Abstract
Background
Application of the Milan criteria is an effective strategy to select patients with hepatocellular carcinoma (HCC) for liver transplantation, but HCC recurrence is still a major concern. The aim of this study was to determine whether interleukin 6 (IL6) polymorphisms and clinical variables are potential predictors for HCC recurrence and prognosis after transplantation.
Methods
A total of 110 consecutive patients with HCC undergoing liver transplantation were enrolled in the study. Six tag single nucleotide polymorphisms in IL6 were genotyped in both the donors and recipients. Demographic characteristics, HCC features, and IL6 polymorphisms were assessed against HCC recurrence.
Results
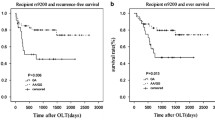
Pretransplant hepatitis B virus DNA (P = 0.014), pretransplant serum alpha-fetoprotein (P = 0.035), number of nodules (P = 0.011), diameter of main nodule (P = 0.001), macrovascular invasion (P = 0.001), microvascular invasion (P = 0.001), HCC exceeding the Milan criteria (P < 0.001), and donor rs2069852 AA genotype (P = 0.010) were associated with HCC recurrence. Recurrence-free survival rate and overall survival rate were significantly lower (P = 0.011 and P = 0.026, respectively) in patients whose donor had the rs2069852 AA genotype than in those whose donor had the AG and GG genotypes. Independent risk factors for recurrence-free survival and overall survival were microvascular invasion (P = 0.003; P = 0.002), HCC exceeding the Milan criteria (P < 0.001; P = 0.001), and donor rs2069852 AA genotype (P = 0.002; P = 0.010).
Conclusions
Our data suggest that donor IL6 rs2069852 polymorphisms may be a potential genetic marker for HCC recurrence after liver transplantation in the Han Chinese population.


Similar content being viewed by others
References
Lafaro KJ, Demirjian AN, Pawlik TM (2015) Epidemiology of hepatocellular carcinoma. Surg Oncol Clin N Am 24:1–17
Zimmerman MA, Ghobrial RM, Tong MJ et al (2008) Recurrence of hepatocellular carcinoma following liver transplantation: a review of preoperative and postoperative prognostic indicators. Arch Surg 143:182–188
Fong ZV, Tanabe KK (2014) The clinical management of hepatocellular carcinoma in the United States, Europe, and Asia: a comprehensive and evidence-based comparison and review. Cancer 120:2824–2838
Bruix J, Gores GJ, Mazzaferro V (2014) Hepatocellular carcinoma: clinical frontiers and perspectives. Gut 63:844–855
Lai Q, Avolio AW, Lerut J et al (2012) Recurrence of hepatocellular cancer after liver transplantation: the role of primary resection and salvage transplantation in East and West. J Hepatol 57:974–979
Rodriguez-Peralvarez M, Tsochatzis E, Naveas MC et al (2013) Reduced exposure to calcineurin inhibitors early after liver transplantation prevents recurrence of hepatocellular carcinoma. J Hepatol 59:1193–1199
Welker MW, Bechstein WO, Zeuzem S et al (2013) Recurrent hepatocellular carcinoma after liver transplantation—an emerging clinical challenge. Transpl Int 26:109–118
Zheng Z, Gao S, Yang Z et al (2014) Single nucleotide polymorphisms in the metastasis-associated in colon cancer-1 gene predict the recurrence of hepatocellular carcinoma after transplantation. Int J Med Sci 11:142–150
Dickmann LJ, Patel SK, Rock DA et al (2011) Effects of interleukin-6 (IL-6) and an anti-IL-6 monoclonal antibody on drug-metabolizing enzymes in human hepatocyte culture. Drug Metab Dispos 39:1415–1422
Yao J, Feng XW, Yu XB et al (2013) Recipient IL-6-572C/G genotype is associated with reduced incidence of acute rejection following liver transplantation. J Int Med Res 41:356–364
Taub R (2004) Liver regeneration: from myth to mechanism. Nat Rev Mol Cell Biol 5:836–847
Ohishi W, Cologne JB, Fujiwara S et al (2014) Serum interleukin-6 associated with hepatocellular carcinoma risk: a nested case-control study. Int J Cancer 134:154–163
Liu Y, Gao SJ, Du BX et al (2014) Association of IL-6 polymorphisms with hepatocellular carcinoma risk: evidences from a meta-analysis. Tumour Biol 35:3551–3561
Falleti E, Fabris C, Toniutto P et al (2009) Interleukin-6 polymorphisms and gender: relationship with the occurrence of hepatocellular carcinoma in patients with end-stage liver disease. Oncology 77:304–313
Fan J, Yang GS, Fu ZR et al (2009) Liver transplantation outcomes in 1,078 hepatocellular carcinoma patients: a multi-center experience in Shanghai, China. J Cancer Res Clin Oncol 135:1403–1412
Mazzaferro V, Regalia E, Doci R et al (1996) Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 334:693–699
Lai Q, Lerut JP (2014) Hepatocellular cancer: how to expand safely inclusion criteria for liver transplantation. Curr Opin Organ Transplant 19:229–234
Takada Y, Tohyama T, Watanabe J (2015) Biological markers of hepatocellular carcinoma for use as selection criteria in liver transplantation. J Hepato Biliary Pancreat Sci 22:279–286
Yao FY, Ferrell L, Bass NM et al (2001) Liver transplantation for hepatocellular carcinoma: expansion of the tumor size limits does not adversely impact survival. Hepatology 33:1394–1403
