Abstract
Background
Depression is a major morbidity and the most common mental disorder among the medical students in medical schools globally. Undergraduate students suffer stress more due to their academic curriculum than the students of other faculties. In low-resource settings like Bangladesh, there is a dearth in research on the mental health of undergraduate medical students. This pilot study was conducted to add to the existing limited evidence by reporting the prevalence of depression and describing sleeping pattern and suicidal tendencies among medical students. Relevantly, we have investigated the overall mental health status among the medical students in Bangladesh.
Methods
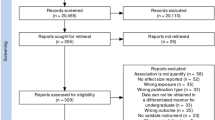
This cross-sectional study was conducted in two medical colleges of Dhaka between July 2013 and December 2013, among 221 Bangladeshi medical students from first to fifth year. By the convenience sampling technique, data were collected by a pretested, structured, self-administered questionnaire and analysis was done by SPSS version 18.0. Depression was assessed by the validated Patient Health Questionnaire-9 (PHQ-9) tool among the respondents. Goldberg’s General Health Questionnaire (GHQ-28) was used for assessing overall mental health status.
Results
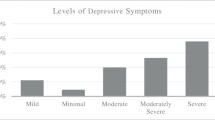
Depression was found in 38.9% of participants, with 3.6%, 14.5%, and 20.8% being severe, moderate, and mild depression, respectively. 17.6% of medical students had suicidal tendency or attempted suicide at least once after attending medical school. The sleeping hours were inadequate and altered after starting this stressful academic course. 33.5% of medical students had poor mental health status. There was a statistically significant association between poor mental health status in the age group less than 22 years old and initial academic study year (1st to 3rd of MBBS).
Conclusion
The findings are suggestive of a higher prevalence of depression among early-year medical students and marginal predominance in males. Suicidal tendency is also higher. This calls for further investigation with situation analysis, qualitative explorations, and surveys to explore the burden of such disorders in Bangladesh.



Similar content being viewed by others
References
Adhikari A, Dutta A, Sapkota S, Chapagain A, Aryal A, Pradhan A (2017) Prevalence of poor mental health among medical students in Nepal: a cross-sectional study. BMC Med Educ 17(1):232. https://doi.org/10.1186/s12909-017-1083-0
Alim SMAHM, Rabbani MG, Karim E et al (2015) Assessment of depression, anxiety and stress among first year MBBS students of a public medical college, Bangladesh. Bang J Psychiatry 29(1):23–29
Bangladesh Medical & Dental Council (BMDC) (2018) Home page at: https://web.bmdc.org.bd/. Accessed 12 Nov 2019
Bergmann C, Muth T, Loerbroks A (2019) Medical students’ perceptions of stress due to academic studies and its interrelationships with other domains of life: a qualitative study. Med Educ Online 24(1):1603526. https://doi.org/10.1080/10872981.2019.1603526
Brazeau CMLR, Shanafelt T, Durning SJ et al (2014) Distress among matriculating medical students relative to the general population. Acad Med 89(11):1520–1525. https://doi.org/10.1097/ACM.0000000000000482
Cochran WG (2007) Sampling techniques, 3rd edn. Wiley, New York
Dyrbye LN, Thomas MR, Shanafelt TD (2006) Systematic review of depression, anxiety, and other indicators of psychological distress among U.S. and Canadian medical students. Acad Med 81(4):354–373. https://doi.org/10.1097/00001888-200604000-00009
Garg K, Agarwal M, Dalal PK (2017) Stress among medical students: a cross-sectional study from a North Indian Medical University. Indian J Psychiatry 59(4):502–504. https://doi.org/10.4103/psychiatry.IndianJPsychiatry_239_17
Goldberg DP (1972) The General Health Questionnaire (GHQ). Companion to psychiatric studies. Oxford University Press, London, pp 172–173
Hill MR, Goicochea S, Merlo LJ (2018) In their own words: stressors facing medical students in the millennial generation. Med Educ Online 23(1):1530558. https://doi.org/10.1080/10872981.2018.1530558
Hossain S, Anjum A, Uddin ME, Rahman MA, Hossain MF (2019) Impacts of socio-cultural environment and lifestyle factors on the psychological health of university students in Bangladesh: a longitudinal study. J Affect Disord 256:393–403. https://doi.org/10.1016/j.jad.2019.06.001
Kindermann D, Jenne MP, Schmid C et al (2019) Motives, experiences and psychological strain in medical students engaged in refugee care in a reception center—a mixed-methods approach. BMC Med Educ 19(1):302. https://doi.org/10.1186/s12909-019-1730-8
Kjeldstadli K, Tyssen R, Finset A et al (2006) Life satisfaction and resilience in medical school—a six-year longitudinal, nationwide and comparative study. BMC Med Educ 6:48. https://doi.org/10.1186/1472-6920-6-48
Kosik RO, Nguyen T, Ko I, Fan AP (2017) Suicidal ideation in medical students. Neuropsychiatry 7(1):9–11. https://doi.org/10.4172/Neuropsychiatry.1000172
Krejcie RV, Morgan DW (1970) Determining sample size for research activities. Educ Psychol Meas 30(3):607–610
