Abstract
Aim
To investigate the features of type-specific persistent HPV infection and the associated risk factors in Uyghur women.
Subjects and methods
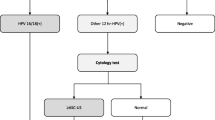
From September 2012 to August 2013, Uyghur women who underwent opportunistic screening for cervical cancer at the People’s Hospital of Xinjiang Uygur Autonomous Region were recruited during the baseline investigation. After testing for HPV infection and genotyping, 300 women with chronic cervicitis and 300 women negative for HPV were enrolled in the nested case-control study. Information came from the sample subjects interviewed using questionnaires and follow-up study.
Results
The type-specific persistent HPV infection rate was 25.50 % (65/255). The top five most common HPV types were HPV16 (48.00 %), HPV18 (31.03 %), HPV58 (28.30 %), HPV52 (23.40 %) and HPV45 (21.43 %). The risk of type-specific persistent HPV infection was increased 4.81-fold for HPV16 compared with non-HPV16. Compared with transient HPV infection, menopause and not using condoms were risk factors for persistent infection.
Conclusion
The risk factors for persistent HPV infection for Uyghur women included having HPV16 infection, having menopause and not using condoms. Regular screening and close follow-up should be carried out in this high-risk population.

Similar content being viewed by others

References
Carcopino X, Bolger N, Henry M, Mancini J, Boubli L, Olive D, Cleary S, Prendiville W, Tamalet C (2011) Evaluation of type‐specific HPV persistence and high‐risk HPV viral load quantitation in HPV positive women under 30 with normal cervical cytology. J Med Virol 83:637–643
De Villiers E-M (2001) Taxonomic classification of papillomaviruses. Papillomavirus Report 12:57–63
García-Piñeres AJ, Hildesheim A, Herrero R, Trivett M, Williams M, Atmetlla I, Ramírez M, Villegas M, Schiffman M, Rodríguez AC, Burk RD, Hildesheim M, Freer E, Bonilla J, Bratti C, Berzofsky JA, Pinto LA (2006) Persistent human papillomavirus infection is associated with a generalized decrease in immune responsiveness in older women. Cancer Res 66:11070–11076
Harper DM, Demars LR (2014) Primary strategies for HPV infection and cervical cancer prevention. Clin Obstet Gynecol 57:256–278
Hildesheim A, Schiffman MH, Gravitt PE, Glass AG, Greer CE, Zhang T, Scott DR, Rush BB, Lawler P, Sherman ME, Kurman RJ, Manos MM (1994) Persistence of type-specific human papillomavirus infection among cytologically normal women. J Infect Dis 169:235–240
Hogewoning CJ, Bleeker MC, van den Brule AJ, Voorhorst FJ, Snijders PJ, Berkhof J, Westenend PJ, Meijer CJ (2003) Condom use promotes regression of cervical intraepithelial neoplasia and clearance of human papillomavirus: a randomized clinical trial. Int J Cancer 107:811–816
Howe ER, Li Z, McGlennen RC, Hellerstedt WL, Downs LS (2009) Type-specific prevalence and persistence of human papillomavirus in women in the United States who are referred for typing as a component of cervical cancer screening. Am J Obstet Gynecol 200:245.e1–245.e7
Lam JUH, Rebolj M, Dugué PA, Bonde J, Lynge E (2014) Condom use in prevention of Human Papillomavirus infections and cervical neoplasia: systematic review of longitudinal studies. J Med Screen 21:38–50
Miranda PM, Silva NN, Pitol BC, Silva ID, Lima-Filho JL, Carvalho RF, Stocco RC, Beçak C, Lima AA (2013) Persistence or clearance of human papillomavirus infections in women in Ouro Preto, Brazil. BioMed Research International 2013
Mitra S (2009) Study of the risk factors for cancer cervix in a speciality hospital in Kolkata. J Com Med 5:1–5