DuBay D, Sandroussi C, Sandhu L et al (2011) Liver transplantation for advanced hepatocellular carcinoma using poor tumor differentiation on biopsy as an exclusion criterion. Ann Surg 253:166–172
Clavien PA, Lesurtel M, Bossuyt PM et al (2012) Recommendations for liver transplantation for hepatocellular carcinoma: an international consensus conference report. Lancet Oncol 13:e11–e22
Li MR, Chen GH, Cai CJ et al (2011) High hepatitis B virus DNA level in serum before liver transplantation increases the risk of hepatocellular carcinoma recurrence. Digestion 84:134–141
Han SH, Reddy KR, Keeffe EB et al (2011) Clinical outcomes of liver transplantation for HBV-related hepatocellular carcinoma: data from the NIH HBV OLT study. Clin Transplant 25:E152–E162
Fitzmorris P, Shoreibah M, Anand BS et al (2015) Management of hepatocellular carcinoma. J Cancer Res Clin Oncol 141:861–876
Duvoux C, Roudot-Thoraval F, Decaens T et al (2012) Liver transplantation for hepatocellular carcinoma: a model including alpha-fetoprotein improves the performance of Milan criteria. Gastroenterology 143:986–994 (e983; quiz e914–985)
Iguchi T, Shirabe K, Aishima S et al (2015) New pathologic stratification of microvascular invasion in hepatocellular carcinoma: predicting prognosis after living-donor liver transplantation. Transplantation 99:1236–1242
Rodriguez-Peralvarez M, Luong TV, Andreana L et al (2013) A systematic review of microvascular invasion in hepatocellular carcinoma: diagnostic and prognostic variability. Ann Surg Oncol 20:325–339
Suo GJ, Zhao ZX (2013) Association of the interleukin-28B gene polymorphism with development of hepatitis virus-related hepatocellular carcinoma and liver cirrhosis: a meta-analysis. Genet Mol Res 12:3708–3717
Wei YG, Liu F, Li B et al (2011) Interleukin-10 gene polymorphisms and hepatocellular carcinoma susceptibility: a meta-analysis. World J Gastroenterol 17:3941–3947
Wei Y, Liu F, Li B et al (2011) Polymorphisms of tumor necrosis factor-alpha and hepatocellular carcinoma risk: a HuGE systematic review and meta-analysis. Dig Dis Sci 56:2227–2236
Li S, Deng Y, Chen ZP et al (2011) Genetic polymorphism of interleukin-16 influences susceptibility to HBV-related hepatocellular carcinoma in a Chinese population. Infect Genet Evol 11:2083–2088
Taki-Eldin A, Zhou L, Xie HY et al (2012) Liver regeneration after liver transplantation. Eur Surg Res 48:139–153
Johnson C, Han Y, Hughart N et al (2012) Interleukin-6 and its receptor, key players in hepatobiliary inflammation and cancer. Transl Gastrointest Cancer 1:58–70
Naugler WE, Sakurai T, Kim S et al (2007) Gender disparity in liver cancer due to sex differences in MyD88-dependent IL-6 production. Science 317:121–124
Karimi MH, Daneshmandi S, Pourfathollah AA et al (2011) Association of IL-6 promoter and IFN-gamma gene polymorphisms with acute rejection of liver transplantation. Mol Biol Rep 38:4437–4443
Zhang G, Zhou B, Wang W et al (2012) A functional single-nucleotide polymorphism in the promoter of the gene encoding interleukin 6 is associated with susceptibility to tuberculosis. J Infect Dis 205:1697–1704
Komatsu Y, Tai H, Galicia JC et al (2005) Interleukin-6 (IL-6)–373 A9T11 allele is associated with reduced susceptibility to chronic periodontitis in Japanese subjects and decreased serum IL-6 level. Tissue Antigens 65:110–114
Brull DJ, Montgomery HE, Sanders J et al (2001) Interleukin-6 gene −174 g > c and −572 g > c promoter polymorphisms are strong predictors of plasma interleukin-6 levels after coronary artery bypass surgery. Arterioscler Thromb Vasc Biol 21:1458–1463
Wu LM, Zhou L, Xu J et al (2013) Lack of association between genetic polymorphisms in cytokine genes and tumor recurrence in patients with hepatocellular carcinoma undergoing transplantation. Hepatobiliary Pancreat Dis Int 12:54–59
Norris CA, He M, Kang LI et al (2014) Synthesis of IL-6 by hepatocytes is a normal response to common hepatic stimuli. PLoS One 9:e96053
Zhang Y, Shi ZL, Yang X et al (2014) Targeting of circulating hepatocellular carcinoma cells to prevent postoperative recurrence and metastasis. World J Gastroenterol 20:142–147
Acknowledgments
This work was supported by the Scientific Research Project of Science and Technology Commission of Shanghai Municipality (No. 134119a6300).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
No author has any conflict of interest.
Ethics statement
Written informed consent forms were obtained from all donors and recipients. The study was approved by the Ethics Committee of Shanghai Jiao Tong University and was conducted strictly under the guidelines of the Declaration of Helsinki.
Additional information
D. Chen and S. Liu are contributed equally to this work.
About this article
Cite this article
Chen, D., Liu, S., Chen, S. et al. Donor interleukin 6 gene polymorphisms predict the recurrence of hepatocellular carcinoma after liver transplantation. Int J Clin Oncol 21, 1111–1119 (2016). https://doi.org/10.1007/s10147-016-1001-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-016-1001-1