Abstract
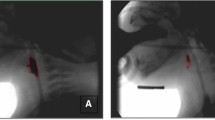
Currently, no method exists to measure the size of pharyngeal and laryngeal structures on endoscopy. Imaging for dysphagia diagnostic techniques, for the most part, still relies on qualitative assumptions and cursory visual examinations to induce patients’ swallowing safety and function. In this proof of concept study, we measured vallecular cavity volume using simultaneous modified barium swallows (MBS) and flexible endoscopic evaluation of swallowing (FEES). Similar to the three-dimensional image compilation fields of facial reconstruction, medical imagery, and forensic science, this proposed methodology combines the two-dimensional images yielded in FEES and MBS videos to calculate estimates of the valleculae in a 3D perspective. A tracking tool was used to measure distances on MBS, while endoscopic specifications were used to find distances on FEES. This combination of ratio measurements allowed for measurement on both the MBS and FEES. In a sample of n = 37 dysphagia patients referred for MBS/FEES studies, the mean distance from the tip of endoscope to the closest point of epiglottis was 25.38 mm, the mean vallecular area outlined on MBS video was 84.72 mm2, the mean epiglottal width was 18.16 mm, and the mean vallecular volume was 1.55 mL. Future application could include tracking growth of tumors, glottic opening, volume of residue and tracking of any other important outcome involving movement, size, and targets of interest with higher precision.







Similar content being viewed by others
References
Rosenbek JC, Robbins JA, Roecker EB, Coyle JL, Wood JL. A penetration-aspiration scale. Dysphagia. 1996;11(2):93–8.
Pearson WG Jr, Molfenter SM, Smith ZM, Steele CM. Image-based measurement of postswallow residue: the normalized residue ratio scale. Dysphagia. 2013;28(2):167–77.
Schwertner RW, Garand KL, Pearson WG Jr. A novel imaging analysis method for capturing pharyngeal constriction during swallowing. J Imaging Sci. 2016;1(1):1–6.
Stuani VT, Rafael F, Manfredi GGP, Cardoso MV, Sant'Ana ACP. Photogrammetry as an alternative for acquiring digital dental models: a proof of concept. Med Hypotheses. 2019;128:43–9.
Chen Q, Xu H, Tan L. Application of composite small calibration objects in traffic accident scene photogrammetry. PLoS ONE. 2015;10:5.
Ramona M, Meier S, Ebert LC, Martinez RM, Sieberth T. Comparison of forensic photo-documentation to a photogrammetric solution using the multi-camera system “Botscan”. Forensic Sci Int. 2018;288:46–52.
Leipner A, Obertová Z, Wermuth M, Thali M, Ottiker T, Sieberth T. 3D mug Shot—3D head models from photogrammetry for forensic identification. Forensic Sci Int. 2019;300:6–12.
Yuan X, Cheng T, Xiaohai X, Gao Z, Li Q, Liu X, Wang X, Song R, Xiangyang J, Zhang Q. High-accuracy and real-time 3D positioning, tracking system for medical imaging applications based on 3D digital image correlation. Opt Lasers Eng. 2017;88:82–90.
IEEE Computer Society. Recognition, analysis, and tracking of faces and gestures in real-time systems. In: Proceedings: IEEE ICCV workshop on recognition, analysis, and tracking of faces and gestures in real-time systems: 13 July, 2001. Vancouver: IEEE Computer Society; 2001.
Garand KL, Schwertner R, Chen A, Pearson WG Jr. Computational analysis of pharyngeal swallowing mechanics in patients with motor neuron disease: a pilot investigation. Dysphagia. 2018;33(2):243–50.
May NH, Pisegna JM, Marchina S, Langmore SE, Kumar S, Jr Pearson WG. Pharyngeal swallowing mechanics secondary to hemispheric stroke. J Stroke Cerebrovasc Dis. 2016;26(5):952–61.
Molfenter SM, Steele CM. The relationship between residue and aspiration on the subsequent swallow: an application of the normalized residue ratio scale. Dysphagia. 2013;28(4):494–500.
“TIMS DICOM.” TIMS MEDICAL, By Foresight Imaging, 2018. www.tims.com/timsdicom-system/.
