios of the superficial, transitional and deep layers were 551 ± 23, 331 ± 12 and 198 ± 7 %, respectively, decreasing from the superficial layer to the deep layer.
3.4 Mechanical properties
Figure 5 displays the mechanical properties of the different layers of the layered Gtn-CS hydrogel. The compressive strength and compressive modulus of the superficial, transitional and deep layers of the layered hydrogel were 165 ± 54, 565 ± 50, 993 ± 108 and 314 ± 31, 1076 ± 164, 2174 ± 142 kPa, respectively, increasing from the superficial layer to the deep layer. Figure 6 shows the photomicrograph of the layered hydrogel before and after deformation (Fig. 6a) and the strain changes versus the depth of the layered hydrogel and pig cartilage (Fig. 6b). The microscopic images of a section of cartilage sample before and after loading can be observed, and the normal strain can be determined according to the previous report [29]. It was shown that the normal strain value decreased along the depth, and the increasing amplitude of the normal strain was largest in the superficial layer. The fitting data suggested that the variation trend of the layered Gtn-CS hydrogel was similar to the natural cartilage.
3.5 In vitro release
To evaluate the spatially controlled and localized release behavior, FD70S was loaded in the superficial, transitional and deep layer samples, and the encapsulation efficiencies were about 80, 80 and 85 %, respectively. Figure 7 presents the FD70S release behaviors from the three different layers. As shown in Fig. 7, a burst release in about 20 % occurred for the S sample, but there was less than 15 % of burst releases for the T and D samples. FD70S was released fastest from the S sample and reached 50 % cumulative release on day 27. For the D sample, almost a zero-order release of FD70S was found after the burst release on day 1. The three layers of the layered Gtn-CS hydrogel showed diverse release behaviors in this study.
3.6 In vitro cytotoxicity
The in vitro cytotoxicity assay result is shown in Fig. 8. According to ISO standards (ISO 10993-5, 1999), the RGR values of the S, T and D samples were all higher than 80 %, and the cytotoxity degree was 0 or 1 grade. However, the positive control group exhibited significantly cytotoxity (3 or 4 grade). Compared with the positive control group, the three different layers of the layered Gtn-CS hydrogel showed good cytocompatability. The results reflected that the layered Gtn-CS hydrogel prepared in this experiment could be potentially used as tissue scaffolds for cartilage repair.
3.7 In vivo experiments and histological analysis
The macroscopic observation results after implantation in articular cartilage-bone defect for 1 and 2 months are presented in Fig. 9. It could be seen that the defect in the non-treated blank group was still large and partially filled with disorganized soft fibrous tissue at 1 month and the joint was slightly degenerated. At 2 months, the defect in the non-treated blank group was filled with fibrous tissue and the defect became smaller than 1 month. After implantation of the O sample for 1 month, the defect was covered with one-third whitish cartilage-like tissue, and the defect was smaller than that of the non-treated blank group. For the T group after 1 month implantation, the defect seemed smaller than that of the O group. The regenerated tissue nearly filled with the defect and the white cartilage-like tissue covered almost the entire surface. But, it could also be seen that the regenerated cartilage surface was not smooth and did not integrate with the natural tissue. At 2 months, better cartilage-bone defect repair results were obtained both in the O and T samples. No concavities were observed and it displayed smooth and integrated regenerated tissue surface. Compared with the O sample, the regenerated cartilage surface in the T sample was more perfect.
