Abstract
Scarce evidence exists about the best treatment for multi-system inflammatory syndrome (MIS-C). We analyzed the effects of steroids, intravenous immunoglobulin (IVIG), and their combination on the probability of discharge over time, the probability of switching to second-line treatment over time, and the persistence of fever 2 days after treatment. We did a retrospective study to investigate the effect of different treatments on children with MIS-C from 1 March 2020 to 1 June 2021. We estimated the time-to-event probability using a Cox model weighted by propensity score to balance the baseline characteristics. Thirty of 132 (22.7%) patients were initially treated with steroids alone, 29/132 (21.9%) with IVIG alone, and 73/132 (55%) with IVIG plus steroids. The probability of early discharge was higher with IVIG than with IVIG plus steroids (hazard ratio [HR] 1.65, 95% CI 1.11–2.45, p = 0.013), but with a higher probability of needing second-line therapy compared to IVIG plus steroids (HR 3.05, 95% CI 1.12–8.25, p = 0.028). Patients on IVIG had a higher likelihood of persistent fever than patients on steroids (odds ratio [OR] 4.23, 95% CI 1.43–13.5, p = 0.011) or on IVIG plus steroids (OR 4.4, 95% CI 2.05–9.82, p < 0.001). No differences were found for this endpoint between steroids or steroids plus IVIG.
Conclusions: The benefits of each approach may vary depending on the outcome assessed. IVIG seemed to increase the probability of earlier discharge over time but also of needing second-line treatment over time. Steroids seemed to reduce persistent fever, and combination therapy reduced the need for escalating treatment.
What is Known: • Steroids plus intravenous immunoglobulin, compared with intravenous immunoglobulin alone for multi-system inflammatory syndrome (MIS-C) might reduce the need for hemodynamic support and the duration of fever, but the certainty of the evidence is low. | |
What is New: • Intravenous immunoglobulin, steroids, and their combination for MIS-C may have different outcomes. • In this study, intravenous immunoglobulin increased the probability of discharge over time, steroids reduced persistent fever, while combination therapy reduced the need for second-line treatments. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multi-system inflammatory syndrome in children (MIS-C) is a newly described condition characterized by the dysregulated response of the immune system after severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection. During the first waves of the coronavirus disease 2019 (COVID-19) pandemic, peaks of MIS-C cases were reported worldwide [1, 2]. In Spain, in August 2020, a national guideline defined the treatment of MIS-C. The first line is IVIG or steroids. In severe cases or without response, it is recommended to combine them [3]. Before this guideline, because of the inflammatory nature of this condition and the overlapping features with Kawasaki disease, attending physicians started treating MIS-C with either steroids, intravenous immunoglobulin (IVIG), or their combination [3,4,5,6,7]. However, there is no high level of evidence that supports the use of one of the three therapeutical options versus the others [8].
The present study aimed to analyze the effect of steroids, IVIG, or their combination on the probability of discharge and of needing second-line treatment over time. As a secondary endpoint, we analyzed the effect of the drugs on persistent fever after 2 days of treatment.
Methods
We assessed children with MIS-C based on the WHO definition [9], and enrolled prospectively in the Epidemiological Study of COVID-19 in Children of the Spanish Society of Pediatrics (EPICO-AEP) [1]. They were diagnosed from 1 March 2020 to 1 June 2021. The study was approved by the Ethics Committee of Hospital 12 de Octubre, Madrid (code 20/101), and other participating hospitals. Participants were enrolled after signed or verbal consent from parents/guardians and by the consent of patients older than 12 years.
Baseline characteristics were described using frequencies for categorical variables and medians (interquartile range [IQR]) for continuous variables in the total population and stratified by treatment received. Groups were compared using chi-square or Fisher’s tests for categorical variables, and Mann–Whitney U tests for continuous variables.
IVIG dose was 2 g/kg, and steroids were 1–2 mg/kg/day of methylprednisolone or equivalent. Patients were discharged after clinical stability and fever resolution. We used a Markovian multi-state model with the clock-forward approach and unidirectional arrows to build a multi-state model. Three transitions were defined: initiation of treatment to hospital discharge (t1), initiation of treatment to second-line therapy (t2), and second-line therapy to hospital discharge (t3). For each transition, we estimated the time-to-event probability (discharge or second-line therapy) according to treatment initiation therapy (IVIG, steroids, or IVIG plus steroids) using a Cox model weighted with propensity score matching to balance baseline characteristics such as age at admission, presence of comorbidities, and period of recruitment. The weights for the propensity score matching were calculated using generalized linear models by estimating the average treatment effect on the treated using.
