Abstract
Background
Neoadjuvant chemoradiation (nCRT) currently is commonly incorporated into the multimodal treatment of locally advanced rectal cancers. This study aimed to compare the short-term outcomes and oncologic adequacy of laparoscopic and conventional open surgery for rectal cancer after nCRT.
Methods
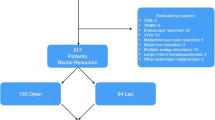
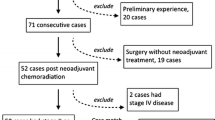
A series of 72 patients who underwent laparoscopic surgery (Lap group) for rectal cancer after nCRT were matched for type of surgery, gender, and American Society of Anesthesiologists (ASA) class with 72 patients who underwent conventional surgery during the same time period (Open group). The short-term outcomes were compared between the two groups of patients.
Results
No significant difference was found between the two groups in terms of age, distance of tumor from the anal verge, body mass index, or posttreatment pathologic stage of the disease. There were significant differences between the Lap and Open groups in terms of blood loss (median: 200 vs 400 ml; P < 0.001), duration of surgery (median: 270 vs 240 min; P < 0.001), time to passing of first flatus (median: 2 vs 3 days; P < 0.001), time to start of normal diet (median: 5 vs 6 days; P < 0.001), and hospital stay (median: 12 vs 15 days; P < 0.001). A significant difference in the number of lymph nodes harvested was not identified between the two groups, although more patients in the Open group had a positive circumferential resection margin than in the Lap group (10 vs 1%; P = 0.03). The short-term benefits of laparoscopic surgery also were observed when the 64 patients who underwent abdominoperineal resection (APR) in each of the two groups were compared separately.
Conclusion
Laparoscopic surgery for rectal cancer, especially laparoscopic APR, after nCRT is safe and associated with earlier recovery of bowel function, a shorter hospital stay, and an oncologically adequate specimen compared with conventional open surgery.
Similar content being viewed by others
References
Miyajima N, Fukunaga M, Hasegawa H, Tanaka J, Okuda J, Watanabe M, Japan Society of Laparoscopic Colorectal Surgery (2009) Results of a multicenter study of 1, 057 cases of rectal cancer treated by laparoscopic surgery. Surg Endosc 23:113–118
Ströhlein MA, Grützner KU, Jauch KW, Heiss MM (2008) Comparison of laparoscopic vs open access surgery in patients with rectal cancer: a prospective analysis. Dis Colon Rectum 51:385–391
Gouvas N, Tsiaoussis J, Pechlivanides G, Zervakis N, Tzortzinis A, Avgerinos C, Dervenis C, Xvnos E (2009) Laparoscopic or open surgery for the cancer of the middle and lower rectum: short-term outcomes of a comparative nonrandomised study. Int J Colorectal Dis 24:761–769
Morino M, Allaix ME, Giraudo G, Corno F, Garrone C (2005) Laparoscopic versus open surgery for extraperitoneal rectal cancer: a prospective comparative study. Surg Endosc 19:1460–1467
Lujan J, Valero G, Hernandez Q, Sanchez A, Frutos MD, Parrilla P (2009) Randomized clinical trial comparing laparoscopic and open surgery in patients with rectal cancer. Br J Surg 96:982–989
Ng SSM, Leung KL, Lee JFY, Yiu RYC, Li JCM, Teoh AYB, Leung WW (2008) Laparoscopic-assisted versus open abdominoperineal resection for low rectal cancer: a prospective randomized trial. Ann Surg Oncol 15:2418–2425
Zhou Z-G, Hu M, Lei W-Z, Yu Y-Y, Cheng Z, LI L, Shu Y, Wang T-C (2004) Laparoscopic vs open total mesorectal excision with anal sphincter preservation for low rectal cancer. Surg Endosc 18:1211–1215
Gao F, Cao Y-F, Chen L-S (2006) Meta-analysis of short-term outcomes after laparoscopic resection for rectal cancer. Int J Colorectal Dis 21:652–656
Aziz O, Constantinides V, Tekkis PP, Athanasiou T, Purkayastha S, Paraskeva P, Darzi AW, Heriot AG (2006) Laparoscopic versus open surgery for rectal cancer: a meta-analysis. Ann Surg Oncol 13:413–424
Breukink S, Pierie JP, Wiggers T (2006) Laparoscopic versus open total mesorectal excision for rectal cancer. Cochrane Database of Systematic Reviews 2006, Issue 4. Art. no. CD005200. doi:10.1002/14651858.CD005200.pub2
Anderson C, Uman G, Pigazzi A (2008) Oncologic outcomes of laparoscopic surgery for rectal cancer: a systematic review and meta-analysis of the literature. Eur J Surg Oncol 34:1135–1142
Laurent C, Leblanc F, Wütrich P, Scheffler M, Rullier E (2009) Laparoscopic versus open surgery for rectal cancer: long-term oncologic results. Ann Surg 250:54–61
Leroy J, Jamali F, Forbes L, Smith M, Rubino F, Mutter D, Marescaux J (2004) Laparoscopic total mesorectal excision (TME) for rectal cancer surgery: long-term outcomes. Surg Endosc 18:281–289
Sauer R, Becker H, Hohenberger W, Rodel C, Wittekind C, Fietkau R, Martus P, Tschmelitsch J, Hager E, Hess CF, Karstens JH, Liersch T, Schmidberger H, Raab R, For the German Rectal Cancer Study Group (2004) Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med 351:1731–1740
