Abstract
Background
Primary spinal pilocytic astrocytoma (PA) is an extremely rare low-grade astrocytoma with unclear natural history. The demographic characteristics, imaging features, and long-term surgical outcomes have not been clarified due to low prevalence and limited reports.
Methods
A retrospective review within a single institution between 2004 and 2018 of all patients with pathologically proven PA was conducted. Patient data including demographics, radiographic features, treatment modalities, and long-term outcomes were evaluated.
Results
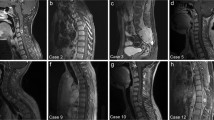
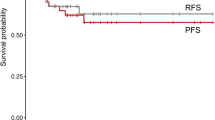
Twenty consecutive patients were identified, and 16 (80%) were male patients, with a mean age at presentation of 29 ± 13 years. The lesion was primarily located in cervical (n = 10, 50%), thoracic (n = 7, 35%), cervico-thoracic junction (n = 2), and lumbar level (n = 1, 5%). The tumor had a mean extension of 4 ± 2 (1–7) vertebral segments. Most PAs were located eccentrically (n = 16, 80%), with most being heterogeneous in appearance (cystic and solid) or purely cystic (n = 14, 70%), and had unclear margins (n = 16, 80%). Eleven patients (55%) had associated syringomyelia. Gross total resection (GTR) was achieved in 11 (55%) patients, and subtotal resection (STR) in 9 (45%). During a mean follow-up of 104 ± 56 months, 2 patients died and recurrence was found in 4 patients (20%), translating to a mean progression-free survival of 21 ± 11 months.
Conclusion
Primary spinal PA is a rare entity with acceptable progression-free survival if treated appropriately. Surgical resection may provide reasonable prolongation of survival, and GTR should be achieved if possible. A close follow-up is recommended especially for residual lesions, and a further in-depth investigation of molecular biomarkers is needed to stratify risk and prognostic factors.





Similar content being viewed by others
References
Azad TD, Pendharkar AV, Pan J, Huang Y, Li A, Esparza R et al (2018) Surgical outcomes of pediatric spinal cord astrocytomas: systematic review and meta-analysis. J Neurosurg Pediatr 22:404–410
Bannykh SI, Mirocha J, Nuno M, Lopategui J, Kandala G (2014) V600E BRAF mutation in pilocytic astrocytoma is associated with a more diffuse growth pattern but does not confer a more aggressive clinical behavior. Clin Neuropathol 33:388–398
Bansal S, Borkar SA, Mahapatra AK (2017) Hydrocephalus associated with spinal intramedullary pilocytic astrocytoma. Asian J Neurosurg 12:217–219
Baran O, Kasimcan O, Sav A, Oruckaptan H (2019) Holocord pilocytic astrocytoma in an adult: a rare case report and review of the literature. World Neurosurg 126:369–375
Bell E, Kanodia AK, Gunaratne B, Edgar A (2018) Leptomeningeal dissemination of spinal pilocytic astrocytoma: a rare entity. BMJ Case Rep 2018:bcr2018226955
Burkhard C, Di Patre PL, Schüler D, Schüler G, Yaşargil MG, Yonekawa Y et al (2003) A population-based study of the incidence and survival rates in patients with pilocytic astrocytoma. J Neurosurg 98:1170–1174
Carey SS, Sadighi Z, Wu S, Chiang J, Robinson GW, Ghazwani Y et al (2019) Evaluating pediatric spinal low-grade gliomas: a 30-year retrospective analysis. J Neuro-Oncol 145:519–529
Choi GH, Oh JK, Kim TY, You NK, Lee HS, Yoon DH et al (2012) The clinical features and surgical outcomes of pediatric patients with primary spinal cord tumor. Childs Nerv Syst 28:897–904
Chourmouzi D, Papadopoulou E, Konstantinidis M, Syrris V, Kouskouras K, Haritanti A et al (2014) Manifestations of pilocytic astrocytoma: a pictorial review. Insights Imaging 5:387–402
Collins VP, Jones DT, Giannini C (2015) Pilocytic astrocytoma: pathology, molecular mechanisms and markers. Acta Neuropathol 129:775–788
