Abstract
Objective
Hypertension is common in patients with aneurysmal subarachnoid hemorrhage (SAH). However, it is still unclear whether premorbid antihypertensive therapy can help to reduce the risk of severe aneurysmal bleeding. Therefore, this study aims to assess the effect of premorbid hypertension control on outcome of patients with aneurysmal SAH.
Methods
We retrospectively reviewed the clinical data of patients with intracranial aneurysms admitted to our institution from February 2012 to December 2017. Based on premorbid hypertension history and use of antihypertensive agents, all patients with aneurysmal SAH were divided into antihypertensive group and uncontrolled group. Patient characteristics, imaging features, clinical complication, and outcome were analyzed between the two groups.
Results
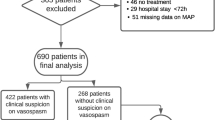
A total of 348 patients with ruptured aneurysms were included in this study. Compared to those with premorbid controlled hypertension, patients with premorbid uncontrolled hypertension presented worse clinical grade, with more severe aneurysmal SAH and more frequent intracerebral hematoma. Patients receiving a treatment for ACEI type or ARB type of drugs in the antihypertensive group suffered from less amount of aneurysmal bleeding, while patients with grade 3 hypertension in the uncontrolled group suffered from more amount of aneurysmal bleeding. Patients with premorbid controlled hypertension had a lower incidence of rebleeding, hydrocephalus, and cerebral vasospasm, and had a lower rate of disability and mortality.
Conclusions
Premorbid hypertension control is associated with favorable clinical outcome of patients with aneurysmal SAH. Besides, the ACEI type or ARB type of antihypertensive agents is associated with the less amount of bleeding after aneurysm rupture.

Similar content being viewed by others
References
Connolly ES Jr, Rabinstein AA, Carhuapoma JR, Derdeyn CP, Dion J, Higashida RT, Hoh BL, Kirkness CJ, Naidech AM, Ogilvy CS, Patel AB, Thompson BG, Vespa P (2012) Guidelines for the management of aneurysmal subarachnoid hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 43:1711–1737
Larrew T, Pryor W 3rd, Weinberg J, Webb S, Battenhouse H, Turk AS, Chaudry I, Spiotta A, Turner R (2015) Aneurysmal subarachnoid hemorrhage: a statewide assessment of outcome based on risk factors, aneurysm characteristics, and geo-demography. J Neurointerv Surg 7:855–860
Lindner SH, Bor AS, Rinkel GJ (2010) Differences in risk factors according to the site of intracranial aneurysms. J Neurol Neurosurg Psychiatry 81:116–118
Steiner T, Juvela S, Unterberg A, Jung C, Forsting M, Rinkel G (2013) European Stroke Organization guidelines for the management of intracranial aneurysms and subarachnoid haemorrhage. Cerebrovasc Dis 35:93–112
Shiue I, Arima H, Hankey GJ, Anderson CS (2011) Location and size of ruptured intracranial aneurysm and serious clinical outcomes early after subarachnoid hemorrhage: a population-based study in Australasia. Cerebrovasc Dis 31:573–579
De Marchis GM, Lantigua H, Schmidt JM, Lord AS, Velander AJ, Fernandez A, Falo MC, Agarwal S, Connolly ES Jr, Claassen J, Mayer SA (2014) Impact of premorbid hypertension on haemorrhage severity and aneurysm rebleeding risk after subarachnoid haemorrhage. J Neurol Neurosurg Psychiatry 85:56–59
Jaja BN, Lingsma H, Schweizer TA, Thorpe KE, Steyerberg EW, Macdonald RL (2015) Prognostic value of premorbid hypertension and neurological status in aneurysmal subarachnoid hemorrhage: pooled analyses of individual patient data in the SAHIT repository. J Neurosurg 122:644–652
Lindgren A, Turner EB, Sillekens T, Meretoja A, Lee JM, Hemmen TM, Koivisto T, Alberts M, Lemmens R, Jääskeläinen JE, Vergouwen MDI, Rinkel GJE (2018) Outcome after clipping and coiling for aneurysmal subarachnoid hemorrhage in clinical practice in Europe, USA, and Australia. Neurosurgery. https://doi.org/10.1093/neuros/nyy223
