Abstract
Background
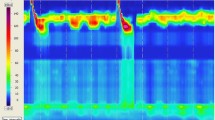
Three variants of Achalasia have been described using high-resolution esophageal manometry (HRM). While manometrically distinct, their clinical significance has yet to be established. Our objective was to compare the outcome after myotomy in patients with these Achalasia subtypes.
Methods
A retrospective chart review was performed to identify patients with Achalasia who had HRM and who underwent Heller myotomy or Per oral endoscopic myotomy (POEM). Symptoms and esophageal clearance by timed barium study were compared before and after treatment.
Results
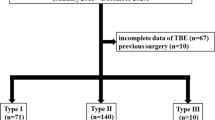
We identified 49 patients, 21 males and 28 females, with a median age of 52 years. The primary symptom in all patients was dysphagia, with a median duration of 4 years (range 4 months–50 years). By HRM, ten patients (20 %) were classified as Type I, 30 (61 %) as Type II, and 9 (18 %) as Type III. At a median follow-up of 16 months after myotomy (range 1–63 months), the median Eckardt score was zero and was similar across subtypes. Relief of dysphagia was also similar across subtypes (80 % of Type I, 93 % of Type II and 89 % of Type III).
On pre-treatment timed barium study, no patient had complete emptying at 1 or 5 min. After myotomy, complete emptying occurred within 1 min in 50 % (20/40) and within 5 min in 60 % (24/40) and was similar across groups.
Conclusion
Myotomy for Achalasia results in excellent symptomatic outcome and improvement in esophageal clearance. There was no difference among the described HRM Achalasia variants. This calls into question the clinical utility of Achalasia sub-classification and affirms the benefit of myotomy for this disease.

Similar content being viewed by others
References
Pandolfino JE, Kwiatek MA, Nealis T, Bulsiewicz W, Post J, Kahrilas PJ (2008) Achalasia: A new clinically relevant classification by high-resolution manometry. Gastroenterology 135:1526–1533
Eckardt A, Eckardt VF (2011) Treatment and surveillance strategies in Achalasia: an update. Nat. Rev. Gastroenterol Hepatol 8:311–319
Fuller L, Huprich JE, Theisen J, Hagen JA, Crookes PF, DeMeester SR, Bremner CG, DeMeester TR, Peters JH (1999) Abnormal esophageal body function: radiographic-manometric correlation. The American Surgeon 65:911–914
Ayazi S, Hagen JA, Zehetner J, Ross O, Wu C, Oezcelik A, Abate E, Sohn HJ, Bank F, Lipham JC, DeMeester SR, DeMeester TR (2009) The Value of high-resolution manometry in the assessment of the resting characteristics of the lower esophageal sphincter. J Gastrointest Surg 13:2113–2120
Carlson DA, Pandolfino JE (2013) High-resolution manometry and esophageal pressure topography filling the gaps of convention manometry. Gastroenterol Clin N Am 42:1–15
Arain MA, Peters JH, Tamhankar AP, Portale G, DeMeester SR, Crookes PF, Hagen JA, Bremner CG, DeMeester TR (2004) Preoperative lower esophageal sphincter pressure affects outcome of laparoscopic esophageal myotomy for Achalasia. J Gastrointest Surg 8:328–334
Conklin JL (2013) Evaluation of esophageal motor function with high-resolution manometry. J Neurogastroenterol Motil 19:281–294
Kahrilas PJ, Ghosh SK, Pandolfino JE (2008) Esophageal motility disorders in terms of pressure topography. J Clin Gastroenterol 42:627–635
Kahrilas PJ (2010) Esophageal motor disorders in terms of high-resolution esophageal pressure topography: what has changed? Am J Gastroenterol 105:981–987
Bredenoord AJ, Fox M, Kahrilas PJ, Pandolfino JE, Schwizer W, Smout AJPM, Conklin JL, Cook IJ, Gyawali P, Hebbard G, Holloway RH, Ke M, Keller J, Mittal R, Peters J, Richter J, Roman S, Rommel N, Sifrim D, Tutuian R, Valdovinos M, Vela MF, Zerbib F (2012) Chicago classification criteria of esophageal motility disorders defined in high resolution esophageal pressure topography (EPT). Neurogastroenterol Motil 24:57–65
Rohof W, Salvador R, Annese V, Des Varannes SB, Chaussade S, Constantini M, Elizalde JI, Gaudric M, Smouth AJ, Tack J, Busch O, Zaninotto G, Boeckxstaens GE (2013) Outcomes of treatment for Achalasia depend on manometric subtype. Gastroenterology 144:718–725
Roman S, Zerbib F, Quenehervé L, Clermidy H, Des Varannes SB, Mion F (2012) The Chicago classification for Achalasia in a french multicentric cohort. Digestive and Liver Disease 44:976–980
Pratap N, Kalapala R, Darisetty S, Joshi N, Ramchandani M, Banerjee R, Lakhtakia S, Gupta R, Tandan M, Rao G, Reddy DN (2011) Achalasia cardia subtyping by high-resolution manometry predicts the therapeutic outcome of pneumatic balloon dilatation. J Neurogastroenterol Motil 17:48–53
Salvador R, Constantini M, Zaninotto G, Morbin T, Rizzetto C, Zanatta L, Ceolin M, Finotti E, Nicoletti L, Dalt GD, Cavallin F, Ancona E (2010) The Preoperative manometric pattern predicts the outcome of surgical treatment for esophageal Achalasia. J Gastrointest Surg 14:1635–1645
Pandolfino JE (2013) Uncovering hidden information in Achalasia using esophageal pressure topography. Gastroenterology 144:681–690
Acknowledgments
None.
Disclosures
Drs. Greene, Chang, Oh, Worrell, and Hagen have nothing to disclose.
Dr. DeMeester is a consultant for Davol, Gore, Novadaq and C2 Therapeutics, none of which are relevant to this work.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Greene, C.L., Chang, E.J., Oh, D.S. et al. High resolution manometry sub-classification of Achalasia: does it really matter?. Surg Endosc 29, 1363–1367 (2015). https://doi.org/10.1007/s00464-014-3804-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3804-3