Summary
Purpose: Both ATV and SL reduce myocardial infarct size (IS) by enhancing expression and activity of NOS isoforms. We investigated whether atorvastatin (ATV) and sildenafil (SL) have synergistic effects on myocardial infarct size (IS) reduction and enhancing nitric oxide synthase (NOS) expression.
Method: Rats were randomized to nine groups: ATV-1 (1 mg/kg/d); ATV-10 (10 mg/kg/d); SL-0.7 (0.7 mg/kg); SL-1 (1 mg/kg); ATV-1 + SL-0.7; water alone (controls); 1400W (iNOS inhibitor; 1 mg/kg); ATV-10 + 1400W; and ATV-1 + SL-0.7 + 1400W. ATV was administered orally for 3 days. SL was administered intraperitoneally 18 h before surgery and 1400W intravenously 15 min before surgery. Rats either underwent 30 min ischemia-4 h reperfusion or the hearts were explanted for immunoblotting and enzyme activity tests without being exposed to ischemia.
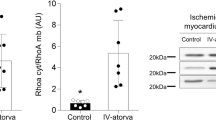
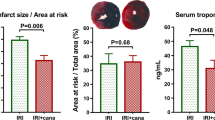
Results: IS (% risk area, mean ± SEM) was smaller in the ATV-10 (13 ± 1%), SL-1 (11 ± 2%), SL-0.7 (18 ± 2%) and ATV-1 + SL-0.7 (9 ± 1%) groups as compared with controls (34 ± 3%; P < 0.001), whereas ATV-1 had no effect (29 ± 2%). ATV-1 + SL-0.7 (9 ± 1%) reduced IS more than SL-0.7 alone (p = 0.012). 1400W abrogated the protective effect of ATV-10 (35 ± 3%) and ATV-1 + SL-0.7 (34 ± 1%). SL-0.7 and ATV-10 increased phosphorylated endothelial (P-eNOS; 210 ± 2.5% and 220 ± 8%) and inducible (iNOS; 151 ± 1% and 154 ± 1%) NOS expression, whereas ATV-1 did not. These changes were significantly enhanced by ATV-1 + SL-0.7 (P-eNOS, 256 ± 2%, iNOS 195 ± 1%). SL-1 increased P-eNOS (311 ± 22%) and iNOS (185 ± 1%) concentrations.
Conclusions: Combining low-dose ATV with SL augments the IS limiting effects through enhanced P-eNOS and iNOS expression.
Similar content being viewed by others
References
Murry CE, Jennings RB, Reimer KA. Preconditioning with ischemia: A delay in lethal cell injury in ischemic myocardium. Circulation 1986;74:1124–1136.
Schulz R, Cohen MV, Behrends M, Downey JM, Heusch G. Signal transduction of ischemic preconditioning. Cardiovasc Res 2001;52:181–198.
Sanada S, Kitakaze M. Ischemic preconditioning: Emerging evidence, controversy, and translational trials. Int J Cardiol 2004;97:263–276.
Bolli R, Dawn B, Tang XL, et al. The nitric oxide hypothesis of late preconditioning. Basic Res Cardiol 1998;93:325–338.
Bolli R, Dawn B, Xuan YT. Role of the JAK-STAT pathway in protection against myocardial ischemia/reperfusion injury. Trends Cardiovasc Med 2003;13:72–79.
Dotani MI, Elnicki DM, Jain AC, Gibson CM. Effect of preoperative statin therapy and cardiac outcomes after coronary artery bypass grafting. Am J Cardiol 2000;86:1128–1130, A6.
Lindenauer PK, Pekow P, Wang K, Gutierrez B, Benjamin EM. Lipid-lowering therapy and in-hospital mortality following major noncardiac surgery. JAMA 2004;291:2092–2099.
Chan AW, Bhatt DL, Chew DP, et al. Early and sustained survival benefit associated with statin therapy at the time of percutaneous coronary intervention. Circulation 2002;105:691–696.
Herrmann J, Lerman A, Baumgart D, et al. Preprocedural statin medication reduces the extent of periprocedural non-Q-wave myocardial infarction. Circulation 2002;106:2180–2183.
Poldermans D, Bax JJ, Kertai MD, et al. Statins are associated with a reduced incidence of perioperative mortality in patients undergoing major noncardiac vascular surgery. Circulation 2003;107:1848–1851.
Durazzo AE, Machado FS, Ikeoka DT, et al. Reduction in cardiovascular events after vascular surgery with atorvastatin: A randomized trial. J Vasc Surg 2004;39:967–975; discussion 975–976.
Pasceri V, Patti G, Nusca A, Pristipino C, Richichi G, Di Sciascio G. Randomized trial of atorvastatin for reduction of myocardial damage during coronary intervention: Results from the ARMYDA (Atorvastatin for Reduction of MYocardial Damage during Angioplasty) study. Circulation 2004;110:674–678.