Marijnen CAM, Kapiteijn E, van de Velde CJH, Martijn H, Steup WH, Wiggers T, Kranenbarg EK, Leer JWH, The cooperative investigators of the Dutch Colorectal Cancer Group (2002) Acute side effects and complications after short-term preoperative radiotherapy combined with total mesorectal excision in primary rectal cancer: report of a multicenter randomized trial. J Clin Oncol 20:817–825
Stockholm Rectal Cancer Study Group (1990) Preoperative short-term radiation therapy in operable rectal carcinoma: a prospective randomized trial. Cancer 66:49–55
Akiyoshi T, Kuroyanagi H, Oya M, Konishi T, Fuuda M, Fujimoto Y, Ueno M, Yamaguchi T, Muto T (2009) Safety of laparoscopic total mesorectal excision for low rectal cancer with preoperative chemoradiation therapy. J Gastrointest Surg 13:521–525
Quirke P, Dixon MF, Durdey P, Williams NS (1986) Local recurrence of rectal adenocarcinoma due to inadequate surgical resection: histological study of lateral tumor spread and surgical excision. Lancet 328:996–999
Nissan A, Guillem JG, Paty PB, Douglas Wong W, Minsky B, Saltz L, Cohen AM (2001) Abdominoperineal resection for rectal cancer at a specialty center. Dis Colon Rectum 44:27–35
Stelzmueller I, Zitt M, Aigner F, Kafka-Ritsch R, Jager R, De Vries A, Lukas P, Eisterer W, Bonatti H, Ofner D (2009) Postoperative morbidity following chemoradiation for locally advanced low rectal cancer. J Gastrointest Surg 13:657–667
Cheung HY, Chung CC, Wong JC, Yau KK, Li MK (2009) Laparoscopic rectal cancer surgery with and without neoadjuvant chemo-irradiation: a comparative study. Surg Endosc 23:147–152
Rezvani M, Franko J, Fassler Sa, Harper SG, Neiman JH, Zebley DM (2007) Outcomes in patients treated by laparoscopic resection of rectal carcinoma after neoadjuvant therapy for rectal cancer. JSLS 11:204–207
Pugliese R, Di Lernia S, Sansonna F, Maggioni D, Ferrari GC, Magistro C, Costanzi A, DeCarli S, Artale S, Pugliese F (2009) Laparoscopic resection for rectal adenocarcinoma. Eur J Surg Oncol 35:497–503
Araujo SE, da Silva eSousa AH Jr, de Campos FG, Habr-Gama A, Dumarco RB, Caravatto PP, Nahas SC, da Silva J, Kiss DR, Gama-Rodrigues JJ (2003) Conventional approach x laparoscopic abdominoperineal resection for rectal cancer treatment after neoadjuvant chemoradiation: results of a prospective randomized trial. Rev Hosp Clin Fac Med Sao Paulo 58:133–140
Kang SB, Park JW, Jeong SY, Nam BH, Choi HS, Kim DW, Lim SB, Lee TG, Kim DY, Kim JS, Chang HJ, Lee HS, Kim SY, Jung KH, Hong YS, Kim JH, Sohn DK, Kim DH, Oh JH (2010) Open versus laparoscopic surgery for mid or low rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): short-term outcomes of an open-label randomized controlled trial. Lancet Oncol 11:637–645
Breukink O, Pierie JPEN, Grond AJK, Hoff C, Wiggers T, Meijerink WJHJ (2005) Laparoscopic versus open total mesorectal excision: a case-control study. Int J Colorectal Dis 20:428–433
Denoya P, Wang H, Sands D, Nogueras J, Weiss E, Wexner SD (2010) Short-term outcomes of laparoscopic total mesorectal excision following neoadjuvant chemoradiotherapy. Surg Endosc 24:933–938
Bullard KM, Trudel JL, Baxter NN, Rothenberger DA (2005) Primary perineal wound closure after preoperative radiotherapy and abdominoperineal resection has a high incidence of wound failure. Dis Colon Rectum 48:438–443
Marks JH, Valsdottir EB, Rather AA, Nweze IC, Newman DA, Chernick MR (2010) Fewer than 12 lymph nodes can be expected in a surgical specimen after high-dose chemoradiation therapy for rectal cancer. Dis Colon Rectum 53:1023–1029
Wijesuriya RE, Deen KI, Hewavisenthi J, Balawardana J, Perera M (2005) Neoadjuvant therapy for rectal cancer downstages the tumor but reduces lymph node harvest significantly. Surg Today 35:442–445
Morcos B, Baker B, Al Masri M, Haddad H, Hashem S (2010) Lymph node yield in rectal cancer surgery: effect of preoperative chemoradiotherapy. Eur J Surg Oncol 36:345–349
Waizer A, Zitron S, Ben-Baruch D (1989) Comparative study for preoperative staging of rectal cancer. Dis Colon Rectum 32:53–56
Augestad KM, Lindsetmo RO, Stulberg J, Reynolds H, Senagore A, Champagne B, Heriot AG, Leblanc F, Delaney CP, International Rectal Cancer Study Group (IRCSG) (2010) International preoperative rectal cancer management: staging, neoadjuvant treatment, and impact of multidisciplinary teams. World J Surg 34:2689–2700
Acknowledgment
We acknowledge the immense help rendered by Mr. M. Sivakumar of the Tumor Registry, Cancer Institute (WIA), Chennai in maintaining the medical records of the patients.
Disclosures
Ramakrishnan Ayloor Seshadri, Ayyappan Srinivasan, RiteshTapkire, and Rajaraman Swaminathan have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Seshadri, R.A., Srinivasan, A., Tapkire, R. et al. Laparoscopic versus open surgery for rectal cancer after neoadjuvant chemoradiation: a matched case-control study of short-term outcomes. Surg Endosc 26, 154–161 (2012). https://doi.org/10.1007/s00464-011-1844-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-1844-5