Abstract
Purpose
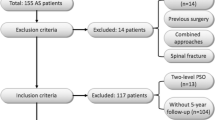
To compare the surgical outcomes between ankylosing spondylitis (AS)-related thoracolumbar kyphosis patients with the lowest instrumented vertebra (LIV) at S1 or above following one-level pedicle subtraction osteotomy (PSO).
Methods
One hundred and two AS patients undergoing one-level PSO with a minimum of 2-year follow-up were included. Twenty-two patients were in group S1 (LIV at S1), and eighty were in group non-S1 (LIV above S1). Radiographic parameters including lumbar lordosis (LL), sacral slope (SS), pelvic incidence (PI), and sagittal vertical axis (SVA) were measured. Oswestry Disability Index (ODI) and visual analog scale (VAS) were applied for clinical assessment.
Results
In both S1 and non-S1 groups, the radiographic parameters and clinical outcomes were significantly improved after surgery (P < 0.05). Patients undergoing distal fusion to S1 had significantly larger preoperative PI–LL mismatch, SVA, and smaller preoperative LL and SS compared to those in group non-S1 (P < 0.05). No significant difference was found between the two groups regarding preoperative and final follow-up ODI and VAS (P > 0.05), as well as the improvement in ODI and VAS (P > 0.05). The incidence of overall complications and each type of complication including the implant failure was similar between group S1 and non-S1 (P > 0.05).
Conclusion
Selecting S1 as the LIV without pelvic fixation following one-level PSO in thoracolumbar kyphosis caused by AS could achieve satisfactory surgical outcomes and might not increase the complications. Patients with relatively severe sagittal imbalance, loss of LL, PI–LL mismatch, and small SS might be the potential candidates for distal fusion to S1 following one-level PSO.



Similar content being viewed by others
References
Park JS, Kim YH, Yang JH et al (2019) Psychological changes and employment outcomes after kyphosis correction in patients with ankylosing spondylitis. Spine (Phila Pa 1976) 44(14):996–1002
Qian BP, Huang JC, Qiu Y et al (2018) Complications of spinal osteotomy for thoracolumbar kyphosis secondary to ankylosing spondylitis in 342 patients: incidence and risk factors. J Neurosurg Spine 30(1):91–98
Park YS, Kim HS, Baek SW (2014) Spinal osteotomy in ankylosing spondylitis: radiological, clinical, and psychological results. Spine J 14(9):1921–1927
Park JS, Kim J, Joo IH et al (2018) Analysis of risk factors for sagittal translation after pedicle subtraction osteotomy in patients with ankylosing spondylitis. Spine J 18(8):1356–1362
Kim KT, Jo DJ, Lee SH et al (2012) Does it need to perform anterior column support after Smith-Petersen osteotomy for ankylosing spondylitis? Eur Spine J 21(5):985–991
Hua WB, Zhang YK, Gao Y et al (2017) Analysis of sagittal parameters in patients undergoing one- or two-level closing wedge osteotomy for correcting thoracolumbar kyphosis secondary to ankylosing spondylitis. Spine (Phila Pa 1976) 42(14):E848–E854
Qian BP, Wang XH, Qiu Y et al (2012) The influence of closing-opening wedge osteotomy on sagittal balance in thoracolumbar kyphosis secondary to ankylosing spondylitis: a comparison with closing wedge osteotomy. Spine (Phila Pa 1976) 37(16):1415–1423
Debarge R, Demey G, Roussouly P (2010) Radiological analysis of ankylosing spondylitis patients with severe kyphosis before and after pedicle subtraction osteotomy. Eur Spine J 19(1):65–70
Kim KT, Suk KS, Cho YJ et al (2002) Clinical outcome results of pedicle subtraction osteotomy in ankylosing spondylitis with kyphotic deformity. Spine(Phila Pa 1976) 27(6):612–618
Qiao M, Qian BP, Zhao SZ et al (2018) Clinical and radiographic results after posterior wedge osteotomy for thoracolumbar kyphosis secondary to ankylosing spondylitis: comparison of long and short segment. World Neurosurg 117:e475–e482
Edwards CC 2nd, Bridwell KH, Patel A et al (2004) Long adult deformity fusions to L5 and the sacrum. A matched cohort analysis. Spine (Phila Pa 1976) 29(18):1996–2005
