Abstract
Purpose
The association between polycystic ovary syndrome (PCOS) and breast cancer remains inconclusive. Conventional observational studies are susceptible to inverse causality and potential confounders. With a Mendelian randomization (MR) approach, we aimed to investigate the causal relationship between genetically predicted PCOS and breast cancer risk.
Methods
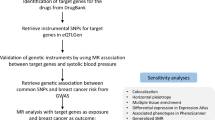
Our study included 11 PCOS-associated single nucleotide polymorphisms as instrumental variables identified by the latest genome-wide association study. Individual-level genetic summary data of participants were obtained from the Breast Cancer Association Consortium, with a total of 122,977 cases and 105,974 controls. The inverse-variance weighted method was applied to estimate the causality between genetically predicted PCOS and breast cancer risk. To further evaluate the pleiotropy, the weighted median and MR-Egger regression methods were implemented as well.
Results
Our study demonstrated that genetically predicted PCOS was causally associated with an increased risk of overall breast cancer (odds ratio (OR) = 1.07; 95% confidence interval (CI) 1.02–1.12, p = 0.005). The subgroup analyses according to immunohistochemical type further illustrated that genetically predicted PCOS was associated with an increased risk of estrogen receptor (ER)-positive breast cancer (OR = 1.09; 95% CI 1.03–1.15, p = 0.002), while no causality was observed for ER-negative breast cancer (OR = 1.02; 95% CI 0.96–1.09, p = 0.463). In addition, no pleiotropy was found in our study.
Conclusions
Our findings indicated that PCOS was likely to be a causal factor in the development of ER-positive breast cancer, providing a better understanding for the etiology of breast cancer and the prevention of breast cancer.
Similar content being viewed by others
Abbreviations
- AR:
-
Androgen receptor
- BCAC:
-
Breast Cancer Association Consortium
- GIANT:
-
Genetic Investigation of Anthropometric Traits
- MRC-IEU:
-
Medical Research Council Integrative Epidemiology Unit
- CIs:
-
Confidence intervals
- BMI:
-
Body mass index
- ER:
-
Estrogen receptor
- GWASs:
-
Genome-wide association studies
- IVs:
-
Instrumental variables
- IVF:
-
In vitro fertilization
- IVW:
-
Inverse-variance weighted
- LD:
-
Linkage disequilibrium
- NIH:
-
National Institutes of Health
- MR:
-
Mendelian randomization
- OCs:
-
Oral contraceptives
- ORs:
-
Odds ratios
- PCOS:
-
Polycystic ovary syndrome
- SNPs:
-
Single nucleotide polymorphisms
References
Sirmans SM, Pate KA (2013) Epidemiology, diagnosis, and management of polycystic ovary syndrome. Clin Epidemiol. https://doi.org/10.2147/CLEP.S37559
Azziz R et al (2016) Polycystic ovary syndrome. Nat Rev 2:16057
Christ JP, Gunning MN, Fauser BCJM (2017) Implications of the 2014 androgen excess and polycystic ovary syndrome society guidelines on polycystic ovarian morphology for polycystic ovary syndrome diagnosis. Reprod Biomed 35(4):480–483
Lansdown AJ et al (2019) Regional cerebral activation accompanies sympathoexcitation in women with polycystic ovary syndrome. J Clin Endocrinol Metab 104(9):3614–3623
Shafiee MN et al (2013) Reviewing the molecular mechanisms which increase endometrial cancer (EC) risk in women with polycystic ovarian syndrome (PCOS): time for paradigm shift? Gynecol Oncol 131(2):489–492
Flint MS et al (2007) Induction of DNA damage, alteration of DNA repair and transcriptional activation by stress hormones. Psychoneuroendocrinology 32(5):470–479
Wild S et al (2000) Long-term consequences of polycystic ovary syndrome: results of a 31 year follow-up study. Hum Fertil 3(2):101–105
Shen CC et al (2015) A nationwide population-based retrospective cohort study of the risk of uterine, ovarian and breast cancer in women with polycystic ovary syndrome. Oncologist 20(1):45–49
Baron JA et al (2001) Metabolic disorders and breast cancer risk (United States). Cancer Causes Control 12(10):875–880
Kim J et al (2016) Polycystic ovarian syndrome (PCOS), related symptoms/sequelae, and breast cancer risk in a population-based case-control study. Cancer Causes Control 27(3):403–414
Yin W et al (2019) Association between polycystic ovary syndrome and cancer risk. JAMA Oncology 5(1):106–107
Anderson KE et al (1997) Association of Stein-Leventhal syndrome with the incidence of postmenopausal breast carcinoma in a large prospective study of women in Iowa. Cancer 79(3):494–499
Gottschau M et al (2015) Risk of cancer among women with polycystic ovary syndrome: a Danish cohort study. Gynecol Oncol 136(1):99–103
Brinton LA et al (2010) Cancer risk among infertile women with androgen excess or menstrual disorders (including polycystic ovary syndrome). Fertil Steril 94(5):1787–1792
Ding DC et al (2018) Association between polycystic ovarian syndrome and endometrial, ovarian, and breast cancer: a population-based cohort study in Taiwan. Medicine (Baltimore) 97(39):e12608
Talamini R et al (1997) Frequency of poly cystic ovary syndrome in patients with premenopausal breast cancer. Br J Cancer 75(11):1699–1703
