Abstract
Background
Parastomal hernia (PSH) is a frequent complication following the creation of a stoma. While a significant number of cases require operative management, data comparing short-term outcomes of laparoscopic versus open repair of parastomal hernias are limited.
Methods
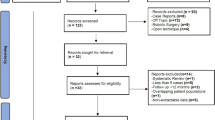
The ACS-NSQIP was retrospectively reviewed from 2005 to 2011 for all PSH cases that underwent open or laparoscopic repair. Patients characteristics, operative details, and outcomes were listed for both procedure types. Selected end points were compared on multivariate regression analysis.
Results
Among the 2,167 identified parastomal hernia cases, only 222 (10.24 %) were treated laparoscopically. The open and laparoscopic groups were similar with respect to mean patient age (63 vs. 63 years; p = 1) and gender distribution as the majority of patients were females (56.8 %). However, open repair was more likely to be performed in patients with a higher ASA class (III and IV) (p < 0.001). Also, the open approach was more likely to be used emergently (8.64 vs. 3.60 %; p = 0.01) and for recurrent hernias (6.99 vs. 3.15 %; p < 0.05). After adjusting for all potential confounders including age, gender, ASA, emergency designation of the operation, hernia type, and wound class, laparoscopy was associated with shorter operative time (137.5 vs. 153.4 min; p < 0.05), shorter length of hospital stay by 3.32 days (p < 0.001), lower risk of overall morbidity (OR = 0.42; p < 0.001), and a lower risk of surgical site infections (OR = 0.35; p < 0.01) compared to open repair. Mortality rates were similar in the laparoscopic and open groups (0.45 vs. 1.59 %, respectively; p = 0.29).
Conclusions
Laparoscopic parastomal hernia repair is safe and appears to be associated with better short-term outcomes compared to open repair in selected cases. Large prospective randomized trials are needed to confirm those results and to assess long-term recurrence rates.
Similar content being viewed by others
References
Turnbull GB (2003) Ostomy statistics: the $64,000 question. Ostomy Wound Manag 49(6):22–23
Brown H, Randle J (2005) Living with a stoma: a review of the literature. J Clin Nurs 14(1):74–81
Persson E, Berndtsson I, Carlsson E, Hallen AM, Lindholm E (2010) Stoma-related complications and stoma size: a 2-year follow up. Colorectal Dis 12(10):971–976
Mahjoubi B, Moghimi A, Mirzaei R, Bijari A (2005) Evaluation of the end colostomy complications and the risk factors influencing them in Iranian patients. Colorectal Dis 7(6):582–587
Neuman HB, Park J, Fuzesi S, Temple LK (2012) Rectal cancer patients’ quality of life with a temporary stoma: shifting perspectives. Dis Colon Rectum 55(11):1117–1124
Kald A, Juul KN, Hjortsvang H, Sjodahl RI (2008) Quality of life is impaired in patients with peristomal bulging of a sigmoid colostomy. Scand J Gastroenterol 43(5):627–633
Ripoche J, Basurko C, Fabbro-Perray P, Prudhomme M (2011) Parastomal hernia. A study of the French federation of ostomy patients. J Visc Surg 148(6):e435–e441
Hansson BM, Slater NJ, van der Velden AS et al (2012) Surgical techniques for parastomal hernia repair: a systematic review of the literature. Ann Surg 255(4):685–695
Israelsson LA (2005) Preventing and treating parastomal hernia. World J Surg 29(8):1086–1089
Hotouras A, Murphy J, Thaha M, Chan C (2013) The persistent challenge of parastomal herniation: a review of the literature and future developments. Colorectal Dis 15(5):e202–e214
Asif A, Ruiz M, Yetasook A et al (2012) Laparoscopic modified Sugarbaker technique results in superior recurrence rate. Surg Endosc 26(12):3430–3434
Craft RO, Huguet KL, McLemore EC, Harold KL (2008) Laparoscopic parastomal hernia repair. Hernia 12(2):137–140
Hansson BM, Bleichrodt RP, de Hingh IH (2009) Laparoscopic parastomal hernia repair using a keyhole technique results in a high recurrence rate. Surg Endosc 23(7):1456–1459
Hansson BM, de Hingh IH, Bleichrodt RP (2007) Laparoscopic parastomal hernia repair is feasible and safe: early results of a prospective clinical study including 55 consecutive patients. Surg Endosc 21(6):989–993
Hansson BM, Morales-Conde S, Mussack T, Valdes J, Muysoms FE, Bleichrodt RP (2013) The laparoscopic modified Sugarbaker technique is safe and has a low recurrence rate: a multicenter cohort study. Surg Endosc 27(2):494–500
