Abstract
Background
Per oral endoscopic myotomy (POEM) has recently emerged as a viable option relative to the classic approach of laparoscopic Heller myotomy (LHM) for the treatment of esophageal achalasia. In this cost-utility analysis of POEM and LHM, we hypothesized that POEM would be cost-effective relative to LHM.
Methods
A stochastic cost-utility analysis of treatment for achalasia was performed to determine the cost-effectiveness of POEM relative to LHM. Costs were estimated from the provider perspective and obtained from our institution’s cost-accounting database. The measure of effectiveness was quality-adjusted life years (QALYs) which were estimated from direct elicitation of utility using a visual analog scale. The primary outcome was the incremental cost-effectiveness ratio (ICER). Uncertainty was assessed by bootstrapping the sample and computing the cost-effectiveness acceptability curve (CEAC).
Results
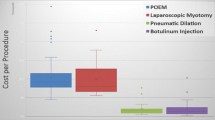
Patients treated within an 11-year period (2004–2016) were recruited for participation (20 POEM, 21 LHM). During the index admission, the mean costs for POEM ($8630 ± $2653) and the mean costs for LHM ($7604 ± $2091) were not significantly different (P = 0.179). Additionally, mean QALYs for POEM (0.413 ± 0.248) were higher than that associated with LHM (0.357 ± 0.338), but this difference was also not statistically significant (P = 0.55). The ICER suggested that it would cost an additional $18,536 for each QALY gained using POEM. There was substantial uncertainty in the ICER; there was a 48.25% probability that POEM was cost-effective at the mean ICER. At a willingness-to-pay threshold of $100,000, there was a 68.31% probability that POEM was cost-effective relative to LHM.
Conclusions
In the treatment of achalasia, POEM appears to be cost-effective relative to LHM depending on one’s willingness-to-pay for an additional QALY.


Similar content being viewed by others
References
Campos GM, Vittinghoff E, Rabl C, Takata M, Gadenstätter M, Ciovica Lin F (2009) Endoscopic and surgical treatments for achalasia: a systematic review and meta-analysis. Ann Surg 249:45–57
Fisichella PM, DeMeester SR, Hungness E, Perretta S, Soper NJ, Rosemurgy A, Torquati A, Sachdeva AK, Patti MG (2015) Emerging techniques in minimally invasive surgery. Pros and Cons. J Gastrointest Surg 19:1355–1362
Kumbhari V, Tieu AH, Onimaru M, El Zein MH, Teitelbaum EN, Ujiki MB, Gitelis ME, Modayil RJ, Hungness ES, Stavropoulos SN, Shiwaku H, Kunda R, Chiu P, Saxena P, Messallam AA, Inoue H, Khashab MA (2015) Peroral endoscopic myotomy (POEM) vs laparoscopic Heller myotomy (LHM) for the treatment of Type III achalasia in 75 patients: a multicenter comparative study. Endosc Int Open 3:E195–E201
Hungness ES, Teitelbaum EN, Santos BF, Arafat FO, Pandolfino JE, Kahrilas PJ, Soper NJ (2013) Comparison of perioperative outcomes between peroral esophageal myotomy (POEM) and laparoscopic Heller myotomy. J Gastrointest Surg 17:228–235
Teitelbaum EN, Rajeswaran S, Zhang R, Sieberg RT, Miller FH, Soper NJ, Hungness ES (2013) Peroral esophageal myotomy (POEM) and laparoscopic Heller myotomy produce a similar short-term anatomic and functional effect. Surgery 154:885–891
Bhayani NH, Kurian AA, Dunst CM, Sharata AM, Rieder E, Swanstrom LL (2014) A comparative study on comprehensive, objective outcomes of laparoscopic Heller myotomy with per-oral endoscopic myotomy (POEM) for achalasia. Ann Surg 259:1098–1103