The H&E staining results are presented in Fig. 10. At 1 month, the defect in the non-treated blank group was mainly filled with fibrous tissue and remained concave where there was a little neocartilage matrix at the periphery. The scaffold would degrade after implantation in vivo to form concavity. In the O group at 1 month, only a part of the cartilage and subchondral bone regenerated and the concavity was clear. In the T group, the concavity became small and fragile cartilage tissue regenerated on the surface, but the regenerated surface did not integrate with the natural tissue surface. After implantation for 2 months, the defect in the non-treated blank group was mainly filled with the fibrous tissue and the concavity was still in sight. Incomplete subchondral bone regenerated under the top fibrocartilaginous tissue was found. In the O sample, there were newly formed cartilage matrix, the new tissues in the defects were partly integrated with the adjacent native tissue, but the cartilage-like tissue was either too thick or too thin compared to the surrounding cartilage tissue. The T group showed new cartilage and subchondral bone regenerated in the defect, and the regenerated cartilage-bone tissue demonstrated a similar morphology to that of the native cartilage-bone tissue. The in vivo implantation results suggested that the multi-layered Gtn-CS hydrogel displayed a good repair result for treatment of articular cartilage-bone defect in vivo for 2 months. Especially, the T hydrogel loading TGF-β1 presented good cartilage and subchondral bone regeneration.
H&E staining images of the cartilage after surgery for 1 and 2 months in knees’ defects (×10). O group: the layered Gtn-CS hydrogel; T group: the layered Gtn-CS hydrogel with TGF-β1; Blank defect: the defect without treatment. The normal and the new defect were positive and negative controls, respectively. C and B represented the cartilage and bone, respectively
4 Discussion
A lot of reports on osteochondral repair focused on creating a multi-layered hydrogel to mimic the properties of articular cartilage [1, 4, 8, 9]. With this purpose, many investigators incorporated natural materials such as collagen, CS and Gtn into hydrogels to aid in mimicking extracellular matrix (ECM) [12, 15]. In order to prepare a multi-layered hydrogel with different properties in each layer to facilitate the osteochondral defect repair, methacrylated Gtn in different methacrylation degrees, methacrylated CS and OV-POSS were used in this study. By changing the chemical composition in each solution for preparation of the superficial, transition and deep layers, the multi-layered Gtn-CS hydrogel exhibited graded transitions in the morphology, swelling ratio and mechanical properties. As shown in Fig. 2, a low methacrylation degree of Gtn-GMA (22 %) was used to prepare the superficial layer, a middle methacrylation degree of Gtn-GMA (39 %) was introduced in the transition layer, and a high methacrylation degree of Gtn-GMA (43 %) together with POSS was added in the deep layer. Furthermore, the total concentration of Gtn-GMA and CS-GMA increased from 8 % in the superficial layer to 15 % in the deep layer.
From the SEM images in Fig. 3, it could be seen that the pores in different layers are connective. Although the global morphology of the multi-layered Gtn-CS hydrogel is not shown, it can also be seen that the pores at the interface of different layers are interlinked. It was assumed that the interconnectivity of the multi-layered Gtn-CS hydrogel were generated during the photocrosslinking process, in which the different solutions for preparation of each layer were added into cylindrical mold one by one, and they was exposed at the same condition under UV light. All the three S, T and D layers exhibited similar porosities above 80 %, but their pore sizes reduced gradually from 115 ± 30 to 51 ± 12 μm. An ideal tissue engineering scaffold should provide 3D environment for cell growth and suitable pore interconnectivity for transporting nutrition and wastes [8]. The suitable pore sizes for bone and cartilage regeneration may be 300–800 and 50–125 μm suggested in the previous report [34]. Although the pore size in the D layer was smaller than the suggested size, the Gtn-CS hydrogel showed well subchondral bone regeneration in the in vivo experiment. Therefore, it may be suggested that the multi-layered Gtn-CS hydrogel prepared in this study benefit the cell adhesion, migration and proliferation. And the graded decrease of the pore sizes from the superficial layer to deep layer demonstrated the similar properties to the natural cartilage and could facilitate the cartilage repair.
