Abstract
Exposure to environmental and occupational contaminants leads to lung cancer. 3-Nitrobenzanthrone (3-nitro-7H-benz[de]anthracen-7-one, 3-NBA) is a potential carcinogen in ambient air or diesel particulate matter. Studies have revealed that short-term exposure to 3-NBA induces cell death, reactive oxygen species activation, and DNA adduct formation and damage. However, details of the mechanism by which chronic exposure to 3-NBA influences lung carcinogenesis remain largely unknown. In this study, human lung epithelial BEAS-2B cells were continuously exposed to 0–10-μM 3-NBA for 6 months. NanoString analysis was conducted to evaluate gene expression in the cells, revealing that 3-NBA–mediated transformation results in a distinct gene expression signature including carbon cancer metabolism, metastasis, and angiogenesis. Alterations in tumor-promoting genes such as EREG (epiregulin), SOX9, E-cadherin, TWIST, and IL-6 were involved in epithelial cell aggressiveness. Kaplan–Meier plotter analyses indicated that increased EREG and IL-6 expressions in early-stage lung cancer cells are correlated with poor survival. In vivo xenografts on 3-NBA–transformed cells exhibited prominent tumor formation and metastasis. EREG knockout cells exposed to 3-NBA for a short period exhibited high apoptosis and low colony formation. By contrast, overexpression of EREG in 3-NBA–transformed cells markedly activated the PI3K/AKT and MEK/ERK signaling pathways, resulting in tumorigenicity. Furthermore, elevated IL-6 and EREG expressions synergistically led to STAT3 signaling activation, resulting in clonogenic cell survival and migration. Taken together, chronic exposure of human lung epithelial cells to 3-NBA leads to malignant transformation, in which the EREG signaling pathway plays a pivotal mediating role.
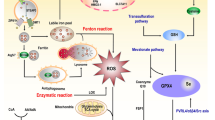
Graphical abstract

• Short-term exposure of lung epithelial cells to 3-NBA can lead to ROS production and cell apoptosis.
• Long-term chronic exposure to 3-NBA upregulates the levels of tumor-promoting genes such as EREG and IL-6.
• Increased EREG expression in 3-NBA–transformed cells markedly contributes to tumorigenesis through PI3K/AKT and MEK/ERK activation and synergistically enhances the IL-6/STAT3 signaling pathway, which promotes tumorigenicity.








Similar content being viewed by others
References
Arlt VM. 3-Nitrobenzanthrone, a potential human cancer hazard in diesel exhaust and urban air pollution: a review of the evidence. Mutagenesis. 2005;20(6):399–410. https://doi.org/10.1093/mutage/gei057.
Arlt VM, Bieler CA, Mier W, Wiessler M, Schmeiser HH. DNA adduct formation by the ubiquitous environmental contaminant 3-nitrobenzanthrone in rats determined by (32)P-postlabeling. Int J Cancer. 2001;93(3):450–4.
Arlt VM, Gingerich J, Schmeiser HH, Phillips DH, Douglas GR, White PA. Genotoxicity of 3-nitrobenzanthrone and 3-aminobenzanthrone in MutaMouse and lung epithelial cells derived from MutaMouse. Mutagenesis. 2008;23(6):483–90. https://doi.org/10.1093/mutage/gen037.
Arlt VM, Stiborova M, Henderson CJ, Osborne MR, Bieler CA, Frei E, et al. Environmental pollutant and potent mutagen 3-nitrobenzanthrone forms DNA adducts after reduction by NAD(P)H:quinone oxidoreductase and conjugation by acetyltransferases and sulfotransferases in human hepatic cytosols. Cancer Res. 2005;65(7):2644–52. https://doi.org/10.1158/0008-5472.CAN-04-3544.
Bauer AK, Velmurugan K, Xiong KN, Alexander CM, Xiong J, Brooks R. Epiregulin is required for lung tumor promotion in a murine two-stage carcinogenesis model. Mol Carcinog. 2017;56(1):94–105. https://doi.org/10.1002/mc.22475.
Bieler CA, Cornelius MG, Stiborova M, Arlt VM, Wiessler M, Phillips DH, et al. Formation and persistence of DNA adducts formed by the carcinogenic air pollutant 3-nitrobenzanthrone in target and non-target organs after intratracheal instillation in rats. Carcinogenesis. 2007;28(5):1117–21. https://doi.org/10.1093/carcin/bgl219.
