Abstract
Background
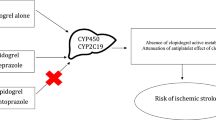
Concomitant use of antiplatelet agents and proton-pump inhibitors (PPIs) has been recommended in patients with a history of gastrointestinal (GI) hemorrhage. However, recent studies have reported that PPIs may alter clopidogrel’s pharmacokinetics and potentially lead to an increased risk of recurrent adverse cardiovascular (CV) events.
Methods
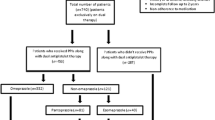
Using Taiwan’s 2000–2006 National Health Insurance database, this population-based retrospective cohort study assessed CV and GI events in patients who had a prior history of GI bleeding and had been prescribed ongoing antiplatelet therapy after acute coronary syndrome (ACS) discharge. We identified 3,580 ACS patients and categorized them into (1) those taking clopidogrel alone, (2) those taking clopidogrel plus PPIs, and (3) those taking aspirin plus PPIs. Cox proportional hazards models were used to assess the association between the use of antiplatelet therapies and CV/GI events.
Results
The clopidogrel only group and the clopidogrel plus PPI group were found to be at lower risk for GI events than the aspirin plus PPI group [adjusted hazard ratio (HR) 0.23 (95% confidence interval; CI 0.14–0.36) and HR 0.70 (0.52–0.96), respectively]. However, while the clopidogrel only group had a lower risk of CV events than the aspirin plus PPI group [HR 0.57 (0.38–0.84)], the clopidogrel plus PPI group had a significantly higher CV risk than the aspirin plus PPI group [HR 1.59 (1.18–2.13)].
Conclusions
Our findings suggest that although the use of clopidogrel plus PPIs provides GI benefits, with this treatment, there is an increased CV risk among patients with a history of GI bleeding.
Similar content being viewed by others
References
Munger MA, Hawkins DW. Atherothrombosis: epidemiology, pathophysiology, and prevention. J Am Pharm Assoc. 2003;44:S5–12.
Tran H, Anand SS. Oral antiplatelet therapy in cerebrovascular disease, coronary artery disease, and peripheral arterial disease. JAMA. 2004;292:1867–74.
Antithrombotic Trialists Collaboration. Collaborative meta-analysis of randomised trials of antiplatelet therapy for prevention of death, myocardial infarction, and stroke in high risk patients. BMJ. 2002;324:71–86.
Harrington RA, Becker RC, Ezekowitz M, Meade TW, O’Connor CM, Vorchheimer DA, et al. Antithrombotic therapy for coronary artery disease. Chest. 2004;126:513S–48S.
Anderson JL, Adams CD, Antman EM, Bridges CR, Califf RM, Casey DE Jr, et al. ACC/AHA 2007 guidelines for the management of patients with unstable angina/non-ST-elevation myocardial infarction. Circulation. 2007;116:e148–304.
Sibbing D, Morath T, Stegherr J, Braun S, Vogt W, Hadamitzky M, et al. Impact of proton pump inhibitors on the antiplatelet effects of clopidogrel. Thromb Haemost. 2009;101:714–9.
Gilard M, Arnaud B, Cornily JC, Le Gal G, Lacut K, Le Calvez G, et al. Influence of omeprazole on the antiplatelet action of clopidogrel associated with aspirin: the randomized, double-blind OCLA (Omeprazole CLopidogrel Aspirin) study. J Am Coll Cardiol. 2008;51:256–60.
Kim KA, Park PW, Hong SJ, Park JY. The effect of CYP2C19 polymorphism on the pharmacokinetics and pharmacodynamics of clopidogrel: a possible mechanism for clopidogrel resistance. Clin Pharmacol Ther. 2008;84:236–42.
Small DS, Farid NA, Payne CD, Weerakkody GJ, Li YG, Brandt JT, et al. Effects of the proton pump inhibitor lansoprazole on the pharmacokinetics and pharmacodynamics of prasugrel and clopidogrel. J Clin Pharmacol. 2008;48:475–84.
Juurlink DN, Gomes T, Ko DT, Szmitko PE, Austin PC, Tu JV, et al. A population-based study of the drug interaction between proton pump inhibitors and clopidogrel. CMAJ. 2009;180:713–8.
Ho PM, Maddox TM, Wang L, Fihn SD, Jesse RL, Peterson ED, et al. Risk of adverse outcomes associated with concomitant use of clopidogrel and proton pump inhibitors following acute coronary syndrome. JAMA. 2009;301:937–44.
Bureau of National Health Insurance. National Health Insurance in Taiwan. 2007. http://www.nhi.gov.tw/english/index.asp. Accessed 19 Dec 2009.
Gent M, Beaumont D, Blanchard J. A randomised, blinded, trial of clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE). Lancet. 1996;348:1329–39.
Chan FK, Ching JY, Hung LC, Wong VW, Leung VK, Kung NN, et al. Clopidogrel versus aspirin and esomeprazole to prevent recurrent ulcer bleeding. N Engl J Med. 2005;352:238–44.
Lai KC, Chu KM, Hui WM, Wong BC, Hung WK, Loo CK, et al. Esomeprazole with aspirin versus clopidogrel for prevention of recurrent gastrointestinal ulcer complications. Clin Gastroenterol Hepatol. 2006;4:860–5.
Yasuda H, Yamada M, Sawada S, Endo Y, Inoue K, Asano F, Takeyama Y, Yoshiba M. Upper gastrointestinal bleeding in patients receiving dual antiplatelet therapy after coronary stenting. Intern Med. 2009;48:1725–30.
Gurbel PA, Lau WC, Tantry US. Omeprazole—a possible new candidate influencing the antiplatelet effect of clopidogrel. J Am Coll Cardiol. 2008;51:261–3.
Siller-Matula JM, Spiel AO, Lang IM, Kreiner G, Christ G, Jilma B. Effects of pantoprazole and esomeprazole on platelet inhibition by clopidogrel. Am Heart J. 2009;157:148.e1–5.
Acknowledgments
The authors thank the Taiwanese Bureau of National Health Insurance and the National Health Research Institutes for use of the NHI database. The content of this article does not represent the official position of either organization, and the authors bear all responsibility for the results and their interpretation. We thank Dr. C. Daniel Mullins of the University of Maryland for providing consultation and assistance with the revised manuscript. The authors also thank James Steed of National University of Kaohsiung, Taiwan, for editing assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsai, YW., Wen, YW., Huang, WF. et al. Cardiovascular and gastrointestinal events of three antiplatelet therapies: clopidogrel, clopidogrel plus proton-pump inhibitors, and aspirin plus proton-pump inhibitors in patients with previous gastrointestinal bleeding. J Gastroenterol 46, 39–45 (2011). https://doi.org/10.1007/s00535-010-0299-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-010-0299-0