Abstract
Background context
Although pain is generally regarded as originating in the lumbar spine, it has been estimated that in 15–30 % of patients, LBP originates from the sacroiliac joint (SIJ).
Purpose
To determine whether sacroiliac joint fusion (SIJF) for LBP is effective in reducing pain when the SIJ is known to be the pain generator.
Study design/setting
Systematic review and meta-analysis.
Methods
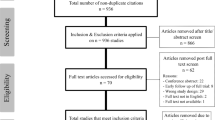
A systematic literature review and meta-analysis was performed of observational studies describing outcome of SIJF in patients with LBP. Outcome measures were VAS pain, ODI, SF-36 PCS/MCS and Majeed score. The following databases were searched: PubMed, Web of Science, Embase, Medline and Google scholar. The methodological quality of selected studies was assessed using the National Heart Lung and Blood Institute case series quality assessment tool. Meta-analysis was used to combine the studies for each outcome and forest plots were prepared. Outcomes were expressed as mean difference (MD).
Results
Six studies were included in the meta-analysis with a mean follow-up of 17.6 months. All outcomes showed statistical and clinical improvement (VAS pain MD: 54.8; 95 % CI 48.6, 61.0; n = 380; p < 0.001, ODI MD: 14.5; 95 % CI 8.4, 20.6; n = 102; p < 0.001, SF-36 PCS MD: -19.5; 95 % CI -24.7, -14.2; n = 140; p < 0.001, SF-36 MCS MD: −8.5; 95 % CI −12.9, −4.1; n = 198; p < 0.001 and Majeed score MD: −35.4; 95 % CI −48.5, −22.2; n = 140; p < 0.001).
Conclusions
SIJF appears to be a satisfactory procedure for alleviating pelvic girdle pain.






Similar content being viewed by others
References
Schwarzer AC, Aprill CN, Bogduck M (1995) The sacroiliac joint in chronic low back pain. Spine 20:31–37
Vleeming A, Albert HB, Ostgaard HC et al (2008) European guidelines for the diagnosis and treatment of pelvic girdle pain. Eur Spine J 17(6):794–819
Schutz A, Grob D (2006) Poor outcome following bilateral sacroiliac joint fusion for degenerative sacroiliac joint syndrome. Acta Orthop Belg 72:296–308
Kibsgard TJ, Roise O, Stug B (2014) Pelvic joint fusions in patients with severe pelvic girdle pain—a prospective single-subject research design study. BMC Musculoskelet Disord 15:85
Sachs D, Capobianco R (2013) Minimally invasive sacroiliac joint fusion: one year outcomes in 40 patients. Adv Orthop 2013:536128
Zaidi HA, Montoure AJ, Dickman CA (2015) Surgical and clinical efficacy of sacroiliac joint fusion: a systematic review of the literature. J Neurosurg Spine 23:59–66
Higgins JPT, Green S (eds) (2009) Cochrane handbook for systematic reviews of interventions. Wiley-Blackwell, Chichester
Majeed SA (1989) Grading the outcome of pelvic fractures. J Bone Joint Surg [Br] 71:304–306
RefWorks [computer program]. Version 2. http://www.refworks.com
The National Heart Lung and Blood Institute. Quality assessment tool for case series studies. Available at http://www.nhlbi.nih.gov/health-pro/guidelines/in-develop/cardiovascular-risk-reduction/tools/case_series. Accessed Oct 2014
RevMan [computer program]. Version 5.2.11, Nordic Cochrane Center, Copenhagen, 2013
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range and the size of the sample. BMC Med Res Methodol 5(1):13–20
Headrick TC (2010) Statistical simulation: power method polynomials and other transformations. Chapman & Hall/CRC, Boca Raton, p 137
Duhon BS, Cher DJ, Wine KD et al (2013) Safety and 6-month effectiveness of minimally invasive sacroiliac joint fusion: a prospective study. Med Dev Evid Res 6:219–229
Mason LW, Chopra I (2013) The percutaneous stabilisation of the sacroiliac joint with hollow modular anchorage screws: a prospective outcome study. Euro Spine J 22:2325–2331
Rudolf L, Capobianco R (2014) Five year clinical and radiographic outcomes after minimally invasive sacroiliac joint fusion using triangular implants. Open Orthop J 8:375–383
Sachs D, Capobianco R, Cher D et al (2014) One year outcomes after minimally invasive sacroiliac joint fusion with a series of triangular implants: a multicenter patient level analysis. Med Dev Evid Res 7:299–304
Khurana A, Guha AR, Mohanty K et al (2009) Percutaneous fusion of the sacroiliac joint with hollow modular anchorage screws. J Bone Joint Surg 91:627–631
Ledonio CGT, Polly DW Jr, Swiontkowski MF (2014) Minimally invasive versus open sacroiliac joint fusion. Clin Orthop Relat Res 472:1831–1838
Stuber KJ (2007) Specificity, sensitivity and predictive values of clinical tests of the sacroiliac joint; a systematic review of the literature. J Can Chiropr Assoc 51(1):30–41
Berthelot JM, Labat JJ, Le Goff B et al (2006) Provocative sacroiliac joint maneuvers and sacroiliac joint block are unreliable for diagnosing sacroiliac joint pain. Joint Bone Spine 73(1):7–23
Tofuku K, Koga H, Komiya S (2015) The diagnostic value of single-photon emission computed tomography/computed tomography for severe joint dysfunction. Euro Spine J 24:859–863
Sembrano JN, Polly DW Jr (2009) How often is low back pain not coming form the back? Spine 34:E27–E32
Maigne JY, Planchon CA (2005) Sacroiliac joint pain after lumbar fusion. A study with anesthetic blocks. Eur Spine J 14:654–658
Wise CL, Dall BE (2008) Minimally invasive sacroiliac arthrodesis: outcomes of a new technique. J Spinal Disord Tech 21:579–584
Slinkard N, Agel J, Swiontkowski MF (2013) Documenation of outcomes for sacroiliac joint fusion: does prior spinal fusion influence outcome? Eur Spine J 22:2318–2324
Kibsgard TJ, Roise O, Sudmann E (2013) Pelvic joint fusions in patients with chronic pelvic girdle pain: a 23-year follow-up. Eur Spine J 22:871–877
Cummings J Jr, Capobianco RA (2013) Minimally invasive sacroiliac joint fusion: one year outcomes in 18 patients. Ann Surg Innov Res 7:12
Hägg O, Fritzell P, Nordwall A (2003) The clinical importance of changes in outcome scores after treatment for chronic low back pain. Eur Spine J 12:12–20
Ostelo RW, de Vet HC (2005) Clinically important outcomes in low back pain. Best Pract Res Clin Rheumatol 19:593–607
Vianin M (2008) Psychometric properties and clinical usefulness of the Oswestry Disabiity Index. J Chiropr Med 7:161–163
Copay AG, Glassman SD, Subach BR (2008) Minimum clinically important difference in lumbar spine surgery patients: a choice of methods using the Oswestry Disability Index, Medical Outcomes Study questionnaire Short Form 36, and pain scales. Spine J 8:968–974
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Lingutla, K.K., Pollock, R. & Ahuja, S. Sacroiliac joint fusion for low back pain: a systematic review and meta-analysis. Eur Spine J 25, 1924–1931 (2016). https://doi.org/10.1007/s00586-016-4490-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4490-8