Abstract
Aims
Observational studies indicated that resting heart rate (RHR) was associated with diabetes mellitus (DM) risk; however, it remains unclear whether the association between RHR and DM is causal. We aimed to examine whether there was causal association of RHR with DM risk.
Methods
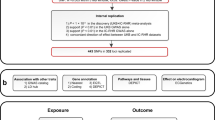
A prospective study including 16,201 middle-aged and older Chinese (7031 males and 9170 females) derived from the Dongfeng-Tongji cohort was performed. Cox proportional hazard regression models were conducted to estimate the associations between RHR and incident DM risk. In 7481 participants, 65 single nucleotide polymorphisms related to RHR were genotyped. A genetic risk score (GRS) of RHR was calculated based on the RHR-associated variants. The causal associations of RHR with DM risk were investigated by Mendelian randomization analysis.
Results
During a mean (SD) follow-up of 4.5 (0.5) years, 1110 diabetes were identified. Compared with the referential RHR group (≤ 60 beats per minute [bpm]), individuals with RHR > 80 bpm have a higher incident diabetes risk, with a hazard ratio of 1.40 (95% confidence interval [CI], 1.05–1.88). With per SD increase in the weighted genetic risk score, the resting heart rate increased by 0.71 bpm (95% CI 0.49–0.93). By using the GRS to estimate the unconfounded effect, we found that higher resting heart rate did not have a causal effect on diabetes risk (OR 1.00 [95% CI 0.95–1.05]).
Conclusions
The present study supported a positive but not a causal association of RHR with incident diabetes risk. More studies are needed to verify our findings.
Similar content being viewed by others
References
Zhou B, Lu Y, Hajifathalian K, Bentham J, Di Cesare M, Danaei G et al (2016) Worldwide trends in diabetes since 1980: a pooled analysis of 751 population-based studies with 4.4 million participants. Lancet 387:1513–1530. https://doi.org/10.1016/S0140-6736(16)00618-8
IDF Diabetes Atlas-eighth edition [Internet]. International Diabetes Federation, Brussels, Belgium. http://www.diabetesatlas.org. Accessed 23 Feb 2017
Xu Y, Wang L, He J, Bi Y, Li M, Wang T et al (2013) Prevalence and control of diabetes in Chinese adults. JAMA 310:948–959. https://doi.org/10.1001/jama.2013.168118
Grassi G, Vailati S, Bertinieri G, Seravalle G, Stella ML, Dell’Oro R et al (1998) Heart rate as marker of sympathetic activity. J Hypertens 16:1635–1639. https://doi.org/10.1097/00004872-199816110-00010
Jamerson KA, Julius S, Gudbrandsson T, Andersson O, Brant DO (1993) Reflex sympathetic activation induces acute insulin resistance in the human forearm. Hypertension 21:618–623. https://doi.org/10.1161/01.hyp.21.5.618
Shigetoh Y, Adachi H, Yamagishi S, Enomoto M, Fukami A, Otsuka M et al (2009) Higher heart rate may predispose to obesity and diabetes mellitus: 20-year prospective study in a general population. Am J Hypertens 22:151–155. https://doi.org/10.1038/ajh.2008.331
Zhang X, Shu XO, Xiang YB, Yang G, Li H, Cai H et al (2010) Resting heart rate and risk of type 2 diabetes in women. Int J Epidemiol 39:900–906. https://doi.org/10.1093/ije/dyq068
Grantham NM, Magliano DJ, Tanamas SK, Soderberg S, Schlaich MP, Shaw JE (2013) Higher heart rate increases risk of diabetes among men: The Australian Diabetes Obesity and Lifestyle (AusDiab) Study. Diabet Med 30:421–427. https://doi.org/10.1111/dme.12045
Li YQ, Sun CQ, Li LL, Wang L, Guo YR, You AG et al (2014) Resting heart rate as a marker for identifying the risk of undiagnosed type 2 diabetes mellitus: a cross-sectional survey. BMC Public Health 14:1052. https://doi.org/10.1186/1471-2458-14-1052
Aune D, OH B, Vatten LJ (2015) Resting heart rate and the risk of type 2 diabetes: a systematic review and dose-response meta-analysis of cohort studies. Nutr Metab Cardiovasc Dis 25:526–534. https://doi.org/10.1016/j.numecd.2015.02.008
Wang L, Cui L, Wang Y, Vaidya A, Chen S, Zhang C et al (2015) Resting heart rate and the risk of developing impaired fasting glucose and diabetes: the Kailuan prospective study. Int J Epidemiol 44:689–699. https://doi.org/10.1093/ije/dyv079
Kim DI, Yang HI, Park JH, Lee MK, Kang DW, Chae JS et al (2016) The association between resting heart rate and type 2 diabetes and hypertension in Korean adults. Heart 102:1757–1762. https://doi.org/10.1136/heartjnl-2015-309119
Lee DH, de Rezende LFM, Hu FB, Jeon JY, Giovannucci EL (2019) Resting heart rate and risk of type 2 diabetes: a prospective cohort study and meta-analysis. Diabetes/Metab Res Rev 35(2):e3095. https://doi.org/10.1002/dmrr.3095
Carnethon MR, Golden SH, Folsom AR, Haskell W, Liao D (2003) Prospective investigation of autonomic nervous system function and the development of type 2 diabetes: the Atherosclerosis Risk In Communities study, 1987–1998. Circulation 107:2190–2195. https://doi.org/10.1161/01.CIR.0000066324.74807.95
