Abstract
Aims
Dietary proteins, including those obtained from animal and plant sources, have inconsistently been correlated with type 2 diabetes mellitus (T2DM) risk. Therefore, a meta-analysis was conducted to evaluate the association between dietary proteins and the risk of T2DM.
Methods
Prospective cohort studies published until November 2018 were systematically searched in PubMed, Embase, and the Cochrane library. The pooled relative risks (RRs) were calculated with 95% confidence intervals (CIs) using the random-effects model.
Results
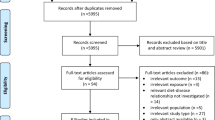
Ten articles involving a total of 21 cohorts were included in the final meta-analysis. A total of 487,956 individuals were recruited in these studies and 38,350 T2DM cases were reported. Analysis of the pooled RRs indicated that high total protein intake was associated with an increased risk of T2DM (RR 1.10; P = 0.006), whereas moderate total protein intake was not significantly associated with T2DM risk (RR 1.00; P = 0.917). Moreover, a higher risk of T2DM was observed with high animal protein intake (RR 1.13; P = 0.013), whereas moderate animal protein intake had little or no effect on T2DM risk (RR 1.06; P = 0.058). Finally, high intake of plant protein did not affect T2DM risk (RR 0.93; P = 0.074), whereas moderate intake was associated with a reduced risk of T2DM (RR 0.94; P < 0.001).
Conclusions
The results of this study indicate that high total protein and animal protein intakes are associated with an increased risk of T2DM, whereas moderate plant protein intake is associated with a decreased risk of T2DM.







Similar content being viewed by others
Change history
30 May 2019
The article Dietary protein intake and subsequent risk of type 2 diabetes: a dose–response meta-analysis of prospective cohort studies written by Jianhong Ye, Qixin Yu, Weihua Mai, Peiling Liang, Xiaoxia Liu, Yunnan Wang was originally published electronically on the publisher’s internet portal (currently SpringerLink) on 30 March 2019 with open access. With the author(s)’ decision to step back from Open Choice, the copyright of the article changed on 30 May 2019 to © Springer-Verlag Italia S.r.l., part of Springer Nature 2019 and the article is forthwith distributed under the terms of copyright.
References
American Diabetes A (2018) Standards of Medical Care in Diabetes-2018 Abridged for Primary Care Providers. Clin Diabetes 36(1):14–37. https://doi.org/10.2337/cd17-0119
Radaelli MG, Martucci F, Perra S, Accornero S, Castoldi G, Lattuada G et al (2018) NAFLD/NASH in patients with type 2 diabetes and related treatment options. J Endocrinol Invest 41(5):509–521. https://doi.org/10.1007/s40618-017-0799-3
Alberti KG (1996) The clinical implications of impaired glucose tolerance. Diabetes Med 13(11):927–937 https://doi.org/10.1002/(SICI)1096-9136(199611)13:11%3C927::AID-DIA279%3E3.0.CO;2-E
de Vegt F, Dekker JM, Jager A, Hienkens E, Kostense PJ, Stehouwer CD et al (2001) Relation of impaired fasting and postload glucose with incident type 2 diabetes in a Dutch population: the Hoorn Study. JAMA 285(16):2109–2113
Tabak AG, Herder C, Rathmann W, Brunner EJ, Kivimaki M (2012) Prediabetes: a high-risk state for diabetes development. Lancet 379(9833):2279–2290. https://doi.org/10.1016/S0140-6736(12)60283-9
Bellou V, Belbasis L, Tzoulaki I, Evangelou E (2018) Risk factors for type 2 diabetes mellitus: an exposure-wide umbrella review of meta-analyses. PLoS One 13(3):e0194127. https://doi.org/10.1371/journal.pone.0194127
Nuttall FQ, Schweim K, Hoover H, Gannon MC (2008) Effect of the LoBAG30 diet on blood glucose control in people with type 2 diabetes. Br J Nutr 99(3):511–519. https://doi.org/10.1017/S0007114507819155
Weickert MO, Roden M, Isken F, Hoffmann D, Nowotny P, Osterhoff M et al (2011) Effects of supplemented isoenergetic diets differing in cereal fiber and protein content on insulin sensitivity in overweight humans. Am J Clin Nutr 94(2):459–471. https://doi.org/10.3945/ajcn.110.004374
Pounis GD, Tyrovolas S, Antonopoulou M, Zeimbekis A, Anastasiou F, Bountztiouka V et al (2010) Long-term animal-protein consumption is associated with an increased prevalence of diabetes among the elderly: the Mediterranean Islands (MEDIS) study. Diabetes Metab 36(6 Pt 1):484–490. https://doi.org/10.1016/j.diabet.2010.06.007
Tian S, Xu Q, Jiang R, Han T, Sun C, Na L (2017) Dietary protein consumption and the risk of Type 2 diabetes: a systematic review and meta-analysis of cohort studies. Nutrients. https://doi.org/10.3390/nu9090982
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. https://doi.org/10.1371/journal.pmed.1000097
Wells G, Shea B, O’connell D, Peterson J, Welch V, Losos M, Tugwell P (2016) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Ottawa Hospital Research Institute, Ottawa (Available in March)
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Ades AE, Lu G, Higgins JP (2005) The interpretation of random-effects meta-analysis in decision models. Med Decis Making 25(6):646–654. https://doi.org/10.1177/0272989X05282643
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Tobias A (1999) Assessing the influence of a single study in the meta-analysis estimate. Stata Tech Bull 47:15–17
