Abstract
Purpose
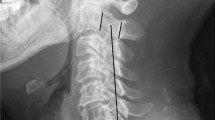
The K-line, which is a virtual line that connects the midpoints of the anteroposterior diameter of the spinal canal at C2 and C7 in a plain lateral radiogram, is a useful preoperative predictive indicator for sufficient decompression by laminoplasty (LMP) for ossification of the posterior longitudinal ligament (OPLL). K-line is defined as (+) when the peak of OPLL does not exceed the K-line, and is defined as (–) when the peak of OPLL exceeds the K-line. For patients with K-line (–) OPLL, LMP often results in poor outcome. The aim of the present study was to compare the clinical outcome of LMP, posterior decompression with instrumented fusion (PDF) and anterior decompression and fusion (ADF) for patients with K-line (–) OPLL.
Methods
The present study included patients who underwent surgical treatment including LMP, PDF and ADF for K-line (–) cervical OPLL. We retrospectively compared the clinical outcome of those patients in terms of Japanese Orthopedic Association score (JOA score) recovery rate.
Results
JOA score recovery rate was significantly higher in the ADF group compared with that in the LMP group and the PDF group. The JOA score recovery rate in the PDF group was significantly higher than that in the LMP group.
Conclusions
LMP should not be used for K-line (–) cervical OPLL. ADF is one of the suitable surgical treatments for K-line (–) OPLL. Both ADF and PDF are applicable for K-line (–) OPLL according to indications set by each institute and surgical decisions.


Similar content being viewed by others
References
Smith ZA, Buchanan CC, Raphael D et al (2011) Ossification of the posterior longitudinal ligament: pathogenesis, management, and current surgical approaches. a review. Neurosurg Focus 30:E10. doi:10.3171/2011.1.FOCUS10256
Matsumoto M, Chiba K, Toyama Y (2012) Surgical treatment of ossification of the posterior longitudinal ligament and its outcomes: posterior surgery by laminoplasty. Spine (Phila Pa 1976) 37:E303–E308
Ogawa Y, Toyama Y, Chiba K et al (2004) Long-term results of expansive open-door laminoplasty for ossification of the posterior longitudinal ligament of the cervical spine. J Neurosurg Spine 1:168–174
Mizuno J, Nakagawa H (2006) Ossified posterior longitudinal ligament: management strategies and outcomes. Spine J 6(Suppl):282S–288S
An HS, Al-Shihabi L, Kurd M (2014) Surgical treatment for ossification of the posterior longitudinal ligament in the cervical spine. J Am Acad Orthop Surg 22:420–429
Sodeyama T, Goto S, Mochizuki M et al (1999) Effect of decompression enlargement laminoplasty for posterior shifting of the spinal cord. Spine (Phila Pa 1976) 24:1527–1531
Iwasaki M, Okuda S, Miyauchi A et al (2007) Surgical strategy for cervical myelopathy due to ossification of the posterior longitudinal ligament: Part 1: Clinical results and limitations of laminoplasty. Spine (Phila Pa 1976) 32:647–653
Ogawa Y (2009) Updates on ossification of posterior longitudinal ligament. Clinical results and problems of posterior decompression for OPLL of the cervical spine. Clin Calcium 19:1493–1498 (In Japanese)
Nishida N, Kanchiku T, Kato Y et al (2014) Biomechanical analysis of cervical myelopathy due to ossification of the posterior longitudinal ligament: effects of posterior decompression and kyphosis following decompression. Exp Ther Med 7:1095–1099
Liu H, Li Y, Chen Y et al (2013) Cervical curvature, spinal cord MRIT2 signal, and occupying ratio impact surgical approach selection in patients with ossification of the posterior longitudinal ligament. Eur Spine J 22:1480–1488
Li H, Dai LY (2011) A systematic review of complications in cervical spine surgery for ossification of the posterior longitudinal ligament. Spine J 11:1049–1057
Fujiyoshi T, Yamazaki M, Kawabe J et al (2008) A new concept for making decisions regarding the surgical approach for cervical ossification of the posterior longitudinal ligament: the K-line. Spine (Phila Pa 1976) 33:E990–E993