Time was measured in days from treatment initiation. A treatment was considered as second line if initiated > 2 days after the first therapy. A multivariable weighted logistic regression analysis was used to estimate the probability of persistent fever (temperature ≥ 38 °C) after 2 days of treatment for each treatment initiation strategy. All the analyses were performed using R software.
Results
Overall, 150 children with MIS-C were enrolled. Only patients initially treated with steroids, IVIG, or IVIG plus steroids were analyzed (n = 132/150; 88%). A total of 18/150 (12%) patients were excluded from the study, including 2 patients treated with steroids plus tocilizumab, 1 treated with tocilizumab, 1 treated with IVIG plus steroids plus anakinra, and 14 with no clear information about initial treatment. In total, 82/132 patients (62.1%) were admitted to a pediatric intensive care unit (PICU), 45/132 patients (34.1%) in the first period, and 87/132 (65.9%) in the second period.
The features of this population according to treatment received are described in Table 1 and according to the period in Supplementary Table 1. The unadjusted and adjusted sample after propensity score matching is summarized in Supplementary Fig. S1. Thirty of 132 patients (22.7%) were initially treated with steroids alone, 29/132 (21.9%) with IVIG alone, and 73/132 (55.3%) with IVIG plus steroids (Supplementary Fig. S2). Thirty-four of 132 (25.7%) patients needed second-line treatment over time: 9/30 (30%) children steroids, 12/29 (41.4%) IVIG, and 13/73 (17.8%) IVIG plus steroids, and 70/132 (53.0%) had persistent fever after 2 days of treatment. Forty-three of 70 (61.4%) patients did not receive a second-line treatment despite persistent fever; 29/43 (67.4%) were initially treated with IVIG plus steroids. In all these cases, fever remised without additional treatment after 48 h. Three patients (2.2%) died.
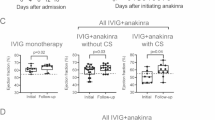
The probability of discharge and of needing second-line treatment was different according to treatment initiation (Fig. 1). The probability of early discharge was 61% higher for patients who initiated treatment with IVIG than for those initiating with IVIG plus steroids (hazard ratio [HR] 1.61, 95% confidence interval [CI]: 1.06–2.44, p = 0.024), whereas no significant differences were observed between patients initiating with steroids versus IVIG plus steroids (HR 1.55, 95% CI: 0.74–3.24, p = 0.246).
Despite the apparent benefit of IVIG on early discharge, the probability of needing second-line treatment was 3 times higher in patients who started on IVIG than on those starting on IVIG plus steroids (HR 3.11, 95% CI: 1.13–8.55, p = 0.028). This was not observed in children who started on steroids (HR 1.70, 95% CI: 0.58–5.00, p = 0.332).
Patients treated with steroids or IVIG plus steroids had a similar probability of persistent fever after treatment initiation (odds ratio [OR] 0.60, 95% CI: 0.31–1.14, p = 0.126). Patients treated with IVIG alone had a higher probability of persistent fever after treatment initiation (OR 4.4, 95% CI: 2.05–9.82, p < 0.001) than patients treated with IVIG plus steroids. When we compared patients initially treated with IVIG or steroids, the former had a 4 times higher probability of persistent fever after treatment initiation (OR 4.23, 95% CI: 1.43–13.5, p = 0.011).
Discussion
This study suggests that the benefits of the examined treatment approaches for MIS-C are different for each outcome assessed. For persistent fever 2 days after treatment, steroids, either alone or in combination with IVIG, seem superior to IVIG alone. Regarding days of admission, IVIG alone is superior to the combination, and the combination is superior to IVIG to the need for treatment escalation.
The results from recent retrospective studies seemed to favor the combination of treatments over steroids or IVIG alone, but the evidence is low, as acknowledged by WHO [8]. Studies in the USA found that the combination of IVIG plus steroids was associated with a lower risk of cardiovascular dysfunction, initiation of vasopressors, and adjunctive therapy versus treatment with IVIG alone [6]. In two studies from France, combination therapy seemed better than IVIG alone to accelerate recovery of cardiac function in patients with cardiogenic shock, and also reduction of fever 2 days after initiation of treatment [5, 10]. The BATS study found that treatment escalation was less common among patients treated with the combination than with either of the other two treatments, but no differences were observed for improvement in the rate of mechanical ventilation, inotropic support, death, or the score on an ordinal clinical-severity scale for any of the three treatments [4].
