Abstract
Background
Hemolytic uremic syndrome (HUS) is a clinical syndrome characterized by hemolytic anemia, thrombocytopenia, and acute kidney injury. Atypical hemolytic uremic syndrome (aHUS) is a devastating disease with significant mortality and high risk of progression to end-stage kidney disease. It is mostly caused by dysregulation of the alternative complement pathway. Cobalamin C (Cbl C) defect is a genetic disorder of cobalamin metabolism and is a rare cause of HUS.
Case-diagnosis/treatment
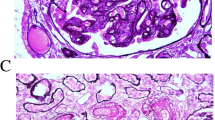
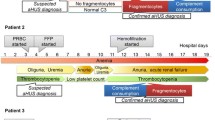
We present a 6-month-old male infant who was admitted to the pediatric intensive care unit (PICU) due to restlessness, severe hypertension, anemia, respiratory distress, and acute kidney injury. Metabolic screening revealed elevated plasma homocysteine levels, low methionine levels, and methylmalonic aciduria, and the patient was diagnosed as having HUS secondary to Cbl C defect. Additionally, complement factor H (CFH) and complement C3 levels were decreased. The infant was treated with betaine, hydroxycobalamin, and folic acid. After treatment, the homocysteine and methylmalonic acid levels were normalized but hemolysis and acute kidney failure persisted. He required continued renal replacement treatment (CRRT) and plasma exchange due to thrombotic microangiopathy (TMA). Therefore, we considered a second mechanism in the pathogenesis as complement dysregulation and gave eculizumab to the patient. After eculizumab treatment, the renal and hematologic indices improved and he was free of dialysis.
Conclusions
To the best of our knowledge, our patient is the first to have Cbl C defect-HUS accompanied by complement dysregulation, who responded well to eculizumab therapy.

Similar content being viewed by others
References
Loirat C, Fakhouri F, Ariceta G, Besbas N, Bitzan M, Bjerre A, Coppo R, Emma F, Johnson S, Karpman D, Landau D, Langman CB, Lapeyraque AL, Licht C, Nester C, Pecoraro C, Riedl M, van de Kar NC, Van de Walle J, Vivarelli M, Fremeaux-Bacchi V, HUS International (2016) An international consensus approach to the management of atypical hemolytic uremic syndrome in children. Pediatr Nephrol 31:15–39
Martinelli D, Deodato F, Dionisi-Vici C (2011) Cobalamin C defect: natural history, pathophysiology and treatment. J Inherit Metab Dis 34:127–135
Carrilo-Carrasco N, Chandler RJ, Venditti CP (2012) Combined methylmalonic acidemia and homocystinuria, cblC type. I. Clinical presentations, diagnosis and management. J Inherit Metab Dis 35:91–102
Adrovic A, Canpolat N, Caliskan S, Sever L, Kıykım E, Agbas A, Baumgartner MR (2016) Cobalamin C defect-hemolytic uremic syndrome caused by new mutation in MMACHC. Pediatr Int 58:763–765
Beck BB, van Spronsen F, Diepstra A, Berger RM, Kömhoff M (2017) Renal thrombotic microangiopathy in patients with cblC defect: review of an under-recognized entity. Pediatr Nephrol 32:733–741
Guigonis V, Frémeaux-Bacchi V, Giraudier S, Favier R, Borderie D, Massy Z, Mougenot B, Rosenblatt DS, Deschênes G (2005) Late-onset thrombocytic microangiopathy caused by cblC disease: association with a factor H mutation. Am J Kidney Dis 45:588–595
Caillaud C, Zaloszyc A, Licht C, Pichault V, Fremeaux-Bacchi V, Fischbach M (2016) CFH gene mutation in a case of Shiga toxin-associated hemolytic uremic syndrome (STEC-HUS). Pediatr Nephrol 31:157–161
European Medicines Agency. Soliris (eculizumab): EU summary of product characteristics. Mar 14 http://www.emea.europa.eu/docs/en_GB/document_library/EPAR_Product_Information/human/ 000791/WC500054208.pdf
Alexion Pharmaceuticals Inc.Soliris-(eculizumab):US prescribing information.4/2014. http://www.accessdata.fda.gov/drugsatfda/docs/label/2014/125166s368s380lbl.pdf
Greenbaum LA, Fila M, Ardissino G, Al-Akash SI, Evans J, Henning P, Lieberman KV, Maringhini S, Pape L, Rees L, Van de Kar NCAJ, Vande Walle J, Ogawa M, Bedrosian CL, Licht C (2016) Eculizumab is a safe and effective treatment in pediatric patients with atypical hemolytic uremic syndrome. Kidney Int 89:701–711
Mache CJ, Acham-Roschitz B, Fremeaux-Bacchi V, Kirschfink M, Zipfel PF, Roedl S, Vester U, Ring E (2009) Complement inhibitor eculizumab in atypical hemolytic uremic syndrome. Clin J Am Soc Nephrol 4:1312–1316
Fremeaux-Bacchi V, Fakhouri F, Garnier A, Bienaime F, Dragon-Durey MA, Ngo S, Moulin B, Servais A, Provot F, Rostaing L, Burtey S, Niaudet P, Deschenes G, Lebranchu Y, Zuber J, Loirat C (2013) Genetics and outcome of atypical hemolytic uremic syndrome: a nationwide French series comparing children and adults. Clin J Am Soc Nephrol 8:554–562
Guo L, Lu MP, Dong GJ, Teng LP, Xu YP, Zou LX, Zheng Q (2017) Clinical and laboratory features of macrophage activation syndrome. Zhongguo Dang Dai Er Ke Za Zhi 19:188–192
Hofer J, Rosales A, Fischer C, Giner T (2014) Extra-renal manifestations of complement-mediated thrombotic microangiopathies. Front Pediatr 2:97
Bechtel K, Iragorri S (2010) Hepatosplenomegaly and reticulocytopenia as prominent features of atypical hemolytic uremic syndrome. Pediatr Emerg Care 26:510–511
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 14 kb)
Rights and permissions
About this article
Cite this article
Barlas, U.K., Kıhtır, H.S., Goknar, N. et al. Hemolytic uremic syndrome with dual caution in an infant: cobalamin C defect and complement dysregulation successfully treated with eculizumab. Pediatr Nephrol 33, 1093–1096 (2018). https://doi.org/10.1007/s00467-018-3941-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-018-3941-3