Abstract
Purpose
The optimal surgical technique for multilevel cervical degenerative disc diseases (DDD) remains controversial. Hybrid surgery (HS) incorporating anterior cervical discectomy and fusion (ACDF) and cervical disc replacement (CDR) is increasingly performed for cervical DDD. This study aims to evaluate the biomechanical and clinical evidence available for HS and to provide a systematic review of current understanding of HS.
Methods
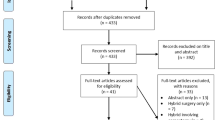
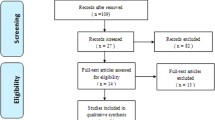
This systematic review was undertaken by following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses Statement. Multiple databases and online registers of clinical trials were searched up to February 2014. The biomechanical and clinical studies on HS for cervical DDD written in English were included. Two authors independently assessed methodological quality and extracted data.
Results
Fifteen studies including eight biomechanical studies and seven clinical studies were indentified. The biomechanical studies showed that HS was benefit to motion preservation of the operative levels and revealed less adverse effect on adjacent segments. All clinical studies demonstrated improvement in validated functional scores after HS. Segment motion and immobilization were achieved at the arthroplasty level and arthrodesis level, respectively. Postoperative assessments and complication rate were similar or in favor of HS when comparing with ACDF or CDR. However, the overall quality of evidence for HS was low to very low.
Conclusions
There is a paucity of high quality evidence for HS. HS may be a safe and efficacious technique to benefit a select group of multilevel cervical DDD, which is needed to be confirmed by further prospective, randomized controlled trials.


Similar content being viewed by others
References
Fay LY, Huang WC, Tsai TY, Wu JC, Ko CC, Tu TH, Wu CL, Cheng H (2013) Differences between arthroplasty and anterior cervical fusion in two-level cervical degenerative disc disease. Eur Spine J 23(3):627–634
Zechmeister I, Winkler R, Mad P (2011) Artificial total disc replacement versus fusion for the cervical spine: a systematic review. Eur Spine J 20(2):177–184
Dmitriev AE, Kuklo TR, Lehman RA Jr, Rosner MK (2007) Stabilizing potential of anterior, posterior, and circumferential fixation for multilevel cervical arthrodesis: an in vitro human cadaveric study of the operative and adjacent segment kinematics. Spine 32(6):E188–E196
Lopez-Espina CG, Amirouche F, Havalad V (2006) Multilevel cervical fusion and its effect on disc degeneration and osteophyte formation. Spine 31(9):972–978
Matsunaga S, Kabayama S, Yamamoto T, Yone K, Sakou T, Nakanishi K (1999) Strain on intervertebral discs after anterior cervical decompression and fusion. Spine 24(7):670–675
Schwab JS, Diangelo DJ, Foley KT (2006) Motion compensation associated with single-level cervical fusion: where does the lost motion go? Spine 31(21):2439–2448
Cepoiu-Martin M, Faris P, Lorenzetti D, Prefontaine E, Noseworthy T, Sutherland L (2011) Artificial cervical disc arthroplasty: a systematic review. Spine 36(25):E1623–E1633
Cason GW, Herkowitz HN (2013) Cervical intervertebral disc replacement. J Bone Joint Surg Am 95(3):279–285
Fallah A, Akl EA, Ebrahim S, Ibrahim GM, Mansouri A, Foote CJ, Zhang Y, Fehlings MG (2012) Anterior cervical discectomy with arthroplasty versus arthrodesis for single-level cervical spondylosis: a systematic review and meta-analysis. PLoS One 7(8):e43407
Kepler CK, Brodt ED, Dettori JR, Albert TJ (2012) Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review comparing multilevel versus single-level surgery. Evid Based Spine Care J 3(S1):19–30
Park DH, Ramakrishnan P, Cho TH, Lorenz E, Eck JC, Humphreys SC, Lim TH (2007) Effect of lower two-level anterior cervical fusion on the superior adjacent level. J Neurosurg Spine 7(3):336–340
Prasarn ML, Baria D, Milne E, Latta L, Sukovich W (2012) Adjacent-level biomechanics after single versus multilevel cervical spine fusion. J Neurosurg Spine 16(2):172–177