The water swollen network in a hydrogel provide a local microenvironment that can modulate cells through various chemical and mechanical signals [35]. It was reported that the swelling ratio was influenced by the crosslinking density, hydrogel composition and network structure [36, 37]. In this study, the swelling ratio of the Gtn-GMA hydrogel was also affected by the crosslinking density and the composition. The higher methacrylated Gtn-GMA with a more amount of double bond in the transitional layer than that in the superficial layer could make the transitional layer have higher crosslinking density and less swelling. The deep layer contained the most amount of the double bond in the highest methacrylation degree of Gtn-GMA and OV-POSS, so that it showed the largest crosslinking density and the lowest swelling ratio. In natural cartilage, the defined collagen network restricts swelling of the tissue, while the negatively charged proteoglycans and low tissue permeability help the tissue swell and retain water [38]. Water within the tissue is important as it bears a large portion of the applied stress under dynamic loading conditions. The water content in natural cartilage is about 70–80 %, and the hydrated polymer network of the hydrogel with high swelling ratio is similar to the native ECM of the cartilage and favorable for cartilage repair [10]. The swelling ratio usually decreases along with the crosslinking density of the network. And in the present study, the swelling ratios also showed the similar relation with the crosslinking density, and the variations from the superficial layer to the deep layer might benefit the cartilage regeneration.
The compressive modulus of cartilage varies with the depth from the articular surface [39]. The compression modulus of adult bovine cartilage ranges from 0.08 to 2.1 MPa from the superficial layer to the deep layer [40]. In our study, the mechanical properties of the different layers of the Gtn-CS hydrogel were improved by increasing the crosslinking density and adding OV-POSS, and both the compressive strength and compressive modulus of the samples demonstrated increase trends from the superficial layer to the deep layer (Fig. 5). From the morphology of all samples shown in Fig. 3, there are interconnected pores with different sizes in multi-layered Gtn-CS hydrogel. The pore sizes in the superficial layer are lager than those in the transition and deep layers. It was reported that the loose network in the hydrogel would result in a high brittleness [12]. In this study, the S sample with larger pores and looser network showed a low compressive modulus, while the distributed small and uniform pores in the T sample were attributed to the higher crosslinking density [41]. Furthermore, the higher crosslinking density and introduction of POSS resulted in the highest compress modulus in the deep hydrogel.
The photocrosslinking hydrogels prepared by modifying various polymers has been used for many tissue engineering studies. The photocrosslinked hydrogels are relatively stiff and stable, but the heterogeneous distribution of crosslinking linkages in photocrosslinked hydrogels results in concentrated stress around the dense crosslinks, causing the hydrogels to fail at low stress [42]. Typically, the compressive modulus of photocrosslinked hydrogels reaches up to a few hundreds of kPa, and the failure stresses are on the order of tens to hundreds of kPa [43, 44]. In this study, the compressive strength and modulus of the superficial layer of the Gtn-CS hydrogel were 165 ± 54 and 314 ± 31 kPa, respectively, lower that those of the transitional layer (565 ± 50 and 1,076 ± 164 kPa), suggesting the mechanical properties of the different layers increased with the crosslinking density. The compressive mechanical properties of the transitional layer were beyond MPa, higher than that of the typically photocrosslinked hydrogel. Hydrogel alone always lacks of adequate mechanical properties [4, 16]. Therefore, a major goal in the application of hydrogels for cartilage tissue engineering scaffold is to developing hydrogels with high mechanical strength. In this study, OV-POSS was added in the deep layer of the Gtn-CS hydrogel to enhance the mechanical strength, and the compressive strength and compressive modulus of the deep layer was 993 ± 108 and 2.174 ± 142 kPa, respectively. The results indicated that the addition of OV-POSS in the photocrosslinked Gtn-CS hydrogel was useful to improve the mechanical properties.
In order to further evaluate the biomechanical properties of the layered hydrogel under physiological loads, an optimized digital image correlation technique was applied to prove the depth-dependent strain of cartilage under sliding load [44]. The natural cartilage exhibited the decrease of the normal strain value along the depth [29]. And, the layered hydrogel prepared in our study also showed the similar phenomenon. Although there was still a gap between the compression modulus of the layered hydrogel and that of the natural cartilage, for example the adult bovine cartilage [39], the Gtn-CS hydrogel with graded transitions in mechanical properties could possibly mimic the natural cartilage environment.