Stranjalis G, Loufardaki M, Koutsarnakis C, Kalamatianos T (2016) Trends in the management and hospital outcome of spontaneous subarachnoid hemorrhage in the post-international subarachnoid aneurysm trial era in Greece: analysis of 719 patients during a 13-year period. World Neurosurg 88:327–332
Zhao B, Tan X, Yang H, Li Z, Zheng K, Xiong Y, Zhong M (2016) Endovascular coiling versus surgical clipping for poor-grade ruptured intracranial aneurysms: postoperative complications and clinical outcome in a multicenter poor-grade aneurysm study. AJNR Am J Neuroradiol 37:873–878
Lord AS, Fernandez L, Schmidt JM, Mayer SA, Claassen J, Lee K, Connolly ES, Badjatia N (2012) Effect of rebleeding on the course and incidence of vasospasm after subarachnoid hemorrhage. Neurology 78:31–37
Kim BJ, Kang HG, Kwun BD, Ahn JS, Lee J, Lee SH, Kang DW, Kim JS, Kwon SU (2017) Small versus large ruptured intracranial aneurysm concerns with the site of aneurysm. Cerebrovasc Dis 43:139–144
Tominari S, Morita A, Ishibashi T, Yamazaki T, Takao H, Murayama Y, Sonobe M, Yonekura M, Saito N, Shiokawa Y, Date I, Tominaga T, Nozaki K, Houkin K, Miyamoto S, Kirino T, Hashi K, Nakayama T (2015) Unruptured Cerebral Aneurysm Study Japan Investigators. Prediction model for 3-year rupture risk of unruptured cerebral aneurysms in Japanese patients. Ann Neurol 77:1050–1059
Can A, Castro VM, Ozdemir YH, Dagen S, Yu S, Dligach D, Finan S, Gainer V, Shadick NA, Murphy S, Cai T, Savova G, Dammers R, Weiss ST, Du R (2017) Association of intracranial aneurysm rupture with smoking duration, intensity, and cessation. Neurology 89:1408–1415
Tawk RG, Grewal SS, Heckman MG, Navarro R, Ferguson JL, Starke EL, Rawal B, Hanel R, Miller D, Wharen RE, Freeman WD (2015) Influence of body mass index and age on functional outcomes in patients with subarachnoid hemorrhage. Neurosurgery 76:136–141
Vlak MH, Rinkel GJ, Greebe P, Algra A (2013) Risk of rupture of an intracranial aneurysm based on patient characteristics: a case-control study. Stroke 44:1256–1259
Hamade YJ, Zammar SG, El Tecle NE, El Ahmadieh TY, Chandler JP, Bendok BR (2014) Hypertension and intracranial aneurysms: association or causation? World Neurosurg 82:e665–e667
Lee HJ, Jang SI, Park EC (2017) Effect of adherence to antihypertensive medication on stroke incidence in patients with hypertension: a population-based retrospective cohort study. BMJ Open 7:e014486
Lindgren AE, Kurki MI, Riihinen A, Koivisto T, Ronkainen A, Rinne J, Hernesniemi J, Eriksson JG, Jääskeläinen JE, von und zu Fraunberg M (2014) Hypertension predisposes to the formation of saccular intracranial aneurysms in 467 unruptured and 1053 ruptured patients in Eastern Finland. Ann Med 46:169–176
Shiue I, Hankey GJ, Arima H, Anderson CS (2011) Suboptimal awareness and control of hypertension increases the risk of subarachnoid hemorrhage in the community: results from the ACROSS. Neurol Res 33:1068–1071
Nuki Y, Tsou TL, Kurihara C, Kanematsu M, Kanematsu Y, Hashimoto T (2009) Elastase-induced intracranial aneurysms in hypertensive mice. Hypertension 54:1337–1344
Tada Y, Wada K, Shimada K, Makino H, Liang EI, Murakami S, Kudo M, Kitazato KT, Nagahiro S, Hashimoto T (2014) Roles of hypertension in the rupture of intracranial aneurysms. Stroke 45:579–586
Lagares A, Jiménez-Roldán L, Gomez PA, Munarriz PM, Castaño-León AM, Cepeda S, Alén JF (2015) Prognostic value of the amount of bleeding after aneurysmal subarachnoid hemorrhage: a quantitative volumetric study. Neurosurgery 77:898–907
Salary M, Quigley MR, Wilberger JE Jr (2007) Relation among aneurysm size, amount of subarachnoid blood, and clinical outcome. J Neurosurg 107:13–17
Griessenauer CJ, Tubbs RS, Foreman PM, Chua MH, Vyas NA, Lipsky RH, Lin M, Iyer R, Haridas R, Walters BC, Chaudry S, Malieva A, Wilkins S, Harrigan MR, Fisher WS 3rd, Shoja MM (2018) Association of renin-angiotensin system genetic polymorphisms and aneurysmal subarachnoid hemorrhage. J Neurosurg 128:86–93
