Abstract
Background
Barrett’s esophagus (BE) is a major risk factor for esophageal adenocarcinoma. It is believed that BE is caused by chronic gastro-esophageal reflux disease (GERD). Laparoscopic anti-reflux surgery (LARS) restores the competency of the cardia and may thereby change the natural course of BE. We studied the impact of LARS on the histological profile of BE and on the control of GERD.
Methods
We identified all patients with BE who underwent LARS from 1994 to 2007 and contacted them to assess post-operative GERD symptoms via questionnaire. Endoscopy findings, histology, 24 hour pH monitoring, and manometry were also collected using our prospectively maintained database. Histological regression was defined as either loss of dysplasia or disappearance of BE.
Results
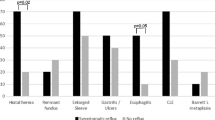
Two hundred and fifteen patients met the initial inclusion criteria; in 82 of them histology from post-operative endoscopy was available for review. Endoscopy was performed a median of 8 years (range, 1–16 years) after surgery. Regression of BE occurred in 18 (22 %) patients while in 6 (7 %) BE progressed to dysplasia or cancer. Thirty-six (43 %) patients underwent pre- and post-operative manometry. The median lower esophageal sphincter pressure increased from 9 to 17 mmHg in these patients. Thirty-four (41 %) patients underwent pre- and post-operative pH studies. The median DeMeester score decreased from 54 to 9. Sixty-seven (82 %) of 82 patients completed the post-operative questionnaire; 86 % of these patients reported improvement in heartburn and regurgitation.
Conclusions
LARS was associated with both physiologic and symptomatic control of GERD in patients with BE. LARS resulted in regression of BE in 22 % of patients and progression in 7 %. Thus, continued surveillance of Barrett’s is needed after LARS.

Similar content being viewed by others
References
Fitzgerald RC, di Pietro M, Ragunath K, Ang Y, Kang JY, Watson P, Trudgill N, Patel P, Kaye PV, Sanders S, O’Donovan M, Bird-Lieberman E, Bhandari P, Jankowski JA, Attwood S, Parsons SL, Loft D, Lagergren J, Moayyedi P, Lyratzopoulos G, de Caestecker J (2014) Guidelines for the diagnosis and management of Barrett’s columnar-lined oesophagus. Gut 63(1):7–42
Zehetner J, DeMeester SR, Ayazi S, Costales JL, Augustin F, Oezcelik A, Lipham JC, Sohn HJ, Hagen JA, DeMeester TR (2010) Long-term follow-up after anti-reflux surgery in patients with Barrett’s esophagus. J Gastrointest Surg 14(10):1483–1491
Sikkema M, Looman CW, Steyerberg EW, Kerkhof M, Kastelein F, van Dekken H, van Vuuren AJ, Bode WA, van der Valk H, Ouwendijk RJ, Giard R, Lesterhuis W, Heinhuis R, Klinkenberg EC, Meijer GA, ter Borg F, Arends JW, Kolkman JJ, van Baarlen J, de Vries RA, Mulder AH, van Tilburg AJ, Offerhaus GJ, ten Kate FJ, Kusters JG, Kuipers EJ, Siersema PD (2011) Predictors for neoplastic progression in patients with Barrett’s esophagus: a prospective cohort study. Am J Gastroenterol 106(7):1231–1238
Oelschlager BK, Barreca M, Chang L, Oleynikov D, Pellegrini CA (2003) Clinical and pathologic response of Barrett’s esophagus to laparoscopic antireflux surgery. Ann Surg 238(4):458–464
Hofstetter WL, Peters JH, DeMeester TR, Hagen JA, DeMeester SR, Crookes PF, Tsai P, Banki F, Bremner CG (2001) Long-term outcome of antireflux surgery in patients with Barrett’s esophagus. Ann Surg 234(4):532–538
Chang EY, Morris CD, Seltman AK, O’Rourke RW, Chan BK, Hunter JG, Jobe BA (2007) The effect of antireflux surgery on esophageal carcinogenesis in patients with Barrett esophagus: a systematic review. Ann Surg 246(1):11–21
Kauer WKH, Peters JH, DeMeester TR, Ireland AP, Bremner CG, Hagen JA (1995) Mixed reflux of gastric and duodenal juices is more harmful to the esophagus than gastric juice alone: the need for surgical therapy re-emphasized. Ann Surg 222(4):525–533
Parilla P, Martínez de Haro LF, Ortiz A, Munitiz V, Molina J, Bermejo J, Canteras M (2003) Long-term results of a randomized prospective study comparing medical and surgical treatment of Barrett’s esophagus. Ann Surg 237(3):291–298
Rees JRE, Lao-Sirieix P, Wong A, Fitzgerald RC (2011) Treatment for Barrett’s oesophagus. Cochrane Database Syst Rev doi:10.1002/14651858
Wassenaar EB, Oelschlager BK (2010) Effect of medical and surgical treatment of Barrett’s metaplasia. World J Gastroenterol 16(30):3773–3779
Goldblum JR, Lauwers GY (2002) Dysplasia arising in Barrett’s esophagus: diagnostic pitfalls and natural history. Semin Diagn Pathol 19(1):12–19
Spechler SJ, Sharma P, Souza RF, Inadomi JM, Shaheen NJ (2011) American gastroenterological association technical review on the management of Barrett’s esophagus. Gastroenterology 140(3):e18–e52
Sharma FalkGW, Weston AP, Reker D, Johnston M, Sampliner RE (2006) Dysplasia and cancer in a large multicenter cohort of patients with Barrett’s esophagus. Clin Gastroenterol Hepatol 4(5):566–572
Hvid-Jensen F, Pedersen L, Drewes AM, Sorensen HT, Funch-Jensen P (2011) Incidence of adenocarcinoma among patients with Barrett’s esophagus. New Engl J Med 365:1375–1383
Millind R, Attwood SE (2012) Natural history of Barrett’s esophagus. World J Gastroenterol 18(27):3483–3491
Curvers WL, Ten Kate FJ, Krishnadath KK, Visser M, Elzer B, Baak LC, Bohmer C, Mallant-Hent RC, van Oijen A, Naber AH, Scholten P, Busch OR, Blaauwgeers HG, Meijer GA, Bergman JJ (2010) Low-grade dysplasia in Barrett’s esophagus: overdiagnosed and underestimated. Am J Gastroenterol 105:1523–1530
Ajumobi A, Bahjri K, Jackson C, Griffin R (2010) Surveillance in Barrett’s esophagus: an audit of practice. Dig Dis Sci 55(6):1615–1621
Acknowledgments
The authors would like to acknowledge Ana Martin for her work on the prospectively maintained Center for Esophageal and Gastric Surgery database. This study was funded by a SAGES grant.
Disclosures
Dr. Oelschlager has the following relationships, none of which are related to the content of this study: Covidien (Resident education grant, consulting), Torax Medical (Research grant), EndoGastric Solutions (Consultant and research grant), VisionGate (Research grant), Cook BioMedical (Instructor/consultant), Web MD (Advisory Board/consultant). Drs. Morrow, Wassenaar, Hinojosa, Loviscek, Pellegrini and Mr. Bushyhead have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Morrow, E., Bushyhead, D., Wassenaar, E. et al. The impact of laparoscopic anti-reflux surgery in patients with Barrett’s esophagus. Surg Endosc 28, 3279–3284 (2014). https://doi.org/10.1007/s00464-014-3601-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3601-z