In order to investigate the controlled release behavior of the layered Gtn-CS hydrogel, FD70S was used as a model and incorporated into the Gtn-CS hydrogel to simulate the bioactive substances release. It was assumed that the release behavior could be affected by the crosslinking density of hydrogels [45]. As shown in the release profile (Fig. 7), the increase of the crosslinking density from the S sample to the D sample could prolong the release of FD70S because the high crosslinking density in the deep layer limited the diffusion of FD70S out of the sample. After introduction of OV-POSS in the deep layer, the crosslinking density increased and the swelling ratio decreased. Therefore, a much slower release rate was obtained. This result was consistent with the previous report [45], because the increased extent of crosslinking leads to a rigid barrier for the substance. This study provided a fundamental study for delivery of TGF-β1 used in the research.
Cytotoxicity was one of the most important factors for the hydrogel. It was reported that most of hydrogels showed a level of cell viabilities about 80 % [46]. In comparison, the cell viabilities in the extracts from different layers of the Gtn-CS hydrogels prepared in this study were higher than 80 %, better than those of some previous photocrosslinked hydrogels [15, 43]. The result demonstrated that the different layers of the layered Gtn-CS hydrogel showed a slight effect on the cell viabilities. Gtn and CS are natural materials with good biocompatibility which have been widely used in hydrogels, and also they have partial structural similarities to glycosaminoglycans and protein in ECM [10, 26, 31]. Therefore, the layered Gtn-CS hydrogel in this study showed low cytotoxity. It was also important to evaluate the effect of OV-POSS on the cytotoxity of the hydrogel. And, from the results showed in Fig. 8, the OV-POSS exhibited a slight effect on the hydrogel cytotoxity. The cell viabilities of all the layers were higher than 80 %, demonstrating that the layered hydrogels was a promising material for tissue engineering.
It was reported that the elasticity of the material would direct stem cell differentiation, for example, elastic materials induce differentiation to the cartilage tissue, and stiff materials induce differentiation to the bone tissue [5]. Therefore, the increased compressive modulus of the layered Gtn-CS hydrogel from the superficial layer to the deep layer may regulate the cartilage and bone regeneration in different regions. Hydrogels prepared from Gtn and CS, which dramatically simulated ECM, could provide a favorable environment for chondrogenesis and osteogenesis [47, 48]. In our study, the H&E results indicated that the layered hydrogel could support the osteochondral defect repair compared with the blank defect group (Fig. 10). In addition, it was easy to distinguish the regenerated cartilage and bone tissue. This result could support that the advantage of this multilayered hydrogel for osteochondral defect repair. The multi-layered structures showed more advantages in osteochondral repair because the discrete changes in properties could mimic highly organized complex structures comprising multiple cell types and heterogeneous ECM [28]. In this research, the layered Gtn-CS hydrogel displayed better results of cartilage and subchondral bone regeneration at 2 months than the non-treated blank group. Growth factors could promote osteochondral tissue regeneration, for example, TGF-β1 could promote BMSC chondrogenic differentiation [49]. The outstanding osteochondral repair result using the layered hydrogel with TGF-β1 also demonstrated this positive effect (Fig. 10). The multi-layer hydrogel showed advantages in cartilage-bone defect repair, and the spatially controlled and localized delivery of TGF-β1 from the Gtn-CS hydrogel further promote the cartilage regeneration in the osteochondral defect.
5 Conclusions
The multilayer-layered Gtn-CS hydrogel with different compositions and properties in each layer was successfully prepared via photocrosslinking by changing the solution concentration and composition. The hydrogel showed well interconnectivity, and the pore size, swelling ratio as well as compressive mechanical properties exhibited a graded transition of from the superficial layer to the deep layer in the hydrogels. The lowest release behavior was found in the deep layer with higher crosslinking density. The three layers in the layered Gtn-CS hydrogel exhibited low cytotoxity in vitro and showed the good repair result for osteochondral defect in vivo, especially when the hydrogel loaded with TGF-β1. In conclusion, the layered Gtn-CS hydrogel prepared in this research combined different compositions and properties in different layers could be potentially used in osteochondral repair. However, the mechanism of bone regeneration based on POSS is unknown, and this study only focuses on the short-term effects of the use of layered hydrogel on osteochondral repair. Long-term studies should be further examined.
