Abstract
Introduction
The results of cardiomyotomy in patients of achalasic megaesophagus with axis deviation are not satisfactory, and several authors have advocated an esophagectomy in these patients. We describe the technical details and outcomes of a novel technique of laparoscopic esophagogastroplasty for end-stage achalasia.
Methods
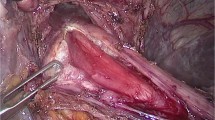
Patients with end-stage achalasia, characterized by tortuous megaesophagus were selected. The surgery was performed in supine position using five abdominal ports. The steps included mobilization of the gastroesophageal junction and lower intrathoracic esophagus, straightening and anchoring the pulled intrathoracic esophagus into the abdomen, and a side-side esophagogastroplasty.
Results
Four patients with megaesophagus due to end-stage achalasia underwent this procedure. The average duration of surgery was 177.5 (range, 120–240) min. All patients could be ambulated on the first postoperative day. Oral feeding was initiated by the third postoperative day, and all patients had significant improvements in their dysphagia scores. All patients had excellent cosmetic results and were discharged by the fifth postoperative day. An upper gastrointestinal contrast study done at 6 weeks after surgery did not show any hold up of contrast, and there was decrease in the convolutions and diameter of the esophagus. At a mean follow-up of 10.5 (range, 3–15) months, all patients are euphagic without significant symptoms of gastroesophageal reflux.
Conclusions
Laparoscopic esophagogastroplasty is an effective option for relieving dysphagia in megaesophagus due to achalasia with axis deviation and is a reasonable alternative before subjecting to a major and potentially morbid esophagectomy.


Similar content being viewed by others
References
Campos GM, Vittinghoff E, Rabl C, Takata M, Gadenstätter M, Lin F, Ciovica R (2009) Endoscopic and surgical treatments for achalasia: a systematic review and meta-analysis. Ann Surg 249(1):45–57
Goldblum JR, Rice TW, Richter JE (1996) Histopathologic features in esophagomyotomy specimens from patients with achalasia. Gastroenterology 111(3):648–654
Woltman TA, Pellegrini CA, Oelschlager BK (2005) Achalasia. Surg Clin North Am 85(3):483–493
Vaezi MF, Richter JE (1999) Diagnosis and management of achalasia. American College of Gastroenterology Practice Parameter Committee. Am J Gastroenterol 94(12):3406–3412
Devaney EJ, Lannettoni MD, Orringer MB, Marshall B (2001) Esophagectomy for achalasia: patient selection and clinical experience. Ann Thorac Surg 72(3):854–858
Palanivelu C, Rangarajan M, Jategaonkar PA, Maheshkumaar GS, Vijay Anand N (2008) Laparoscopic transhiatal esophagectomy for ‘sigmoid’ megaesophagus following failed cardiomyotomy: experience of 11 patients. Dig Dis Sci 53(6):1513–1518
Gockel I, Kneist W, Eckardt VF, Oberholzer K, Junginger T (2004) Subtotal esophageal resection in motility disorders of the esophagus. Dig Dis 22(4):396–401
Pechlivanides G, Chrysos E, Athanasakis E, Tsiaoussis J, Vassilakis JS, Xynos E (2001) Laparoscopic Heller cardiomyotomy and Dor fundoplication for esophageal achalasia: possible factors predicting outcome. Arch Surg 136(11):1240–1243
Stefanidis D, Richardson W, Farrell TM, Kohn GP, Augenstein V, Fanelli RD, Society of American Gastrointestinal and Endoscopic Surgeons (2012) SAGES guidelines for the surgical treatment of esophageal achalasia. Surg Endosc 26(2):296–311
Hsu HS, Wang CY, Hsieh CC, Huang MH (2003) Short-segment colon interposition for end-stage achalasia. Ann Thorac Surg 76(5):1706–1710
Banki F, Mason RJ, DeMeester SR, Hagen JA, Balaji NS, Crookes PF, Bremner CG, Peters JH, DeMeester TR (2002) Vagal-sparing esophagectomy: a more physiologic alternative. Ann Surg 236(3):324–335 discussion 335-336
Disclosures
Drs. Amit Javed and Anil K. Agarwal have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Agarwal, A.K., Javed, A. Laparoscopic esophagogastroplasty: a minimally invasive alternative to esophagectomy in the surgical management of megaesophagus with axis deviation. Surg Endosc 27, 2238–2242 (2013). https://doi.org/10.1007/s00464-012-2751-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-012-2751-0