Carnethon MR, Yan L, Greenland P, Garside DB, Dyer AR, Metzger B et al (2008) Resting heart rate in middle age and diabetes development in older age. Diabetes Care 31:335–339. https://doi.org/10.2337/dc07-0874
Smith GD, Ebrahim S (2004) Mendelian randomization: prospects, potentials, and limitations. Int J Epidemiol 33:30–42. https://doi.org/10.1093/ije/dyh132
den Hoed M, Eijgelsheim M, Esko T, Brundel BJ, Peal DS, Evans DM et al (2013) Identification of heart rate-associated loci and their effects on cardiac conduction and rhythm disorders. Nat Genet 45:621–631. https://doi.org/10.1038/ng.2610
Eppinga RN, Hagemeijer Y, Burgess S, Hinds DA, Stefansson K, Gudbjartsson DF et al (2016) Identification of genomic loci associated with resting heart rate and shared genetic predictors with all-cause mortality. Nat Genet 48:1557–1563. https://doi.org/10.1038/ng.3708
Wang F, Zhu J, Yao P, Li X, He M, Liu Y et al (2013) Cohort profile: the Dongfeng–Tongji cohort study of retired workers. Int J Epidemiol 42:731–740. https://doi.org/10.1093/ije/dys053
He M, Wu C, Xu J, Guo H, Yang H, Zhang X et al (2014) A genome wide association study of genetic loci that influence tumour biomarkers cancer antigen 19-9, carcinoembryonic antigen and alpha fetoprotein and their associations with cancer risk. Gut 63:143–151. https://doi.org/10.1136/gutjnl-2012-303434
He M, Xu M, Zhang B, Liang J, Chen P, Lee JY et al (2015) Meta-analysis of genome-wide association studies of adult height in East Asians identifies 17 novel loci. Hum Mol Genet 24:1791–1800. https://doi.org/10.1093/hmg/ddu583
American Diabetes Association (2014) Diagnosis and classification of diabetes mellitus. Diabetes Care 37(Suppl 1):S81–S90. https://doi.org/10.2337/dc14-S081
Lawlor DA, Harbord RM, Sterne JA, Timpson N, Davey Smith G (2008) Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med 27:1133–1163. https://doi.org/10.1002/sim.3034
Dai X, Yuan J, Yao P, Yang B, Gui L, Zhang X et al (2013) Association between serum uric acid and the metabolic syndrome among a middle- and old-age Chinese population. Eur J Epidemiol 28:669–676. https://doi.org/10.1007/s10654-013-9829-4
Freathy RM, Timpson NJ, Lawlor DA, Pouta A, Ben-Shlomo Y, Ruokonen A et al (2008) Common variation in the FTO gene alters diabetes-related metabolic traits to the extent expected given its effect on BMI. Diabetes 57:1419–1426. https://doi.org/10.2337/db07-1466
Didelez V, Sheehan N (2007) Mendelian randomization as an instrumental variable approach to causal inference. Stat Methods Med Res 16:309–330. https://doi.org/10.1177/0962280206077743
Cho YS, Chen CH, Hu C, Long J, Ong RT, Sim X et al (2011) Meta-analysis of genome-wide association studies identifies eight new loci for type 2 diabetes in east Asians. Nat Genet 44:67–72. https://doi.org/10.1038/ng.1019
Morris AP, Voight BF, Teslovich TM, Ferreira T, Segre AV, Steinthorsdottir V et al (2012) Large-scale association analysis provides insights into the genetic architecture and pathophysiology of type 2 diabetes. Nat Genet 44:981–990. https://doi.org/10.1038/ng.2383
Zhao W, Rasheed A, Tikkanen E, Lee JJ, Butterworth AS, Howson JMM et al (2017) Identification of new susceptibility loci for type 2 diabetes and shared etiological pathways with coronary heart disease. Nat Genet 49:1450–1457. https://doi.org/10.1038/ng.3943
Holmes MV, Asselbergs FW, Palmer TM, Drenos F, Lanktree MB, Nelson CP et al (2015) Mendelian randomization of blood lipids for coronary heart disease. Eur Heart J 36:539–550. https://doi.org/10.1093/eurheartj/eht571
Runcie CJ, Reeve W, Reidy J, Dougall JR (1990) A comparison of measurements of blood pressure, heart-rate and oxygenation during inter-hospital transport of the critically ill. Intensive Care Med 16:317–322. https://doi.org/10.1007/bf01706357
Acknowledgements
The authors would like to thank all study subjects for participating in the present DFTJ-cohort study as well as all volunteers for assisting in collecting the samples and data.
Funding
This work was supported by the grant from the National Natural Science Foundation (Grant NSFC-81522040 and 81473051); the Program for HUST Academic Frontier Youth Team, and National Key R&D Program of China (2017YFC0907501).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study has been approved by the Ethics and Human Subject Committee of the School of Public Health, Tongji Medical College, and Dongfeng General Hospital, the Dongfeng Motor Corporation (DMC).
Informed consent
All study participants provided written informed consents.
Additional information
Managed by Massimo Federici.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Long, T., Wang, J., Han, X. et al. Association between resting heart rate and incident diabetes risk: a Mendelian randomization study. Acta Diabetol 56, 1037–1044 (2019). https://doi.org/10.1007/s00592-019-01344-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-019-01344-3