Stefanidis D, Fanelli RD, Price R, Richardson W (2014) SAGES guidelines for the introduction of new technology and techniques. Surg Endosc 28:2257–2271
Traverso LW (1996) Technology and surgery. Dilemma of the gimmick, true advances, and cost effectiveness. Surg Clin North Am 76:129–138
Olson SA, Obremskey WT, Bozic KJ (2013) Healthcare technology: physician collaboration in reducing the surgical cost. Clin Orthop Related Res 471:1854–1864
Docimo S Jr, Shope AJ, Winder JS, Haluck RS, Pauli EM (2016) Reduced postoperative pain scores and narcotic use favor per-oral endoscopic myotomy over laparoscopic Heller myotomy. Surg Endosc 31:795–800
Orenstein SBRS, Pauli EM, Phillips MS, Ponsky JL, Marks JM (2015) Peroral endoscopic myotomy (POEM) leads to similar results in patients with and without prior endoscopic or surgical therapy. Surg Endosc 29:1060–1070
Woo RK, Skarsgard ED (2015) Innovating for quality and value: utilizing national quality improvement programs to identify opportunities for responsible surgical innovation. Semin Pediatr Surg 24:138–140
Deyo RA, Cherkin DC, Ciol MA (1992) Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol 45:613–619
Chuah SK, Chiu CH, Tai WC, Lee JH, Lu HI (2013) Current status in the treatment options for esophageal achalasia. World J Gastroenterol 19:5421–5429
Talukdar R, Inoue H, Nageshwar Reddy D (2015) Efficacy of peroral endoscopic myotomy (POEM) in the treatment of achalasia: a systematic review and meta-analysis. Surg Endosc 29:3030–3046
Hungness ESSJ, Teitelbaum EN, Kahrilas PJ, Pandolfino JE, Soper NJ (2016) Per-oral endoscopic myotomy (POEM) after the learning curve: durable long-term results with a low complication rate. Ann Surg 264:508–517
Inoue HSH, Ikeda H, Onimaru M, Sato C, Minami H, Yokomichi H, Kobayashi Y, Grimes KL, Kudo SE (2015) Per-oral endoscopic myotomy: a series of 500 patients. J Am Coll Surg 221:256–264
Zaninotto G, Costantini M, Portale G, Battaglia G, Molena D, Carta A, Costantino M, Nicoletti L, Ancona E (2002) Etiology, diagnosis, and treatment of failures after laparoscopic Heller myotomy for achalasia. Ann Surg 235:186–192
Werner YB, Costamagna G, Swanström LL, von Renteln D, Familiari P, Sharata AM, Noder T, Schachschal G, Kersten JF, Rösch T (2016) Clinical response to peroral endoscopic myotomy in patients with idiopathic achalasia at a minimum follow-up of 2 years. Gut 65:899–906
Lukacz ES, Lawrence JM, Burchette RJ, Luber KM, Nager CW, Buckwalter JG (2004) The use of visual analog scale in urogynecologic research: a psychometric evaluation. Am J Obstet Gynecol 191:165–170
Noel CW, Lee DJ, Kong Q, Xu W, Simpson C, Brown D, Gilbert RW, Gullane PJ, Irish JC, Huang SH, O’Sullivan B, Goldstein DP, de Almeida JR (2015) Comparison of health state utility measures in patients with head and neck cancer. JAMA Otolaryngol Head Neck Surg 141:696–703
Stark PA, Myles PS, Burke JA (2013) Development and psychometric evaluation of a postoperative quality of recovery score: the QoR-15. Anesthesiology 118:1332–1340
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Drs. Greenleaf, Winder, Hollenbeak, Haluck, Mathew and Pauli have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Greenleaf, E.K., Winder, J.S., Hollenbeak, C.S. et al. Cost-effectiveness of per oral endoscopic myotomy relative to laparoscopic Heller myotomy for the treatment of achalasia. Surg Endosc 32, 39–45 (2018). https://doi.org/10.1007/s00464-017-5629-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5629-3