Casal-Mourino A, Valdes L, Barros-Dios JM, Ruano-Ravina A. Lung cancer survival among never smokers. Cancer Lett. 2019;451:142–9. https://doi.org/10.1016/j.canlet.2019.02.047.
Cervena T, Vrbova K, Rossnerova A, Topinka J, Rossner P Jr. Short-term and long-term exposure of the MucilAir model to polycyclic aromatic hydrocarbons. Altern Lab Anim. 2019;47(1):9–18. https://doi.org/10.1177/0261192919841484.
Chen S, Schoen J. Air-liquid interface cell culture: from airway epithelium to the female reproductive tract. Reprod Domest Anim. 2019;54(Suppl 3):38–45. https://doi.org/10.1111/rda.13481.
Courcot E, Leclerc J, Lafitte JJ, Mensier E, Jaillard S, Gosset P, et al. Xenobiotic metabolism and disposition in human lung cell models: comparison with in vivo expression profiles. Drug Metab Dispos. 2012;40(10):1953–65. https://doi.org/10.1124/dmd.112.046896.
Cox AD, Der CJ. Biological assays for cellular transformation. Methods Enzymol. 1994;238:277–94. https://doi.org/10.1016/0076-6879(94)38026-0.
Eckel SP, Cockburn M, Shu YH, Deng H, Lurmann FW, Liu L, et al. Air pollution affects lung cancer survival. Thorax. 2016;71(10):891–8. https://doi.org/10.1136/thoraxjnl-2015-207927.
Field RW, Withers BL. Occupational and environmental causes of lung cancer. Clin Chest Med. 2012;33(4):681–703. https://doi.org/10.1016/j.ccm.2012.07.001.
Fischer PH, Marra M, Ameling CB, Hoek G, Beelen R, de Hoogh K, et al. Air pollution and mortality in seven million adults: the Dutch Environmental Longitudinal Study (DUELS). Environ Health Perspect. 2015;123(7):697–704. https://doi.org/10.1289/ehp.1408254.
Fisher DT, Appenheimer MM, Evans SS. The two faces of IL-6 in the tumor microenvironment. Semin Immunol. 2014;26(1):38–47. https://doi.org/10.1016/j.smim.2014.01.008.
Gibbons DL, Byers LA, Kurie JM. Smoking, p53 mutation, and lung cancer. Mol Cancer Res. 2014;12(1):3–13. https://doi.org/10.1158/1541-7786.MCR-13-0539.
Grimmer G, Brune H, Deutsch-Wenzel R, Dettbarn G, Jacob J, Naujack KW, et al. Contribution of polycyclic aromatic hydrocarbons and nitro-derivatives to the carcinogenic impact of diesel engine exhaust condensate evaluated by implantation into the lungs of rats. Cancer Lett. 1987;37(2):173–80. https://doi.org/10.1016/0304-3835(87)90160-1.
Gyorffy B, Surowiak P, Budczies J, Lanczky A. Online survival analysis software to assess the prognostic value of biomarkers using transcriptomic data in non-small-cell lung cancer. PLoS One. 2013;8(12):e82241. https://doi.org/10.1371/journal.pone.0082241.
Hamra GB, Guha N, Cohen A, Laden F, Raaschou-Nielsen O, Samet JM, et al. Outdoor particulate matter exposure and lung cancer: a systematic review and meta-analysis. Environ Health Perspect. 2014;122(9):906–11. https://doi.org/10.1289/ehp.1408092201289/ehp/1408092.
Han X, Na T, Wu T, Yuan BZ. Human lung epithelial BEAS-2B cells exhibit characteristics of mesenchymal stem cells. PLoS One. 2020;15(1):e0227174. https://doi.org/10.1371/journal.pone.0227174.
Hansen T, Seidel A, Borlak J. The environmental carcinogen 3-nitrobenzanthrone and its main metabolite 3-aminobenzanthrone enhance formation of reactive oxygen intermediates in human A549 lung epithelial cells. Toxicol Appl Pharmacol. 2007;221(2):222–34. https://doi.org/10.1016/j.taap.2007.03.003.
He RW, Braakhuis HM, Vandebriel RJ, Staal YCM, Gremmer ER, Fokkens PHB, et al. Optimization of an air-liquid interface in vitro cell co-culture model to estimate the hazard of aerosol exposures. J Aerosol Sci. 2021;153:105703. https://doi.org/10.1016/j.jaerosci.2020.105703.
