Abstract
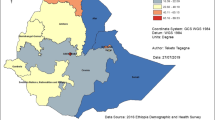
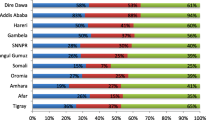
Understanding inequalities in spatial accessibility to prenatal care over space and time is critical for policymakers to plan a more effective distribution of health resources, improve access to prenatal care, and promote maternal and infant health. However, urban–rural inequalities in spatial accessibility to prenatal care have not been well studied. Using geographic information systems and the two-transportation-mode two-step floating catchment area method, we first assess and compare the spatial variation and urban–rural inequalities of spatial accessibility to prenatal care in Georgia for years 2000 and 2010. Then we designate census-tract-based prenatal care shortage areas that have both poor spatial accessibility and high demand population in each year. The results show that, for both years 2000 and 2010, spatial accessibility to prenatal care was best in urban core areas and decreased as rurality increases. However, the differences among suburban, urban influence, and rural areas were reduced over the decade. A total of eight census tracts, most located on the fringe of metropolitan Atlanta, had a prenatal care shortage in both years. According to the results, we suggest that spatial accessibility to prenatal care in non-urban-core areas in Georgia needs more attention from policymakers.





Similar content being viewed by others
References
Conway, K. S., & Kutinova, A. (2006). Maternal health: Does prenatal care make a difference? Health Economics, 15(5), 461–488.
Dai, D., & Wang, F. (2011). Geographic disparities in accessibility to food stores in southwest Mississippi. Environment and Planning B: Planning and Design, 38(4), 659–677.
Department of Health and Human Services. (1980). Criteria for designation of health manpower shortage areas: Final regulations. Federal Register, 45, 50436–50439.
Georgia Department of Public Health. (2018). OASIS: Online analytical statistical information system. https://oasis.state.ga.us/. Accessed April 29, 2018.
Georgia Secretary of State. (2017). Professional licensing search. http://verify.sos.ga.gov/verification/. Accessed June 1, 2017.
Goodchild, M. F., & Lam, N. S. (1980). Areal interpolation: A variant of the traditional spatial problem. Geo-Processing, 1, 297–312.
Gortmaker, S. L. (1979). The effects of prenatal care upon the health of the newborn. American Journal of Public Health, 69(7), 653–660.
Guagliardo, M. F. (2004). Spatial accessibility of primary care: Concepts, methods and challenges. International Journal of Health Geographics, 3(1), 3.
Health Resources and Services Administration. (2010). Primary care service area data 2010 (census tract basis). https://datawarehouse.hrsa.gov/data/dataDownload/pcsa2010download.aspx. Accessed March 1, 2016.
Health Resources and Services Administration. (2016). Health professional shortage areas (HPSAs). https://bhw.hrsa.gov/shortage-designation/hpsas. Accessed March 1, 2017.
Heaman, M. I., Moffatt, M., Elliott, L., Sword, W., Helewa, M. E., Morris, H., et al. (2014). Barriers, motivators and facilitators related to prenatal care utilization among inner-city women in Winnipeg, Canada: A case-control study. BMC Pregnancy and Childbirth, 14(1), 227.
Howell, A. J., & Timberlake, J. M. (2014). Racial and ethnic trends in the suburbanization of poverty in US metropolitan areas, 1980–2010. Journal of Urban Affairs, 36(1), 79–98.
Johnson, A. A., El-Khorazaty, M. N., Hatcher, B. J., Wingrove, B. K., Milligan, R., Harris, C., et al. (2003). Determinants of late prenatal care initiation by African American women in Washington, DC. Maternal and Child Health Journal, 7(2), 103–114.
Kogan, M. D., Alexander, G. R., Kotelchuck, M., & Nagey, D. A. (1994). Relation of the content of prenatal care to the risk of low birth weight: Maternal reports of health behavior advice and initial prenatal care procedures. JAMA, 271(17), 1340–1345.
Krueger, P. M., & Scholl, T. O. (2000). Adequacy of prenatal care and pregnancy outcome. The Journal of the American Osteopathic Association, 100(8), 485–492.
Li, R., & Tong, D. (2017). Incorporating activity space and trip chaining into facility siting for accessibility maximization. Socio-Economic Planning Sciences, 60, 1–14.
Luo, W., & Qi, Y. (2009). An enhanced two-step floating catchment area (E2SFCA) method for measuring spatial accessibility to primary care physicians. Health & Place, 15(4), 1100–1107.
Luo, W., & Wang, F. (2003). Measures of spatial accessibility to health care in a GIS environment: Synthesis and a case study in the Chicago region. Environment and Planning B, 30(6), 865–884.
Mao, L., & Nekorchuk, D. (2013). Measuring spatial accessibility to healthcare for populations with multiple transportation modes. Health & Place, 24, 115–122.
