Abstract
Purpose
Breast cancer is the most common cancer in reproductive age women, and treatment can affect fertility; however, there is often concern regarding the safety of increased estradiol (E2) levels and potential delays in treatment with ovarian stimulation for fertility preservation (FP). The aim of this study was to compare recurrence and survival in breast cancer patients who pursued FP without concurrent letrozole to those who did not (non-FP).
Methods
We reviewed charts of women with breast cancer who contacted the FP patient navigator (PN) at Northwestern University from 01/2005–01/2018. Oncology and fertility outcome data were collected. Data were analyzed by Chi-square test or regression, as appropriate. Kaplan–Meier curves were used to examine breast cancer recurrence and survival. Statistical analyses were performed with SPSS IBM Statistics 26.0 for Windows.
Results
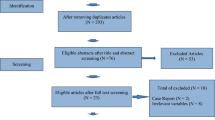
332 patients were included, of which 157 (47.3%) underwent FP. Median days to treatment after consulting the PN was 35 in the FP group and 21 in non-FP (p < 0.05). Cancer recurrence was noted in 7 (4.7%) FP patients and 13 (7.9%) non-FP patients (NS), and mortality in 5 (3.2%) FP patients and 7 (4.2%) non-FP patients (NS). Within the FP group, no significant differences were found in recurrence or mortality based on ER status, age, BMI, peak E2 level or total gonadotropin dose. Likelihood of pursuing FP was primarily a function of age and parity, and was not affected by breast cancer stage. To date, 21 have used cryopreserved specimens, and 13 (62%) had a live birth.
Conclusions
FP is safe and effective in breast cancer patients, regardless of receptor status; E2 elevations and the 2-week delay in treatment start are unlikely to be clinically significant. These findings are unique in that our institution does not use concomitant letrozole during stimulation to minimize E2 elevations in breast cancer patients.


Similar content being viewed by others
References
Rodriguez-Wallberg KA, Oktay K (2010) Fertility preservation in women with breast cancer. Clin Obstet Gynecol 53(4):753. https://doi.org/10.1097/GRF.0b013e3181f96e00
Noone AM, Howlader N, Krapcho M, Miller D, Brest A, Yu M et al (2018) SEER cancer statistics review, 1975–2015. National Cancer Institute, Bethesda
Letourneau JM, Ebbel EE, Katz PP, Katz A, Ai WZ, Chien AJ et al (2012) Pretreatment fertility counseling and fertility preservation improve quality of life in reproductive age women with cancer. Cancer 118(6):1710–1717. https://doi.org/10.1002/cncr.26459
Shnorhavorian M, Harlan LC, Smith AW, Keegan THM, Lynch CF, Prasad PK et al (2015) Fertility preservation knowledge, counseling, and actions among adolescent and young adult patients with cancer: a population-based study. Cancer 121(19):3499–3506. https://doi.org/10.1002/cncr.29328
Rodgers RJ, Reid GD, Koch J, Deans R, Ledger WL, Friedlander M et al (2017) The safety and efficacy of controlled ovarian hyperstimulation for fertility preservation in women with early breast cancer: a systematic review. Hum Reprod 32(5):1033–1045. https://doi.org/10.1093/humrep/dex027
Rodriguez-Wallberg KA, Eloranta S, Krawiec K, Lissmats A, Bergh J, Liljegren A (2018) Safety of fertility preservation in breast cancer patients in a register-based matched cohort study. Breast Cancer Res Treat 167(3):761–769. https://doi.org/10.1007/s10549-017-4555-3
Partridge AH, Gelber S, Peppercorn J, Sampson E, Knudsen K, Laufer M et al (2004) Web-based survey of fertility issues in young women with breast cancer. J Clin Oncol 22(20):4174–4183. https://doi.org/10.1200/jco.2004.01.159
Achille MA, Rosberger Z, Robitaille R, Lebel S, Gouin J-P, Bultz BD et al (2006) Facilitators and obstacles to sperm banking in young men receiving gonadotoxic chemotherapy for cancer: the perspective of survivors and health care professionals. Hum Reprod 21(12):3206–3216. https://doi.org/10.1093/humrep/del307
Crawshaw MA, Glaser AW, Hale JP, Sloper P (2009) Male and female experiences of having fertility matters raised alongside a cancer diagnosis during the teenage and young adult years. Eur J Cancer Care 18(4):381–390. https://doi.org/10.1111/j.1365-2354.2008.01003.x
Yee S, Abrol K, McDonald M, Tonelli M, Liu KE (2012) Addressing oncofertility needs: views of female cancer patients in fertility preservation. J Psychosoc Oncol 30(3):331–346. https://doi.org/10.1080/07347332.2012.664257
Loren AW, Mangu PB, Beck LN, Brennan L, Magdalinski AJ, Partridge AH et al (2013) Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. J Clin Oncol 31(19):2500–2510. https://doi.org/10.1200/JCO.2013.49.2678