Masaki Y, Yamazaki M, Okawa A et al (2007) An analysis of factors causing poor surgical outcome in patients with cervical myelopathy due to ossification of the posterior longitudinal ligament: anterior decompression with spinal fusion versus laminoplasty. J Spinal Disord Tech 20:7–13
Azuma Y, Kato Y, Taguchi T (2010) Etiology of cervical myelopathy induced by ossification of the posterior longitudinal ligament: determining the responsible level of OPLL myelopathy by correlating static compression and dynamic factors. J Spinal Disord Tech 23:166–169
Nishida N, Kanchiku T, Kato Y, et al (2014) Cervical ossification of the posterior longitudinal ligament: Biomechanical analysis of the influence of static and dynamic factors. J Spinal Cord Med [Epub ahead of print]
Maruo K, Moriyama T, Tachibana T et al (2014) The impact of dynamic factors on surgical outcomes after double-door laminoplasty for ossification of the posterior longitudinal ligament of the cervical spine. J Neurosurg Spine 21:938–943
Fujiyoshi T, Yamazaki M, Okawa A et al (2011) Outcome of posterior decompression surgery for cervical OPLL patients of the K-line (-) group: laminoplasty versus posterior decompression with instrumented fusion. J Spine Res 2:231–235
Hirabayashi K, Toyama Y (1997) Choice of surgical procedure for cervical ossification of the posterior longitudinal ligaments. In: Yonenobu K, Sakou T, Ono K (eds) Ossification of the posterior longitudinal ligament. Springer-Verlag, Tokyo p 135–42
Japanese Orthopaedic Association (1994) Scoring system for cervical myelopathy. Nippon Seikeigeka Gakkai Zasshi 68:490–503 (in Japanese)
Fujimori T, Iwasaki M, Okuda S et al (2014) Long-term results of cervical myelopathy due to ossification of the posterior longitudinal ligament with an occupying ratio of 60% or more. Spine (Phila Pa 1976) 39:58–67
Kim B, Yoon do H, Shin HC et al (2015) Surgical outcome and prognostic factors of anterior decompression and fusion for cervical compressive myelopathy due to ossification of the posterior longitudinal ligament. Spine J 15:875–884
Sakai K, Okawa A, Takahashi M et al (2012) Five-year follow-up evaluation of surgical treatment for cervical myelopathy caused by ossification of the posterior longitudinal ligament: a prospective comparative study of anterior decompression and fusion with floating method versus laminoplasty. Spine (Phila Pa 1976) 37:367–376
Mochizuki M, Aiba A, Hashimoto M et al (2009) Cervical myelopathy in patients with ossification of the posterior longitudinal ligament. J Neurosurg Spine 10:122–128
Chen Y, Yang L, Liu Y et al (2014) Surgical results and prognostic factors of anterior cervical corpectomy and fusion for ossification of the posterior longitudinal ligament. PLoS One 9:e102008. doi:10.1371/journal.pone.0102008
Kimura A, Seichi A, Hoshino Y et al (2012) Perioperative complications of anterior cervical decompression with fusion in patients with ossification of the posterior longitudinal ligament: a retrospective, multi-institutional study. J Orthop Sci 17:667–672
Yang H, Yang L, Chen D, Wang X, Lu X, Yuan W (2015) Implications of different patterns of “double-layer sign” in cervical ossification of the posterior longitudinal ligament. Eur Spine J 24:1631–1639
Yang H, Lu X, Wang X et al (2015) A new method to determine whether ossified posterior longitudinal ligament can be resected completely and safely: spinal canal “Rule of Nine” on axial computed tomography. Eur Spine J 24:1673–1680
Goel A, Nadkarni T, Shah A, Rai S, Rangarajan V, Kulkarni A (2015) Is Only Stabilization the Ideal Treatment for Ossified Posterior Longitudinal Ligament? Report of Early Results with a Preliminary Experience in 14 Patients. World Neurosurg 84:813–819
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest about the present manuscript.
Rights and permissions
About this article
Cite this article
Koda, M., Mochizuki, M., Konishi, H. et al. Comparison of clinical outcomes between laminoplasty, posterior decompression with instrumented fusion, and anterior decompression with fusion for K-line (–) cervical ossification of the posterior longitudinal ligament. Eur Spine J 25, 2294–2301 (2016). https://doi.org/10.1007/s00586-016-4555-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4555-8