Abstract
Objective
The aim of this study was to evaluate and compare early postoperative discomfort and wound healing outcomes between patients who underwent periodontal surgery with and without enamel matrix derivative (EMD), using retrospective questionnaires and postoperative clinical examinations.
Materials and methods
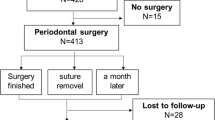
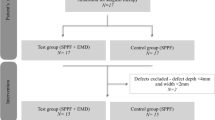
All enrolled patients filled out the self-report questionnaire after suture removal. The severity and duration of subjective pain and swelling were evaluated using visual analog scale (VAS) scores and wound healing parameters (dehiscence/fenestration, spontaneous bleeding, persistent swelling, and ulceration). Chi-squared tests, two-tailed independent t tests, analysis of variance, and multiple logistic regression analysis were performed to identify significant differences between the two groups (surgery with EMD and surgery without EMD).
Results
The severity of pain and swelling did not differ between patients who underwent surgery with and without EMD, but the durations of pain (P < 0.001) and swelling (P = 0.019) were significantly lower in patients who underwent surgery with EMD. Multivariate analysis with adjustment for confounding variables showed that wound healing outcomes including dehiscence/fenestration, spontaneous bleeding, and ulceration did not differ significantly between the two groups, and only persistent swelling showed significant differences (odds ratio 4.03, 95% CI 1.17–13.78; P = 0.026).
Conclusions
No difference was observed in the severity of early postoperative discomfort and wound healing outcomes between patients who underwent surgery with and without EMD, but shorter durations of postoperative pain and swelling were evident in patients who underwent surgery with EMD.
Clinical relevance
Adjunctive EMD used in periodontal surgery has clinical advantages for reducing the durations of postoperative pain and swelling.



Similar content being viewed by others
References
Fardal O, McCulloch CA (2012) Impact of anxiety on pain perception associated with periodontal and implant surgery in a private practice. J Periodontol 83:1079–1085. https://doi.org/10.1902/jop.2011.110562
Kim S, Lee YJ, Lee S, Moon HS, Chung MK (2013) Assessment of pain and anxiety following surgical placement of dental implants. Int J Oral Maxillofac Implants 28:531–535. https://doi.org/10.11607/jomi.2713
Griffin TJ, Cheung WS, Zavras AI, Damoulis PD (2006) Postoperative complications following gingival augmentation procedures. J Periodontol 77:2070–2079. https://doi.org/10.1902/jop.2006.050296
Weisensee W, Scheer M, Muller L, Rothamel D, Kistler F, Bayer G et al (2012) Impact of anxiety parameters on prospective and experienced pain intensity in implant surgery. Implant Dent 21:502–506. https://doi.org/10.1097/ID.0b013e3182703a44
Mei CC, Lee FY, Yeh HC (2016) Assessment of pain perception following periodontal and implant surgeries. J Clin Periodontol 43:1151–1159. https://doi.org/10.1111/jcpe.12618
Oswal S, Ravindra S, Sinha A, Manjunath S (2014) Antibiotics in periodontal surgeries: a prospective randomised cross over clinical trial. J Indian Soc Periodontol 18:570–574. https://doi.org/10.4103/0972-124X.142443
Lee JH, Lee JS, Park JY, Choi JK, Kim DW, Kim YT, Choi SH (2015) Association of lifestyle-related comorbidities with periodontitis: a Nationwide cohort study in Korea. Medicine (Baltimore) 94:e1567. https://doi.org/10.1097/MD.0000000000001567
Lee JH, Oh JY, Youk TM, Jeong SN, Kim YT, Choi SH (2017) Association between periodontal disease and non-communicable diseases: a 12-year longitudinal health-examinee cohort study in South Korea. Medicine (Baltimore) 96:e7398. https://doi.org/10.1097/MD.0000000000007398