Stein DM, Victorson DE, Choy JT, Waimey KE, Pearman TP, Smith K et al (2014) Fertility preservation preferences and perspectives among adult male survivors of pediatric cancer and their parents. J Adolesc Young Adult Oncol 3(2):75–82. https://doi.org/10.1089/jayao.2014.0007
Partridge AH, Pagani O, Abulkhair O, Aebi S, Amant F, Azim HA Jr et al (2014) First international consensus guidelines for breast cancer in young women (BCY1). Breast 23(3):209–220. https://doi.org/10.1016/j.breast.2014.03.011
Dewald SR, Natarajan L, Su I (2017) Fertility preservation and decisional regret in young breast cancer survivors: a longitudinal analysis. J Clin Oncol 35(5):106. https://doi.org/10.1200/JCO.2017.35.5_suppl.106
Larsen EC, Müller J, Schmiegelow K, Rechnitzer C, Andersen AN (2003) Reduced ovarian function in long-term survivors of radiation-and chemotherapy-treated childhood cancer. J Clin Endocrinol Metab 88(11):5307–5314. https://doi.org/10.1210/jc.2003-030352
Gardino SL, Jeruss JS, Woodruff TK (2010) Using decision trees to enhance interdisciplinary team work: the case of oncofertility. J Assist Reprod Genet 27(5):227–231. https://doi.org/10.1007/s10815-010-9413-8
Eskander RN, Randall LM, Berman ML, Tewari KS, Disaia PJ, Bristow RE (2011) Fertility preserving options in patients with gynecologic malignancies. Am J Obstet Gynecol 205(2):103–110. https://doi.org/10.1016/j.ajog.2011.01.025
Society for Assisted Reproductive Technology, American Society for Reproductive Medicine (2004) Assisted reproductive technology in the United States: 2000 results generated from the American Society for Reproductive Medicine/Society for Assisted Reproductive Technology Registry. Fertil Steril 81(5):1207–1220. https://doi.org/10.1016/j.fertnstert.2004.01.017
Wallace WHB, Anderson RA, Irvine DS (2005) Fertility preservation for young patients with cancer: who is at risk and what can be offered? Lancet Oncol 6(4):209–218. https://doi.org/10.1016/s1470-2045(05)70092-9
Oktay K, Harvey BE, Partridge AH, Quinn GP, Reinecke J, Taylor HS et al (2018) Fertility preservation in patients with cancer: ASCO clinical practice guideline update. J Clin Oncol 36(19):1994–2001. https://doi.org/10.1200/JCO.2018.78.1914
Bann CM, Treiman K, Squiers L, Tzeng J, Nutt S, Arvey S et al (2015) Cancer survivors’ use of fertility preservation. J Womens Health 24(12):1030–1037. https://doi.org/10.1089/jwh.2014.5160
Klock SC, Zhang JX, Kazer RR (2010) Fertility preservation for female cancer patients: early clinical experience. Fertil Steril 94(1):149–155. https://doi.org/10.1016/j.fertnstert.2009.03.028
Moravek MB, Confino R, Smith KN, Kazer RR, Klock SC, Lawson AK et al (2018) Long-term outcomes in cancer patients who did or did not pursue fertility preservation. Fertil Steril 109(2):349–355. https://doi.org/10.1016/j.fertnstert.2017.10.029
Chien AJ, Chambers J, Mcauley F, Kaplan T, Letourneau J, Hwang J et al (2017) Fertility preservation with ovarian stimulation and time to treatment in women with stage II–III breast cancer receiving neoadjuvant therapy. Breast Cancer Res Treat 165(1):151–159. https://doi.org/10.1007/s10549-017-4288-3
Pike MC, Spicer DV, Dahmoush L, Press MF (1993) Estrogens, progestogens, normal breast cell proliferation, and breast cancer risk. Epidemiol Rev 15(1):17–35. https://doi.org/10.1093/oxfordjournals.epirev.a036102
Sonmezer M, Oktay K (2006) Fertility preservation in young women undergoing breast cancer therapy. Oncologist 11(5):422–434. https://doi.org/10.1634/theoncologist.11-5-422
Samavat H, Kurzer MS (2015) Estrogen metabolism and breast cancer. Cancer Lett 356(2):231–243. https://doi.org/10.1016/j.canlet.2014.04.018
Cole PA, Robinson CH (1990) Mechanism and inhibition of cytochrome P-450 aromatase. J Med Chem 33(11):2933–2942
Oktay K, Buyuk E, Libertella N, Akar M, Rosenwaks Z (2005) Fertility preservation in breast cancer patients: a prospective controlled comparison of ovarian stimulation with tamoxifen and letrozole for embryo cryopreservation. J Clin Oncol 23(19):4347–4353. https://doi.org/10.1200/jco.2005.05.037
Papanikolaou EG, Polyzos NP, Humaidan P, Pados G, Bosch E, Tournaye H et al (2011) Aromatase inhibitors in stimulated IVF cycles. Reprod Biol Endocrinol 9(1):85. https://doi.org/10.1186/1477-7827-9-85
Reddy J, Oktay K (2012) Ovarian stimulation and fertility preservation with the use of aromatase inhibitors in women with breast cancer. Fertil Steril 98(6):1363–1369. https://doi.org/10.1016/j.fertnstert.2012.09.022
