Abstract
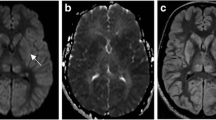
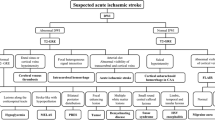
In the emergency setting, a regional area of restricted diffusion involving the basal ganglia typically represents an acute infarct due to small vessel occlusion. However, it is important to consider additional differentials, specifically systemic causes. This article will review anatomy of the basal ganglia and pertinent associated vasculature, followed by other entities that can be a cause of restricted diffusion. These include hemolytic uremic syndrome, hypereosinophilic syndrome, fat embolism, meningitis, and hypoxic-ischemic injury. It is important to recognize presenting findings in these conditions, as the radiologist may be the first to give an accurate diagnosis or prompt additional testing.








Similar content being viewed by others
References
Hegde AN et al (2011) Differential diagnosis for bilateral abnormalities of the basal ganglia and thalamus. Radiographics 31(1):5–30
Djulejić V et al (2016) Clinical significance of blood supply to the internal capsule and basal ganglia. J Clin Neurosci 25:19–26
Beltz EE, Mullins ME (2010) Radiological reasoning: hyperintensity of the basal ganglia and cortex on FLAIR and diffusion-weighted imaging. AJR 195(3):S1–S8
Kamalian S et al (2015) Stroke differential diagnosis and mimics: part 1. Appl Radiol 44(11):26–39
Bekiesinka-Figatowska M, Mierzewska H, Jurkiewicz E (2013) Basal ganglia lesions in children and adults. Eur J Radiol 82(5):837–849
Moake JL (2002) Thrombotic microangiopathies. NEJM 347(8):589–600
Wengenroth M et al (2013) Central nervous system involvement in adults with epidemic hemolytic uremic syndrome. AJNR Am J Neuroradiol 34(5):1016–1021
Yu WL et al (2015) Thrombotic thrombocytopenic pupura with concomitant small- and large-vessel thrombosis, atypical posterior reversible encephalopathy syndrome and cerebral microbleeds. Oxf Med Case Reports 2:179–182
Steinborn M et al (2004) CT and MRI in haemolytic uraemic syndrome with central nervous system involvement: distribution of lesions and prognostic value of imaging findings. Pediatr Radiol 34(10):805–810
Burrus TM, Wijdicks EF, Rabinstein AA (2009) Brain lesions are most often reversible in acute thrombotic thrombocytopenic purpura. Neurology 73(1):66–70
Kim GB, Kwon JH, Kang DS (1993) Hypereosinophilic syndrome: imaging findings in patients with hepatic involvement. AJR 161(3):577–580
Roufosse FE, Goldman M, Cogan E (2007) Hypereosinophilic syndromes. Orphanet J Rare Dis 2:37
Lee EJ et al (2009) Hypereosinophilia with multiple thromboembolic cerebral infracts and focal intracerebral hemorrhage. Korean J Radiol 10(5):511–514
Sethi HS, Schmidley JW (2010) Cerebral infarcts in the setting of eosinophilia: three cases and a discussion. Arch Neurol 67(10):1275–1277
Noureen N, Rana MT (2008) Hypereosinophilic syndrome causing acute hemiplegia in childhood. J Coll Physicians Surg Pak 18(6):384–385
Ishii J et al (2015) Multiple cerebral infarctions in a patient with hypereosinophilic syndrome with Lӧffler endocarditis: a case report. Rinsho Shinkeigaku 55(3):175–170
Simon AD, Ulmer JL, Strottmann JM, Contrast-Enhanced MR (2003) Imaging of cerebral fat embolism: case report and review of the literature. AJNR Am J Neuroradiol 24(1):97–101
Gupta B et al (2011) Cerebral fat embolism: a diagnostic challenge. Saudi J Anaesth 5(3):348–352
Zhou Y et al (2015) Pathogenesis, diagnosis and treatment of cerebral fat embolism. Chin J Traumatol 18(2):120–123
Kamenar E, Burger PC (1980) Cerebral fat embolism: a neuropathological study of a microembolic state. Stroke 11(5):477–484
Zaitsu et al (2010) Susceptibility-weighted imaging of cerebral fat embolism. J Comput Assist Tomogr 34(1):107–112
Ahluwalia VV et al (2013) MRI spectrum of CNS tuberculosis. JIACM 14(1):83–90
Mitchell BC, Dehkharghani S (2014) Imaging of intracranial infectious disease in adults. Appl Radiol 43(2):6–15
Huang BY, Castillo M (2008) Hypoxic-ischemic brain injury: imaging findings from birth to adulthood. Radiographics 28(2):417–439
Bathla G, Hegde AN (2013) MRI and CT appearances in metabolic encephalopathies due to systemic diseases in adults. Clin Radiol 68(6):545–554
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Bhatt, A.A., Brucker, J.L. & Almast, J. Beyond stroke—uncommon causes of diffusion restriction in the basal ganglia. Emerg Radiol 25, 87–92 (2018). https://doi.org/10.1007/s10140-017-1550-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-017-1550-2