Lee JH, Choi JK, Jeong SN, Choi SH (2018) Charlson comorbidity index as a predictor of periodontal disease in elderly participants. J Periodontal Implant Sci 48:92–102. https://doi.org/10.5051/jpis.2018.48.2.92
Smiley CJ, Tracy SL, Abt E, Michalowicz BS, John MT, Gunsolley J, Cobb CM, Rossmann J, Harrel SK, Forrest JL, Hujoel PP, Noraian KW, Greenwell H, Frantsve-Hawley J, Estrich C, Hanson N (2015) Systematic review and meta-analysis on the nonsurgical treatment of chronic periodontitis by means of scaling and root planning with or without adjuncts. J Am Dent Assoc 146:508–524 e505. https://doi.org/10.1016/j.adaj.2015.01.028
Eli I, Schwartz-Arad D, Baht R, Ben-Tuvim H (2003) Effect of anxiety on the experience of pain in implant insertion. Clin Oral Implants Res 14:115–118
Cortellini P, Tonetti MS (2009) Improved wound stability with a modified minimally invasive surgical technique in the regenerative treatment of isolated interdental intrabony defects. J Clin Periodontol 36:157–163. https://doi.org/10.1111/j.1600-051X.2008.01352.x
Cortellini P (2012) Minimally invasive surgical techniques in periodontal regeneration. J Evid Based Dent Pract 12:89–100. https://doi.org/10.1016/S1532-3382(12)70021-0
Heden G, Wennstrom JL (2006) Five-year follow-up of regenerative periodontal therapy with enamel matrix derivative at sites with angular bone defects. J Periodontol 77:295–301. https://doi.org/10.1902/jop.2006.050071
Sculean A, Chiantella GC, Arweiler NB, Becker J, Schwarz F, Stavropoulos A (2008) Five-year clinical and histologic results following treatment of human intrabony defects with an enamel matrix derivative combined with a natural bone mineral. Int J Periodontics Restorative Dent 28:153–161
Izumi Y, Aoki A, Yamada Y, Kobayashi H, Iwata T, Akizuki T, Suda T, Nakamura S, Wara-Aswapati N, Ueda M, Ishikawa I (2011) Current and future periodontal tissue engineering. Periodontol 56:166–187. https://doi.org/10.1111/j.1600-0757.2010.00366.x
Miron RJ, Sculean A, Cochran DL, Froum S, Zucchelli G, Nemcovsky C, Donos N, Lyngstadaas SP, Deschner J, Dard M, Stavropoulos A, Zhang Y, Trombelli L, Kasaj A, Shirakata Y, Cortellini P, Tonetti M, Rasperini G, Jepsen S, Bosshardt DD (2016) Twenty years of enamel matrix derivative: the past, the present and the future. J Clin Periodontol 43:668–683. https://doi.org/10.1111/jcpe.12546
Bosshardt DD (2008) Biological mediators and periodontal regeneration: a review of enamel matrix proteins at the cellular and molecular levels. J Clin Periodontol 35:87–105. https://doi.org/10.1111/j.1600-051X.2008.01264.x
Isehed C, Svenson B, Lundberg P, Holmlund A (2018) Surgical treatment of peri-implantitis using enamel matrix derivative, an RCT: 3- and 5-year follow-up. J Clin Periodontol 45:744–753. https://doi.org/10.1111/jcpe.12894
Wennstrom JL, Lindhe J (2002) Some effects of enamel matrix proteins on wound healing in the dento-gingival region. J Clin Periodontol 29:9–14
Tonetti MS, Fourmousis I, Suvan J, Cortellini P, Bragger U, Lang NP, on behalf of the European Research Group on Periodontology (ERGOPERIO) (2004) Healing, post-operative morbidity and patient perception of outcomes following regenerative therapy of deep intrabony defects. J Clin Periodontol 31:1092–1098. https://doi.org/10.1111/j.1600-051X.2004.00615.x
Morris K (2013) Revising the Declaration of Helsinki. Lancet 381:1889–1890
Faul F, Erdfelder E, Lang AG, Buchner A (2007) G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods 39:175–191
Rincon JC, Haase HR, Bartold PM (2003) Effect of Emdogain on human periodontal fibroblasts in an in vitro wound-healing model. J Periodontal Res 38:290–295
Tonnesen MG, Feng X, Clark RA (2000) Angiogenesis in wound healing. J Investig Dermatol Symp Proc 5:40–46. https://doi.org/10.1046/j.1087-0024.2000.00014.x
Folkman J, Shing Y (1992) Angiogenesis. J Biol Chem 267:10931–10934
