Abstract
Background
Ferroptosis, a type of programmed cell death triggered by oxidative stress, was suspected to play a role in ulcerative colitis. Indigo naturalis is highly effective against ulcerative colitis, but its mechanism is unclear. This study found that indigo naturalis treatment suppressed ferroptosis.
Methods
We analyzed 770 mRNA expressions of patients with ulcerative colitis. Suppression of ferroptosis by indigo naturalis treatment was shown using a cell death assay. Malondialdehyde levels and reactive oxygen species were analyzed in CaCo-2 cells treated with indigo naturalis. Glutathione metabolism was shown by metabolomic analysis. Extraction of the ingredients indigo naturalis from the rectal mucosa was performed using liquid chromatograph—mass spectrometry.
Results
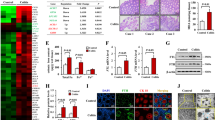
Gene expression profiling showed that indigo naturalis treatment increased antioxidant genes in the mucosa of patients with ulcerative colitis. In vitro analysis showed that nuclear factor erythroid-2-related factor 2-related antioxidant gene expression was upregulated by indigo naturalis. Indigo naturalis treatment rendered cells resistant to ferroptosis. Metabolomic analysis suggested that an increase in reduced glutathione by indigo naturalis. The protein expression of CYP1A1 and GPX4 was increased in the rectum by treatment with indigo naturalis. The main ingredients of indigo naturalis, indirubin and indigo inhibited ferroptosis. Indirubin was detected in the rectal mucosa of patients with ulcerative colitis who were treated with indigo naturalis.
Conclusions
Suppression of ferroptosis by indigo naturalis in the intestinal epithelium could be therapeutic target for ulcerative colitis. The main active ingredient of indigo naturalis may be indirubin.







Similar content being viewed by others
Abbreviations
- AHR:
-
Aryl hydrocarbon receptor
- CYP1A1:
-
Cytochrome P450 1a1
- Cys:
-
Cysteine
- DMSO:
-
Dimethyl sulfoxide
- FICZ:
-
6-Formylindolo[3, 2-b]carbazole
- GABA:
-
Gamma-aminobutyric acid
- γ-Glu-Cys:
-
Gamma-glutamylcysteine
- GCL:
-
Glutamate-cysteine ligase
- GCLC:
-
Glutamate-cysteine ligase catalytic subunit
- GCLM:
-
Glutamate-cysteine ligase modifier subunit
- GPX4:
-
Glutathione peroxidase 4
- GSH:
-
Reduced glutathione
- GSSG:
-
Glutathione disulfide
- GSTP1:
-
Pi-class glutathione S-transferase
- Gln:
-
Glutamine
- Glu:
-
Glutamic acid
- Gly:
-
Glycine
- HDAC2:
-
Histone deacetylase 2
- H2O2 :
-
Hydrogen peroxide
- HO-1:
-
Heme oxygenase-1
- IN:
-
Indigo naturalis
- LC/MS:
-
Liquid chromatography—mass spectrometry
- MDA:
-
Malondialdehyde
- NADPH:
-
Nicotinamide adenine dinucleotide phosphate
- NRF2:
-
Nuclear factor erythroid-2-related factor 2
- PRDX2:
-
Peroxiredoxin 2
- ROS:
-
Reactive oxygen species
- PCR:
-
Polymerase chain reaction
- SELENBP1:
-
Selenium binding protein 1
- SOD1:
-
Superoxide dismutase 1
- SOD2:
-
Superoxide dismutase 2
- SRXN:
-
Sulfiredoxin-1
- Ser:
-
Serine
- TCDD:
-
Tetrachlorodibenzo-para-dioxin
- TNF:
-
Tumor necrosis factor
- TXN:
-
Thioredoxin 1
- TXNR:
-
Thioredoxin reductase 1
- UC:
-
Ulcerative colitis
References
Molodecky NA, Soon IS, Rabi DM, et al. Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology. 2012;142:46-54.e42 (quiz e30).
Barnes EL, Loftus EV Jr., Kappelman MD. Effects of race and ethnicity on diagnosis and management of inflammatory bowel diseases. Gastroenterology. 2021;160:677–89.