Jing B, Wang T, Sun B, Xu J, Xu D, Liao Y, et al. IL6/STAT3 signaling orchestrates premetastatic niche formation and immunosuppressive traits in lung. Cancer Res. 2020;80(4):784–97. https://doi.org/10.1158/0008-5472.CAN-19-2013.
Kamitani S, Yamauchi Y, Kawasaki S, Takami K, Takizawa H, Nagase T, et al. Simultaneous stimulation with TGF-beta1 and TNF-alpha induces epithelial mesenchymal transition in bronchial epithelial cells. Int Arch Allergy Immunol. 2011;155(2):119–28. https://doi.org/10.1159/000318854.
Kida H, Yoshida M, Hoshino S, Inoue K, Yano Y, Yanagita M, et al. Protective effect of IL-6 on alveolar epithelial cell death induced by hydrogen peroxide. Am J Phys Lung Cell Mol Phys. 2005;288(2):L342–9. https://doi.org/10.1152/ajplung.00016.2004.
Kim BG, Lee PH, Lee SH, Kim YE, Shin MY, Kang Y, et al. Long-term effects of diesel exhaust particles on airway inflammation and remodeling in a mouse model. Allergy, Asthma Immunol Res. 2016;8(3):246–56. https://doi.org/10.4168/aair.2016.8.3.246.
Kobayashi S, Yamada-Okabe H, Suzuki M, Natori O, Kato A, Matsubara K, et al. LGR5-positive colon cancer stem cells interconvert with drug-resistant LGR5-negative cells and are capable of tumor reconstitution. Stem Cells. 2012;30(12):2631–44. https://doi.org/10.1002/stem.1257.
Kunitake E, Shimamura K, Katayama H, Takemoto K, Yamamoto A, Hisanaga A, et al. Studies concerning carcinogenesis of diesel particulate extracts following intratracheal instillation, subcutaneous injection, or skin application. Dev Toxicol Environ Sci. 1986;13:235–52.
Levine AJ, Puzio-Kuter AM, Chan CS, Hainaut P. The role of the p53 protein in stem-cell biology and epigenetic regulation. Cold Spring Harb Perspect Med. 2016;6(9). https://doi.org/10.1101/cshperspect.a026153.
Li J, Lan T, Zhang C, Zeng C, Hou J, Yang Z, et al. Reciprocal activation between IL-6/STAT3 and NOX4/Akt signalings promotes proliferation and survival of non-small cell lung cancer cells. Oncotarget. 2015;6(2):1031–48. https://doi.org/10.18632/oncotarget.2671.
Libalova H, Milcova A, Cervena T, Vrbova K, Rossnerova A, Novakova Z, et al. Kinetics of ROS generation induced by polycyclic aromatic hydrocarbons and organic extracts from ambient air particulate matter in model human lung cell lines. Mutat Res Genet Toxicol Environ Mutagen. 2018;827:50–8. https://doi.org/10.1016/j.mrgentox.2018.01.006.
Lindvall C, Hou M, Komurasaki T, Zheng C, Henriksson M, Sedivy JM, et al. Molecular characterization of human telomerase reverse transcriptase-immortalized human fibroblasts by gene expression profiling: activation of the epiregulin gene. Cancer Res. 2003;63(8):1743–7.
Liu S, Wang Y, Han Y, Xia W, Zhang L, Xu S, et al. EREG-driven oncogenesis of head and neck squamous cell carcinoma exhibits higher sensitivity to erlotinib therapy. Theranostics. 2020;10(23):10589–605. https://doi.org/10.7150/thno.47176.
Liu S, Ye D, Xu D, Liao Y, Zhang L, Liu L, et al. Autocrine epiregulin activates EGFR pathway for lung metastasis via EMT in salivary adenoid cystic carcinoma. Oncotarget. 2016;7(18):25251–63. https://doi.org/10.18632/oncotarget.7940.
Liu XL, Zhang XT, Meng J, Zhang HF, Zhao Y, Li C, et al. ING5 knockdown enhances migration and invasion of lung cancer cells by inducing EMT via EGFR/PI3K/Akt and IL-6/STAT3 signaling pathways. Oncotarget. 2017;8(33):54265–76. https://doi.org/10.18632/oncotarget.17346.