Since published papers have generally favored the combination of treatments, patients with MIS-C in recent waves have been treated mostly with combined treatments. This limits the observational evaluation of the different approaches. Therefore, we focused on the first waves and adjusted by time.
Our study shows that each treatment seems to have pros and cons. The anti-inflammatory actions of steroids may help to decrease persistent fever after 2 days of treatment, but the regimen typically lasts a minimum of 3 days, and a tapering regimen is needed for prolonged treatments, compared with IVIG alone, which is usually administered in less than 48 h and may accelerate the discharge. If the inflammation of some patients needs strong immunomodulation, and benefits from a combined approach, it is reasonable that IVIG plus steroids are superior to steroids or IVIG alone for the endpoint of escalation of treatment.
The reasons for the reduced benefit of the combination therapy in fever defervescence or early discharge are unclear. It is possible that the combination therapy is beneficial for hemodynamic endpoints as suggested in previous research [6, 10], but less for clinical endpoints such as fever or discharge. Fever is a frequent adverse reaction to IVIG, which may have reduced the benefit of the combined treatment concerning the persistence of fever compared to steroids. However, IVIG-associated fever is a rate-dependent phenomenon that usually occurs during or immediately after the infusion, and rarely 2 days later, as measured here.
Different responses to specific types of immunomodulation might be attributable to genetic differences, SARS-CoV-2 variants, re-exposure to differing or mismatched variants, or prolonged and repetitive exposure to virus circulating within a community [7].
There are limitations to the study. The population was small; the study was not specifically powered for some clinical outcomes, including long-term outcomes such as the presence of aneurysms, which have not been analyzed. However, the population was more homogeneous than the population described in other studies. A major limitation was our inability to analyze relevant endpoints such as shock, PICU admission, or inotropic support after treatment initiation, as children were admitted to the PICU in shock, and patients subsequently received IVIG or steroids, or both, as per guidelines for patients with severe disease, only after the endpoints were reached. Furthermore, we did not have information about the timing of inotrope treatment, aneurysm development, or change of ejection fraction before/after the treatment was prescribed, which impacted the analysis of the effectiveness of these outcomes. Other factors, not evaluated in our study, such as the costs or adverse events associated with each treatment, should be considered, balanced with their clinical benefits.
In conclusion, each treatment seems to have pros and cons according to the different outcomes, also considering the availability of the product and economic factors. Clinical trials are necessary to thoroughly evaluate the effectiveness and safety of the available treatments in short- and long-term outcomes.
Data availability
Anonymized data underlying this article will be shared upon reasonable request to the corresponding author.
Code availability
Not applicable.
Abbreviations
- COVID-19:
-
Coronavirus disease 2019
- HR:
-
Hazard ratio
- IQR:
-
Interquartile range
- IVIG:
-
Intravenous immunoglobulin
- MIS-C:
-
Multi-system inflammatory syndrome in children
- OR:
-
Odds ratio
- PICU:
-
Pediatric intensive care unit
- SARS-CoV-2:
-
Severe acute respiratory syndrome coronavirus 2
- EPICO-AEP:
-
Spanish Society of Pediatrics
References
Moraleda C, Serna-Pascual M, Soriano-Arandes A et al (2020) Multi-inflammatory syndrome in children related to severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) in Spain. Clinical Infect Dis ciaa1042. https://doi.org/10.1093/cid/ciaa1042
Bautista-Rodriguez C, Sanchez-de-Toledo J, Clark BC et al (2021) Multisystem inflammatory syndrome in children: an international survey. Pediatrics 147:e2020024554. https://doi.org/10.1542/peds.2020-024554
García-Salido A, Antón J, Martínez-Pajares JD et al (2021) Documento español de consenso sobre diagnóstico, estabilización y tratamiento del síndrome inflamatorio multisistémico pediátrico vinculado a SARS-CoV-2 (SIM-PedS). Anales de Pediatría 94:116.e1-116.e11. https://doi.org/10.1016/j.anpedi.2020.09.005
McArdle AJ, Vito O, Patel H et al (2021) Treatment of multisystem inflammatory syndrome in children. N Engl J Med 385:11–22. https://doi.org/10.1056/NEJMoa2102968
