Abstract
Introduction
Concomitant cardiovascular comorbidities in patients with cancer are not uncommon. There is limited data on the impact of cardiovascular comorbidities on in-hospital mortality in patients admitted with neutropenic fever.
Methods
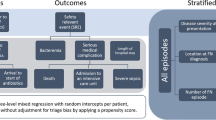
This is a retrospective cohort study using the 2016 NIS database of adults (> 18 years old) hospitalized for neutropenic fever as the primary diagnosis. The primary outcome studied is all-cause mortality in patients with neutropenic fever. ICD-10-CM codes were used to identify cardiovascular risk factors including smoking; hyperlipidemia; peripheral vascular diseases; hypertension; history of cerebrovascular disease or transient ischemic attack; and cardiovascular morbidities including atrial fibrillation, coronary artery disease, and congestive heart failure. Multivariate linear regression analysis was used to adjust for cofounders.
Results
A total of 28,060 patients were admitted with neutropenic fever in 2016. Average age was 43.9 ± 1.7 years, and 49.3% were females. Among the cases identified, 205 patients died during hospitalization with an overall in-hospital mortality of 0.7%. Atrial fibrillation was independently associated with higher in-hospital mortality (odds ratio [OR] 3.01; CI 1.38 to 6.57; p = 0.005) as was congestive heart failure (OR 3.15; CI 1.08 to 10.14; p = 0.049).
Conclusion
Atrial fibrillation and congestive heart failure were associated with higher inpatient mortality in patients with neutropenic fever. Identifying the risk factors for increased mortality in patients with neutropenic fever is important for risk stratification and guiding clinicians in taking therapeutic decisions in this set of patients.

Similar content being viewed by others
References
Freifeld AG, Bow EJ, Sepkowitz KA, Boeckh MJ, Ito JI, Mullen CA, Raad II, Rolston KV, Young JA, Wingard JR, Infectious Diseases Society of America (2011) Clinical practice guideline for the use of antimicrobial agents in neutropenic patients with cancer: 2010 update by the Infectious Diseases Society of America. Clin Infect Dis 52(4):e56–e93
Dulisse B, Li X, Gayle JA, Barron RL, Ernst FR, Rothman KJ, Legg JC, Kaye JA (2013) A retrospective study of the clinical and economic burden during hospitalizations among cancer patients with febrile neutropenia. J Med Econ 16(6):720–735
Crawford J, Dale DC, Lyman GH (2004) Chemotherapy-induced neutropenia: risks, consequences, and new directions for its management. Cancer. 100(2):228–237
Boada Burutaran M, Guadagna R, Grille S, Stevenazzi M, Guillermo C, Diaz L (2015) Results of high-risk neutropenia therapy of hematology-oncology patients in a university hospital in Uruguay. Rev Bras Hematol Hemoter 37(1):28–33
Klastersky J (2004) Management of fever in neutropenic patients with different risks of complications. Clin Infect Dis 39(Suppl 1):S32–S37
Perron T, Emara M, Ahmed S (2014) Time to antibiotics and outcomes in cancer patients with febrile neutropenia. BMC Health Serv Res 14:162
Weycker D, Barron R, Kartashov A, Legg J, Lyman GH (2014) Incidence, treatment, and consequences of chemotherapy-induced febrile neutropenia in the inpatient and outpatient settings. J Oncol Pharm Pract 20(3):190–198
Baden LR, Swaminathan S, Angarone M, Blouin G, Camins BC, Casper C, Cooper B, Dubberke ER, Engemann AM, Freifeld AG, Greene JN, Ito JI, Kaul DR, Lustberg ME, Montoya JG, Rolston K, Satyanarayana G, Segal B, Seo SK, Shoham S, Taplitz R, Topal J, Wilson JW, Hoffmann KG, Smith C (2016) Prevention and treatment of cancer-related infections, version 2.2016, NCCN clinical practice guidelines in oncology. J Natl Compr Cancer Netw 14(7):882–913
