Abstract
Objectives
We sought to distinguish area at risk from salvage myocardial zone and to predict left ventricle functional recovery in the convalescent stage by Texture Analysis (TA) of T2−Mapping.
Methods
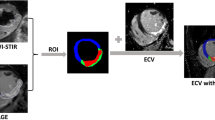
One hundred and six patients diagnosed with AMI and treated with percutaneous coronary intervention (PCI) underwent acute cardiac magnetic resonance imaging (CMR) and 45 of whom had a subsequent CMR scan following recovery. Cine imaging, T2−Mapping, T2−weighted STIR imaging, and LGE imaging were performed. In the texture analysis, regions of interest (infarcted, salvageable, and remote) were drawn by two blinded, independent readers.
Results
Seven independent texture features on T2−Mapping were selected: Perc.50%, S(2,2)InvDfMom, S(2.−2)AngScMom, S(4,0)Entropy, 45dgrLngREmph, 45dgr_Fraction and 135dr_GLevNonU. Among them, the average value of 135dr_GLevNonU in the infarct zone, AAR zone, and the remote zone was: 61.96±26.03, 31.811±18.933 and 99.839±26.231, respectively. Additionally, 135dr_GLevNonU provided the highest area under the curve (AUC) from the receiver operating characteristic curve (ROC curve) for distinguishing AAR from the infarct zone in each subgroup (all patients, patients with MVO and)were 0.845 ± 0.052 0.855 ± 0.083 and 0.845 ± 0.066, respectively, and were more promise than T2−Mapping mean (p<0.001). The AUC for differentiating AAR from the remote zone is 0.942±0.041. Texture features are not associated with convalescent decreased strain, ejection fraction (EF) or left ventricle remodeling (LVR) in analysis (p>0.05).
Conclusion
TA of T2−mapping can distinguish AAR from both the infarct zone and the remote myocardial zone without LGE imaging in reperfused AMI. However, these features are not able to predict patients’ functional recovery in the convalescent stage.






Similar content being viewed by others
Abbreviations
- TA:
-
Texture analysis
- AAR:
-
Area at risk
- PCI:
-
Percutaneous coronary intervention
- CMR:
-
Cardiac magnetic resonance imaging
- AMI:
-
Myocardial infarction
- AMI:
-
Acute myocardial infarction
- T2W-STIR:
-
T2-weighted short-tau triple inversion recovery
- LGE:
-
Late gadolinium enhancement
- AUC:
-
Area under the curve
- ROC curve:
-
Receiver operating characteristic curve
- MVO:
-
Microvascular obstruction
- IMH:
-
Intramyocardial hemorrhage
- EF:
-
Ejection fraction
- LVR:
-
Left ventricle remodeling
- ACS:
-
Acute coronary syndrome
- CKD:
-
Chronic kidney diseases
- FIS:
-
Final infarct size
- FWHM:
-
Full width at half maximum
- EDV:
-
End-diastolic volume
- ESV:
-
End-systolic volume
- SAX:
-
Short axis
- ICC:
-
Intraclass correlation coefficient
- ROI:
-
Region of interest
- SSFP:
-
Steady-state free precession
- HD:
-
Hemodialysis
References
Moore A et al (2019) Acute myocardial infarct. Radiol Clin North Am 57(1):45–55
Baessler B et al (2018) Subacute and chronic left ventricular myocardial scar: accuracy of texture analysis on nonenhanced cine MR images. Radiology 286(1):103–112
Kim HW et al (2015) Relationship of T2-weighted MRI myocardial hyperintensity and the ischemic area-at-risk. Circ Res 117(3):254–265
Lota AS, Gatehouse PD, Mohiaddin RH (2017) T2 mapping and T2* imaging in heart failure. Heart Fail Rev 22(4):431–440
Hammer-Hansen S et al (2014) Distinction of salvaged and infarcted myocardium within the ischaemic area-at-risk with T2 mapping. Eur Heart J Cardiovasc Imaging 15(9):1048–1053
Baessler B et al (2019) Cardiac MRI and texture analysis of myocardial T1 and T2 maps in myocarditis with acute versus chronic symptoms of heart failure. Radiology 292(3):608–617
Baessler B et al (2018) Texture analysis and machine learning of non-contrast T1-weighted MR images in patients with hypertrophic cardiomyopathy-preliminary results. Eur J Radiol 102:61–67
Khan JN et al (2015) Comparison of semi-automated methods to quantify infarct size and area at risk by cardiovascular magnetic resonance imaging at 15.T and 30.T field strengths. BMC Res Notes 8:52