Muñoz N, Bosch FX, de Sanjosé S, Herrero R, Castellsagué X, Shah KV, Snijders PJ, Meijer CJ (2003) Epidemiologic classification of human papillomavirus types associated with cervical cancer. N Engl J Med 348:518–527
Muñoz N, Bosch FX, Castellsagué X, Díaz M, de Sanjose S, Hammouda D, Shah KV, Meijer CJ (2004) Against which human papillomavirus types shall we vaccinate and screen? The international perspective. Int J Cancer 111:278–285
Nam EJ, Kim JW, Kim SW, Kim YT, Kim JH, Yoon BS, Cho NH, Kim S (2007) The expressions of the Rb pathway in cervical intraepithelial neoplasia; predictive and prognostic significance. Gynecol Oncol 104:207–211
Nielsen A, Kjaer SK, Munk C, Osler M, Iftner T (2010) Persistence of high‐risk human papillomavirus infection in a population‐based cohort of Danish women. J Med Virol 82:616–623
Schiffman M, Herrero R, Desalle R, Hildesheim A, Wacholder S, Rodriguez AC, Bratti MC, Sherman ME, Morales J, Guillen D, Alfaro M, Hutchinson M, Wright TC, Solomon D, Chen Z, Schussler J, Castle PE, Burk RD (2005) The carcinogenicity of human papillomavirus types reflects viral evolution. Virology 337:76–84
Schlecht NF, Kulaga S, Robitaille J, Ferreira S, Santos M, Miyamura RA, Duarte-Franco E, Rohan TE, Ferenczy A, Villa LL, Franco EL (2001) Persistent human papillomavirus infection as a predictor of cervical intraepithelial neoplasia. JAMA 286:3106–3114
Smith E, Johnson S, Ritchie J, Feddersen D, Wang D, Turek L, Haugen T (2004) Persistent HPV infection in postmenopausal age women. Int J Gynecol Obstet 87:131–137
Sui S, Jiao Z, Niyazi M, Lu P, Qiao Y (2012) Genotype distribution and behavioral risk factor analysis of human papillomavirus infection in Uyghur women. Asian Pac J Cancer Prev 14:5861–5865
Woodman CB, Collins S, Winter H, Bailey A, Ellis J, Prior P, Yates M, Rollason TP, Young LS (2001) Natural history of cervical human papillomavirus infection in young women: a longitudinal cohort study. Lancet 357:1831–1836
Yang L, Li N, Guo LW, Li Q, Cui H, Dai M (2013) Prevalence of human papilloma virus and analysis of it’s risk factors in Daqing city, Heilongjiang province in 2010. Chin J Prev Med 47:118–123
Zhang B, Zhou AF, Zhu CC, Zhang L, Xiang B, Chen Z, Hu RH, Zhang YQ, Qiu L, Zhang YM, Xiong CD, Du YK, Shi YQ (2013) Risk factors for cervical cancer in rural areas of Wuhan china: a matched case-control study. Asian Pac J Cancer Prev 14:7595–7600
Acknowledgments
This research was supported by grants from the research project of the People’s Hospital of Xinjiang Uygur Autonomous Region, “The study on the risk factors of high-risk HPV persistent infection in Uygur women” (20140203).
Authors’ contributions
MN, SS and LW conceived of the study, participated in its design and coordination and helped to collect data and do statistical analysis as well as draft the manuscript. KCZ, ZJ and PL participated in the collection of clinical and experimental data and performed the statistical analysis and drafting of the manuscript as well as the manuscript review and final calibration. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors indicated no potential conflicts of interest.
Additional information
Shuang Sui and Mayineur Niyazi1 are the co-first authors
Rights and permissions
About this article
Cite this article
Sui, S., Niyazi, M., Wang, L. et al. A nested case-control study on type-specific persistent HPV infection in Uyghur women. J Public Health 24, 245–251 (2016). https://doi.org/10.1007/s10389-016-0720-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-016-0720-0