Deeks JJ, Altman DG, Bradburn MJ (2001) Statistical methods for examining heterogeneity and combining results from several studies in meta-analysis. Syst Rev Health Care Meta Anal Context:285–312
Thompson SG, Higgins JP (2002) How should meta-regression analyses be undertaken and interpreted? Stat Med 21(11):1559–1573
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50(4):1088–1101
Alhazmi A, Stojanovski E, McEvoy M, Garg ML (2014) Macronutrient intake and type 2 diabetes risk in middle-aged Australian women. Results from the Australian Longitudinal Study on Women’s Health. Public Health Nutr 17(7):1587–1594. https://doi.org/10.1017/S1368980013001870
Ericson U, Sonestedt E, Gullberg B, Hellstrand S, Hindy G, Wirfalt E, Orho-Melander M (2013) High intakes of protein and processed meat associate with increased incidence of type 2 diabetes. Br J Nutr 109(6):1143–1153. https://doi.org/10.1017/S0007114512003017
Malik VS, Li Y, Tobias DK, Pan A, Hu FB (2016) Dietary protein intake and risk of Type 2 diabetes in US men and women. Am J Epidemiol 183(8):715–728. https://doi.org/10.1093/aje/kwv268
Nanri A, Mizoue T, Kurotani K, Goto A, Oba S, Noda M et al (2015) Low-carbohydrate diet and type 2 diabetes risk in Japanese men and women: the Japan Public Health Center-Based Prospective Study. PLoS One 10(2):e0118377. https://doi.org/10.1371/journal.pone.0118377
Shang X, Scott D, Hodge AM, English DR, Giles GG, Ebeling PR, Sanders KM (2016) Dietary protein intake and risk of type 2 diabetes: results from the Melbourne Collaborative Cohort Study and a meta-analysis of prospective studies. Am J Clin Nutr 104(5):1352–1365. https://doi.org/10.3945/ajcn.116.140954
Sluijs I, Beulens JW, Spijkerman AM, Grobbee DE, Van der Schouw YT (2010) Dietary intake of total, animal, and vegetable protein and risk of type 2 diabetes in the European Prospective Investigation into Cancer and Nutrition (EPIC)-NL study. Diabetes care 33(1):43–48
Song Y, Manson JE, Buring JE, Liu S (2004) A prospective study of red meat consumption and type 2 diabetes in middle-aged and elderly women: the women’s health study. Diabetes care 27(9):2108–2115
Tinker LF, Sarto GE, Howard BV, Huang Y, Neuhouser ML, Mossavar-Rahmani Y et al (2011) Biomarker-calibrated dietary energy and protein intake associations with diabetes risk among postmenopausal women from the Women’s Health Initiative. Am J Clin Nutr 94(6):1600–1606
van Nielen M, Feskens EJ, Mensink M, Sluijs I, Molina E, Amiano P et al (2014) Dietary protein intake and incidence of type 2 diabetes in Europe: the EPIC-InterAct Case-Cohort Study. Diabetes Care 37(7):1854–1862. https://doi.org/10.2337/dc13-2627
Virtanen HEK, Koskinen TT, Voutilainen S, Mursu J, Tuomainen TP, Kokko P et al (2017) Intake of different dietary proteins and risk of type 2 diabetes in men: the Kuopio Ischaemic Heart Disease Risk Factor Study. Br J Nutr 117(6):882–893. https://doi.org/10.1017/S0007114517000745
Bao W, Bowers K, Tobias DK, Hu FB, Zhang C (2013) Prepregnancy dietary protein intake, major dietary protein sources, and the risk of gestational diabetes mellitus: a prospective cohort study. Diabetes Care 36(7):2001–2008. https://doi.org/10.2337/dc12-2018
Goueslard K, Cottenet J, Mariet AS, Sagot P, Petit JM, Quantin C (2017) Early screening for type 2 diabetes following gestational diabetes mellitus in France: hardly any impact of the 2010 guidelines. Acta Diabetol 54(7):645–651
Wang TJ, Larson MG, Vasan RS, Cheng S, Rhee EP, McCabe E, Lewis GD, Fox CS, Jacques PF, Fernandez C, O’Donnell CJ, Carr SA, Mootha VK, Florez JC, Souza A, Melander O, Clish CB, Gerszten RE (2011) Metabolite profiles and the risk of developing diabetes. Nat Med 17(4):448–453. https://doi.org/10.1038/nm.2307
Würtz P, Havulinna AS, Soininen P, Tynkkynen T, Prieto-Merino D, Tillin T et al (2015) Metabolite profiling and cardiovascular event riskclinical perspective: a prospective study of 3 population-based cohorts. Circulation 131(9):774–785
Wittenbecher C, Mühlenbruch K, Kröger J, Jacobs S, Kuxhaus O, Floegel A et al (2015) Amino acids, lipid metabolites, and ferritin as potential mediators linking red meat consumption to type 2 diabetes. Am J Clin Nutr 101(6):1241–1250
Young VR, Pellett PL (1994) Plant proteins in relation to human protein and amino acid nutrition. Am J Clin Nutr 59(5 Suppl):1203S–1212S. https://doi.org/10.1093/ajcn/59.5.1203S
Karastergiou K, Smith SR, Greenberg AS, Fried SK (2012) Sex differences in human adipose tissues–the biology of pear shape. Biol Sex Differ 3(1):13
Kautzky-Willer A, Harreiter J, Pacini G (2016) Sex and gender differences in risk, pathophysiology and complications of Type 2 diabetes mellitus. Endocr Rev 37(3):278–316. https://doi.org/10.1210/er.2015-1137
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Additional information
Managed by Antonio Secchi.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article was revised: Due to a retrospective Open Access cancellation.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ye, J., Yu, Q., Mai, W. et al. Dietary protein intake and subsequent risk of type 2 diabetes: a dose–response meta-analysis of prospective cohort studies. Acta Diabetol 56, 851–870 (2019). https://doi.org/10.1007/s00592-019-01320-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-019-01320-x