Khan JN et al (2015) Comparison of cardiovascular magnetic resonance feature tracking and tagging for the assessment of left ventricular systolic strain in acute myocardial infarction. Eur J Radiol 84(5):840–848
Wang J et al (2018) Native T1 and T2 mapping by cardiovascular magnetic resonance imaging in pressure overloaded left and right heart diseases. J Thorac Dis 10(5):2968–2975
Kim HS et al (2019) Preoperative CT texture features predict prognosis after curative resection in pancreatic cancer. Sci Rep 9(1):17389
Fang WH et al (2020) Resectable pancreatic ductal adenocarcinoma: association between preoperative CT texture features and metastatic nodal involvement. Cancer Imaging 20(1):17
de Jager DJ et al (2009) Cardiovascular and noncardiovascular mortality among patients starting dialysis. JAMA 302(16):1782–1789
Garg P et al (2018) Role of cardiac T1 mapping and extracellular volume in the assessment of myocardial infarction. Anatol J Cardiol 19(6):404–411
Graham-Brown MP et al (2017) Native T1 mapping: inter-study, inter-observer and inter-center reproducibility in hemodialysis patients. J Cardiovasc Magn Reson 19(1):21
Zhang N et al (2019) Deep learning for diagnosis of chronic myocardial infarction on nonenhanced cardiac cine MRI. Radiology 291(3):606–617
Hansen E et al (2019) Validation of contrast enhanced cine steady-state free precession and T2-weighted CMR for assessment of ischemic myocardial area-at-risk in the presence of reperfusion injury. Int J Cardiovasc Imaging 35(6):1039–1045
Kidambi A et al (2017) Myocardial Extracellular volume estimation by CMR predicts functional recovery following acute MI. JACC Cardiovasc Imaging 10(9):989–999
Shao XN et al (2018) Texture analysis of magnetic resonance T1 mapping with dilated cardiomyopathy: a machine learning approach. Medicine 97(37):e12246
Gibbs T et al (2018) Quantitative assessment of myocardial scar heterogeneity using cardiovascular magnetic resonance texture analysis to risk stratify patients post-myocardial infarction. Clin Radiol 73(12):1059.e17-1059.e26
Bulluck H et al (2017) Full left ventricular coverage is essential for the accurate quantification of the area-at-risk by T1 and T2 mapping. Sci Rep 7(1):4871
Acknowledgements
We acknowledge the assistance from Rui Wu, Ruo-yang Shi and Yi-si Dai, who provided a lot of help in data processing.
Funding
Supported by National Natural Science Foundation of China (No.81873886 and No.81873887), Shanghai Shenkang Hospital Development Center Clinical Research and Cultivation Project (SHDC12018X21); Shanghai Science and technology innovation action plan, technology standard project (19DZ2203800); Shanghai Jiao Tong University school of medicine Double hundred outstanding person projrect (20191904); Shanghai Jiao Tong University medical cross project YG2017QN44.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no known conflicts of interest associated with this publication and there has been no significant financial support for this work that could have influenced its outcome.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
10554_2021_2336_MOESM1_ESM.tif
Supplementary file1 (TIF 6397 kb) Receiver operating characteristic (ROC) analyses for participants in differentiating infarcted and salvageable myocardium in all acute patients (a), patients without MVO (b) and patients with MVO (c).The ROC value for (a) is: Mean,0.647±0.074; Perc.500.639±0.074; (2,2)InvDfMom0.585±0.077; (2,-2)AngScMom0.647±0.074; (4,0)Entropy0.759±0.074; 45dgrLngREmph0.791±0.061; 45dgr_Fraction0.772±0.064;135dr_GLevNonU0.845±0.052.
Rights and permissions
About this article
Cite this article
Fan, ZY., Wu, Cw., An, DA. et al. Myocardial area at risk and salvage in reperfused acute MI measured by texture analysis of cardiac T2 mapping and its prediction value of functional recovery in the convalescent stage. Int J Cardiovasc Imaging 37, 3549–3560 (2021). https://doi.org/10.1007/s10554-021-02336-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10554-021-02336-7