Mancini GJ, McClusky DA 3rd, Khaitan L et al (2007) Laparoscopic parastomal hernia repair using a nonslit mesh technique. Surg Endosc 21(9):1487–1491
Mizrahi H, Bhattacharya P, Parker MC (2012) Laparoscopic slit mesh repair of parastomal hernia using a designated mesh: long-term results. Surg Endosc 26(1):267–270
Muysoms F (2007) Laparoscopic repair of parastomal hernias with a modified Sugarbaker technique. Acta Chir Belg 107(4):476–480
Safadi B (2004) Laparoscopic repair of parastomal hernias: early results. Surg Endosc 18(4):676–680
Wara P, Andersen LM (2011) Long-term follow-up of laparoscopic repair of parastomal hernia using a bilayer mesh with a slit. Surg Endosc 25(2):526–530
Steele SR, Lee P, Martin MJ, Mullenix PS, Sullivan ES (2003) Is parastomal hernia repair with polypropylene mesh safe? Am J Surg 185(5):436–440
Guzman-Valdivia G, Guerrero TS, Laurrabaquio HV (2008) Parastomal hernia-repair using mesh and an open technique. World J Surg 32(3):465–470
Longman RJ, Thomson WH (2005) Mesh repair of parastomal hernias: a safety modification. Colorectal Dis 7(3):292–294
Stelzner S, Hellmich G, Ludwig K (2004) Repair of paracolostomy hernias with a prosthetic mesh in the intraperitoneal onlay position: modified Sugarbaker technique. Dis Colon Rectum 47(2):185–191
van Sprundel TC, van der Hoop AG (2005) Modified technique for parastomal hernia repair in patients with intractable stoma-care problems. Colorectal Dis 7(5):445–449
Pastor DM, Pauli EM, Koltun WA, Haluck RS, Shope TR, Poritz LS (2009) Parastomal hernia repair: a single center experience. J Soc Laparoendosc Surg 13(2):170–175
American College of Surgeons National Surgical Quality Improvement Program (NSQIP) (2012) User guide for the participant use data file, 2005–2010. http://site.acsnsqip.org/participant-use-data-file/. Accessed 19 Oct 2012
Simorov A, Shaligram A, Shostrom V, Boilesen E, Thompson J, Oleynikov D (2012) Laparoscopic colon resection trends in utilization and rate of conversion to open procedure: a national database review of academic medical centers. Ann Surg 256(3):462–468
Kang CY, Halabi WJ, Luo R, Pigazzi A, Nguyen NT, Stamos MJ (2012) Laparoscopic colorectal surgery: a better look into the latest trends. Arch Surg 147(8):724–731
Berger D, Bientzle M (2007) Laparoscopic repair of parastomal hernias: a single surgeon’s experience in 66 patients. Dis Colon Rectum 50(10):1668–1673
Sauerland S, Walgenbach M, Habermalz B, Seiler CM, Miserez M (2011) Laparoscopic versus open surgical techniques for ventral or incisional hernia repair. Cochrane Database Syst Rev 3:CD007781
LeBlanc KA, Bellanger DE, Whitaker JM, Hausmann MG (2005) Laparoscopic parastomal hernia repair. Hernia 9(2):140–144
Veenhof AA, Vlug MS, van der Pas MH et al (2012) Surgical stress response and postoperative immune function after laparoscopy or open surgery with fast track or standard perioperative care: a randomized trial. Ann Surg 255(2):216–221
Hemandas AK, Abdelrahman T, Flashman KG et al (2010) Laparoscopic colorectal surgery produces better outcomes for high risk cancer patients compared to open surgery. Ann Surg 252(1):84–89
Kang CY, Halabi WJ, Chaudhry OO et al (2013) A nationwide analysis of laparoscopy in high-risk colorectal surgery patients. J Gastrointest Surg 17(2):382–391
Pilgrim CH, McIntyre R, Bailey M (2010) Prospective audit of parastomal hernia: prevalence and associated comorbidities. Dis Colon Rectum 53(1):71–76
Disclosures
The Department of Statistics at UC Irvine, with which V. Nguyen and M. Phelan are affiliated, was paid a statistical consulting fee by the Department of Surgery at UC Irvine. The Department of Surgery at UC Irvine, with which S. Mills is affiliated, was paid an educational grant from Ethicon. Ethicon, Covidien, Olympus, Adolor, and NiTi gave educational grants and speaker fees to the Department of Surgery at UC Irvine, with which M. Stamos is affiliated. Intuitive Surgical paid consultancy and educational grants to the Department of Surgery at UC Irvine, with which A. Pigazzi is affiliated.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Halabi, W.J., Jafari, M.D., Carmichael, J.C. et al. Laparoscopic versus open repair of parastomal hernias: an ACS-NSQIP analysis of short-term outcomes. Surg Endosc 27, 4067–4072 (2013). https://doi.org/10.1007/s00464-013-3062-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-3062-9