Burkhardt R, Hammerle CH, Lang NP, Research Group on Oral Soft Tissue B, Wound H (2015) Self-reported pain perception of patients after mucosal graft harvesting in the palatal area. J Clin Periodontol 42:281–287. https://doi.org/10.1111/jcpe.12357
Weisel JW (2007) Structure of fibrin: impact on clot stability. J Thromb Haemost 5(Suppl 1):116–124. https://doi.org/10.1111/j.1538-7836.2007.02504.x
Canakci CF, Canakci V (2007) Pain experienced by patients undergoing different periodontal therapies. J Am Dent Assoc 138:1563–1573
Urban T, Wenzel A (2010) Discomfort experienced after immediate implant placement associated with three different regenerative techniques. Clin Oral Implants Res 21:1271–1277. https://doi.org/10.1111/j.1600-0501.2010.01943.x
Tan WC, Krishnaswamy G, Ong MM, Lang NP (2014) Patient-reported outcome measures after routine periodontal and implant surgical procedures. J Clin Periodontol 41:618–624. https://doi.org/10.1111/jcpe.12248
Canakci V, Canakci CF (2007) Pain levels in patients during periodontal probing and mechanical non-surgical therapy. Clin Oral Investig 11:377–383. https://doi.org/10.1007/s00784-007-0126-z
Matthews DC, McCulloch CA (1993) Evaluating patient perceptions as short-term outcomes of periodontal treatment: a comparison of surgical and non-surgical therapy. J Periodontol 64:990–997. https://doi.org/10.1902/jop.1993.64.10.990
Cattaneo V, Rota C, Silvestri M, Piacentini C, Forlino A, Gallanti A, Rasperini G, Cetta G (2003) Effect of enamel matrix derivative on human periodontal fibroblasts: proliferation, morphology and root surface colonization. An in vitro study. J Periodontal Res 38:568–574
Lyngstadaas SP, Lundberg E, Ekdahl H, Andersson C, Gestrelius S (2001) Autocrine growth factors in human periodontal ligament cells cultured on enamel matrix derivative. J Clin Periodontol 28:181–188
Yuan K, Chen CL, Lin MT (2003) Enamel matrix derivative exhibits angiogenic effect in vitro and in a murine model. J Clin Periodontol 30:732–738
Schlueter SR, Carnes DL, Cochran DL (2007) In vitro effects of enamel matrix derivative on microvascular cells. J Periodontol 78:141–151. https://doi.org/10.1902/jop.2007.060111
Iruela-Arispe ML, Sage EH (1993) Endothelial cells exhibiting angiogenesis in vitro proliferate in response to TGF-beta 1. J Cell Biochem 52:414–430. https://doi.org/10.1002/jcb.240520406
Guimaraes GF, de Araujo VC, Nery JC, Peruzzo DC, Soares AB (2015) Microvessel density evaluation of the effect of enamel matrix derivative on soft tissue after implant placement: a preliminary study. Int J Periodontics Restorative Dent 35:733–738. https://doi.org/10.11607/prd.2044
Van der Pauw MT, Van den Bos T, Everts V, Beertsen W (2000) Enamel matrix-derived protein stimulates attachment of periodontal ligament fibroblasts and enhances alkaline phosphatase activity and transforming growth factor beta1 release of periodontal ligament and gingival fibroblasts. J Periodontol 71:31–43. https://doi.org/10.1902/jop.2000.71.1.31
Funding
This research was supported by Wonkwang University in 2019.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the Institutional Review Board (IRB) of Daejeon Dental Hospital, Wonkwang University (approval no. W1807/001-001).
Informed consent
All enrolled patients provided written fully informed consent in accordance with the IRB guidelines, and the study was conducted in accordance with the Declaration of Helsinki and the Guidelines on Good Clinical Practice.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lee, JH., Park, YS., Kim, YT. et al. Assessment of early discomfort and wound healing outcomes after periodontal surgery with and without enamel matrix derivative: an observational retrospective case-control study. Clin Oral Invest 24, 229–237 (2020). https://doi.org/10.1007/s00784-019-02941-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-02941-w