Abstract
Purpose
In skeletally immature patients with adolescent idiopathic scoliosis (AIS), vertebral body tethering (VBT) as a fusionless minimally invasive treatment option has been shown to correct the deformity by growth modulation. This prospective cohort study aimed to present the minimum 2 years’ results of double-sided VBT applied to double curves of 13 skeletally immature patients with AIS.
Methods
Thirteen skeletally immature patients with AIS and double curves were included. All patients were followed up within a brace for at least 6 weeks. A decision to proceed with surgery was established after the detection of curve progression within the brace (> 40° thoracic, > 35° lumbar) with a minimum curve flexibility of 30%.
Results
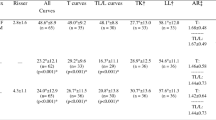
Patients had an average age of 11.8 years, average follow-up duration of 36.4 months (range 24 to 46), average preoperative main thoracic/thoracolumbar or lumbar curve magnitudes of 48.2°/45.3°. An average of 11.8 levels of tethering was undertaken. Thoracic screws were placed thoracoscopically, while mini-thoracotomy/lumbotomy was added for thoracolumbar levels. Postoperatively, an average first erect thoracic/thoracolumbar major curve magnitudes of 17.3°/14.3° were acquired, while they improved to 9.7°/8.2° at the last follow-up. No neurologic or implant-related complications were acquired.
Conclusion
Double-sided VBT was detected to provide 80% of thoracic (48.2° to 9.7°) and 82% of thoracolumbar–lumbar curve correction (45.3° to 8.2°) as a result of average two years. As being a growth modulating treatment option, double-sided VBT as applied under strict inclusion criteria was shown to be safe and effective for the correction of double curves in skeletally immature patients with AIS, by yielding a gradual, growth-assisted correction of both curves together with the preservation of coronal–sagittal balance without any major complications.



Similar content being viewed by others
References
Boudissa M, Eid A, Bourgeois E et al (2017) Early outcomes of spinal growth tethering for idiopathic scoliosis with a novel device: a prospective study with 2 years of follow-up. Childs Nerv Syst 33:813–818. https://doi.org/10.1007/s00381-017-3367-4
Samdani AF, Ames RJ, Kimball JS et al (2014) Anterior vertebral body tethering for idiopathic scoliosis: two-year results. Spine (Phila Pa 1976) 39:1688–1693. https://doi.org/10.1097/BRS.0000000000000472
Crawford CH 3rd, Lenke LG (2010) Growth modulation by means of anterior tethering resulting in progressive correction of juvenile idiopathic scoliosis: a case report. J Bone Joint Surg Am 92:202–209. https://doi.org/10.2106/JBJS.H.01728
Charles YP, Daures J-P, de Rosa V, Dimeglio A (2006) Progression risk of idiopathic juvenile scoliosis during pubertal growth. Spine (Phila Pa 1976) 31:1933–1942. https://doi.org/10.1097/01.brs.0000229230.68870.97
Lonstein JE, Carlson JM (1984) The prediction of curve progression in untreated idiopathic scoliosis during growth. J Bone Joint Surg Am 66:1061–1071
Green DW, Lawhorne TW, Widmann RF et al (2011) Long-term magnetic resonance imaging follow-up demonstrates minimal transitional level lumbar disc degeneration after posterior spine fusion for adolescent idiopathic scoliosis. Spine (Phila Pa 1976) 36:1948–1954. https://doi.org/10.1097/BRS.0b013e3181ff1ea9
Kepler CK, Meredith DS, Green DW, Widmann RF (2012) Long-term outcomes after posterior spine fusion for adolescent idiopathic scoliosis. Curr Opin Pediatr 24:68–75. https://doi.org/10.1097/MOP.0b013e32834ec982
Danielsson AJ, Nachemson AL (2003) Back pain and function 22 years after brace treatment for adolescent idiopathic scoliosis: a case-control study-part I. Spine (Phila Pa 1976) 28:2078–2085. https://doi.org/10.1097/01.BRS.0000084268.77805.6F ((discussion 2086))
Danielsson AJ, Romberg K, Nachemson AL (2006) Spinal range of motion, muscle endurance, and back pain and function at least 20 years after fusion or brace treatment for adolescent idiopathic scoliosis: a case-control study. Spine (Phila Pa 1976) 31:275–283. https://doi.org/10.1097/01.brs.0000197652.52890.71
Samdani AF, Ames RJ, Kimball JS et al (2015) Anterior vertebral body tethering for immature adolescent idiopathic scoliosis: one-year results on the first 32 patients. Eur spine J Off Publ Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cerv Spine Res Soc 24:1533–1539. https://doi.org/10.1007/s00586-014-3706-z
Newton PO, Kluck DG, Saito W et al (2018) Anterior spinal growth tethering for skeletally immature patients with scoliosis: a retrospective look two to four years postoperatively. J Bone Joint Surg Am 100:1691–1697. https://doi.org/10.2106/JBJS.18.00287
