Abstract
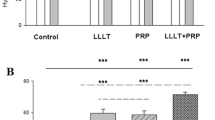
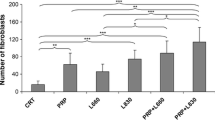
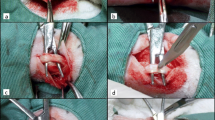
The objective of this study was to investigate the effects of low-level laser therapy (LLLT) treatment alone (λ = 660 nm and λ = 830 nm) or associated with platelet-rich plasma (PRP). We used 54 male rats divided into six groups, with nine animals each: group 1, partial tenotomy; group 2 (GII), PRP; group 3 (GIII): λ660 nm; group 4 (GIV), λ830 nm; group 5 (GV), PRP + λ660 nm; and group 6 (GVI), PRP + λ830 nm. The protocol used was power density 0.35 W/cm2, energy 0.2 J, energy density 7.0 J/cm2, time 20 s per irradiated point, and number of points 3. Animals in groups GII, GV, and GVI received treatment with PRP, consisting of a single dose of 0.2 mL directly into the surgical site, on top of the tenotomy. Animals were killed on the 13th day post-tenotomy and their tendons were surgically removed for a quantitative analysis using polarization microscopy. The percentages of collagen fibers of types I and III were expressed as mean ± SD. Higher values of collagen fibers type I were obtained for groups GV and GVI when compared with all other groups (p < 0.05), whereas groups GIII and GIV showed no significant difference between them (p > 0.05). For collagen type III, a significant difference was observed between GII and all other groups (p < 0.5), but no significant difference was found between GIII and GIV and between GV and GVI. Results showed that the deposition of collagen type I was higher when treatment with PRP and LLLT was combined, suggesting a faster regeneration of the tendon.



Similar content being viewed by others
References
Longo UG, Ronga M, Maffulli N (2009) Achilles tendinopathy. Sports Med Arthrosc Rev 17(2):112–126
Sharma P, Maffulli N (2005) Tendon injury and tendinopathy: healing and repair. J Bone Joint Surg Am 87:187–202
Liu SH, Yang RS, Al-Shaikh R, Lane JM (1995) Collagen in tendon, ligament, and bone healing. A current review. Clin Orthop 318:265–278
Chen CH, Tsai JL, Wang YH, Lee CL, Chen JK, Huang MH (2009) Low-level laser irradiation promotes cell proliferation and mRNA expression of type I collagen and decorin in porcine Achilles tendon fibroblasts in vitro. J Orthop Res 27:646–650
Casalechi HL, Leal-Junior EC, Xavier M, Silva JA Jr, de Carvalho PD, Aimbire F, Albertini R (2012) Low-level laser therapy in experimental model of collagenase-induced tendinitis in rats: effects in acute and chronic inflammatory phases. Lasers Med Sci. doi:10.1007/s10103-012-1189-x
Pires D, Xavier M, Araújo T, Silva JA Jr, Aimbire F, Albertini R (2011) Low-level laser therapy (LLLT; 780 nm) acts differently on mRNA expression of anti- and pro-inflammatory mediators in an experimental model of collagenase-induced tendinitis in rat. Lasers Med Sci 26:85–94
Neves MA, Pinfildi CE, Wood VT, Gobbato RC, da Silva FM, Parizotto NA, Hochman B, Ferreira LM (2011) Different power settings of LLLT on the repair of the calcaneal tendon. Photomed Laser Surg 29(10):663–668
Joensen J, Gjerdet NR, Hummelsund S, Iversen V, Lopes-Martins RA, Bjordal JM (2012) An experimental study of low-level laser therapy in rat Achilles tendon injury. Lasers Med Sci 27(1):103–111
Carrinho PM, Renno AC, Koeke P, Salate AC, Parizotto NA, Vidal BC (2006) Comparative study using 685-nm and 830-nm lasers in the tissue repair of tenotomized tendons in the mouse. Photomed Laser Surg 24(6):754–758
Oliveira FS, Pinfildi CE, Parizoto NA, Liebano RE, Bossini PS, Garcia EB, Ferreira LM (2009) Effect of low level laser therapy (830 nm) with different therapy regimes on the process of tissue repair in partial lesion calcaneous tendon. Lasers Surg Med 41(4):271–276
Elwakil TF (2007) An in-vivo experimental evaluation of He-Ne laser photostimulation in healing Achilles tendons. Lasers Med Sci 22(1):53–59
Demir H, Menku P, Kirnap M, Calis M, Ikizceli I (2004) Comparison of the effects of laser, ultrasound, and combined laser + ultrasound treatments in experimental tendon healing. Lasers Surg Med 35(1):84–89
Wang X, Qiu Y, Triffitt J, Carr A, Xia Z, Sabokbar A (2012) Proliferation and differentiation of human tenocytes in response to platelet rich plasma: an in vitro and in vivo study. J Orthop Res 30(6):982–990
de Mos M, van der Windt AE, Jahr H et al (2008) Can platelet-rich plasma enhance tendon repair? A cell culture study. Am J Sports Med 36:1171–1178
Monto RR (2012) Platelet rich plasma treatment for chronic Achilles tendinosis. Foot Ankle Int 33(5):379–385
Xiong X, Wu L, Xiang D, Ni G, Zhao P, Yu B (2012) Effect of platelet-rich plasma injection on early healing of Achilles tendon rupture in rats. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 26(4):466–471
