Abstract
Purpose
Oral health is essential to general health and well-being and is severely impacted by head and neck cancer (HNC) and its treatment. This study aimed to describe how people who have been treated for HNC cope with altered oral health and function and to identify their supportive care needs.
Methods
A qualitative, descriptive approach was used. Data was collected from individual interviews with six participants 6 months after treatment. Data analysis was performed by qualitative content analysis involving inductive and directed approaches. Directed content analysis was guided by the Stress, Appraisal and Coping Model.
Results
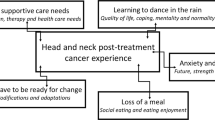
Three themes describing changed oral health were identified from the data: dimensions of eating, maintaining oral health after treatment and adapting to the chronic side effects of treatment. A strong use of problem-focussed coping was described, in addition to the importance of peer support in adapting to the psychosocial outcomes of treatment. Support needs identified related to increased access to specialist dental oncology services post treatment, information needs and a need for more psychological support.
Conclusion
The study findings describe the experience of a sample of people who have received treatment for HNC. Due to a demographically homogenous sample and the strong use of positive coping strategies, the results presented may not describe the experience of the wider HNC population; however, these results provide insight into factors that may influence positive coping.


Similar content being viewed by others
References
Meurman JH, Gronroos L (2010) Oral and dental health care of oral cancer patients: hyposalivation, caries and infections. Oral Oncol 46(6):464–467
Fang FM, Chien CY, Kuo SC, Chiu HC, Wang CJ (2004) Changes in quality of life of head-and-neck cancer patients following postoperative radiotherapy. Acta Oncol 43(6):571–578
Penner JL, McClement SE, Sawatzky JA (2007) Management of dysphagia in advanced oropharyngeal cancer. Int J Palliat Nurs 13(5):206–212
So WKW, Chan RJ, Chan DNS, Hughes BGM, Chair SY, Choi KC, Chan CWH (2012) Quality-of-life among head and neck cancer survivors at 1 year after treatment—a systematic review. Eur J Cancer 48(15):2391–2408
World Health Organisation (2014) Oral Health. http://www.who.int/topics/oral_health/en/. Accessed 30 Jan 2014
Epstein JB, Huhmann MB (2012) Dietary and nutritional needs of patients after therapy for head and neck cancer. J Am Dent Assoc 143(6):588–592
Barrios R, Tsakos G, Garcia-Medina B, Martinez-Lara I, Bravo M (2014) Oral health-related quality of life and malnutrition in patients treated for oral cancer. Support Care Cancer
Ma L, Poulin P, Feldstain A, Chasen MR (2013) The association between malnutrition and psychological distress in patients with advanced head-and-neck cancer. Curr Oncol 20(6):e554–e560
Penner JL (2009) Psychosocial care of patients with head and neck cancer. Semin Oncol Nurs 25(3):231–241
Chen SC, Tsai MC, Liu CL, Yu WP, Liao CT, Chang JT (2009) Support needs of patients with oral cancer and burden to their family caregivers. Cancer Nurs 32(6):473–481
Chen SC, Lai YH, Liao CT, Chang JT, Lin CY, Fan KH, Huang BS (2013) Supportive care needs in newly diagnosed oral cavity cancer patients receiving radiation therapy. Psychooncology 22(6):1220–1228
Dall’Armi L, Simpson GK, Forstner D, Simpson T, Roydhouse JK, White KJ (2013) The information needs of patients with head and neck cancer and their caregivers: a short report of instrument development and testing. Appl Nurs Res: ANR 26(1):40–44
Henry M, Habib LA, Morrison M, Yang JW, Li XJ, Lin S, Zeitouni A, Payne R, Macdonald C, Mlynarek A, Kost K, Black M, Hier M (2013) Head and neck cancer patients want us to support them psychologically in the posttreatment period: Survey results. Palliat Support Care:1–13
Patton MQ (2002) Qualitative research & evaluation methods, 3rd edn. Sage Publications, Thousand Oaks
Sandelowski M (2000) Whatever happened to qualitative description? Res Nurs Health 23(4):334–340
Elo S, Kyngas H (2008) The qualitative content analysis process. J Adv Nurs 62(1):107–115
Hsieh HF, Shannon SE (2005) Three approaches to qualitative content analysis. Qual Health Res 15(9):1277–1288
Lazarus R, Folkman S (1984) Stress, appraisal and coping. Springer Publishing Inc, New York
Bigatti SM, Steiner JL, Miller KD (2012) Cognitive appraisals, coping and depressive symptoms in breast cancer patients. Stress Health 28(5):355–361
Moore K, Ford P, Farah C (2014) Support needs and quality of life in oral cancer: a systematic review. Int J Dent Hyg 12(1):36–47
Hansen E (2006) Successful qualitative health research: a practical introduciton. Allen & Unwin, Crows Nest