Long AS, Lemieux CL, Arlt VM, White PA. Tissue-specific in vivo genetic toxicity of nine polycyclic aromatic hydrocarbons assessed using the MutaMouse transgenic rodent assay. Toxicol Appl Pharmacol. 2016;290:31–42. https://doi.org/10.1016/j.taap.2015.11.010.
Luanpitpong S, Wang L, Castranova V, Rojanasakul Y. Induction of stem-like cells with malignant properties by chronic exposure of human lung epithelial cells to single-walled carbon nanotubes. Part Fibre Toxicol. 2014;11:22. https://doi.org/10.1186/1743-8977-11-22.
Malm SW, Amouzougan EA, Klimecki WT. Fetal bovine serum induces sustained, but reversible, epithelial-mesenchymal transition in the BEAS-2B cell line. Toxicol in Vitro. 2018;50:383–90. https://doi.org/10.1016/j.tiv.2018.04.008.
Matheu A, Collado M, Wise C, Manterola L, Cekaite L, Tye AJ, et al. Oncogenicity of the developmental transcription factor Sox9. Cancer Res. 2012;72(5):1301–15. https://doi.org/10.1158/0008-5472.CAN-11-3660.
Nagy E, Adachi S, Takamura-Enya T, Zeisig M, Moller L. DNA damage and acute toxicity caused by the urban air pollutant 3-nitrobenzanthrone in rats: characterization of DNA adducts in eight different tissues and organs with synthesized standards. Environ Mol Mutagen. 2006;47(7):541–52. https://doi.org/10.1002/em.20227.
Nagy E, Adachi S, Takamura-Enya T, Zeisig M, Moller L. DNA adduct formation and oxidative stress from the carcinogenic urban air pollutant 3-nitrobenzanthrone and its isomer 2-nitrobenzanthrone, in vitro and in vivo. Mutagenesis. 2007;22(2):135–45. https://doi.org/10.1093/mutage/gel067.
Nagy E, Zeisig M, Kawamura K, Hisamatsu Y, Sugeta A, Adachi S, et al. DNA adduct and tumor formations in rats after intratracheal administration of the urban air pollutant 3-nitrobenzanthrone. Carcinogenesis. 2005;26(10):1821–8. https://doi.org/10.1093/carcin/bgi141.
Olsson AC, Gustavsson P, Kromhout H, Peters S, Vermeulen R, Bruske I, et al. Exposure to diesel motor exhaust and lung cancer risk in a pooled analysis from case-control studies in Europe and Canada. Am J Respir Crit Care Med. 2011;183(7):941–8. https://doi.org/10.1164/rccm.201006-0940OC.
Oya E, Ovrevik J, Arlt VM, Nagy E, Phillips DH, Holme JA. DNA damage and DNA damage response in human bronchial epithelial BEAS-2B cells following exposure to 2-nitrobenzanthrone and 3-nitrobenzanthrone: role in apoptosis. Mutagenesis. 2011;26(6):697–708. https://doi.org/10.1093/mutage/ger035.
Phi KK, Smith MC, Tokarsky EJ, Suo Z. Kinetic investigation of translesion synthesis across a 3-nitrobenzanthrone-derived DNA lesion catalyzed by human DNA polymerase kappa. Chem Res Toxicol. 2019;32(8):1699–706. https://doi.org/10.1021/acs.chemrestox.9b00219.
Pink M, Verma N, Zerries A, Schmitz-Spanke S. Dose-dependent response to 3-nitrobenzanthrone exposure in human urothelial cancer cells. Chem Res Toxicol. 2017;30(10):1855–64. https://doi.org/10.1021/acs.chemrestox.7b00174.
Qu X, Sandmann T, Frierson H Jr, Fu L, Fuentes E, Walter K, et al. Integrated genomic analysis of colorectal cancer progression reveals activation of EGFR through demethylation of the EREG promoter. Oncogene. 2016;35(50):6403–15. https://doi.org/10.1038/onc.2016.170.
Santos AG, da Rocha GO, de Andrade JB. Occurrence of the potent mutagens 2-nitrobenzanthrone and 3-nitrobenzanthrone in fine airborne particles. Sci Rep. 2019;9(1):1. https://doi.org/10.1038/s41598-018-37186-2.
Scheller J, Chalaris A, Schmidt-Arras D, Rose-John S. The pro- and anti-inflammatory properties of the cytokine interleukin-6. Biochim Biophys Acta. 2011;1813(5):878–88. https://doi.org/10.1016/j.bbamcr.2011.01.034.