Ouldali N, Toubiana J, Antona D et al (2021) Association of intravenous immunoglobulins plus methylprednisolone vs immunoglobulins alone with course of fever in multisystem inflammatory syndrome in children. JAMA 325:855. https://doi.org/10.1001/jama.2021.0694
Son MBF, Murray N, Friedman K et al (2021) Multisystem inflammatory syndrome in children — initial therapy and outcomes. N Engl J Med 385:23–34. https://doi.org/10.1056/NEJMoa2102605
DeBiasi RL (2021) Immunotherapy for MIS-C — IVIG, glucocorticoids, and biologics. N Engl J Med 385:74–75. https://doi.org/10.1056/NEJMe2108276
Living guidance for clinical management of COVID-19 (2021) Living guidance, 23 Nov 2021 – World Health Organization (WHO). https://www.who.int/publications/i/item/WHO-2019-nCoV-clinical-2021-2. Last Accessed, 12 Jan 2022
Multisystem inflammatory syndrome in children and adolescents temporally related to COVID-19 (2021) https://www.who.int/news-room/commentaries/detail/multisystem-inflammatory-syndrome-in-children-and-adolescents-with-covid-19. Accessed 9 Jul 2021
Belhadjer Z, Auriau J, Méot M et al (2020) Addition of corticosteroids to immunoglobulins is associated with recovery of cardiac function in multi-inflammatory syndrome in children. Circulation 142:2282–2284. https://doi.org/10.1161/CIRCULATIONAHA.120.050147
Funding
This study was supported by Project PI20/00095, from the Instituto de Salud Carlos III (Ministry of Economy, Industry and Competitiveness) and cofounded by the European Union Regional Development Fund. Juan Miguel Mesa is supported by Fundación para la Investigación Biomédica del Hospital Universitario Infanta Sofía y del Hospital del Henares (FIB 03/2020) and Universidad Europea de Madrid (UEM20/01). Carlos Grasa is funded by the Spanish Ministry of Science and Innovation—Instituto de Salud Carlos III and Fondos FEDER (Contrato Río Hortega CM19/00015) and co-funded by the European Union. Serena Villaverde is funded by the Spanish Ministry of Science and Innovation—Instituto de Salud Carlos III and Fondos FEDER (Contrato Río Hortega CM20/00173) and co-funded by the European Union. David Aguilera-Alonso is supported by a specific Research Project of the Spanish Society of Paediatrics (Asociación Española de Pediatría); Grant Covid-19 EPICO-AEP 2020. Kenneth McCreath is a Scientific Editor funded by Universidad Europea de Madrid.
Author information
Authors and Affiliations
Consortia
Contributions
Alfredo Tagarro and Cinta Moraleda designed the study, contributed to the collection and interpretation of the data, were responsible for data management, drafted the initial manuscript, and reviewed the final version. Sara Domínguez-Rodríguez was responsible for data management, performed the statistical analysis, and reviewed the final version. Juan Miguel Mesa was responsible for data management, contributed to the creation of the manuscript, and reviewed the final version. Cristina Epalza, Carlos Grasa, María Isabel Iglesias-Bouzas, Elisa Fernández-Cooke, Cristina Calvo, Serena Villaverde, David Torres-Fernández, Ana Méndez-Echevarria, Inés Leoz, María Fernández-Pascual, Jesús Saavedra-Lozano, Beatriz Soto, David Aguilera-Alonso, Jacques G. Rivière, Victoria Fumadó, Leticia Martínez-Campos, Ana Vivancos, Francisco Javier Pilar-Orive, Pedro Alcalá, Beatriz Ruiz, Ana López-Machín and Manuel Oltra, contributed to the collection and interpretation of the data, the creation of the manuscript, and reviewed the final version. All the authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the Ethics Committee of Hospital 12 de Octubre, Madrid (code 20/101), and other participating hospitals.
Consent to participate
Participants were enrolled after signed or verbal consent from parents/guardians and by the consent of patients older than 12 years.
Consent for publication
All authors reviewed and approved the manuscript and agreed to publish this work.
Competing interests
The authors declare no competing interests.
Additional information
Communicated by Peter de Winter
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
A complete list of study group members appears in the supplementary.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tagarro, A., Domínguez-Rodríguez, S., Mesa, J.M. et al. Treatments for multi-system inflammatory syndrome in children — discharge, fever, and second-line therapies. Eur J Pediatr 182, 461–466 (2023). https://doi.org/10.1007/s00431-022-04649-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-022-04649-8