Abstract
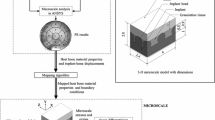
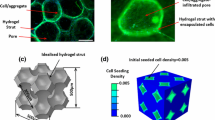
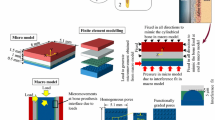
Bone ingrowth into a porous surface is one of the primary methods for fixation of orthopaedic implants. Improved understanding of bone formation and fixation of these devices should improve their performance and longevity. In this study predictions of bone ingrowth into an implant porous coating were investigated using mechano-reculatory models. The mechano-regulatory tissue differentiation algorithm proposed by Lacroix et al., and a modified version that enforces a tissue differentiation pathway by transitioning from differentiation to bone adaptation were investigated. The modified algorithm resulted in nearly the same behavior as the original algorithm when applied to a fracture-healing model. The algorithms were further compared using micromechanical finite element model of a beaded porous scaffold. Predictions of bone and fibrous tissue formation were compared between the two algorithms and to clinically observed phenomena. Under loading conditions corresponding to a press-fit hip stem, the modified algorithm predicted bone ingrowth into approximately 25% of the pore space, which is similar to that reported in experimental studies, while the original algorithm was unstable. When micromotion at the bone-implant interface was simulated, 20 μm of transverse displacement resulted in soft tissue formation at the bone-implant interface and minimal bone ingrowth. In contrast, 10 and 5 μm of micromotion resulted in bone filling 40% of the pore space and a stable interface, again consistent with clinical and experimental observations.
Similar content being viewed by others
References
Andreykiv A, Prendergast PJ, van Keulen F, Swieszkowski W, Rozing PM (2005) Bone ingrowth simulation for a concept glenoid component design. J Biomech 38:1023–033
Beaupre GS, Orr TE, Carter DR (1990) An approach for time- dependent bone modeling and remodeling–theoretical development. J Orthop Res 8:651–61
Beck JD, Canfield BL, Haddock SM, Chen TJH, Kothari M, Keaveny TM (1997) Three-dimensional imaging of trabecular bone using the Computer Numerically Controlled Milling technique. Bone 21:281–87
Burke DW, Bragdon CR, O’Connor DO, Jasty M, Harris WH (1993) Dynamic measurement of interface mechanics in-vivo and the effect of micromotions on bone in-growth into a porous surface device under controlled loads in-vivo. In: 39th Orthop Res Soc, Chicago
Carter DR, Hayes WC (1976) Bone compressive strength: the influence of density and strain rate. Science 194:1174–176
Carter DR, Blenman PR, Beaupre GS (1988) Correlations between mechanical stress history and tissue differentiation in initial fracture healing. J Orthop Res 6:736–48
Claes LE, Heigele CA (1999) Magnitudes of local stress and strain along bony surfaces predict the course and type of fracture healing. J Biomech 32:255–66
Claes LE, Heigele CA, Neidlinger-Wilke C, Kaspar D, Seidl W, Margevicius KJ, Augat P (1998) Effects of mechanical factors on the fracture healing process. Clin Orthop Relat Res S132–S147
Fischer KJ, Jacobs CR, Levenston ME, Carter DR (1996) Different loads can produce similar bone density distributions. Bone 19:127–35
Frost HM (1987) Bone “mass” and the “mechanostat” a proposal. Anat Rec 219:1–
Gardner TN, Stoll T, Marks L, Mishra S, Knothe Tate M (2000) The influence of mechanical stimulus on the pattern of tissue differentiation in a long bone fracture—an FEM study. J Biomech 33:415–25
Hernandez CJ, Beaupre GS, Keller TS, Carter DR (2001) The influence of bone volume fraction and ash fraction on bone strength and modulus. Bone 29:74–8
Huiskes R, Weinans H, Grootenboer HJ, Dalstra M, Fudala B, Slooff TJ (1987) Adaptive bone-remodeling theory applied to prosthetic-design analysis. J Biomech 20:1135–150
Huiskes R, Weinans H, Dalstra M (1989) Adaptive bone remodeling and biomechanical design considerations for noncemented total hip arthroplasty. Orthopedics 12:1255–267
Huiskes R, Weinans H, van Rietbergen B (1992) The relationship between stress shielding and bone resorption around total hip stems and the effects of flexible materials. Clin Orthop 274:124–34