Turan V, Bedoschi G, Moy F, Oktay K (2013) Safety and feasibility of performing two consecutive ovarian stimulation cycles with the use of letrozole-gonadotropin protocol for fertility preservation in breast cancer patients. Fertil Steril 100(6):1681–5.e1. https://doi.org/10.1016/j.fertnstert.2013.08.030
Oktay K, Turan V, Kim J (2015) Long-term safety of fertility preservation by ovarian stimulation and concurrent aromatase inhibitor treatment in women with breast cancer. J Clin Oncol 33(15):9521
Oktay K, Turan V, Bedoschi G, Pacheco FS, Moy F (2015) Fertility preservation success subsequent to concurrent aromatase inhibitor treatment and ovarian stimulation in women with breast cancer. J Clin Oncol 33(22):2424–2429. https://doi.org/10.1200/JCO.2014.59.3723
Allen PB, Pavone ME, Smith KN, Kazer R, Rademaker AW, Lawson AK et al (2018) The impact of fertility preservation on treatment delay and progression-free survival in women with lymphoma: a single-centre experience. Br J Haematol 180(6):901–904. https://doi.org/10.1111/bjh.14466
Akel RA, Guo XM, Moravek MB, Confino R, Smith KN, Lawson AK et al (2020) Ovarian stimulation is safe and effective for patients with gynecologic cancer. J Adolesc Young Adult Oncol 9(3):367–374. https://doi.org/10.1089/jayao.2019.0124
Pavone ME, Innes J, Hirshfeld-Cytron JE, Kazer R, Zhang J (2011) Comparing thaw survival, implantation and live birth rates from cryopreserved zygotes, embryos and blastocysts. J Hum Reprod Sci 4(1):23–28. https://doi.org/10.4103/0974-1208.82356
Kim J, Turan V, Oktay K (2016) Long-term safety of letrozole and gonadotropin stimulation for fertility preservation in women with breast cancer. J Clin Endocrinol Metab 101(4):1364–1371. https://doi.org/10.1210/jc.2015-3878
Goldrat O, Gervy C, Englert Y, Delbaere A, Demeestere I (2015) Progesterone levels in letrozole associated controlled ovarian stimulation for fertility preservation in breast cancer patients. Hum Reprod 30(9):2184–2189. https://doi.org/10.1093/humrep/dev155
Shapira M, Raanani H, Meirow D (2015) IVF for fertility preservation in breast cancer patients: efficacy and safety issues. J Assist Reprod Genet 32(8):1171–1178. https://doi.org/10.1007/s10815-015-0519-x
Oktay K, Hourvitz A, Sahin G, Oktem O, Safro B, Cil A et al (2006) Letrozole reduces estrogen and gonadotropin exposure in women with breast cancer undergoing ovarian stimulation before chemotherapy. J Clin Endocrinol Metab 91(10):3885–3890. https://doi.org/10.1210/jc.2006-0962
Domingo J, Guillén V, Ayllón Y, Martínez M, Muñoz E, Pellicer A et al (2012) Ovarian response to controlled ovarian hyperstimulation in cancer patients is diminished even before oncological treatment. Fertil Steril 97(4):930–934. https://doi.org/10.1016/j.fertnstert.2012.01.093
Revelli A, Porcu E, Levi Setti PE, Delle Piane L, Merlo DF, Anserini P (2013) Is Letrozole needed for controlled ovarian stimulation in patients with estrogen receptor-positive breast cancer? Gynecol Endocrinol 29(11):993–996. https://doi.org/10.3109/09513590.2013.819083
Colleoni M, Sun Z, Price KN, Karlsson P, Forbes JF, Thürlimann B et al (2016) Annual hazard rates of recurrence for breast cancer during 24 years of follow-up: results From the International Breast Cancer Study Group Trials I to V. J Clin Oncol 34(9):927–935. https://doi.org/10.1200/JCO.2015.62.3504
Wangchinda P, Ithimakin S (2016) Factors that predict recurrence later than 5 years after initial treatment in operable breast cancer. World J Surg Oncol 14(1):223. https://doi.org/10.1186/s12957-016-0988-0
Acknowledgements
The authors wish to thank all faculty, nurses, and staff at Northwestern Fertility and Reproductive Medicine for the excellent care they provide patients.
Funding
This study was funded by the National Institutes of Health and Northwestern Memorial Foundation Evergreen Grant (to MEP) and P50 HD076188 (MEP, PI: T. Woodruff).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors Molly B. Moravek, Rafael Confino, Angela K. Lawson, Kristin N. Smith, Ralph R. Kazer, Susan C. Klock, Jacqueline S. Jeruss and Mary Ellen Pavone declares that they have no conflict of interest. William J. Gradishar is the Editor-in-Chief of Breast Cancer Research and Treatment.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Moravek, M.B., Confino, R., Lawson, A.K. et al. Predictors and outcomes in breast cancer patients who did or did not pursue fertility preservation. Breast Cancer Res Treat 186, 429–437 (2021). https://doi.org/10.1007/s10549-020-06031-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-020-06031-4