Colnat-Coulbois S, Klein O, Braun M, Thouvenot P, Marchal JC (2010) Management of intramedullary cystic pilocytic astrocytoma with rhenium-186 intracavitary irradiation: case report. Neurosurgery 66:E1023–E1024 discussion E1024
Dauleac C, Messerer R, Obadia-Andre N, Afathi M, Barrey CY (2019) Cysts associated with intramedullary ependymomas of the spinal cord: clinical, MRI and oncological features. J Neuro-Oncol 144:385–391
Diaz-Aguilar D, ReFaey K, Clifton W, Durcanova B, Chen SG, Deen HG et al (2019) Prognostic factors and survival in low grade gliomas of the spinal cord: a population-based analysis from 2006 to 2012. J Clin Neurosci 61:14–21
Ebner FH, Schittenhelm J, Roser F, Scheel-Walter H, Tatagiba M, Schuhmann MU (2012) Management of holocord pilocytic astrocytomas in children and adolescents: an update. Pediatr Neurosurg 48:133–140
Harraher CD, Vogel H, Steinberg GK (2013) Spinal pilocytic astrocytoma in an elderly patient. World Neurosurg 79(5–6):799
Horger M, Ritz R, Beschorner R, Fenchel M, Nägele T, Danz S et al (2011) Spinal pilocytic astrocytoma: MR imaging findings at first presentation and following surgery. Eur J Radiol 79:389–399
Jiang Y, Lv L, Yin S, Zhou P, Jiang S (2020) Primary spinal pilocytic astrocytoma: clinical study with long-term follow-up in 16 patients and a literature review. Neurosurg Rev 43:719–727
Karikari IO, Nimjee SM, Hodges TR, Cutrell E, Hughes BD, Powers CJ et al (2011) Impact of tumor histology on resectability and neurological outcome in primary intramedullary spinal cord tumors: a single-center experience with 102 patients. Neurosurgery 68:188–197 discussion 197
Kobayashi K, Ando K, Kato F, Kanemura T, Sato K, Kamiya M et al (2018) MRI characteristics of spinal ependymoma in WHO grade II: a review of 59 cases. Spine (Phila Pa 1976) 43:E525–e530
Marko NF, Weil RJ (2012) The molecular biology of WHO grade I astrocytomas. Neuro-Oncology 14:1424–1431
Martinelli C, Gabriele F, Manai F, Ciccone R, Novara F, Sauta E et al (2020) The search for molecular markers in a gene-orphan case study of a pediatric spinal cord pilocytic astrocytoma. Cancer Genomics Proteomics 17:117–130
McBride D, Aljuboori Z, Hattab EM, Downs R, Woo S, Williams B et al (2018) An elderly patient presenting with a primary spinal multifocal intradural extramedullary pilocytic astrocytoma: a case report and review of the literature. BMC Cancer 18:806
McCormick PC, Torres R, Post KD, Stein BM (1990) Intramedullary ependymoma of the spinal cord. J Neurosurg 72:523–532
Miyata K, Hori T, Shimomura Y, Joko M, Takayasu M, Okumura A (2018) Pseudoprogression successfully treated with bevacizumab in a child with spinal pilocytic astrocytoma. Childs Nerv Syst 34:2305–2308
Ohgaki H, Kleihues P (2005) Population-based studies on incidence, survival rates, and genetic alterations in astrocytic and oligodendroglial gliomas. J Neuropathol Exp Neurol 64:479–489
She DJ, Lu YP, Xiong J, Geng DY, Yin B (2019) MR imaging features of spinal pilocytic astrocytoma. BMC Med Imaging 19:5
Tabash MA (2019) Characteristics, survival and incidence rates and trends of pilocytic astrocytoma in children in the United States; SEER-based analysis. J Neurol Sci 400:148–152
Takamiya S, Hatanaka KC, Ishi Y, Seki T, Yamaguchi S (2020) Spinal cord anaplastic astrocytoma with BRAF V600E mutation: a case report and review of literature. Neuropathology 40:275–279
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee by the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Tumor - Glioma
The hospital in the article refers to the Chinese PLA General Hospital
Rights and permissions
About this article
Cite this article
Zhang, L., Li, T., Qiao, G. et al. Clinical characteristics and long-term surgical outcomes of spinal pilocytic astrocytoma: a report of twenty cases. Acta Neurochir 163, 3005–3013 (2021). https://doi.org/10.1007/s00701-020-04606-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-020-04606-0