Martin, J. A., Hamilton, B. E., Sutton, P. D., Ventura, S. J., Mathews, T. J., Kirmeyer, S., & Osterman, M. J .K. (2010). Births: Final data for 2007. In National vital statistics reports (Vol. 58, No. 24). National Center for Health Statistics, Centers for Disease Control and Prevention.
McLafferty, S., & Grady, S. (2004). Prenatal care need and access: A GIS analysis. Journal of Medical Systems, 28(3), 321–333.
Mieszkowski, P., & Mills, E. S. (1993). The causes of metropolitan suburbanization. The Journal of Economic Perspectives, 7(3), 135–147.
Miller, H. J. (2005). Place-based versus people-based accessibility. In D. M. Levinson & K. J. Krizek (Eds.), Access to destinations (pp. 63–89). Emerald Group Publishing Limited.
Niedzielski, M. A., & Eric Boschmann, E. (2014). Travel time and distance as relative accessibility in the journey to work. Annals of the Association of American Geographers, 104(6), 1156–1182.
Pebley, A. R., Goldman, N., & Rodriguez, G. (1996). Prenatal and delivery care and childhood immunization in Guatemala: Do family and community matter? Demography, 33(2), 231–247.
Pilkington, H., Blondel, B., Drewniak, N., & Zeitlin, J. (2012). Choice in maternity care: Associations with unit supply, geographic accessibility and user characteristics. International Journal of Health Geographics, 11(1), 35.
Shoff, C., Yang, T.-C., & Matthews, S. A. (2012). What has geography got to do with it? Using GWR to explore place-specific associations with prenatal care utilization. GeoJournal, 77(3), 331–341. https://doi.org/10.1007/s10708-010-9405-3.
Spelke, B., Zertuche, A. D., & Rochat, R. (2016). Obstetric provider maldistribution: Georgia, USA, 2011. Maternal and Child Health Journal, 20(7), 1333–1340.
Tong, D., Lin, W.-H., Mack, J., & Mueller, D. (2010). Accessibility-based multicriteria analysis for facility siting. Transportation Research Record: Journal of the Transportation Research Board, 2174, 128–137.
United States Department of Agriculture. (2016). Rural–urban commuting area codes (RUCA). https://www.ers.usda.gov/data-products/rural-urban-commuting-area-codes/. Accessed June 6, 2017.
Wan, N., Zou, B., & Sternberg, T. (2012). A three-step floating catchment area method for analyzing spatial access to health services. International Journal of Geographical Information Science, 26(6), 1073–1089.
Wang, F. (2012). Measurement, optimization, and impact of health care accessibility: A methodological review. Annals of the Association of American Geographers, 102(5), 1104–1112.
Wang, L. (2011). Analysing spatial accessibility to health care: A case study of access by different immigrant groups to primary care physicians in Toronto. Annals of GIS, 17(4), 237–251.
Wang, F., & Luo, W. (2005). Assessing spatial and nonspatial factors for healthcare access: Towards an integrated approach to defining health professional shortage areas. Health & Place, 11(2), 131–146.
Wang, F., McLafferty, S., Escamilla, V., & Luo, L. (2008). Late-stage breast cancer diagnosis and health care access in Illinois. The Professional Geographer, 60(1), 54–69.
Wang, F., & Tang, Q. (2013). Planning toward equal accessibility to services: A quadratic programming approach. Environment and Planning B: Planning and Design, 40(2), 195–212.
Weissman, J. S., Stern, R., Fielding, S. L., & Epstein, A. M. (1991). Delayed access to health care: Risk factors, reasons, and consequences. Annals of Internal Medicine, 114(4), 325–331.
WHO. (2008). Primary health care (now more than ever). The World Health Report 2008.
WHO. (2016). Pregnant women must be able to access the right care at the right time, says WHO. http://www.who.int/mediacentre/news/releases/2016/antenatal-care-guidelines/en/. Accessed March 18, 2017.
Williams, S., & Wang, F. (2014). Disparities in accessibility of public high schools, in metropolitan Baton Rouge, Louisiana 1990–2010. Urban Geography, 35(7), 1066–1083.
Yin, P. (2017). Does better spatial access lead to better utilization of prenatal care? A population study in Georgia. The Professional Geographer. https://doi.org/10.1080/00330124.2017.1385402.
Yoon, S., Li, H., Jun, J., Ogle, J., Guensler, R., & Rodgers, M. (2005). Methodology for developing transit bus speed-acceleration matrices for load-based mobile source emissions models. Transportation Research Record: Journal of the Transportation Research Board, 1941, 26–33.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yin, P. Urban–rural inequalities in spatial accessibility to prenatal care: a GIS analysis of Georgia, USA, 2000–2010. GeoJournal 84, 671–683 (2019). https://doi.org/10.1007/s10708-018-9884-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10708-018-9884-1