Pehlivanoglu T, Oltulu I, Ofluoglu E et al (2020) Thoracoscopic vertebral body tethering for adolescent idiopathic scoliosis: a minimum of 2 years’ results of 21 patients. J Pediatr Orthop. https://doi.org/10.1097/BPO.0000000000001590
Nault M-L, Parent S, Phan P et al (2010) A modified Risser grading system predicts the curve acceleration phase of female adolescent idiopathic scoliosis. J Bone Joint Surg Am 92:1073–1081. https://doi.org/10.2106/JBJS.H.01759
Sanders JO, Browne RH, McConnell SJ et al (2007) Maturity assessment and curve progression in girls with idiopathic scoliosis. J Bone Joint Surg Am 89:64–73. https://doi.org/10.2106/JBJS.F.00067
Peterson LE, Nachemson AL (1995) Prediction of progression of the curve in girls who have adolescent idiopathic scoliosis of moderate severity. Logistic regression analysis based on data from The Brace Study of the Scoliosis Research Society. J Bone Joint Surg Am 77:823–827. https://doi.org/10.2106/00004623-199506000-00002
Danielsson AJ, Hasserius R, Ohlin A, Nachemson AL (2007) A prospective study of brace treatment versus observation alone in adolescent idiopathic scoliosis: a follow-up mean of 16 years after maturity. Spine (Phila Pa 1976) 32:2198–2207. https://doi.org/10.1097/BRS.0b013e31814b851f
Karol LA, Virostek D, Felton K, Wheeler L (2016) Effect of compliance counseling on brace use and success in patients with adolescent idiopathic scoliosis. J Bone Joint Surg Am 98:9–14. https://doi.org/10.2106/JBJS.O.00359
Karol LA, Virostek D, Felton K et al (2016) the effect of the risser stage on bracing outcome in adolescent idiopathic scoliosis. J Bone Joint Surg Am 98:1253–1259. https://doi.org/10.2106/JBJS.15.01313
Weinstein SL, Dolan LA, Wright JG, Dobbs MB (2013) Effects of bracing in adolescents with idiopathic scoliosis. N Engl J Med 369:1512–1521. https://doi.org/10.1056/NEJMoa1307337
D’Amato CR, Griggs S, McCoy B (2001) Nighttime bracing with the Providence brace in adolescent girls with idiopathic scoliosis. Spine (Phila Pa 1976) 26:2006–2012
Schwieger T, Campo S, Weinstein SL et al (2016) Body image and quality-of-life in untreated versus brace-treated females with adolescent idiopathic scoliosis. Spine (Phila Pa 1976) 41:311–319. https://doi.org/10.1097/BRS.0000000000001210
Danielsson AJ, Hasserius R, Ohlin A, Nachemson AL (2012) Body appearance and quality of life in adult patients with adolescent idiopathic scoliosis treated with a brace or under observation alone during adolescence. Spine (Phila Pa 1976) 37:755–762. https://doi.org/10.1097/BRS.0b013e318231493c
Newton PO, Farnsworth CL, Faro FD et al (2008) Spinal growth modulation with an anterolateral flexible tether in an immature bovine model: disc health and motion preservation. Spine (Phila Pa 1976) 33:724–733. https://doi.org/10.1097/BRS.0b013e31816950a0
Newton PO, Fricka KB, Lee SS et al (2002) Asymmetrical flexible tethering of spine growth in an immature bovine model. Spine (Phila Pa 1976) 27:689–693
Braun JT, Ogilvie JW, Akyuz E et al (2004) Fusionless scoliosis correction using a shape memory alloy staple in the anterior thoracic spine of the immature goat. Spine (Phila Pa 1976) 29:1980–1989
Lenke LG, Dobbs MB (2007) Management of juvenile idiopathic scoliosis. J Bone Joint Surg Am 89(Suppl 1):55–63. https://doi.org/10.2106/JBJS.F.00644
Newton PO, Yaszay B, Upasani VV et al (2010) Preservation of thoracic kyphosis is critical to maintain lumbar lordosis in the surgical treatment of adolescent idiopathic scoliosis. Spine (Phila Pa 1976) 35:1365–1370. https://doi.org/10.1097/BRS.0b013e3181dccd63
Yu E, Khan SN (2014) Does less invasive spine surgery result in increased radiation exposure? A systematic review. Clin Orthop Relat Res 472:1738–1748. https://doi.org/10.1007/s11999-014-3503-3
Hayda RA, Hsu RY, DePasse JM, Gil JA (2018) Radiation Exposure and Health Risks for Orthopaedic Surgeons. J Am Acad Orthop Surg 26:268–277. https://doi.org/10.5435/JAAOS-D-16-00342
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest and nothing to disclose. These authors, their immediate family, and any research foundation with which they are affiliated did not receive any financial payments or other benefits from any commercial entity related to the subject of this article. These authors meets each of the authorship requirements as stated in the Uniform Requirements for Manuscripts Submitted to Biomedical Journals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pehlivanoglu, T., Oltulu, I., Erdag, Y. et al. Double-sided vertebral body tethering of double adolescent idiopathic scoliosis curves: radiographic outcomes of the first 13 patients with 2 years of follow-up. Eur Spine J 30, 1896–1904 (2021). https://doi.org/10.1007/s00586-021-06745-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-06745-z