Ghasemi N, Mortazavizadeh MR, Khorasani Gerdekoohi A (2010) Frequency of poly cystic ovary syndrome in patients with premenopausal breast cancer. Int J Reprod Biomed 8(2):86
Shobeiri F, Jenabi E (2016) The association between polycystic ovary syndrome and breast cancer: a meta-analysis. Obstet Gynecol Sci 59(5):367–372
Carvalho MJ et al (2019) Controversial association between polycystic ovary syndrome and breast cancer. Eur J Obstet Gynecol Reprod Biol 243:125–132
Key TJ et al (2011) Circulating sex hormones and breast cancer risk factors in postmenopausal women: reanalysis of 13 studies. Br J Cancer 105(5):709–722
Lawlor DA et al (2008) Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med 27(8):1133–1163
Shi Y et al (2012) Genome-wide association study identifies eight new risk loci for polycystic ovary syndrome. Nat Genet 44(9):1020–1025
Chen ZJ et al (2011) Genome-wide association study identifies susceptibility loci for polycystic ovary syndrome on chromosome 2p16.3, 2p21 and 9q33.3. Nat Genet 43(1):55–59
Burgess S et al (2015) Using published data in Mendelian randomization: a blueprint for efficient identification of causal risk factors. Eur J Epidemiol 30(7):543–552
Pierce BL, Burgess S (2013) Efficient design for Mendelian randomization studies: subsample and 2-sample instrumental variable estimators. Am J Epidemiol 178(7):1177–1184
Harris HR et al (2019) Association between genetically predicted polycystic ovary syndrome and ovarian cancer: a Mendelian randomization study. Int J Epidemiol 48(3):822–830
Day F et al (2018) Large-scale genome-wide meta-analysis of polycystic ovary syndrome suggests shared genetic architecture for different diagnosis criteria. PLoS Genet 14(12):e1007813
Hemani G et al (2018) The MR-Base platform supports systematic causal inference across the human phenome. eLife 7:e34408
About BCAC – The Breast Cancer Association Consortium. Centre for Cancer Genetic Epidemiology> https://bcac.ccge.medschl.cam.ac.uk/. Accessed 28 Mar 2020
VanderWeele TJ et al (2014) Methodological challenges in mendelian randomization. Epidemiology 25(3):427–435
Bowden J et al (2017) A framework for the investigation of pleiotropy in two-sample summary data Mendelian randomization. Stat Med 36(11):1783–1802
Dimitrakakis C, Bondy C (2009) Androgens and the breast. Breast Cancer Res 11(5):212
Berrino F et al (2005) Serum testosterone levels and breast cancer recurrence. Int J Cancer 113(3):499–502
Schmitt M et al (2001) Dehydroepiandrosterone stimulates proliferation and gene expression in MCF-7 cells after conversion to estradiol. Mol Cell Endocrinol 173:1–2
Ortmann J et al (2002) Testosterone and 5 alpha-dihydrotestosterone inhibit in vitro growth of human breast cancer cell lines. Gynecol Endocrinol 16(2):113–120
Farhat GN et al (2011) Sex hormone levels and risks of estrogen receptor-negative and estrogen receptor-positive breast cancers. J Natl Cancer Inst 103(7):562–570
Cummings SR et al (2005) Sex hormones, risk factors, and risk of estrogen receptor-positive breast cancer in older women: a long-term prospective study. Cancer Epidemiol Biomark Prev 14(5):1047–1051
Haendler B, Cleve A (2012) Recent developments in antiandrogens and selective handrogen receptor modulators. Mol Cell Endocrinol 352(1–2):79–91
Lin H-Y et al (2009) Androgen-induced human breast cancer cell proliferation is mediated by discrete mechanisms in estrogen receptor-alpha-positive and -negative breast cancer cells. J Steroid Biochem Mol Biol 113(3–5):182–188
Clark NM et al (2014) Prevalence of polycystic ovary syndrome phenotypes using updated criteria for polycystic ovarian morphology: an assessment of over 100 consecutive women self-reporting features of polycystic ovary syndrome. Reprod Sci 21(8):1034–1043
Acknowledgements
The authors acknowledge the efforts of the consortia in providing high-quality GWAS resources for researchers. Data and material are available from corresponding GWAS consortium. The authors also thank Ms. Lindsey Hamblin for helping to edit the manuscript.
Funding
This study was supported by the National Key R&D Program of China [2016YFC0905400]; China National Science Foundation [81871893, 81501996]; Key Project of Guangzhou Scientific Research Project [201804020030]; High-level university construction project of Guangzhou Medical University [20182737, 201721007, 201715907, 2017160107]; IVATS National key R&D Program [2017YFC0907903, 2017YFC0112704]; and Application, industrialization, and generalization of surgical incision protector [2011B090400589].
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
This article does not contain any studies with human participants or animals performed by any of the authors. Thus, there is no need for informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wen, Y., Wu, X., Peng, H. et al. Breast cancer risk in patients with polycystic ovary syndrome: a Mendelian randomization analysis. Breast Cancer Res Treat 185, 799–806 (2021). https://doi.org/10.1007/s10549-020-05973-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-020-05973-z