Vissink A, Burlage FR, Spijkervet FK, Jansma J, Coppes RP (2003) Prevention and treatment of the consequences of head and neck radiotherapy. Crit Rev Oral Biol Med 14(3):213–225
Scully C, Epstein JB (1996) Oral health care for the cancer patient. Eur J Cancer B Oral Oncol 32B(5):281–292
Beech N, Robinson S, Porceddu S, Batstone M (2014) Dental management of patients irradiated for head and neck cancer. Aust Dent J 59(1):20–28
Dental Board of Australia (2014) Guidelines for scope of practice. Australian Health Practioner Regulation Agency. http://www.dentalboard.gov.au/Codes-Guidelines/Policies-Codes-Guidelines/Guidelines-Scope-of-practice.aspx. Accessed 17.10.14 2014
Roing M, Hirsch JM, Holmstrom I (2007) The uncanny mouth—a phenomenological approach to oral cancer. Patient Educ Couns 67(3):301–306
Rose-Ped AM, Bellm LA, Epstein JB, Trotti A, Gwede C, Fuchs HJ (2002) Complications of radiation therapy for head and neck cancers. The patient’s perspective. Cancer Nurs 25(6):461–467, quiz 468–469
Nund RL, Ward EC, Scarinci NA, Cartmill B, Kuipers P, Porceddu SV (2014) The lived experience of dysphagia following non-surgical treatment for head and neck cancer. Int J Speech Lang Pathol 16(3):282–289
Moore KA, Ford PJ, Farah CS (2014) “I have quality of life…but…”: exploring support needs important to quality of life in head and neck cancer. Eur J Oncol Nurs 18(2):192–200
Maher NG, Britton B, Hoffman GR (2013) Early screening in patients with head and neck cancer identified high levels of pain and distress. J Oral Maxillofac Surg 71(8):1458–1464
Neilson K, Pollard A, Boonzaier A, Corry J, Castle D, Smith D, Trauer T, Couper J (2013) A longitudinal study of distress (depression and anxiety) up to 18 months after radiotherapy for head and neck cancer. Psychooncology 22(8):1843–1848
Llewellyn CD, Horney DJ, McGurk M, Weinman J, Herold J, Altman K, Smith HE (2013) Assessing the psychological predictors of benefit finding in patients with head and neck cancer. Psychooncology 22(1):97–105
Harrington S, McGurk M, Llewellyn CD (2008) Positive consequences of head and neck cancer: key correlates of finding benefit. J Psychosoc Oncol 26(3):43–62
Lang H, France E, Williams B, Humphris G, Wells M (2013) The psychological experience of living with head and neck cancer: a systematic review and meta-synthesis. Psycho-Oncology 22(12):2648–2663
Fang CY, Longacre ML, Manne SL, Ridge JA, Lango MN, Burtness BA (2012) Informational needs of head and neck cancer patients. Health Technol (Berl) 2(1):57–62
So WK, Choi KC, Chen JM, Chan CW, Chair SY, Fung OW, Wan RW, Mak SS, Ling WM, Ng WT, Yu BW (2014) Quality of life in head and neck cancer survivors at 1 year after treatment: the mediating role of unmet supportive care needs. Support Care Cancer. doi:10.1007/s00520-014-2278-0
Chen SC, Yu WP, Chu TL, Hung HC, Tsai MC, Liao CT (2010) Prevalence and correlates of supportive care needs in oral cancer patients with and without anxiety during the diagnostic period. Cancer Nurs 33(4):280–289
Egestad H (2013) The significance of fellow patients for head and neck cancer patients in the radiation treatment period. Eur J Oncol Nurs 17(5):618–624
Solomon P (2004) Peer support/peer provided services underlying processes, benefits, and critical ingredients. Psychiatr Rehabil J 27(4):392–401
Blixen C, Perzynski A, Kanuch S, Dawson N, Kaiser D, Lawless ME, Seeholzer E, Sajatovic M (2014) Training peer educators to promote self-management skills in people with serious mental illness (SMI) and diabetes (DM) in a primary health care setting. Primary health care research & development: 1–11
Ford P, Clifford A, Gussy K, Gartner C (2013) A systematic review of peer-support programs for smoking cessation in disadvantaged groups. Int J Environ Res Publ Health 10(11):5507–5522
Duffy SA, Terrell JE, Valenstein M, Ronis DL, Copeland LA, Connors M (2002) Effect of smoking, alcohol, and depression on the quality of life of head and neck cancer patients. Gen Hosp Psychiatry 24(3):140–147
Kanatas A, Ghazali N, Lowe D, Rogers SN (2012) The identification of mood and anxiety concerns using the patients concerns inventory following head and neck cancer. Int J Oral Maxillofac Surg 41(4):429–436
Chen AM, Daly ME, Vazquez E, Courquin J, Luu Q, Donald PJ, Farwell DG (2013) Depression among long-term survivors of head and neck cancer treated with radiation therapy. JAMA otolaryngol–Head Neck Surg 139(9):885–889
Acknowledgments
This study was funded by the Dental Hygiene Association of Australia’s Research Fund.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 36 kb)
Rights and permissions
About this article
Cite this article
Pateman, K.A., Ford, P.J., Batstone, M.D. et al. Coping with an altered mouth and perceived supportive care needs following head and neck cancer treatment. Support Care Cancer 23, 2365–2373 (2015). https://doi.org/10.1007/s00520-015-2607-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-015-2607-y