Naganuma M, Sugimoto S, Mitsuyama K, et al. Efficacy of Indigo naturalis in a multicenter randomized controlled trial of patients with ulcerative colitis. Gastroenterology. 2018;154:935–47.
Uchiyama K, Takami S, Suzuki H, et al. Efficacy and safety of short-term therapy with indigo naturalis for ulcerative colitis: an investigator-initiated multicenter double-blind clinical trial. PLoS ONE. 2020;15: e0241337.
Matsuno Y, Torisu T, Umeno J, et al. One-year clinical efficacy and safety of indigo naturalis for active ulcerative colitis: a real-world prospective study. Intest Res. 2022;20:260–8.
Sugimoto S, Naganuma M, Kiyohara H, et al. Clinical efficacy and safety of oral Qing-Dai in patients with ulcerative colitis: a single-center open-label prospective study. Digestion. 2016;93:193–201.
Matsuno Y, Hirano A, Torisu T, et al. Short-term and long-term outcomes of indigo naturalis treatment for inflammatory bowel disease. J Gastroenterol Hepatol. 2020;35:412–7.
Saiki JP, Andreasson JO, Grimes KV, et al. Treatment-refractory ulcerative colitis responsive to indigo naturalis. BMJ Open Gastroenterol. 2021;8(1):e000813.
Naganuma M, Sugimoto S, Fukuda T, et al. Indigo naturalis is effective even in treatment-refractory patients with ulcerative colitis: a post hoc analysis from the INDIGO study. J Gastroenterol. 2020;55:169–80.
Hiraide T, Teratani T, Uemura S, et al. Pulmonary arterial hypertension caused by AhR signal activation protecting against colitis. Am J Respir Crit Care Med. 2021;203:385–8.
Naganuma M, Sugimoto S, Suzuki H, et al. Adverse events in patients with ulcerative colitis treated with indigo naturalis: a Japanese nationwide survey. J Gastroenterol. 2019;54:891–6.
Kawai S, Iijima H, Shinzaki S, et al. Indigo naturalis ameliorates murine dextran sodium sulfate-induced colitis via aryl hydrocarbon receptor activation. J Gastroenterol. 2017;52:904–19.
Bock KW. From TCDD-mediated toxicity to searches of physiologic AHR functions. Biochem Pharmacol. 2018;155:419–24.
Jena G, Trivedi PP, Sandala B. Oxidative stress in ulcerative colitis: an old concept but a new concern. Free Radic Res. 2012;46:1339–45.
Wang Z, Li S, Cao Y, et al. Oxidative stress and carbonyl lesions in ulcerative colitis and associated colorectal cancer. Oxid Med Cell Longev. 2016;2016:9875298.
Wan Y, Yang L, Jiang S, et al. Excessive apoptosis in ulcerative colitis: crosstalk between apoptosis, ROS, ER stress, and intestinal homeostasis. Inflamm Bowel Dis. 2022;28:639–48.
Dixon SJ, Lemberg KM, Lamprecht MR, et al. Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell. 2012;149:1060–72.
Xu M, Tao J, Yang Y, et al. Ferroptosis involves in intestinal epithelial cell death in ulcerative colitis. Cell Death Dis. 2020;11:86.
Qi-Yue Y, Ting Z, Ya-Nan H, et al. From natural dye to herbal medicine: a systematic review of chemical constituents, pharmacological effects and clinical applications of indigo naturalis. Chin Med. 2020;15:127.
Babicki S, Arndt D, Marcu A, et al. Heatmapper: web-enabled heat mapping for all. Nucleic Acids Res. 2016;44:W147–53.
Gillespie M, Jassal B, Stephan R, et al. The reactome pathway knowledgebase 2022. Nucleic Acids Res. 2022;50:D687–92.
Bedre R, (2020) reneshbedre/bioinfokit: Bioinformatics data analysis and visualization toolkit. Zenodo
Livak KJ, Schmittgen TD. Analysis of relative gene expression data using real-time quantitative PCR and the 2[-Delta Delta C (T)] method. Methods. 2001;25:402–8.
Ma Q. Role of nrf2 in oxidative stress and toxicity. Annu Rev Pharmacol Toxicol. 2013;53:401–26.
