Abstract
Background
Previous studies on renal oligohydramnios (ROH) report highly variable outcome and identify early onset of ROH and presence of extrarenal manifestations as predictors of adverse outcome in most cases. Data on termination of pregnancy (TOP) and associated parental decision-making processes are mostly missing, but context-sensitive for the interpretation of these findings. We provide here a comprehensive analysis on the diagnosis, prenatal decision-making and postnatal clinical course in all pregnancies with ROH at our medical centre over an 8-year period.
Methods
We report retrospective chart review data on 103 consecutive pregnancies from 2008 to 2015 with a median follow-up of 554 days.
Results
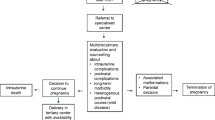
After ROH diagnosis, 38 families opted for TOP. This decision was associated with onset of ROH (p < 0.001), underlying renal disease (p = 0.001) and presence of extrarenal manifestations (p = 0.02). Eight infants died in utero and 8 cases were lost to follow-up. Of the 49 liveborn children, 11 received palliative and 38 underwent active care. Overall survival of the latter group was 84.2% (n = 32) corresponding to 31% of all pregnancies (32 out of 103) analysed. One third of the surviving infants needed renal replacement therapy during the first 6 weeks of life.
Conclusions
Over one third of pregnancies with ROH were terminated and the parental decision was based on risk factors associated with adverse outcome. Neonatal death was rare in the actively treated infants and the overall outcome promising. Our study illustrates that only careful analysis of the whole process, from prenatal diagnosis via parental decision-making to postnatal outcome, allows sensible interpretation of outcome data.


Similar content being viewed by others
References
Klaassen I, Neuhaus TJ, Mueller-Wiefel DE, Kemper MJ (2007) Antenatal oligohydramnios of renal origin: long-term outcome. Nephrol Dial Transplant 22:432–439
Mehler K, Beck BB, Kaul I, Rahimi G, Hoppe B, Kribs A (2011) Respiratory and general outcome in neonates with renal oligohydramnios—a single-centre experience. Nephrol Dial Transplant 26:3514–3522
Spiro JE, Konrad M, Rieger-Fackeldey E, Masjosthusmann K, Amler S, Klockenbusch W, Schmitz R (2015) Renal oligo- and anhydramnios: cause, course and outcome—a single-center study. Arch Gynecol Obstet 292:327–336
Grijseels EWM, van-Hornstra PTME, LCP G, Cohen-Overbeek TE, de Krijger RR, Smit BJ, Cransberg K (2011) Outcome of pregnancies complicated by oligohydramnios or anhydramnios of renal origin. Prenat Diagn 31:1039–1045
Hogan J, Dourthe ME, Blondiaux E, Jouannic JM, Garel C, Ulinski T (2012) Renal outcome in children with antenatal diagnosis of severe CAKUT. Pediatr Nephrol 27:497–502
Morris RK, Quinlan-Jones E, Kilby MD, Khan KS (2007) Systematic review of accuracy of fetal urine analysis to predict poor postnatal renal function in cases of congenital urinary tract obstruction. Prenat Diagn 27:900–911
Aulbert W, Kemper MJ (2016) Severe antenatally diagnosed renal disorders: background, prognosis and practical approach. Pediatr Nephrol 31:563–574
Magann EF, Ounpraseuth S, Chauhan SP, Ranganathan AS, Dajani NK, Bergstrom J, Morrison JC (2015) Correlation of ultrasound estimated with dye-determined or directly measured amniotic fluid volume revisited. Gynecol Obstet Investig 79:46–49
Hackl A, Mehler K, Gottschalk I, Vierzig A, Eydam M, Hauke J, Beck BB, Liebau MC, Ensenauer R, Weber LT, Habbig S (2017) Disorders of fatty acid oxidation and autosomal recessive polycystic kidney disease-different clinical entities and comparable perinatal renal abnormalities. Pediatr Nephrol 32:791–800
Morris RK, Middleton LJ, Malin GL, Quinlan-Jones E, Daniels J, Khan KS, Deeks J, Kilby MD, PLUTO Collaborative Group (2015) Outcome in fetal lower urinary tract obstruction: a prospective registry study. Ultrasound Obstet Gynecol 46:424–431