Shin DA, Yi S, Yoon do H, Kim KN, Shin HC (2009) Artificial disc replacement combined with fusion versus two-level fusion in cervical two-level disc disease. Spine 34(11):1153–1159 discussion 1160–1161
Auerbach JD, Jones KJ, Fras CI, Balderston JR, Rushton SA, Chin KR (2008) The prevalence of indications and contraindications to cervical total disc replacement. Spine J 8(5):711–716
Barbagallo GM, Assietti R, Corbino L, Olindo G, Foti PV, Russo V, Albanese V (2009) Early results and review of the literature of a novel hybrid surgical technique combining cervical arthrodesis and disc arthroplasty for treating multilevel degenerative disc disease: opposite or complementary techniques? Eur Spine J 18(Suppl 1):29–39
Hey HW, Hong CC, Long AS, Hee HT (2013) Is hybrid surgery of the cervical spine a good balance between fusion and arthroplasty? Pilot results from a single surgeon series. Eur Spine J 22(1):116–122
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6:e1000100
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73(9):712–716
Higgins JPT, Green S (2011) Cochrane handbook for systematic reviews of interventions version 5.1.0 (updated March 2011). The Cochrane Collaboration. Available from www. cochrane-handbook.org
Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, Norris S, Falck-Ytter Y, Glasziou P, DeBeer H, Jaeschke R, Rind D, Meerpohl J, Dahm P, Schunemann HJ (2011) GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol 64(4):383–394
Balshem H, Helfand M, Schunemann HJ, Oxman AD, Kunz R, Brozek J, Vist GE, Falck-Ytter Y, Meerpohl J, Norris S, Guyatt GH (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol 64(4):401–406
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, Schunemann HJ (2008) GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ 336(7650):924–926
Barrey C, Campana S, Persohn S, Perrin G, Skalli W (2012) Cervical disc prosthesis versus arthrodesis using one-level, hybrid and two-level constructs: an in vitro investigation. Eur Spine J 21(3):432–442
Cho BY, Lim J, Sim HB, Park J (2010) Biomechanical analysis of the range of motion after placement of a two-level cervical ProDisc-C versus hybrid construct. Spine 35(19):1769–1776
Cunningham BW, Hu N, Zorn CM, McAfee PC (2010) Biomechanical comparison of single- and two-level cervical arthroplasty versus arthrodesis: effect on adjacent-level spinal kinematics. Spine J 10(4):341–349
Faizan A, Goel VK, Biyani A, Garfin SR, Bono CM (2012) Adjacent level effects of bi level disc replacement, bi level fusion and disc replacement plus fusion in cervical spine––a finite element based study. Clin Biomech (Bristol, Avon) 27(3):226–233
Lee MJ, Dumonski M, Phillips FM, Voronov LI, Renner SM, Carandang G, Havey RM, Patwardhan AG (2011) Disc replacement adjacent to cervical fusion: a biomechanical comparison of hybrid construct versus two-level fusion. Spine 36(23):1932–1939
Martin S, Ghanayem AJ, Tzermiadianos MN, Voronov LI, Havey RM, Renner SM, Carandang G, Abjornson C, Patwardhan AG (2011) Kinematics of cervical total disc replacement adjacent to a two-level, straight versus lordotic fusion. Spine 36(17):1359–1366
Safavi-Abbasi S, Reyes PM, Abjornson C, Crawford NR (2013) Feasibility and biomechanics of multilevel arthroplasty and combined cervical arthrodesis and arthroplasty. J Spinal Disord Tech (Epub ahead of print)
Zhao Y, Li Q, Mo Z, Sun Y, Fan Y (2013) Finite element analysis of cervical arthroplasty combined with fusion against 2-level fusion. J Spinal Disord Tech 26(6):347–350
Cardoso MJ, Mendelsohn A, Rosner MK (2011) Cervical hybrid arthroplasty with 2 unique fusion techniques. J Neurosurg Spine 15(1):48–54
Kang L, Lin D, Ding Z, Liang B, Lian K (2013) Artificial disk replacement combined with midlevel ACDF versus multilevel fusion for cervical disk disease involving 3 levels. Orthopedics 36(1):e88–e94