Wakabayashi N, Slocum SL, Skoko JJ, et al. When NRF2 talks, who’s listening? Antioxid Redox Signal. 2010;13:1649–63.
Shaw P, Chattopadhyay A. Nrf2-ARE signaling in cellular protection: mechanism of action and the regulatory mechanisms. J Cell Physiol. 2020;235:3119–30.
Yeager RL, Reisman SA, Aleksunes LM, et al. Introducing the “TCDD-inducible AhR-Nrf2 gene battery.” Toxicol Sci. 2009;111:238–46.
Singh R, Chandrashekharappa S, Bodduluri SR, et al. Enhancement of the gut barrier integrity by a microbial metabolite through the Nrf2 pathway. Nat Commun. 2019;10:89.
Tocmo R, Le B, Heun A, et al. Prenylated xanthones from mangosteen (Garcinia mangostana) activate the AhR and Nrf2 pathways and protect intestinal barrier integrity in HT-29 cells. Free Radic Biol Med. 2021;163:102–15.
Tonelli C, Chio IIC, Tuveson DA. Transcriptional regulation by Nrf2. Antioxid Redox Signal. 2018;29:1727–45.
Lu J, Holmgren A. The thioredoxin antioxidant system. Free Radic Biol Med. 2014;66:75–87.
Loboda A, Damulewicz M, Pyza E, et al. Role of Nrf2/HO-1 system in development, oxidative stress response and diseases: an evolutionarily conserved mechanism. Cell Mol Life Sci. 2016;73:3221–47.
Ramesh A, Varghese SS, Doraiswamy J, et al. Role of sulfiredoxin in systemic diseases influenced by oxidative stress. Redox Biol. 2014;2:1023–8.
Stockwell BR. Ferroptosis turns 10: Emerging mechanisms, physiological functions, and therapeutic applications. Cell. 2022;185:2401–21.
Stockwell BR, Friedmann Angeli JP, Bayir H, et al. Ferroptosis: a regulated cell death Nexus linking metabolism, redox biology, and disease. Cell. 2017;171:273–85.
Chen L, Na R, Danae McLane K, et al. Overexpression of ferroptosis defense enzyme Gpx4 retards motor neuron disease of SOD1G93A mice. Sci Rep. 2021;11:12890.
Shou Y, Yang L, Yang Y, et al. Inhibition of keratinocyte ferroptosis suppresses psoriatic inflammation. Cell Death Dis. 2021;12:1009.
Kobayashi Y, Ohfuji S, Kondo K, et al. Association between dietary iron and zinc intake and development of ulcerative colitis: a case-control study in Japan. J Gastroenterol Hepatol. 2019;34:1703–10.
Millar AD, Rampton DS, Blake DR. Effects of iron and iron chelation in vitro on mucosal oxidant activity in ulcerative colitis. Aliment Pharmacol Ther. 2000;14:1163–8.
Liu JZ, van Sommeren S, Huang H, et al. Association analyses identify 38 susceptibility loci for inflammatory bowel disease and highlight shared genetic risk across populations. Nat Genet. 2015;47:979–86.
Safe S, Jayaraman A, Chapkin RS. Ah receptor ligands and their impacts on gut resilience: structure-activity effects. Crit Rev Toxicol. 2020;50:463–73.
Yoshimatsu Y, Sujino T, Miyamoto K, et al. Aryl hydrocarbon receptor signals in epithelial cells govern the recruitment and location of Helios(+) Tregs in the gut. Cell Rep. 2022;39: 110773.
Rouse M, Singh NP, Nagarkatti PS, et al. Indoles mitigate the development of experimental autoimmune encephalomyelitis by induction of reciprocal differentiation of regulatory T cells and Th17 cells. Br J Pharmacol. 2013;169:1305–21.
Singh NP, Singh UP, Singh B, et al. Activation of aryl hydrocarbon receptor (AhR) leads to reciprocal epigenetic regulation of FoxP3 and IL-17 expression and amelioration of experimental colitis. PLoS ONE. 2011;6: e23522.
Quintana FJ, Basso AS, Iglesias AH, et al. Control of T(reg) and T(H)17 cell differentiation by the aryl hydrocarbon receptor. Nature. 2008;453:65–71.