Slowik A, Borratynska A, Pera J, Betlej M, Dziedzic T, Krzyszkowski T, Czepko R, Figlewicz DA, Szczudlik A (2004) II genotype of the angiotensin-converting enzyme gene increases the risk for subarachnoid hemorrhage from ruptured aneurysm. Stroke 35:1594–1597
Kaddumukasa M, Ddumba E, Duncan P, Goldstein LB (2012) Poststroke hypertension in Africa. Stroke 43:3402–3404
Kettani FZ, Dragomir A, Côté R, Roy L, Bérard A, Blais L, Lalonde L, Moreau P, Perreault S (2009) Impact of a better adherence to antihypertensive agents on cerebrovascular disease for primary prevention. Stroke 40:213–220
Pittman DG, Tao Z, Chen W, Stettin GD (2010) Antihypertensive medication adherence and subsequent healthcare utilization and costs. Am J Manag Care 16:568–576
Shin S, Song H, Oh SK, Choi KE, Kim H, Jang S (2013) Effect of antihypertensive medication adherence on hospitalization for cardiovascular disease and mortality in hypertensive patients. Hypertens Res 36:1000–1005
Rosengart AJ, Schultheiss KE, Tolentino J, Macdonald RL (2007) Prognostic factors for outcome in patients with aneurysmal subarachnoid hemorrhage. Stroke 38:2315–2321
Funding
National Natural Science Foundation of China (No. 81671160; No. 81571159) and 13th Five-Year National Key Research Project of China (2016YFC1300800; 2016YFC1300804; 2016YFC1300805) provided financial support. The sponsor had no role in the design or conduct of this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (Chongqing Medical University First Affiliated Hospital) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, formal consent is not required.
Additional information
Comments
My wife is a cardiologist. She believes strongly in the prophylactic treatment of hypertension, for many good reasons, including prevention of hypertensive secondary effects on multiple organ systems. Here in this report we have another compelling reason to endorse the prophylactic treatment of hypertension. We have a retrospective analysis of SAH patients to evaluate their outcomes in two categories, premorbid hypertension controlled with antihypertensive treatment, or premorbid hypertension but uncontrolled medically. It seems, from this report, that hypertensive patients who had SAH while successfully controlled on antihypertensive treatment at the time of their ictus enjoyed a more favorable clinical course, perhaps because of a limit on escaped blood (at least in patients receiving ACEI type or ARB type of drugs), or perhaps for other, not discerned, factors. The hypertension-controlled patients also suffered less rebleeding, hydrocephalus, and DIND, and had overall lower disability and mortality.
Of course any question brings up so many more equally interesting questions, which were not designed to be addressed here. Why was bleed volume selectively reduced by the ACEI and ARB treatments? Does antihypertensive treatment prevent aneurysm growth for patients under observation, or even de novo aneurysm formation?
One lesson for me is that I must be especially careful to confirm proper antihypertensive management in the large number of consultations I see for patients with UIA who defer treatment. Another lesson, I suppose, would be to listen carefully to my wife’s advice, as this study validates her aggressive approach to treatment of even silent hypertension.
Christopher Loftus
PA, USA
This article is part of the Topical Collection on Vascular Neurosurgery - Aneurysm
Rights and permissions
About this article
Cite this article
Zheng, J., Xu, R., Liu, G. et al. Effect of premorbid hypertension control on outcome of patients with aneurysmal subarachnoid hemorrhage. Acta Neurochir 160, 2401–2407 (2018). https://doi.org/10.1007/s00701-018-3699-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-018-3699-1