Jones SP, Trocha SD, Lefer DJ. Pretreatment with simvastatin attenuates myocardial dysfunction after ischemia and chronic reperfusion. Arterioscler Thromb Vasc Biol 2001;21:2059–2064.
Jones S, Gibson M, Rimmer D, Gibson T, Sharp B, Lefer D. Direct vascular and cardioprotective effects of rosuvastatin, a new HMG-CoA reductase inhibitor. J Am Coll Cardiol 2002;40:1172–1178.
Scalia R, Gooszen ME, Jones SP, et al. Simvastatin exerts both anti-inflammatory and cardioprotective effects in apolipoprotein E-deficient mice. Circulation 2001;103:2598–2603.
Lefer DJ, Scalia R, Jones SP, et al. HMG-CoA reductase inhibition protects the diabetic myocardium from ischemia-reperfusion injury. FASEB J 2001;15:1454–1456.
Wayman NS, Ellis BL, Thiemermann C. Simvastatin reduces infarct size in a model of acute myocardial ischemia and reperfusion in the rat. Med Sci Monit 2003;9:BR155–159.
Wolfrum S, Grimm M, Heidbreder M, et al. Acute reduction of myocardial infarct size by a hydroxymethyl glutaryl coenzyme a reductase inhibitor is mediated by endothelial nitric oxide synthase. J Cardiovasc Pharmacol 2003;41:474–480.
Birnbaum Y, Ashitkov T, Uretsky BF, Ballinger S, Motamedi M. Reduction of infarct size by short-term pretreatment with atorvastatin. Cardiovasc Drugs Ther 2003;17:25–30.
Tavackoli S, Ashitkov T, Hu ZY, Motamedi M, Uretsky BF, Birnbaum Y. Simvastatin-induced myocardial protection against ischemia-reperfusion injury is mediated by activation of ATP-sensitive K+ channels. Cor Artery Dis 2004;15:53–58.
Hernandez-Perera O, Perez-Sala D, Navarro-Antolin J, et al. Effects of the 3-hydroxy-3-methylglutaryl-CoA reductase inhibitors, atorvastatin and simvastatin, on the expression of endothelin-1 and endothelial nitric oxide synthase in vascular endothelial cells. J Clin Invest 1998;101:2711–2719.
Kaesemeyer WH, Caldwell RB, Huang J, Caldwell RW. Pravastatin sodium activates endothelial nitric oxide synthase independent of its cholesterol-lowering actions. J Am Coll Cardiol 1999;33:234–241.
Amin-Hanjani S, Stagliano NE, Yamada M, Huang PL, Liao JK, Moskowitz MA. Mevastatin, an HMG-CoA reductase inhibitor, reduces stroke damage and upregulates endothelial nitric oxide synthase in mice. Stroke 2001;32:980–986.
Laufs U, La Fata V, Plutzky J, Liao JK. Upregulation of endothelial nitric oxide synthase by HMG CoA reductase inhibitors. Circulation 1998;97:1129–1135.
Laufs U, Gertz K, Huang P, et al. Atorvastatin upregulates type III nitric oxide synthase in thrombocytes, decreases platelet activation, and protects from cerebral ischemia in normocholesterolemic mice. Stroke 2000;31:2442–2449.
Laufs U, Gertz K, Dirnagl U, Bohm M, Nickenig G, Endres M. Rosuvastatin, a new HMG-CoA reductase inhibitor, upregulates endothelial nitric oxide synthase and protects from ischemic stroke in mice. Brain Res 2002;942:23–30.
Birnbaum Y, Ye Y, Rosanio S, et al. Prostaglandins mediate the cardioprotective effects of atorvastatin against ischemia-reperfusion injury. Cardiovasc Res 2005;65:345–355.
Salloum F, Yin C, Xi L, Kukreja RC. Sildenafil induces delayed preconditioning through inducible nitric oxide synthase-dependent pathway in mouse heart. Circ Res 2003;92:595–597.
Ockaili R, Salloum F, Hawkins J, Kukreja RC. Sildenafil (Viagra) induces powerful cardioprotective effect via opening of mitochondrial K(ATP) channels in rabbits. Am J Physiol Heart Circ Physiol 2002;283:H1263–H1269.
Das A, Ockaili R, Salloum F, Kukreja RC. Protein kinase C plays an essential role in sildenafil-induced cardioprotection in rabbits. Am J Physiol Heart Circ Physiol 2004;286:H1455–1460.
Das S, Maulik N, Das DK, Kadowitz PJ, Bivalacqua TJ. Cardioprotection with sildenafil, a selective inhibitor of cyclic 3′,5′-monophosphate-specific phosphodiesterase 5. Drugs Exp Clin Res 2002;28:213–219.
Bremer YA, Salloum F, Ockaili R, Chou E, Moskowitz WB, Kukreja RC. Sildenafil Citrate (Viagra) induces cardioprotective effects after ischemia/reperfusion injury in infant rabbits. Pediatr Res 2004;57:22–27.