Kumar SG, Kattimani S, Sarkar S, Kar SS (2017) Prevalence of depression and its relation to stress level among medical students in Puducherry, India. Ind Psychiatry J 26(1):86–90
Mao Y, Zhang N, Liu J, Zhu B, He R, Wang X (2019) A systematic review of depression and anxiety in medical students in China. BMC Med Educ 19(1):327. https://doi.org/10.1186/s12909-019-1744-2
Melaku L, Mossie A, Negash A (2015) Stress among medical students and its association with substance use and academic performance. J Biomed Educ 2015:149509. https://doi.org/10.1155/2015/149509
Mitsui N, Asakura S, Shimizu Y et al (2014) The association between suicide risk and self-esteem in Japanese university students with major depressive episodes of major depressive disorder. Neuropsychiatr Dis Treat 10:811–816. https://doi.org/10.2147/NDT.S59349
Nojomi M, Gharayee B (2007) Medical students and mental health by SCL-90-R. Med J Islam Repub Iran 21(2):71–78
Pereira MAD, Barbosa MA, de Rezende JC, Damiano RF (2015) Medical student stress: an elective course as a possibility of help. BMC Res Notes 8:430. https://doi.org/10.1186/s13104-015-1399-y
Puthran R, Zhang MW, Tam WW, Ho RC (2016) Prevalence of depression amongst medical students: a meta-analysis. Med Educ 50(4):456–468. https://doi.org/10.1111/medu.12962
Rotenstein LS, Ramos MA, Torre M et al (2016) Prevalence of depression, depressive symptoms, and suicidal ideation among medical students: a systematic review and meta-analysis. JAMA 316(21):2214–2236. https://doi.org/10.1001/jama.2016.17324
Schwenk TL, Davis L, Wimsatt LA (2010) Depression, stigma, and suicidal ideation in medical students. JAMA 304(11):1181–1190. https://doi.org/10.1001/jama.2010.1300
Shah MMA, Ahmed S, Arafat SMY (2017) Demography and risk factors of suicide in Bangladesh: a six-month paper content analysis. Psychiatry J 2017:3047025. https://doi.org/10.1155/2017/3047025
Shahnaz A, Bagley C, Simkhada P, Kadri S (2017) Suicidal behaviour in Bangladesh: a scoping literature review and a proposed public health prevention model. Open J Soc Sci 5(7):254–282. https://doi.org/10.4236/jss.2017.57016
Sherina MS, Rampal L, Kaneson N (2004) Psychological stress among undergraduate medical students. Med J Malaysia 59(2):207–211
Sohrabi MR, Malih N, Karimi HR, Hajihashemi Z (2019) Effect of general medical degree curricular change on mental health of medical students: a concurrent controlled educational trial. Iran J Psychiatry 14(1):40–46
Uttra AM, Uttra MGM, Rauf A, Uttra MM, Hassan UH, Batool A (2017) Prevalence of depression; a cross-sectional study among MBBS students of Sargodha medical college, Sargodha Pakistan. Prof Med J 24(3):482–489. https://doi.org/10.17957/tpmj/17.3708
World Health Organization, Regional Office for South-East Asia (2007) WHO-AIMS report on mental health system in Bangladesh. WHO Regional Office for South-East Asia, New Delhi, India
Yeasmin T (2018) Medical student commits suicide after failing one exam 11 times in 5 years. Dhaka Tribune
Zavlin D, Jubbal KT, Noe JG, Gansbacher B (2017) A comparison of medical education in Germany and the United States: from applying to medical school to the beginnings of residency. German Med Sci 15:Doc15. https://doi.org/10.3205/000256
Acknowledgements
The authors want to express sincere gratitude to Prof. Dr. Ahmed Neaz, Advisor, Department of Public Health, American International University-Bangladesh (AIUB) for his valuable advice whilst conducting the study. The contributions of Dr. Palash Golder, Dr. Rashedul Islam from Shaheed Suhrawardy Medical College, Dhaka; Dr. Gourab Adhikary, Dr. Kazi Rezaul Ahsan, Shumona Sharmin Salam from ICDDR, B are well acknowledged by the study team for their kind support during data collection, analysis, and report preparation phase.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
M.T.H. drafted the protocol, tool, translated the tool, analyzed, and prepared the draft report. R.D.G. supported the data collection and reviewed the manuscript. N.A.M., A.G., R.N.N., and M.S.T.H.K. supported the tool development, data collection, and took part in primary analysis. F.A. and S.H. prepared the tables and results section. V.P. prepared the discussion segment. H.R.M. and K.N.K. critically reviewed the manuscript. S.Y. supported data collection and reviewed the manuscript. N.I. supervised this project.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical considerations
Approval was obtained from the ethics committee of American International University-Bangladesh. The procedures used in this study adhere to the tenets of the Declaration of Helsinki. Each participant provided written informed consent. Detailed study-related information, including objectives, brief methods, and data confidentiality procedure, was provided via a printed handout. Privacy and confidentiality of the respondents during data collection were maintained strictly.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hasan, M.T., Hossain, S., Gupta, R.D. et al. Depression, sleeping pattern, and suicidal ideation among medical students in Bangladesh: a cross-sectional pilot study. J Public Health (Berl.) 30, 465–473 (2022). https://doi.org/10.1007/s10389-020-01304-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-020-01304-0