Morris RK, Malin GL, Quinlan-Jones E, Middleton LJ, Hemming K, Burke D, Daniels JP, Khan KS, Deeks J, Kilby MD (2013) Percutaneous vesicoamniotic shunting versus conservative management for fetal lower urinary tract obstruction (PLUTO): a randomised trial. Lancet 382:1496–1506
Spaggiari E, Stirnemann JJ, Heidet L, Dreux S, Ville Y, Oury JF, Delezoide AL, Muller F (2013) Outcome following prenatal diagnosis of severe bilateral renal hypoplasia. Prenat Diagn 33:1167–1172
Kumar M, Thakur S, Puri A, Shukla S, Sharma S, Perumal V, Chawla R, Gupta U (2014) Fetal renal anomaly: factors that predict survival. J Pediatr Urol 10:1001–1007
Kemper MJ, Neuhaus TJ, Timmermann K, Hueneke B, Laube G, Harps E, Mueller-Wiefel DE (2001) Antenatal oligohydramnios of renal origin: postnatal therapeutic and prognostic challenges. Clin Nephrol 56:S9–12
Ulkumen BA, Pala HG, Baytur YB, Koyuncu FM (2015) Outcomes and management strategies in pregnancies with early onset oligohydramnios. Clin Exp Obstet Gynecol 42:355–357
Rees L (2007) Long-term peritoneal dialysis in infants. Perit Dial Int 27(Suppl 2):S180–S184
Feinstein S, Rinat C, Becker-Cohen R, Ben-Shalom E, Schwartz SB, Frishberg Y (2008) The outcome of chronic dialysis in infants and toddlers—advantages and drawbacks of haemodialysis. Nephrol Dial Transplant 23:1336–1345
Wood EG, Hand M, Briscoe DM, Donaldson LA, Yiu V, Harley FL, Warady BA, Ellis EN (2001) Risk factors for mortality in infants and young children on dialysis. Am J Kidney Dis 37:573–579
Van Stralen KJ, Borzych-Dużalka D, Hataya H, Kennedy SE, Jager KJ, Verrina E, Inward C, Rönnholm K, Vondrak K, Warady BA, Zurowska AM, Schaefer F, Cochat P, ESPN/ERA-EDTA registry; IPPN registry; ANZDATA registry; Japanese RRT registry (2014) Survival and clinical outcomes of children starting renal replacement therapy in the neonatal period. Kidney Int 86:168–174
Carey WA, Talley LI, Sehring SA, Jaskula JM, Mathias RS (2007) Outcomes of dialysis initiated during the neonatal period for treatment of end-stage renal disease: a north American pediatric renal trials and collaborative studies special analysis. Pediatrics 119:e468–e473
Carey WA, Martz KL, Warady BA (2015) Outcome of patients initiating chronic peritoneal dialysis during the first year of life. Pediatrics 136:e615–e622
Wedekin M, Ehrich JHH, Offner G, Pape L (2010) Renal replacement therapy in infants with chronic renal failure in the first year of life. Clin J Am Soc Nephrol 5:18–23
Rheault MN, Rajpal J, Chavers B, Nevins TE (2009) Outcomes of infants <28 days old treated with peritoneal dialysis for end-stage renal disease. Pediatr Nephrol 24:2035–2039
Lantos JD, Warady BA (2013) The evolving ethics of infant dialysis. Pediatr Nephrol 28:1943–1947
Alamo L, Laswad T, Schnyder P, Meuli R, Vial Y, Osterheld MC, Gudinchet F (2010) Fetal MRI as complement to US in the diagnosis and characterization of anomalies of the genito-urinary tract. Eur J Radiol 76:258–264
Gupta P, Kumar S, Sharma R, Gadodia A, Roy KK, Sharma JB (2010) The role of magnetic resonance imaging in fetal renal anomalies. Int J Gynaecol Obstet 111:209–212
Rees L (2014) The dilemmas surrounding the decision to start chronic dialysis in the neonate. Kidney Int 86:18–20
Rees L (2016) Renal replacement therapies in neonates: issues and ethics. Semin Fetal Neonatal Med 22:104–108
Dionne JM, d’Agincourt-Canning L (2015) Sustaining life or prolonging dying? Appropriate choice of conservative care for children in end-stage renal disease: an ethical framework. Pediatr Nephrol 30:1761–1769
Teh JC, Frieling ML, Sienna JL, Geary DF (2011) Attitudes of caregivers to management of end-stage renal disease in infants. Perit Dial Int 31:459–465
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors declare that they have no conflicts of interest related to the study.
Rights and permissions
About this article
Cite this article
Mehler, K., Gottschalk, I., Burgmaier, K. et al. Prenatal parental decision-making and postnatal outcome in renal oligohydramnios. Pediatr Nephrol 33, 651–659 (2018). https://doi.org/10.1007/s00467-017-3812-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-017-3812-3