References
Nukavarapu SP, Dorcemus DL. Osteochondral tissue engineering: current strategies and challenges. Biotechnol Adv. 2013;31:706–21.
Chung C, Burdick JA. Engineering cartilage tissue. Adv Drug Deliv Rev. 2008;60:243–62.
Matsuda H, Kitamura N, Kurokawa T, Arakaki K, Gong JP, Kanaya F, Yasuda K. Influence of the gel thickness on in vivo hyaline cartilage regeneration induced by double-network gel implanted at the bottom of a large osteochondral defect: short-term results. BMC Musculoskelet Disord. 2013;14:50–9.
Pan Y, Shen Q, Pan C, Wang J. Compressive mechanical characteristics of multi-layered gradient hydroxyapatite reinforced poly (vinyl alcohol) gel biomaterial. J Mater Sci Technol. 2013;29:551–6.
Nguyen LH, Kudva AK, Guckert NL, Linse KD, Roy K. Unique biomaterial compositions direct bone marrow stem cells into specific chondrocytic phenotypes corresponding to the various zones of articular cartilage. Biomaterials. 2011;32:1327–38.
Kim IL, Mauck RL, Burdick JA. Hydrogel design for cartilage tissue engineering: a case study with hyaluronic acid. Biomaterials. 2011;32:8771–82.
Hollander AP, Dickinson SC, Kafienah W. Stem cells and cartilage development: complexities of a simple tissue. Stem Cells. 2010;28:1992–6.
Harley BA, Lynn AK, Wissner-Gross Z, Bonfield W, Yannas IV, Gibson LJ. Design of a multiphase osteochondral scaffold III: fabrication of layered scaffolds with continuous interfaces. J Biomed Mater Res A. 2010;92:1078–93.
Nguyen LH, Kudva AK, Saxena NS, Roy K. Engineering articular cartilage with spatially-varying matrix composition and mechanical properties from a single stem cell population using a multi-layered hydrogel. Biomaterials. 2011;32:6946–52.
Hu X, Ma L, Wang C, Gao C. Gelatin hydrogel prepared by photo-initiated polymerization and loaded with TGF-beta1 for cartilage tissue engineering. Macromol Biosci. 2009;9:1194–201.
Bian L, Hou C, Tous E, Rai R, Mauck RL, Burdick JA. The influence of hyaluronic acid hydrogel crosslinking density and macromolecular diffusivity on human MSC chondrogenesis and hypertrophy. Biomaterials. 2013;34:413–21.
Tang Y, Sun J, Fan H, Zhang X. An improved complex gel of modified gellan gum and carboxymethyl chitosan for chondrocytes encapsulation. Carbohyd Polym. 2012;88:46–53.
Klein TJ, Rizzi SC, Schrobback K, Reichert JC, Jeon JE, Crawford RW, Hutmacher DW. Long-term effects of hydrogel properties on human chondrocyte behavior. Soft Matter. 2010;6:5175–83.
Galois L, Hutasse S, Cortial D, Rousseau CF, Grossin L, Ronziere MC, Herbage D, Freyria A-M. Bovine chondrocyte behaviour in three-dimensional type I collagen gel in terms of gel contraction, proliferation and gene expression. Biomaterials. 2006;27:79–90.
Shin H, Olsen BD, Khademhosseini A. The mechanical properties and cytotoxicity of cell-laden double-network hydrogels based on photocrosslinkable gelatin and gellan gum biomacromolecules. Biomaterials. 2012;33:3143–52.
Stammen JA, Williams S, Ku DN, Guldberg RE. Mechanical properties of a novel PVA hydrogel in shear and unconfined compression. Biomaterials. 2001;22:799–806.
Wu G, Su B, Zhang W, Wang C. In vitro behaviors of hydroxyapatite reinforced polyvinyl alcohol hydrogel composite. Mater Chem Phys. 2008;107:364–9.