Denison MS, Faber SC. And now for something completely different: diversity in ligand-dependent activation of Ah receptor responses. Curr Opin Toxicol. 2017;2:124–31.
Miao W, Hu L, Scrivens PJ, et al. Transcriptional regulation of NF-E2 p45-related factor (NRF2) expression by the aryl hydrocarbon receptor-xenobiotic response element signaling pathway: direct cross-talk between phase I and II drug-metabolizing enzymes. J Biol Chem. 2005;280:20340–8.
Lebwohl MG, Stein Gold L, Strober B, et al. Phase 3 trials of tapinarof cream for plaque psoriasis. N Engl J Med. 2021;385:2219–29.
Lillig CH, Berndt C, Holmgren A. Glutaredoxin systems. Biochim Biophys Acta. 2008;1780:1304–17.
Forcina GC, Dixon SJ. GPX4 at the crossroads of lipid homeostasis and ferroptosis. Proteomics. 2019;19: e1800311.
Dodson M, Castro-Portuguez R, Zhang DD. NRF2 plays a critical role in mitigating lipid peroxidation and ferroptosis. Redox Biol. 2019;23: 101107.
Yang WS, Stockwell BR. Ferroptosis: death by lipid peroxidation. Trends Cell Biol. 2016;26:165–76.
Kagan VE, Mao G, Qu F, et al. Oxidized arachidonic and adrenic PEs navigate cells to ferroptosis. Nat Chem Biol. 2017;13:81–90.
Schreiner P, Martinho-Grueber M, Studerus D, et al. Nutrition in inflammatory bowel disease. Digestion. 2020;101(Suppl 1):120–35.
de Silva PS, Olsen A, Christensen J, et al. An association between dietary arachidonic acid, measured in adipose tissue, and ulcerative colitis. Gastroenterology. 2010;139:1912–7.
Tjonneland A, Overvad K, Bergmann MM, et al. Linoleic acid, a dietary n-6 polyunsaturated fatty acid, and the aetiology of ulcerative colitis: a nested case-control study within a European prospective cohort study. Gut. 2009;58:1606–11.
Sido B, Hack V, Hochlehnert A, et al. Impairment of intestinal glutathione synthesis in patients with inflammatory bowel disease. Gut. 1998;42:485–92.
Ozawa K, Mori D, Hatanaka A, et al. Comparison of the anti-colitis activities of Qing Dai/Indigo naturalis constituents in mice. J Pharmacol Sci. 2020;142:148–56.
Stasiak N, Kukuła-Koch W, Głowniak K. Modern industrial and pharmacological applications of indigo dye and its derivatives–a review. Acta Pol Pharm. 2014;71:215–21.
Xu C, Sun S, Johnson T, et al. The glutathione peroxidase Gpx4 prevents lipid peroxidation and ferroptosis to sustain treg cell activation and suppression of antitumor immunity. Cell Rep. 2021;35: 109235.
Feuerstein JD, Isaacs KL, Schneider Y, et al. AGA clinical practice guidelines on the management of moderate to severe ulcerative colitis. Gastroenterology. 2020;158:1450–61.
Acknowledgements
We thank Ellen Knapp, PhD, from Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript. We appreciate the technical assistance from The Research Support Center, Research Center for Human Disease Modeling, Kyushu University Graduate School of Medical Sciences.
Funding
This work was supported by JSPS KAKENHI grants ‘[Grant-in-Aid for Scientific Research (C) JP21K06783 and Grant-in-Aid for Young Scientists (B) JP22K15668]’.
Author information
Authors and Affiliations
Contributions
AY, NI and TT conceived the idea of the study. AY, and TT were involved in the data analysis. JU, KK, SF, YF, YM, TM, and TT collected the clinical data and contributed to data interpretation. AYo, KM, KA, TK, and TT contributed to drafting of the manuscript and critical revision. All authors revised the manuscript, approved the manuscript to be published, and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yokote, A., Imazu, N., Umeno, J. et al. Ferroptosis in the colon epithelial cells as a therapeutic target for ulcerative colitis. J Gastroenterol 58, 868–882 (2023). https://doi.org/10.1007/s00535-023-02016-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-023-02016-4