Seidel A, Dahmann D, Krekeler H, Jacob J. Biomonitoring of polycyclic aromatic compounds in the urine of mining workers occupationally exposed to diesel exhaust. Int J Hyg Environ Health. 2002;204(5-6):333–8. https://doi.org/10.1078/1438-4639-00116.
Shelly M, Pinkas-Kramarski R, Guarino BC, Waterman H, Wang LM, Lyass L, et al. Epiregulin is a potent pan-ErbB ligand that preferentially activates heterodimeric receptor complexes. J Biol Chem. 1998;273(17):10496–505. https://doi.org/10.1074/jbc.273.17.10496.
Silva EM, Mariano VS, Pastrez PRA, Pinto MC, Castro AG, Syrjanen KJ, et al. High systemic IL-6 is associated with worse prognosis in patients with non-small cell lung cancer. PLoS One. 2017;12(7):e0181125. https://doi.org/10.1371/journal.pone.0181125.
Steinberg P. In vitro-in vivo carcinogenicity. Adv Biochem Eng Biotechnol. 2017;157:81–96. https://doi.org/10.1007/10_2015_5013.
Steiner S, Bisig C, Petri-Fink A, Rothen-Rutishauser B. Diesel exhaust: current knowledge of adverse effects and underlying cellular mechanisms. Arch Toxicol. 2016;90(7):1541–53. https://doi.org/10.1007/s00204-016-1736-5.
Stiborova M, Cechova T, Borek-Dohalska L, Moserova M, Frei E, Schmeiser HH, et al. Activation and detoxification metabolism of urban air pollutants 2-nitrobenzanthrone and carcinogenic 3-nitrobenzanthrone by rat and mouse hepatic microsomes. Neuro Endocrinol Lett. 2012;33(Suppl 3):8–15.
Stiborova M, Martinek V, Svobodova M, Sistkova J, Dvorak Z, Ulrichova J, et al. Mechanisms of the different DNA adduct forming potentials of the urban air pollutants 2-nitrobenzanthrone and carcinogenic 3-nitrobenzanthrone. Chem Res Toxicol. 2010;23(7):1192–201. https://doi.org/10.1021/tx100052d.
Sun S, Schiller JH, Gazdar AF. Lung cancer in never smokers--a different disease. Nat Rev Cancer. 2007;7(10):778–90. https://doi.org/10.1038/nrc2190.
Sunaga N, Kaira K. Epiregulin as a therapeutic target in non-small-cell lung cancer. Lung Cancer (Auckl). 2015;6:91–8. https://doi.org/10.2147/LCTT.S60427.
Sunaga N, Kaira K, Imai H, Shimizu K, Nakano T, Shames DS, et al. Oncogenic KRAS-induced epiregulin overexpression contributes to aggressive phenotype and is a promising therapeutic target in non-small-cell lung cancer. Oncogene. 2013;32(34):4034–42. https://doi.org/10.1038/onc.2012.402.
Szklarczyk D, Morris JH, Cook H, Kuhn M, Wyder S, Simonovic M, et al. The STRING database in 2017: quality-controlled protein-protein association networks, made broadly accessible. Nucleic Acids Res. 2017;45(D1):D362–8. https://doi.org/10.1093/nar/gkw937.
Takamura-Enya T, Kawanishi M, Yagi T, Hisamatsu Y. Structural identification of DNA adducts derived from 3-nitrobenzanthrone, a potent carcinogen present in the atmosphere. Chem Asian J. 2007;2(9):1174–85. https://doi.org/10.1002/asia.200700061.
Veldman-Jones MH, Brant R, Rooney C, Geh C, Emery H, Harbron CG, et al. Evaluating robustness and sensitivity of the NanoString Technologies nCounter Platform to enable multiplexed gene expression analysis of clinical samples. Cancer Res. 2015;75(13):2587–93. https://doi.org/10.1158/0008-5472.CAN-15-0262.
Vermeer PD, Panko L, Karp P, Lee JH, Zabner J. Differentiation of human airway epithelia is dependent on erbB2. Am J Phys Lung Cell Mol Phys. 2006;291(2):L175–80. https://doi.org/10.1152/ajplung.00547.2005.