“Final Cut Pro.” Apple, Pro AFC, IN:10.3.4. www.support.apple.com/en-us/HT201237.
Rasband W. ImageJ 1.49v. Bethesda: National Institutes of Health; 1997–2015.
Schneider CA, Rasband WS, Eliceiri KW. NIH image to ImageJ: 25 years of image analysis. Nat Methods. 2012;9(7):671–5.
Neubauer PD, Hersey DP, Leder SB. Pharyngeal residue severity rating scales based on fiberoptic endoscopic evaluation of swallowing: a systematic review. Dysphagia. 2016;31(3):352–9.
Rademaker AW, Pauloski BR, Logemann JA, Shanahan TK. Oropharyngeal swallow efficiency as a representative measure of swallowing function. J Speech Hear Res. 1994;37(2):314–25.
Martin-Harris B, Brodsky MB, Michel Y, et al. MBS measurement tool for swallow impairment—MBSImp: establishing a standard. Dysphagia. 2008;23(4):392–405.
Hutcheson KA, Barrow MP, Barringer DA, et al. Dynamic imaging grade of swallowing toxicity (DIGEST): scale development and validation. Cancer. 2017;123(1):62–70.
Imam H, Marrero F, Shay S. Impedance nadir values correlate with barium bolus amount. Dis Esophagus. 2012;25(7):600–7.
Ding P, Campbell-Malone R, Holman SD, Lukasik SL, Thexton AJ, German RZ. The effect of unilateral superior laryngeal nerve lesion on swallowing threshold volume. Laryngoscope. 2013;123(8):1942–7.
Ding P, Fung GS, Lin M, Holman SD, German RZ. The effect of bilateral superior laryngeal nerve lesion on swallowing: a novel method to quantitate aspirated volume and pharyngeal threshold in videofluoroscopy. Dysphagia. 2015;30(1):47–56.
Choi DG, Bok Y, Kim JS, Shim I, Kweon IS. Structure-from-motion in 3D space using 2D lidars. Sensors. 2017. https://doi.org/10.3390/s17020242.
Singh K, Singh S, Gupta R, Gathwal C, Bansal P, Singh M. A feasibility study to assess vallecula and pyriform sinus using protocol-based ultrasonic evaluation of floor of mouth and upper airway. Saudi J Anaesth. 2017;11(3):299–304.
Dyer JC, Leslie P, Drinnan MJ. Objective computer-based assessment of valleculae residue—is it useful? Dysphagia. 2008;23(1):7–15.
Kaneoka AS, Langmore SE, Krisciunas GP, et al. The boston residue and clearance scale: preliminary reliability and validity testing. Folia Phoniatr Logop. 2013;65(6):312–7.
Neubauer PD, Rademaker AW, Leder SB. The yale pharyngeal residue severity rating scale: an anatomically defined and image-based tool. Dysphagia. 2015;30(5):521–8.
Park JM, Yong SY, Kim JH, et al. Cutoff value of pharyngeal residue in prognosis prediction after neuromuscular electrical stimulation therapy for Dysphagia in subacute stroke patients. Ann Rehabil Med. 2014;38(5):612–9.
Pisegna JM, Kaneoka A, Langmore S. Danger zones: rating residue in 3 zones to identify those at risk for penetration/aspiration on FEES. Phoenix: Dysphagia Research Society; 2016.
Daniel MM, Lorenzi MC, da Costa LC, Lorenzi-Filho G. Pharyngeal dimensions in healthy men and women. Clinics. 2007;62(1):5–10.
Lin J, Walsted ES, Backer V, Hull JH, Elson D. Quantification and analysis of laryngeal closure from endoscopic videos. IEEE Trans Biomed Eng. 2018;66(4):1127–36.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No potential conflict of interest was reported by the authors.
Research Involving Human Participants
MBS and FEES videos used in this study were from procedures already ordered for patient by physician (second author) as part of treatment. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, K., Pisegna, J.M., Kennedy, S. et al. Measuring Vallecular Volume on Flexible Endoscopic Evaluation of Swallowing: A Proof of Concept Study. Dysphagia 36, 96–107 (2021). https://doi.org/10.1007/s00455-020-10106-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00455-020-10106-1