Taplitz RA, Kennedy EB, Bow EJ, Crews J, Gleason C, Hawley DK, Langston AA, Nastoupil LJ, Rajotte M, Rolston K, Strasfeld L, Flowers CR (2018) Outpatient management of fever and neutropenia in adults treated for malignancy: American Society of Clinical Oncology and Infectious Diseases Society of America clinical practice guideline update. J Clin Oncol 36(14):1443–1453
Kuderer NM, Dale DC, Crawford J, Cosler LE, Lyman GH (2006) Mortality, morbidity, and cost associated with febrile neutropenia in adult cancer patients. Cancer. 106(10):2258–2266
Culakova E, Poniewierski MS, Crawford J, Dale DC, Lyman GH (2014) Impact of comorbidities on length of stay and mortality in hospitalized patients with cancer and febrile neutropenia. Blood 124(21):2601. https://doi.org/10.1182/blood.V124.21.2601.2601
Houchens RLRD, Elixhauser A, Jiang J (2014) Nationwide inpatient sample redesign final report. U.S. Agency for Healthcare Research and Quality
Kozma CM, Dickson M, Chia V, Legg J, Barron R (2012) Trends in neutropenia-related inpatient events. J Oncol Pract 8(3):149–155. https://doi.org/10.1200/JOP.2011.000360
Tai E, Guy GP, Dunbar A, Richardson LC (2017) Cost of cancer-related neutropenia or fever hospitalizations, United States, 2012. J Oncol Pract 13(6):e552–ee61
Thursky KA, Worth LJ (2015) Can mortality of cancer patients with fever and neutropenia be improved? Curr Opin Infect Dis 28(6):505–513
Shaw AT, Kim DW, Nakagawa K, Seto T, Crino L, Ahn MJ et al (2013) Crizotinib versus chemotherapy in advanced ALK-positive lung cancer. N Engl J Med 368(25):2385–2394
Ahn S, Lee YS (2012) Predictive factors for poor prognosis febrile neutropenia. Curr Opin Oncol 24(4):376–380
Uys A, Rapoport BL, Fickl H, Meyer PW, Anderson R (2007) Prediction of outcome in cancer patients with febrile neutropenia: comparison of the multinational association of supportive care in cancer risk-index score with procalcitonin, C-reactive protein, serum amyloid A, and interleukins-1beta, −6, −8 and −10. Eur J Cancer Care (Engl) 16(6):475–483
Li Y, Family L, Yang SJ, Klippel Z, Page JH, Chao C (2017) Risk of febrile neutropenia associated with select myelosuppressive chemotherapy regimens in a large community-based oncology practice. J Natl Compr Cancer Netw 15(9):1122–1130
Asnani A, Manning A, Mansour M, Ruskin J, Hochberg EP, Ptaszek LM (2017) Management of atrial fibrillation in patients taking targeted cancer therapies. Cardio-Oncology. 3(1):2
Gazewood JD, Turner PL (2017) Heart failure with preserved ejection fraction: diagnosis and management. Am Fam Physician 96(9):582–588
Klastersky J, Paesmans M, Rubenstein EB, Boyer M, Elting L, Feld R, Gallagher J, Herrstedt J, Rapoport B, Rolston K, Talcott J, for the Study Section on Infections of Multinational Association for Supportive Care in Cancer (2000) The multinational association for supportive care in cancer risk index: a multinational scoring system for identifying low-risk febrile neutropenic cancer patients. J Clin Oncol 18(16):3038–3051
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflict of interest to disclose. Authors have full control of all primary data and data can be provided if requested.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Atallah-Yunes, S.A., Kadado, A.J., Haddadin, F. et al. Impact of cardiovascular comorbidities on inpatient mortality in patients hospitalized with neutropenic fever. Support Care Cancer 29, 509–513 (2021). https://doi.org/10.1007/s00520-020-05518-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-020-05518-6