Wang J, Sutti A, Wang X, Lin T. Fast responsive and morphologically robust thermo-responsive hydrogel nanofibres from poly(N-isopropylacrylamide) and POSS crosslinker. Soft Matter. 2011;7:4364–9.
Renò F, Carniato F, Rizzi M, Marchese L, Laus M, Antonioli D. POSS/gelatin-polyglutamic acid hydrogel composites: preparation, biological and mechanical characterization. J Appl Polym Sci. 2013;129:699–706.
Wu J, Ge Q, Mather PT. PEG-POSS multiblock polyurethanes: synthesis, characterization and hydrogel formation. Macromolecules. 2010;43:7637–49.
Im GI, Lee JH. Repair of osteochondral defects with adipose stem cells and a dual growth factor-releasing scaffold in rabbits. J Biomed Mater Res B Appl Biomater. 2010;92:552–60.
Mohan N, Dormer NH, Caldwell KL, Key VH, Berkland CJ, Detamore MS. Continuous gradients of material composition and growth factors for effective regeneration of the osteochondral interface. Tissue Eng Part A. 2011;17:2845–55.
Sridhar BV, Doyle NR, Randolph MA, Anseth KS. Covalently tethered TGF-b1 with encapsulated chondrocytes in a PEG hydrogel system enhances extracellular matrix production. J Biomed Mater Res A Appl Biomater. 2014;102:4464–72.
Han FX, Zhou F, Yang XL, Zhao J, Zhao YH, Yuan XY. A pilot study of conically graded chitosan-gelatin hydrogel/PLGA scaffold with dual-delivery of TGF-β1 and BMP-2 for regeneration of cartilage-bone interface. J Biomed Mater Res B Appl Biomater. 2014. doi:10.1002/jbm.b.33314.
Pierce BF, Tronci G, Rossle M, Neffe AT, Jung F, Lendlein A. Photocrosslinked co-networks from glycidylmethacrylated gelatin and poly(ethylene glycol) methacrylates. Macromol Biosci. 2012;12:484–93.
Zhu Y, Gao C, Liu X, Shen J. Surface modification of polycaprolactone membrane via aminolysis and biomacromolecule immobilization for promoting cytocompatibility of human endothelial cells. Biomacromolecules. 2002;3:1312–9.
Poon YF, Zhu YB, Shen JY, Chan-Park MB, Ng SC. Cytocompatible hydrogels based on photocrosslinkable methacrylated O-carboxymethylchitosan with tunable charge: synthesis and characterization. Adv Funct Mater. 2007;17:2139–50.
Tang GW, Zhang H, Zhao YH, Li XR, Yuan XY, Wang M. Prolonged release from PLGA/HAp scaffolds containing drug-loaded PLGA/gelatin composite microspheres. J Mater Sci Mater Med. 2012;23:419–29.
Zhang CQ, Gao LL, Dong LM, Liu HY. Depth-dependent normal strain of articular cartilage under sliding load by the optimized digital image correlation technique. Mater Sci Eng C. 2012;32:2390–5.
Han FX, Zhang H, Zhao J, Zhao YH, Yuan XY. Diverse release behaviors of water-soluble bioactive substances from fibrous membranes prepared by emulsion and suspension electrospinning. J Biomater Sci Polym Ed. 2013;24:1244–59.
Han FX, Jia XL, Dai DD, Yang XL, Zhao J, Zhao YH, Yuan XY. Performance of a multilayered small-diameter vascular scaffold dual-loaded with VEGF and PDGF. Biomaterials. 2013;34:7302–13.
Zhou YL, Nie W, Zhao J, Yuan XY. Rapidly in situ forming adhesive hydrogel based on a PEG-maleimide modified polypeptide through Michael addition. J Mater Sci Mater Med. 2013;24:2277–86.
Xie X, Wang Y, Zhao C, Guo S, Liu S, Jia W, Tuan RS, Zhang C. Comparative evaluation of MSCs from bone marrow and adipose tissue seeded in PRP-derived scaffold for cartilage regeneration. Biomaterials. 2012;33:7008–18.