Lee SB, Cho KS, Kim JY, Yoo DS, Lee TG, Huh PW (2012) Hybrid surgery of multilevel cervical degenerative disc disease: review of literature and clinical results. J Korean Neurosurg Soc 52(5):452–458
Ren X, Chu T, Jiang T, Wang W, Wang J, Changqing L, Zhang Z (2012) Cervical disc replacement combined with cage fusion for the treatment of multi-level cervical disc herniation. J Spinal Disord Tech (Epub ahead of print)
Yang B, Li H, Zhang T, He X, Xu S (2012) The incidence of adjacent segment degeneration after cervical disc arthroplasty (CDA): a meta analysis of randomized controlled trials. PLoS One 7:e35032
Chang UK, Kim DH, Lee MC, Willenberg R, Kim SH, Lim J (2007) Changes in adjacent-level disc pressure and facet joint force after cervical arthroplasty compared with cervical discectomy and fusion. J Neurosurg Spine 7(1):33–39
Dmitriev AE, Cunningham BW, Hu N, Sell G, Vigna F, McAfee PC (2005) Adjacent level intradiscal pressure and segmental kinematics following a cervical total disc arthroplasty: an in vitro human cadaveric model. Spine 30(10):1165–1172
Mo ZJ, Zhao YB, Wang LZ, Sun Y, Zhang M, Fan YB (2014) Biomechanical effects of cervical arthroplasty with U-shaped disc implant on segmental range of motion and loading of surrounding soft tissue. Eur Spine J 23(3):613–621
Maldonado CV, Paz RD, Martin CB (2011) Adjacent-level degeneration after cervical disc arthroplasty versus fusion. Eur Spine J 20(Suppl 3):403–407
Song KJ, Choi BW, Jeon TS, Lee KB, Chang H (2011) Adjacent segment degenerative disease: is it due to disease progression or a fusion-associated phenomenon? Comparison between segments adjacent to the fused and non-fused segments. Eur Spine J 20(11):1940–1945
DiAngelo DJ, Roberston JT, Metcalf NH, McVay BJ, Davis RC (2003) Biomechanical testing of an artificial cervical joint and an anterior cervical plate. J Spinal Disord Tech 16(4):314–323
Hilibrand AS, Robbins M (2004) Adjacent segment degeneration and adjacent segment disease: the consequences of spinal fusion? Spine J 4(6 Suppl):190S–194S
Maiman DJ, Kumaresan S, Yoganandan N, Pintar FA (1999) Biomechanical effect of anterior cervical spine fusion on adjacent segments. Biomed Mater Eng 9(1):27–38
Eck JC, Humphreys SC, Lim TH, Jeong ST, Kim JG, Hodges SD, An HS (2002) Biomechanical study on the effect of cervical spine fusion on adjacent-level intradiscal pressure and segmental motion. Spine 27(22):2431–2434
Puttlitz CM, Rousseau MA, Xu Z, Hu S, Tay BK, Lotz JC (2004) Intervertebral disc replacement maintains cervical spine kinetics. Spine 29(24):2809–2814
Verma K, Gandhi SD, Maltenfort M, Albert TJ, Hilibrand AS, Vaccaro AR, Radcliff KE (2013) Rate of adjacent segment disease in cervical disc arthroplasty versus single-level fusion: meta-analysis of prospective studies. Spine 38(26):2253–2257
Lund T, Oxland TR (2011) Adjacent level disk disease––is it really a fusion disease? Orthop Clin North Am 42(4):529–541
Cho SK, Riew KD (2013) Adjacent segment disease following cervical spine surgery. J Am Acad Orthop Surg 21(1):3–11
Sekhon LH, Sears W, Duggal N (2005) Cervical arthroplasty after previous surgery: results of treating 24 discs in 15 patients. J Neurosurg Spine 3(5):335–341
Acknowledgments
This project was supported by the National Natural Science Foundation of China (Nos. 11120101001 and 11202017), the 111 Project (No. B13003), National Science & Technology Pillar Program (Nos. 2012BAI18B05, 2012BAI18B07 and 2012BAI22B02), Research Fund for the Doctoral Program of Higher Education of China (20131102130004).
Conflict of interest
None of the authors has any potential conflict of interest.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Z. Jia and Z. Mo have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Jia, Z., Mo, Z., Ding, F. et al. Hybrid surgery for multilevel cervical degenerative disc diseases: a systematic review of biomechanical and clinical evidence. Eur Spine J 23, 1619–1632 (2014). https://doi.org/10.1007/s00586-014-3389-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3389-5