Huiskes R, Driel WD, Prendergast PJ, SOballe K (1997) A biomechanical regulatory model for periprosthetic fibrous-tissue differentiation. J Mater Sci Mater Med 8:785–88
Isaksson H, van Donkelaar CC, Huiskes R, Ito K (2006a) Corroboration of mechanoregulatory algorithms for tissue differentiation during fracture healing: Comparison with in vivo results. J Orthop Res 24:898–07
Isaksson H, Wilson W, van Donkelaar CC, Huiskes R, Ito K (2006b) Comparison of biophysical stimuli for mechano-regulation of tissue differentiation during fracture healing. J Biomech 39:1507–516
Keaveny TM, Bartel DL (1994) Fundamental load transfer patterns for press-fit, surface-treated intramedullary fixation stems. J Biomech 27:1147–157
Kelly DJ, Prendergast PJ (2004) Effect of a degraded core on the mechanical behaviour of tissue-engineered cartilage constructs: a poro-elastic finite element analysis. Med Biol Eng Comput 42:9–3
Kelly DJ, Prendergast PJ (2005) Mechano-regulation of stem cell differentiation and tissue regeneration in osteochondral defects. J Biomech 38:1413–422
Kienapfel H, Sprey C, Wilke A, Griss P (1999) Implant fixation by bone ingrowth. J Arthroplasty 14:355–68
Lacroix D, Prendergast PJ (2002) A mechano-regulation model for tissue differentiation during fracture healing: analysis of gap size and loading. J Biomech 35:1163–171
Lacroix D, Prendergast PJ, Li G, Marsh D (2002) Biomechanical model to simulate tissue differentiation and bone regeneration: application to fracture healing. Med Biol Eng Comput 40:14–1
Loboa EG, Wren TAL, Beaupre GS, Carter DR (2003) Mechanobiology of soft skeletal tissue differentiation–a computational approach of a fiber-reinforced poroelastic model based on homogeneous and isotropic simplifications. Biomech Model Mechanobiol 2:83–6
Prendergast PJ, Huiskes R, Soballe K (1997) Biophysical stimuli on cells during tissue differentiation at implant interfaces. J Biomech 30:539–48
Qin YX, McLeod KJ, Guilak F, Chiang FP, Rubin CT (1996) Correlation of bony ingrowth to the distribution of stress and strain parameters surrounding a porous-coated implant. J Orthop Res 14:862–70
Ramamurti BS, Orr TE, Bragdon CR, Lowenstein JD, Jasty M, Harris WH (1997) Factors influencing stability at the interface between a porous surface and cancellous bone: a finite element analysis of a canine in vivo micromotion experiment. J Biomed Mater Res 36:274–80
Ryd L, Albrektsson BE, Carlsson L, Dansgard F, Herberts P, Lindstrand A, Regner L, Toksvig-Larsen S (1995) Roentgen stereophotogrammetric analysis as a predictor of mechanical loosening of knee prostheses. J Bone Joint Surg BR 77:377–83
Spears IR, Pfleiderer M, Schneider E, Hille E, Bergmann G, Morlock MM (2000) Interfacial conditions between a press-fit acetabular cup and bone during daily activities: implications for achieving bone in-growth. J Biomech 33:1471–477
Spector M (1982) Bone ingrowth into porous polymers. In: Williams DF (ed) Biocompatibility of orthopedic implants. CRC Press, Inc., Boca Raton
Sumner DR, Turner TM, Urban RM, Galante JO (1992) Remodeling and ingrowth of bone at two years in a canine cementless total hip-arthroplasty model. J Bone Joint Surg AM 74:239–50
Szmukler-Moncler S, Salama H, Reingewirtz Y, Dubruille JH (1998) Timing of loading and effect of micromotion on bone-dental implant interface: review of experimental literature. J Biomed Mater Res 43:192–03
Tuan RS (2004) Biology of developmental and regenerative skeletogenesis. Clin Orthop Relat Res (427 Suppl):S105–17
Weinans H, Huiskes R, Grootenboer HJ (1992) Effects of material properties of femoral hip components on bone remodeling. J Orthop Res 10:845–53
Wren TA, Beaupre GS, Carter DR (2000) Mechanobiology of tendon adaptation to compressive loading through fibrocartilaginous metaplasia. J Rehabil R D 37:135–43
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, X., Niebur, G.L. Bone ingrowth into a porous coated implant predicted by a mechano-regulatory tissue differentiation algorithm. Biomech Model Mechanobiol 7, 335–344 (2008). https://doi.org/10.1007/s10237-007-0100-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10237-007-0100-3