Kukreja RC, Ockaili R, Salloum F, et al. Cardioprotection with phosphodiesterase-5 inhibition–a novel preconditioning strategy. J Mol Cell Cardiol 2004;36:165–173.
Castro MM, Rizzi E, Rascado RR, Nagassaki S, Bendhack LM, Tanus-Santos JE. Atorvastatin enhances sildenafil-induced vasodilation through nitric oxide-mediated mechanisms. Eur J Pharmacol 2004;498:189–194.
Garvey EP, Oplinger JA, Furfine ES, et al. 1400W is a slow, tight binding, and highly selective inhibitor of inducible nitric-oxide synthase in vitro and in vivo. J Biol Chem 1997;272:4959–4963.
Shinmura K, Tang XL, Wang Y, et al. Cyclooxygenase-2 mediates the cardioprotective effects of the late phase of ischemic preconditioning in conscious rabbits. Proc Natl Acad Sci USA 2000;97:10197–10202.
Das A, Xi L, Kukreja RC. Phosphodiesterase-5 inhibitor sildenafil preconditions adult cardiac myocytes against necrosis and apoptosis: Essential role of nitric oxide signaling. J Biol Chem 2005;280:12944–12955.
Brouet A, Sonveaux P, Dessy C, Moniotte S, Balligand JL, Feron O. Hsp90 and caveolin are key targets for the proangiogenic nitric oxide-mediated effects of statins. Circ Res 2001;89:866–873.
Fleming I, Busse R. Molecular mechanisms involved in the regulation of the endothelial nitric oxide synthase. Am J Physiol Regul Integr Comp Physiol 2003;284:R1–12.
Zhao T, Xi L, Chelliah J, Levasseur JE, Kukreja RC. Inducible nitric oxide synthase mediates delayed myocardial protection induced by activation of adenosine A(1) receptors: Evidence from gene-knockout mice. Circulation 2000;102:902–907.
Shinmura K, Xuan YT, Tang XL, et al. Inducible nitric oxide synthase modulates cyclooxygenase-2 activity in the heart of conscious rabbits during the late phase of ischemic preconditioning. Circ Res 2002;90:602–608.
Guo Y, Jones WK, Xuan YT, et al. The late phase of ischemic preconditioning is abrogated by targeted disruption of the inducible NO synthase gene. Proc Natl Acad Sci USA 1999;96:11507–11512.
Reffelmann T, Kloner RA. Effects of sildenafil on myocardial infarct size, microvascular function, and acute ischemic left ventricular dilation. Cardiovasc Res 2003;59:441–449.
Kureishi Y, Luo Z, Shiojima I, et al. The HMG-CoA reductase inhibitor simvastatin activates the protein kinase Akt and promotes angiogenesis in normocholesterolemic animals. Nat Med 2000;6:1004–1010.
Bell RM, Yellon DM. Atorvastatin, administered at the onset of reperfusion, and independent of lipid lowering, protects the myocardium by up-regulating a pro-survival pathway. J Am Coll Cardiol 2003;41:508–515.
Endres M, Laufs U, Huang Z, et al. Stroke protection by 3-hydroxy-3-methylglutaryl (HMG)-CoA reductase inhibitors mediated by endothelial nitric oxide synthase. Proc Natl Acad Sci U S A 1998;95:8880–8885.
Bell RM, Smith CC, Yellon DM. Nitric oxide as a mediator of delayed pharmacological (A(1) receptor triggered) preconditioning; is eNOS masquerading as iNOS? Cardiovasc Res 2002;53:405–413.
Shinmura K, Nagai M, Tamaki K, Tani M, Bolli R. COX-2-derived prostacyclin mediates opioid-induced late phase of preconditioning in isolated rat hearts. Am J Physiol Heart Circ Physiol 2002;283:H2534–H2543.
Kato T, Hashikabe H, Iwata C, Akimoto K, Hattori Y. Statin blocks Rho/Rho-kinase signalling and disrupts the actin cytoskeleton: Relationship to enhancement of LPS-mediated nitric oxide synthesis in vascular smooth muscle cells. Biochim Biophys Acta 2004;1689:267–272.
Birnbaum Y, Ye Y, Atar S, et al. Atorvastatin-induced myocardial protection against ischemia: iNOS mediates the increase in COX2 activity [abstract]. Circulation Research 2005;97:38.
Przyklenk K, Kloner RA. Sildenafil citrate (Viagra) does not exacerbate myocardial ischemia in canine models of coronary artery stenosis. J Am Coll Cardiol 2001;37:286–292.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosanio, S., Ye, Y., Atar, S. et al. Enhanced Cardioprotection Against Ischemia-Reperfusion Injury with Combining Sildenafil with Low-Dose Atorvastatin. Cardiovasc Drugs Ther 20, 27–36 (2006). https://doi.org/10.1007/s10557-005-5203-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-005-5203-4