Keeney M, Pandit A. The osteochondral junction and its repair via bi-phasic tissue engineering scaffolds. Tissue Eng Part B. 2009;15:55–73.
Tibbitt MW, Anseth KS. Hydrogels as extracellular matrix mimics for 3D cell culture. Biotechnol Bioeng. 2009;103:655–63.
Durmaz S, Okay O. Acrylamide/2-acrylamido-2-methylpropane sulfonic acid sodium salt-based hydrogels: synthesis and characterization. Polymer. 2000;41:3693–704.
Liu Y, Chan-Park MB. Hydrogel based on interpenetrating polymer networks of dextran and gelatin for vascular tissue engineering. Biomaterials. 2009;30:196–207.
Elder BD, Athanasiou KA. Hydrostatic pressure in articular cartilage tissue engineering: from chondrocytes to tissue regeneration. Tissue Eng Part B Rev. 2009;15:43–53.
Nguyen QT, Hwang Y, Chen AC, Varghese S, Sah RL. Cartilage-like mechanical properties of poly (ethylene glycol)-diacrylate hydrogels. Biomaterials. 2012;33:6682–90.
Schinagl RM, Gurskis D, Chen AC, Sah RL. Depth-dependent confined compression modulus of full-thickness bovine articular cartilage. J Orthopaed Res. 1997;15:499–506.
Zhang L, Li K, Xiao W, Zheng L, Xiao Y, Fan H, Zhang X. Preparation of collagen-chondroitin sulfate-hyaluronic acid hybrid hydrogel scaffolds and cell compatibility in vitro. Carbohyd Polym. 2011;84:118–25.
Gong JP. Why are double network hydrogels so tough? Soft Matter. 2010;6:2583–90.
Burdick JA, Chung C, Jia X, Randolph MA, Langer R. Controlled degradation and mechanical behavior of photopolymerized hyaluronic acid networks. Biomacromolecules. 2005;6:386–91.
Gao LL, Zhang CQ, Yang YB, Shi JP, Jia YW. Depth-dependent strain fields of articular cartilage under rolling load by the optimized digital image correlation technique. Mater Sci Eng C Mater Biol Appl. 2013;33:2317–22.
Sivakumaran D, Maitland D, Oszustowicz T, Hoare T. Tuning drug release from smart microgel-hydrogel composites via cross-linking. J Colloid Interf Sci. 2013;392:422–30.
Li Q, Yang D, Ma G, Xu Q, Chen X, Lu F, Nie J. Synthesis and characterization of chitosan-based hydrogels. Int J Biol Macromol. 2009;44:121–7.
Gentile P, Chiono V, Carmagnola I, Hatton PV. An overview of poly(lactic-co-glycolic) acid (PLGA)-based biomaterials for bone tissue engineering. Int J Mol Sci. 2014;15:3640–59.
Pasqui D, Torricelli P, De Cagna M, Fini M, Barbucci R. Carboxymethyl cellulose-hydroxyapatite hybrid hydrogel as a composite material for bone tissue engineering applications. J Biomed Mater Res A. 2014;102:1568–79.
Iwakura T, Sakata R, Reddi AH. Induction of chondrogenesis and expression of superficial zone protein in synovial explants with TGF-beta1 and BMP-7. Tissue Eng Part A. 2013;19:2638–44.
Acknowledgments
This work was financially supported by the Natural Science Foundation of China (No. 51073117) and also by the Scientific Research Foundation of Graduate School of Tianjin University. The work of mechanical test was immensely aided by the team of Professor Chunqiu Zhang in Tianjin Key Laboratory for Control Theory & Applications in Complicated Industry Systems, School of Mechanical Engineering, Tianjin University of Technology, China.
Author information
Authors and Affiliations
Corresponding author
Additional information
Fengxuan Han and Xiaoling Yang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Han, F., Yang, X., Zhao, J. et al. Photocrosslinked layered gelatin-chitosan hydrogel with graded compositions for osteochondral defect repair. J Mater Sci: Mater Med 26, 160 (2015). https://doi.org/10.1007/s10856-015-5489-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10856-015-5489-0