Shen FH, Mason JR, Shimer AL et al (2013) Pelvic fixation for adult scoliosis. Eur Spine J 22(Suppl 2):S265–S275
Saigal R, Lau D, Wadhwa R et al (2014) Unilateral versus bilateral iliac screws for spinopelvic fixation: are two screws better than one? Neurosurg Focus 36(5):E10
Jia F, Wang G, Liu X et al (2020) Comparison of long fusion terminating at L5 versus the sacrum in treating adult spinal deformity: a meta-analysis. Eur Spine J 29(1):24–35
Cho KJ, Suk SI, Park SR et al (2009) Arthrodesis to L5 versus S1 in long instrumentation and fusion for degenerative lumbar scoliosis. Eur Spine J 18(4):531–537
Eck KR, Bridwell KH, Ungacta FF et al (2001) Complications and results of long adult deformity fusions down to L4, L5, and the sacrum. Spine (Phila Pa 1976) 26(9):E182–E192
Swamy G, Berven SH, Bradford DS (2007) The selection of L5 versus S1 in long fusions for adult idiopathic scoliosis. Neurosurg Clin N Am 18(2):281–288
Yao Z, Zheng G, Zhang Y et al (2016) Selection of lowest instrumented vertebra for thoracolumbar kyphosis in ankylosing spondylitis. Spine (Phila Pa 1976) 41(7):591–597
Qian BP, Jiang J, Qiu Y et al (2013) Radiographical predictors for postoperative sagittal imbalance in patients with thoracolumbar kyphosis secondary to ankylosing spondylitis after lumbar pedicle subtraction osteotomy. Spine (Phila Pa 1976) 38(26):E1669–E1675
Vialle R, Levassor N, Rillardon L et al (2005) Radiographic analysis of the sagittal alignment and balance of the spine in asymptomatic subjects. J Bone Joint Surg Am 87(2):260–267
Qian BP, Jiang J, Qiu Y et al (2014) The presence of a negative sacral slope in patients with ankylosing spondylitis with severe thoracolumbar kyphosis. J Bone Joint Surg Am 96(22):e188
Linhares D, Cacho Rodrigues P, Ribeiro da Silva M et al (2019) Minimum of 10-year follow-up of V-rod technique in lumbar spondylolysis. Eur Spine J 28(7):1743–1749
Daubs MD, Lenke LG, Cheh G et al (2007) Adult spinal deformity surgery: complications and outcomes in patients over age 60. Spine (Phila Pa 1976) 32(20):2238–2244
Charosky S, Guigui P, Blamoutier A et al (2012) Complications and risk factors of primary adult scoliosis surgery: a multicenter study of 306 patients. Spine(Phila Pa 1976) 37(8):693–700
Mok JM, Cloyd JM, Bradford DS et al (2009) Reoperation after primary fusion for adult spinal deformity: rate, reason, and timing. Spine (Phila Pa 1976) 34(8):832–839
Weistroffer JK, Perra JH, Lonstein JE et al (2008) Complications in long fusions to the sacrum for adult scoliosis: minimum five-year analysis of fifty patients. Spine (Phila Pa 1976) 33(13):1478–1483
Yasuda T, Hasegawa T, Yamato Y et al (2016) Lumbosacral junctional failures after long spinal fusion for adult spinal deformity-which vertebra is the preferred distal instrumented vertebra? Spine Deform 4(5):378–384
Murayama H, Liang J, Bennett JM et al (2015) Trajectories of body mass index and their associations with mortality among older Japanese: do they differ from those of western populations? Am J Epidemiol 182(7):597–605
Donnelly S, Doyle DV, Denton A et al (1994) Bone mineral density and vertebral compression fracture rates in ankylosing spondylitis. Ann Rheum Dis 53(2):117–121
Acknowledgements
Bang-ping Qian has received funding from Jiangsu Provincial Medical Talent Program (ZDRCA2016068). Yong Qiu has received funding from the Jiangsu Provincial Key Medical Center (YXZXA2016009). This study was approved by the University Institutional Review Board.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Huang, Jc., Diao, Wy., Qian, Bp. et al. Can fusion to S1 maintain favorable surgical outcomes following one-level pedicle subtraction osteotomy in patients with thoracolumbar kyphosis secondary to ankylosing spondylitis?. Eur Spine J 29, 3028–3037 (2020). https://doi.org/10.1007/s00586-020-06538-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06538-w