Del Buono A, Papalia R, Denaro V, Maccauro G, Maffulli N (2011) Platelet rich plasma and tendinopathy: state of the art. Int J Immunopathol Pharmacol 24(1 Suppl 2):79–83
Taylor DW, Petrera M, Hendry M, Theodoropoulos JS (2011) A systematic review of the use of platelet-rich plasma in sports medicine as a new treatment for tendon and ligament injuries. Clin J Sport Med 21(4):344–352
Geng Z, Wang C, Zhou H (2011) Effect of platelet-rich plasma on tendon healing. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi 25(3):344–348
Paoloni J, De Vos RJ, Hamilton B, Murrell GA, Orchard J (2011) Platelet-rich plasma treatment for ligament and tendon injuries. Clin J Sport Med 21(1):37–45
Jo CH, Kim JE, Yoon KS, Shin S (2012) Platelet-rich plasma stimulates cell proliferation and enhances matrix gene expression and synthesis in tenocytes from human rotator cuff tendons with degenerative tears. Am J Sports Med 40(5):1035–1045
Tohidnezhad M, Varoga D, Wruck CJ, Brandenburg LO, Seekamp A, Shakibaei M, Sönmez TT, Pufe T, Lippross S. Platelet-released growth factors can accelerate tenocyte proliferation and activate the anti-oxidant response element. 2011; 135(5):453-460
Froum SJ, Wallace SS, Tarnow DP, Chao SC (2002) Effect of platelet-rich plasma on bone growth and osseointegration in human maxillary sinus grafts: three bilateral case reports. Int J Periodontics Restor Dent 22(1):45–53
Carmona JU (2006) Use of autologous platelet concentrates for the treatment of musculoskeletal injuries in the horse. 91 f. Tesis (Doctorado en Medicina y Sanidad Animales) - Universitat Autònoma de Barcelona
Schnabel LV, Mohammed HO, Miller BJ, McDermott WG, Jacobson MS, Santangelo KS, Fortier LA (2007) Platelet rich plasma (PRP) enhanced anabolic gene expression patterns in flexor digitorum superficialis tendons. J Orthop Res 25(2):230–240
Silva RD, Glazebrook MA, Campos VC (2011) Vasconcelos AC Achilles tendinosis: a morphometrical study in a rat model. Int J Clin Exp Pathol 4(7):683–691
Aspenberg P, Virchenko O (2004) Platelet concentrate injection improves Achilles tendon repair in rats. Acta Orthop Scand 75(1):93–99
Barbosa D, de Souza RA, Xavier M, da Silva FF, Arisawa EA, Villaverde AG (2012) Effects of low-level laser therapy (LLLT) on bone repair in rats: optical densitometry analysis. Lasers Med Sci. doi:10.1007/s10103-012-1125-0
Silva RD (2008) Modelo experimental de indução à tendinose de Aquiles: Um estudo morfométrico [Dissertação] Belo Horizonte: Faculdade de Medicina de Minas Gerais (MG): Universidade Federal de Minas Gerais - UFMG
Debus ES, Schmidt K, Ziegler UE, Thiede A (2000) The role of growth factors in wound healing. Zentralbl Chir 125(Suppl 1):49–55
Shanaman R, Filtein MR, Danesh MMJ (2001) Localized ridge augmentation using GBR and platelet-rich plasma: case reports. Int J Periodontics Restor Dent 21(4):345–355
Bihari J, Mester AR (1997) The biostimulative effect of low level laser therapy on long standing crural ulcers using helium-neon laser, helium-neon laser plus infrared lasers, and noncoherent light: preliminary report of a randomized double blind comparative study. Laser Ther 11(2):11–18
Dugrillon A, Kluter H (2002) Current use of platelet concentrates for topical application in tissue repair. Ther Transfus Med 29(23):67–70
Junqueira LCU, Cossermerlli R (1978) Brentani. Differential staining of collagens type I, II and III by Sirius Red and polarization microscopy. Arch Histol Jpn 41(3):267–274
Hock JM, Canalis E (1994) Platelet-derived growth factor enhances bone cell replication, but not differentiated function of osteoblasts. Endocrinology 134(3):1423–1428
Karu T (1998) The science of low power laser therapy. Gordon and Breach Science Publishers, Australia, pp 23–29
Reddy G, Gum S, Stehno B, Enwemeka C (1998) Biochemistry and biomechanics of healing tendon: part II. Effects of combined laser therapy and electrical stimulation. Med Sci Sports Exerc 30(6):794–800
Wood VT, Pinfildi CE, Neves MA, Parizoto NA, Hochman B, Ferreira LM (2010) Collagen changes and realignment induced by low-level laser therapy and low-intensity ultrasound in the calcaneal tendon. Lasers Surg Med 42(6):559–565
Acknowledgments
We thank the Instituto de Ciências Biomédicas, Universidade de São Paulo, for the technical and laboratory assistance related to histological analysis.
Conflict of interest
No competing financial interests exist.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Barbosa, D., de Souza, R.A., de Carvalho, W.R.G. et al. Low-level laser therapy combined with platelet-rich plasma on the healing calcaneal tendon: a histological study in a rat model. Lasers Med Sci 28, 1489–1494 (2013). https://doi.org/10.1007/s10103-012-1241-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-012-1241-x