Voronkova MA, Luanpitpong S, Rojanasakul LW, Castranova V, Dinu CZ, Riedel H, et al. SOX9 regulates cancer stem-like properties and metastatic potential of single-walled carbon nanotube-exposed cells. Sci Rep. 2017;7(1):11653. https://doi.org/10.1038/s41598-017-12037-8.
Wang X, Wang Y, Xiao G, Wang J, Zu L, Hao M, et al. Hypermethylated in cancer 1(HIC1) suppresses non-small cell lung cancer progression by targeting interleukin-6/Stat3 pathway. Oncotarget. 2016;7(21):30350–64. https://doi.org/10.18632/oncotarget.8734.
Wang Y, Jing Y, Ding L, Zhang X, Song Y, Chen S, et al. Epiregulin reprograms cancer-associated fibroblasts and facilitates oral squamous cell carcinoma invasion via JAK2-STAT3 pathway. J Exp Clin Cancer Res. 2019;38(1):274. https://doi.org/10.1186/s13046-019-1277-x.
White PA, Douglas GR, Phillips DH, Arlt VM. Quantitative relationships between lacZ mutant frequency and DNA adduct frequency in MutaMouse tissues and cultured cells exposed to 3-nitrobenzanthrone. Mutagenesis. 2017;32(2):299–312. https://doi.org/10.1093/mutage/gew067.
Wu SM, Lin SL, Lee KY, Chuang HC, Feng PH, Cheng WL, et al. Hepatoma cell functions modulated by NEK2 are associated with liver cancer progression. Int J Cancer. 2017;140(7):1581–96. https://doi.org/10.1002/ijc.30559.
Yang L, Shi P, Zhao G, Xu J, Peng W, Zhang J, et al. Targeting cancer stem cell pathways for cancer therapy. Signal Transduct Target Ther. 2020;5(1):8. https://doi.org/10.1038/s41392-020-0110-5.
Zhang J, Iwanaga K, Choi KC, Wislez M, Raso MG, Wei W, et al. Intratumoral epiregulin is a marker of advanced disease in non-small cell lung cancer patients and confers invasive properties on EGFR-mutant cells. Cancer Prev Res (Phila). 2008;1(3):201–7. https://doi.org/10.1158/1940-6207.CAPR-08-0014.
Zhou CH, Ye LP, Ye SX, Li Y, Zhang XY, Xu XY, et al. Clinical significance of SOX9 in human non-small cell lung cancer progression and overall patient survival. J Exp Clin Cancer Res. 2012;31:18. https://doi.org/10.1186/1756-9966-31-18.
Acknowledgements
We thank the CRISPR Gene Targeting Core Lab at Taipei Medical University for providing technical support. This manuscript was edited by Wallace Academic Editing.
Availability of data and material
The datasets used or analyzed are available from the corresponding author upon reasonable request.
Code availability
Deregulated KEGG pathways were identified using STRING software (http://string-db.org). Differential genes were analyzed (www.kmplot.com) using Kaplan–Meier plotter with published lung cancer microarray datasets.
Funding
This work was supported by grants from the Ministry of Science and Technology of the Republic of China (MOST: 108-2314-B-038-111-MY3 and 108-2314-B-038-063-MY3), Ministry of Education of the Republic of China (DP2-109-21121-01-T-01), Taipei Medical University and Shuang Ho Hospital (109TMU-SHH-09), Taipei Medical University (TMU107-AE1-B04), and Shuang Ho Hospital (108-FRP-04 and 109-FRP-03).
Author information
Authors and Affiliations
Contributions
KYC and CHT designed the study and wrote the manuscript. PHF and WLS drafted the manuscript and interpreted the data. SCH, CWL, NVH, CSL, and WTL collected the primary data and prepared the figures. TTC and YHT contributed to the literature review and performed statistical analysis. KYL and SMW supervised and reviewed the entire project and manuscript preparation. All authors have read and approved the manuscript.
Ethics declarations
Ethics approval
All protocols for animal experiments were approved by the Taipei Medical University Institutional Animal Care and Use Committee.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflicts of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 3717 kb)
Rights and permissions
About this article
Cite this article
Chen, KY., Tseng, CH., Feng, PH. et al. 3-Nitrobenzanthrone promotes malignant transformation in human lung epithelial cells through the epiregulin-signaling pathway. Cell Biol Toxicol 38, 865–887 (2022). https://doi.org/10.1007/s10565-021-09612-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10565-021-09612-1